Abstract
Background:
Clavicular fractures are commonly encountered in daily practice, and most cases are operated under general surgery. Until now, there has been a debate about the best approach to manage pain in such cases.Objectives:
We aimed to evaluate whether ultrasound-guided clavipectoral block [clavipectoral fascial plane block (CPB)] would be safe and effective in cases with clavicular fractures.Methods:
This prospective randomized study included a total of 40 patients with clavicular fractures; they were divided into 2 groups. Group 1 included 20 cases who underwent CPB, and group 2 included 20 cases who underwent placebo block. Pain score, duration of analgesia, total analgesic consumption, and procedure-related complications were noted and recorded.Results:
Despite the comparable demographic data between the 2 groups, pain scores were significantly lower in group 1 than in group 2, starting from postanesthesia care unit (PACU) admission until 12 hours after the operation. Group 1 showed a significant reduction in 24-hour opioid consumption and significant prolongation of the duration of analgesia compared to the placebo. Patient satisfaction was significantly better in group 1 than in group 2. No block-related adverse events were recorded.Conclusions:
CPB is a safe and effective regional technique that should be used for pain management after clavicular fixation surgery.Keywords
1. Background
Clavicular fractures are frequently encountered in orthopedic practice, and about 80% of these fractures are located in the mid-shaft region. Due to the complexity and variability of the nerve supply of the clavicle, there is an ongoing debate regarding the optimum regional anesthetic technique that could be applied to decrease pain in such cases (1, 2).
It is worthy to mention that the supraclavicular nerve, a branch from the superficial cervical plexus, provides sensory innervation for the skin overlying the clavicle (3). Nevertheless, there is some controversy regarding the sensory nerve supply of the clavicle itself. Some authors believe that it receives its innervation from the suprascapular nerve, while others believe that it is supplied by branches from the brachial plexus nerves, including the long thoracic, subclavian, and suprascapular nerves (3, 4).
In fact, multiple approaches are available to manage clavicular fractures, including general anesthesia or regional techniques such as interscalene brachial plexus combined with superficial cervical plexus blockade (5-7).
The clavipectoral fascial plane block (CPB) is an effective and safe novel regional anesthesia technique, which was originally described by Valdés-Vilches in 2017. They reported injection of about 10 - 15 mL of the local anesthetic agent under ultrasonographic guidance into the space between the clavipectoral fascia and the periosteum of the clavicle itself, on both medial and lateral aspects of the fracture area (8).
Based on intensive literature research, there is a paucity of prospective randomized clinical trials evaluating the safety and efficacy of this novel regional anesthetic technique in adult patients’ midclavicular fractures. That is why we conducted the current study.
2. Objectives
The aim of this study was to evaluate whether ultrasound-guided clavipectoral block (CPB) would be safe and effective in cases with clavicular fractures.
3. Methods
This prospective randomized clinical trial was conducted at the Anesthesia and Intensive Care Department of Tanta University, Egypt, over a period of 6 months from October 2020 to March 2021. This study was approved by the Ethics Committee of Tanta University, Egypt (Number 34111/9/20) and then registered in the Pan African Clinical Trial Registry (code: PACTR202010665720209).
We included adult patients of either sex, aged between 18 and 60 years, diagnosed with clavicular fractures requiring surgical fixation, and classified as class I or II according to the American Society of Anesthesiologists (ASA). On the other hand, we excluded patients with the following criteria: patients’ refusal, body mass index (BMI) ≥ 35 kg/m2, coagulopathy, known allergy to study medications, neurological deficit on the side of surgery, previous neck surgery or radiotherapy, or history of chronic analgesic use. Additionally, uncooperative patients and patients with local infection at the site of surgery were also excluded.
Using the sealed opaque envelope technique, 40 participants were allocated into 2 equal groups: (1) group 1 (the clavipectoral block group; n = 20); and (2) group 2 (the placebo group; n = 20). A nurse blinded to the study procedure and data collection made group assignments.
