Abstract
Introduction:
The os trigonum syndrome is a common cause of posterior ankle pain, often affecting ballet dancers, soccer players, runners and gymnasts who frequently force the ankle into plantar flexion. In rare cases, onset of the os trigonum syndrome followed an acute injury.Case Presentation:
A 62-year-old female patient was admitted with load depended ankle pain and swelling, lasting for five years which promptly started after a car accident. We incidentally discovered os trigonum on plain radiography on a lateral view of the right ankle.Conclusions:
The os trigonum syndrome should take in consideration in elderly subject who had posterior ankle pain starting after a car accident.Keywords
1. Introduction
An os trigonum is one of the bony ossicles of the foot and sits posterior to the talus on the lateral foot radiograph. The os trigonum syndrome might be present in up to seven percent of the population; however, it is commonly asymptomatic and called as a syndrome when the os trigonum is presented with ankle pain (1). Several factors consisting of os trigonum or the Stieda process fracture, an avulsion injury of the posterior talofibular ligament, or cartilaginous synchondrosis disruption might lead os trigonum syndrome (2). It is more frequently bilateral than unilateral and is more predominantly symptomatic in men than in women (3). It is predominantly seen in ballet dancers, soccer players, runners and gymnasts, due to repeated full plantar flexion of the ankle which is resulted with impingement of os trigonum between the posterior lip of the tibia and the calcaneus (4). Meanwhile, symptomatic os trigonum is an unusual cause of ankle pain in late adulthood. In this report, the case of a 62-year-old female patient with a unilateral os trigonum syndrome, which was the result of trauma, has been discussed.
2. Case Presentation
A 62-year-old female patient was admitted to Istanbul Haydarpasa Numune Training and Research Hospital, a physical medicine and rehabilitation outpatient clinic, with load depended ankle pain and swelling, which started approximately 5 years prior to admission. She had stiffness and symptoms typically exacerbated by walking particularly during push-off. She also described difficulty sleeping at night due to pain in her right foot for a year. She was a housewife. She had a history of car accident five years ago. Physical examination reveals posterolateral tenderness and swelling on palpation between the Achilles tendon and medial malleolus. Passive plantar flexion of the ankle and active resisted flexion of the toe reproduce the patient’s symptom. Patient’s pain was evaluated by the visual analog scale and noted as 9 cm. Also, no limitations were observed in range of motion. On rheumatologic evaluation, there were no remarkable findings. She had no systemic diseases.
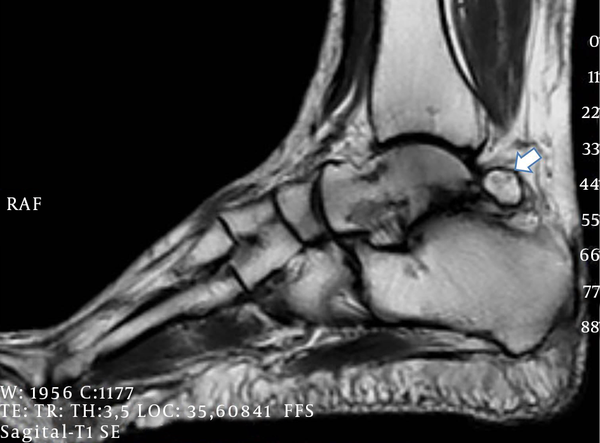
A complete blood count, electrolyte, and acute phase reactant tests revealed no abnormalities. In plain radiography on a lateral view of the right ankle shows a large and round os trigonum with well-defined corticated margins, subchondral cyst formation in the talus and os trigonum due to degenerative change. Sagittal T1-weighted (Figure 1) magnetic resonance imaging (MRI) shows bone marrow oedema in the os trigonum, osteoarthritis of the joint between the os trigonum and calcaneus and flexor hallucis longus tenosynovitis. Based on the findings mentioned above, the patient was diagnosed as having the os trigonum syndrome.
Sagital-T1 Weighted Magnetic Resonance Image of the Os Trigonum (Arrow)
Rest, ice, oral nonsteroidal anti-inflammatory drugs, bracing and also a home exercise program, including stretching and strengthening exercise of the ankle and foot, were initially recommended to provide relief of pain while increasing the range of motion and strength. The home exercise program was ordered starting with 3 repetitions and three sets in a day, which was initially increased to 20 repetitions at the end of the second week. After the treatment and home exercise program for two weeks, pain visual analog score was decreased to 2cm which was 9 cm at baseline (Table 1), and then the patient was followed clinically.