Before surgery, all cases were subjected to history taking, general and local examination, routine laboratory and radiological investigations. Chest X-ray was performed to rule out pneumothorax, hemothorax, or multiple ipsilateral rib fractures that may present in such cases. Then, informed written consent was obtained from all cases after a complete explanation of the benefits and drawbacks of each intervention. Additionally, patients were informed how to use the Visual Analogue Scale (VAS) to assess pain (9).
All participants were required to fast overnight before surgery. On arrival to the operating theater, routine hemodynamic parameters, including electrocardiogram (ECG), blood pressure, heart rate, oxygen saturation, and temperature, were measured. Also, an IV line (18-gauge cannula) was inserted, and all patients received midazolam 0.05 mg/kg before induction of anesthesia.
Anesthesia was induced in all patients using fentanyl 2 mcg, propofol 2 mg/kg, and cisatracurium 0.15 mg/kg IV to facilitate endotracheal intubation. Maintenance of anesthesia was achieved by cisatracurium 0.15 mg/kg and isoflurane 1.5 - 2% in oxygen and air mixture.
In all patients, the ultrasound-guided block was performed by an experienced anesthesiologist, who had no further role in the study, after induction of anesthesia and before starting surgery when the patient was in the supine position, sterilized, and covered with sterile sheets.
For the clavipectoral block group, the procedure was performed under the guidance of a high frequency (10 - 12 MHz) linear probe. The probe was placed on the skin covering the anterior surface of the clavicle on both the medial and lateral sides of the fracture. The needle was inserted from caudal to cephalic direction using the in-plane approach to avoid pneumothorax. A total of 30 mL of the local anesthetic mixture (1: 1 bupivacaine 0.5% + lidocaine 2%) was injected between the clavipectoral fascia and the clavicle periosteum on both the medial and lateral side of the fracture equally (Figure 1).
Clavipectoral block; A, before injection; and B, after injection (N, needle pathway; CPF, clavipectoral fascia; PM, pectoralis major muscle; LA, spread of local anesthetic).
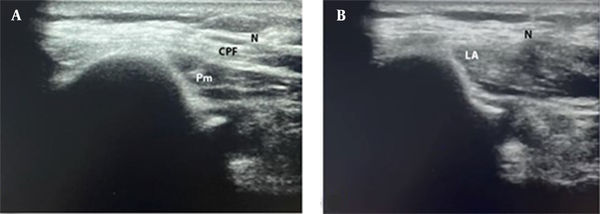
In the placebo group, using the same device and steps, the placebo block was performed. Normal saline (about 30 mL) was injected on both the medial and lateral sides of the fracture at the same plane used for injection in the clavipectoral group.
The pain was assessed by VAS at the following time points: on arrival to PACU and then at 2, 6, 12, and 24 hours after surgery. If the patient reported VAS ≥ 4, IV tramadol 50 mg was administered, and the total 24-hour analgesic consumption was recorded. The patients were asked to rate their degree of satisfaction regarding the analgesic technique on a 5-point scale (0, very satisfied; 1, satisfied; 2, neither satisfied nor dissatisfied; 3, dissatisfied; 4, very dissatisfied). The duration of analgesia was also recorded, and it was defined as the time passing from the time of block until the first analgesic request (10). Additionally, any adverse events related to the blocks within 24 hours were also recorded. Of note, outcome parameters were assessed by another anesthesiologist blinded to the study groups.
The required sample size was calculated on a 2-sample independent t test according to the visual analogue scale score (VAS) reported 2 hours after surgery in our pilot study. It had mean values of 2.00 ± 1.78 and 4.04 ± 2.07 in the block and placebo groups, respectively. Using these data and to achieve a study power of 80%, more than 16 patients in each group were required to detect a significant difference of 2 in the VAS readings. To avoid dropouts, a total of 20 patients were included in each group.
Data were analyzed using SPSS version 26 (SPSS Inc, Chicago, Ill, USA). Categorical data were expressed as frequencies and percentages (%), while in the quantitative data, we used mean and SD for normally distributed data and median and range for abnormally distributed data. To compare 2 groups with categorical variables, the chi-square test (or Fisher exact test) was used. To compare 2 groups with normally distributed quantitative variables, the independent samples t test was used, and the Mann-Whitney U test was used if the data were abnormally distributed. P values < 0.05 were considered significant.
4. Results
According to Figure 1, 59 patients were eligible for our study, 11 patients did not meet our inclusion criteria (4 patients had previous neck surgeries, 3 patients were on chronic analgesic use, 1 patient had a severe hepatic impairment, 1 patient had renal failure, and 2 patients had BMI ≥ 35 kg/m2), and 8 patients declined to participate. Finally, a total of 40 patients were enrolled and randomized into 2 equal groups (n = 20 each; Figure 2).
Randomized trial flow diagram, including enrollment, intervention allocation, and analysis.
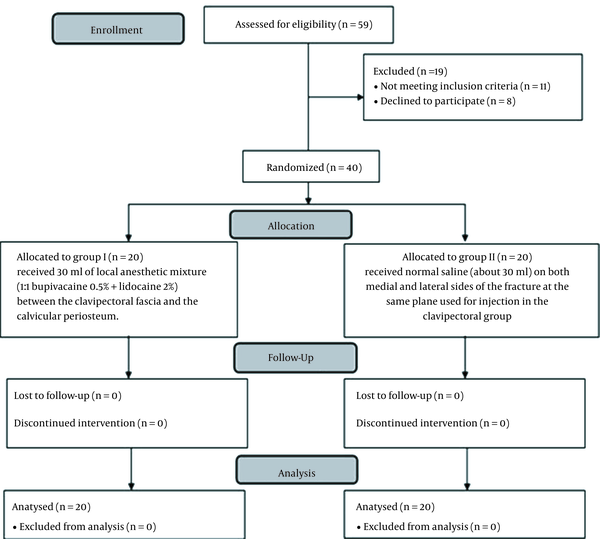
The demographic characteristics, including age, sex, and duration of operation, were comparable between both groups, as shown in Table 1.
| Variables | Group 1; (n = 20) | Group 2; (n = 20) | P Value | CI 95% |
|---|---|---|---|---|
| Age | 35.9 ± 11.9 | 35.7 ± 13.8 | 0.697 | (-9.86; 6.66) |
| ASA physical status | 0.735 | |||
| I | 13 (65) | 14 (70) | ||
| II | 7 (35) | 6 (30) | ||
| Gender | 0.723 | |||
| Male | 15 (75) | 14 (70) | ||
| Female | 5 (25) | 6 (30) | ||
| Duration (min) | 52.55 ± 4.90 | 53.15 ± 5.02 | 0.704 | (-3.78; 2.58) |
| Weight (kg) | 73.65 ± 9.31 | 76.90 ± 8.98 | 0.268 | (-9.11; 2.61) |
VAS was significantly reduced in the clavipectoral block group than in the placebo group, starting immediately from PACU admission until 12 hours after the operation (Table 2).
| Variables | Group 1; (n = 20) | Group 2; (n = 20) | P Value |
|---|---|---|---|
| PACU | 0 [IQ 0 - 1 (R 0 - 1)] | 1 [IQ 0.250 - 1 (R 0 - 2)] | 0.003 b |
| 2 h | 0 [IQ 0 - 1 (R 0 - 1)] | 2 [IQ 1 - 2 (R 0 - 3)] | < 0.001 b |
| 6 h | 1 [IQ 0 - 2 (R 0 - 2)] | 4 [IQ 2.25 - 4 (R 1 - 5)] | < 0.001 b |
| 12 h | 3 [IQ 2 - 4 (R 2 - 5)] | 4 [IQ 3 - 4 (R 2 - 5)] | 0.033 b |
| 24 h | 4.5 [IQ 4 - 5 (R 3 - 6)] | 5 [IQ 4 - 5 (R 4 - 6)] | 0.148 |
Accordingly, the median tramadol consumption in group 1 (50 mg [interquartile range 100 - 100]) was significantly decreased compared with group 2 (100 mg [interquartile range 100 - 150]; P < 0.001; Table 3).
| Variables | Group 1; (n = 20) | Group 2; (n = 20) | P Value b |
|---|---|---|---|
| Tramadol dose (mg) | 100 [IQ 100 - 100 (R 50 - 100)] | 150 [IQ 100 - 150 (R 100 - 150)] | < 0.001 |
| Duration (h) | 16 [IQ 12 - 18.75 (R 12 - 20)] | 6 [IQ 6 - 7.75 (R 6 - 10)] | < 0.001 |
| Patient’s satisfaction | 0.002 | ||
| Very satisfied | 16 (80) | 5 (25) | |
| Satisfied | 3 (15) | 13 (65) | |
| Neither satisfied nor dissatisfied | 1 (5) | 2 (10) | |
| Dissatisfied | 0 (0) | 0 (0) | |
| Very dissatisfied | 0 (0) | 0 (0) |
The median duration of analgesia in group I was 16 hours (interquartile range 12 - 18.75), which was significantly longer compared with group 2 (median = 6 hours [interquartile range 6 - 7.75]; P < 0.001; Table 3).
Also, patient satisfaction was significantly better in the block group (P = 0.002*). No block-related complications were reported in our study (Table 3).
5. Discussion
In general, our results showed no significant differences between the 2 study groups in terms of general characteristics. This ensures our proper randomization. Additionally, it should negate any bias that might have skewed the results in favor of one group rather than the other.
Also, our results revealed that CPB was associated with a significantly lower VAS in PACU and 12 hours after the operation, with a significant reduction in total opioid consumption in patients who received the block. Moreover, the duration of analgesia showed a significant prolongation in the same group and better patient satisfaction. No complications were also reported related to the injection technique.
The current literature is poor on clinical trials handling the efficacy of CPB in clavicular fractures. All of the existing reports are small case series, and to the best of our knowledge, this is the first prospective randomized study to evaluate the efficacy of CPB in clavicular fractures. This represents the strong point of the current study.
Due to the lack of reliable cadaveric studies regarding the innervation of the human clavicle, there is still great controversy about its detailed nerve supply. However, it is agreed that the clavicle and anterior shoulder regions receive a dual nerve supply from both the cervical and brachial plexuses. Therefore, 2 regional anesthetic techniques are required to establish effective pain management in patients with clavicle fractures (11). Previous studies have suggested a combination of superficial cervical plexus block with interscalene block seeking the same aim (7, 12-14). This combination is not only time-consuming, but also has its own complications, including phrenic nerve palsy, Horner syndrome, and vocal cord paralysis (15). Other rare serious complications include total spinal anesthesia, pneumothorax, and vertebral artery injection (11).
The lower VAS and lower total postoperative opioid consumption in our results can be explained by the theory that CPB should provide effective pain relief as all sensory nerves supplying the clavicle pass through the clavipectoral plane except for the suprascapular nerve, which supplies the skin overlying the clavicle. However, Kukreja et al. (11) reported that sensory blockade was noted in this area. They attributed their findings to multiple causes: infiltration of the injected anesthetic agent used in the block itself, diffusion from the local anesthetic infiltration used before the block, or blockade of some branches that might pass through that plane causing sensory loss.
In the same previous study, which included 3 cases undergoing clavicular surgeries, CPB was effective in reducing postoperative pain to zero in PACU in 2 cases. The third case reported a VAS of 6 as the patient had associated-back injuries. However, that case reported 100% satisfaction regarding the block technique (11).
Atalay et al. (16) conducted a case series, including 5 patients (aged 18 - 37 years) undergoing surgery for clavicular fractures. All patients were commenced on postoperative ibuprofen 400 mg every 8 hours. The duration of analgesia ranged between 12 and 22 hours, and at these time points, patients reported VAS between 2 and 4. The authors also reported no complications regarding the pain management technique.
Moreover, Yoshimura and Morimoto (17) confirmed the efficacy of the same technique in their case report, including 2 cases with the same fractures. The first patient reported 0/10 VAS, and no analgesics were needed until the next day. The other patient with COPD reported a VAS of 1 - 2/10 after surgery, and no analgesics were required 13 hours after surgery.
Ueshima et al. reported the application of the same technique in a 57-year-old diabetic patient with coronary artery disease diagnosed with a clavicular fracture. CPB was performed before surgery. The patient experienced 0 out of 10 on a numerical pain scale after the operation. The patient was only commenced on paracetamol 1 gm per 8 hours and maintained that score throughout the first 48 hours after surgery. The procedure was not associated with any complications (18).
Ince and colleagues applied CPB on a 51-year-old male patient with a midshaft clavicular fracture. The pain scale decreased from 8/10 before block till 0/10 after surgery. Subsequent pain assessment revealed 0, 2, 3, 4, 2, and 3 readings at 1, 2, 4, 8, 12, and 24 hours after surgery, respectively. No complications were reported indicating the safety of the block (8).
Our study has several limitations. First, we did not document the sensory distribution of the block. Second, we needed further randomized trials to compare clavipectoral block with other techniques (such as brachial plexus block) to evaluate the effectiveness of CPB as an alternative technique.
5.1. Conclusions
The results of this prospective study indicate that clavipectoral block is a safe and effective regional technique that should be used for pain management after clavicular fixation surgery.
References
-
1.
Qin M, Zhao S, Guo W, Tang L, Li H, Wang X, et al. Open reduction and plate fixation compared with non-surgical treatment for displaced midshaft clavicle fracture: A meta-analysis of randomized clinical trials. Medicine (Baltimore). 2019;98(20). e15638. [PubMed ID: 31096481]. [PubMed Central ID: PMC6531279]. https://doi.org/10.1097/MD.0000000000015638.
-
2.
Edinoff AN, Girma B, Trettin KA, Horton CC, Kaye AJ, Cornett EM, et al. Novel Regional Nerve Blocks in Clinical Practice: Evolving Techniques for Pain Management. Anesth Pain Med. 2021;11(4). e118278. [PubMed ID: 34692446]. [PubMed Central ID: PMC8520672]. https://doi.org/10.5812/aapm.118278.
-
3.
Divizia M, Germani G, Urti I, Imani F, Varrassi G, Meloncelli S. Endoscopic Neuromodulation of Suprascapular Nerve in Chronic Shoulder Pain: A Case Report. Anesth Pain Med. 2020;10(2). e103624. [PubMed ID: 32754436]. [PubMed Central ID: PMC7352948]. https://doi.org/10.5812/aapm.103624.
-
4.
Tran DQ, Tiyaprasertkul W, Gonzalez AP. Analgesia for clavicular fracture and surgery: a call for evidence. Reg Anesth Pain Med. 2013;38(6):539-43. [PubMed ID: 24121609]. https://doi.org/10.1097/AAP.0000000000000012.
-
5.
Sharma P, Shrestha BR. Regional Anaesthesia in Clavicle Surgery. JNMA J Nepal Med Assoc. 2017;56(206):265-7. [PubMed ID: 28746327]. https://doi.org/10.31729/jnma.3152.
-
6.
Margulis R, Francis J, Tischenkel B, Bromberg A, Pedulla D, Grtisenko K, et al. Comparison of Dexmedetomidine and Dexamethasone as Adjuvants to Ultra-Sound Guided Interscalene Block in Arthroscopic Shoulder Surgery: A Double-Blinded Randomized Placebo-Controlled Study. Anesth Pain Med. 2021;11(3). e117020. [PubMed ID: 34540645]. [PubMed Central ID: PMC8438728]. https://doi.org/10.5812/aapm.117020.
-
7.
Faiz SHR, Mohseni M, Imani F, Attaee MK, Movassaghi S, Rahimzadeh P. Comparison of Ultrasound-Guided Supra-scapular Plus Axillary Nerve Block with Interscalene Block for Postoperative Pain Management in Arthroscopic Shoulder Surgery; A Double-Blinded Randomized Open-Label Clinical Trial. Anesth Pain Med. 2021;11(2). e112540. [PubMed ID: 34336619]. [PubMed Central ID: PMC8314074]. https://doi.org/10.5812/aapm.112540.
-
8.
Ince I, Kilicaslan A, Roques V, Elsharkawy H, Valdes L. Ultrasound-guided clavipectoral fascial plane block in a patient undergoing clavicular surgery. J Clin Anesth. 2019;58:125-7. [PubMed ID: 31377668]. https://doi.org/10.1016/j.jclinane.2019.07.011.
-
9.
Heller GZ, Manuguerra M, Chow R. How to analyze the Visual Analogue Scale: Myths, truths and clinical relevance. Scand J Pain. 2016;13:67-75. [PubMed ID: 28850536]. https://doi.org/10.1016/j.sjpain.2016.06.012.
-
10.
Acharya R, Baksi R, Mohapatra P. Comparative Analysis of Duration of Postoperative Analgesia between Levobupivacaine and Levobupivacaine with Clonidine after Ultrasound-Guided Transversus Abdominis Plane Block in Patients Undergoing Lower Segment Cesarean Section. Anesth Essays Res. 2018;12(4):943-8. [PubMed ID: 30662135]. [PubMed Central ID: PMC6319051]. https://doi.org/10.4103/aer.AER_163_18.
-
11.
Kukreja P, Davis CJ, MacBeth L, Feinstein J, Kalagara H. Ultrasound-Guided Clavipectoral Fascial Plane Block for Surgery Involving the Clavicle: A Case Series. Cureus. 2020;12(7). e9072. [PubMed ID: 32782888]. [PubMed Central ID: PMC7413568]. https://doi.org/10.7759/cureus.9072.
-
12.
Olofsson M, Taffe P, Kirkham KR, Vauclair F, Morin B, Albrecht E. Interscalene brachial plexus block for surgical repair of clavicle fracture: a matched case-controlled study. BMC Anesthesiol. 2020;20(1):91. [PubMed ID: 32312249]. [PubMed Central ID: PMC7171737]. https://doi.org/10.1186/s12871-020-01005-x.
-
13.
Banerjee S, Acharya R, Sriramka B. Ultrasound-Guided Inter-scalene Brachial Plexus Block with Superficial Cervical Plexus Block Compared with General Anesthesia in Patients Undergoing Clavicular Surgery: A Comparative Analysis. Anesth Essays Res. 2019;13(1):149-54. [PubMed ID: 31031496]. [PubMed Central ID: PMC6444954]. https://doi.org/10.4103/aer.AER_185_18.
-
14.
Fugelli CG, Westlye ET, Ersdal H, Strand K, Bjorshol C. Combined Interscalene Brachial Plexus and Superficial Cervical Plexus Nerve Block for Midshaft Clavicle Surgery: A Case Series. AANA J. 2019;87(5):374-8. [PubMed ID: 31612842].
-
15.
Verelst P, van Zundert A. Respiratory impact of analgesic strategies for shoulder surgery. Reg Anesth Pain Med. 2013;38(1):50-3. [PubMed ID: 23132510]. https://doi.org/10.1097/AAP.0b013e318272195d.
-
16.
Atalay YO, Ciftci B, Ekinci M, Yesiltas S. The effectiveness of clavipectoral fascia plane block for analgesia after clavicle surgery: a report of five cases. Minerva Anestesiol. 2020;86(9):992-3. [PubMed ID: 32420714]. https://doi.org/10.23736/s0375-9393.20.14503-6.
-
17.
Yoshimura M, Morimoto Y. Use of clavipectoral fascial plane block for clavicle fracture: Two case reports. Saudi J Anaesth. 2020;14(2):284-5. [PubMed ID: 32317907]. [PubMed Central ID: PMC7164465]. https://doi.org/10.4103/sja.SJA_52_20.
-
18.
Ueshima H, Ishihara T, Hosokawa M, Otake H. RETRACTED: Clavipectoral fascial plane block in a patient with dual antiplatelet therapy undergoing emergent clavicular surgery. J Clin Anesth. 2020;61:109648. [PubMed ID: 31732427]. https://doi.org/10.1016/j.jclinane.2019.109648.