Effects of Rest, Ice, Oral Nonsteroidal Anti-Inflammatory Drugs, Bracing and Home Exercise Program on Pain and Range of Motion
| At Baseline | After Treatment | |
|---|---|---|
| Pain visual analog score | 9 | 2 |
| Ankle range of motion | No limitations | No limitations |
3. Discussion
An os trigonum, also called a posterior ankle impingement syndrome, was initially reported as an accessory ossicle by Rosenmuller in 1804 and resulted of bony and soft-tissue compression in the posterior tibiocalcaneal interval (2, 5). Often as its name suggests, the shape is triangular, with anterior, inferior, and posterior surfaces; however, it can be oval or rounded and variable in size (6, 7). Most patients with an os trigonum are actually asymptomatic and present with just incidentally abnormal radiographic findings in 7% of the population (1). Although mostly asymptomatic, they can gain clinical relevance by trauma or stress on the complex biomechanical system of the foot (3). The os trigonum syndrome has been frequently reported in sport activities that force the ankle into plantar flexion such as ballet, dance, judo, football, basketball, running, and soccer (2). In rare cases, onset of the os trigonum syndrome followed an acute injury (3). As in our case, car accident might initiate the condition.
Diagnosis of the os trigonum syndrome is based primarily on clinical history, physical examination and plain radiography, which may show the presence of an os trigonum. Magnetic resonance imaging can identify the abnormality manifests as bone marrow edema, a fracture line, or fluid in the synchondrosis or osteoarthritis of the joint between the os trigonum and calcaneus and associated flexor hallucis longus pathology (8). If an os trigonum is absent on radiography in chronic ankle pain, an MRI can also help diagnosis.
Treatment begins with nonsurgical treatment including nonsteroidal anti-inflammatory drug (NSAID), steroids and physical therapy exercise (4). The aims of a conservative approach consist of reducing swelling, increasing strength of ankle and food muscles and mobilization of ankle. The NSAIDs and steroids are helpful on reducing swelling by moderating inflammation while exercise program can help the talus to glide forwards slightly during plantar flexion by strengthening the ankle and foot muscles (9). Our case responded dramatically to conservative treatment. In addition to nonsteroidal anti-inflamatuar therapy and physical therapy, symptomatic athletes may need surgical excision of os trigonum secondary to unavoidable plantar flexion associated with their sport (3). This surgery can be performed using open or arthroscopic approaches (3, 10).
As a conclusion, the os trigonum syndrome should also be taken into consideration in patients complaining with posterior ankle pain apart from other frequently encountered causes like dancing, running and playing soccer.
References
-
1.
Maquirriain J. Posterior ankle impingement syndrome. J Am Acad Orthop Surg. 2005;13(6):365-71. [PubMed ID: 16224109].
-
2.
Nault ML, Kocher MS, Micheli LJ. Os trigonum syndrome. J Am Acad Orthop Surg. 2014;22(9):545-53. [PubMed ID: 25157036]. https://doi.org/10.5435/JAAOS-22-09-545.
-
3.
Abramowitz Y, Wollstein R, Barzilay Y, London E, Matan Y, Shabat S, et al. Outcome of resection of a symptomatic os trigonum. J Bone Joint Surg Am. 2003;85-A(6):1051-7. [PubMed ID: 12784001].
-
4.
Horibe S, Kita K, Natsu-ume T, Hamada M, Mae T, Shino K. A novel technique of arthroscopic excision of a symptomatic os trigonum. Arthroscopy. 2008;24(1):121 e1-4. [PubMed ID: 18182212]. https://doi.org/10.1016/j.arthro.2007.04.019.
-
5.
Rosenmüller J. De nonnullis musculorum corporis humani varietatibus. Klaubarth; 1804.
-
6.
Davies MB. The os trigonum syndrome. The Foot. 2004;14(3):119-23. https://doi.org/10.1016/j.foot.2003.12.008.
-
7.
Nwawka OK, Hayashi D, Diaz LE, Goud AR, Arndt W3, Roemer FW, et al. Sesamoids and accessory ossicles of the foot: anatomical variability and related pathology. Insights Imaging. 2013;4(5):581-93. [PubMed ID: 24006205]. https://doi.org/10.1007/s13244-013-0277-1.
-
8.
Rungprai C, Tennant JN, Phisitkul P. Disorders of the Flexor Hallucis Longus and Os Trigonum. Clin Sports Med. 2015;34(4):741-59. [PubMed ID: 26409593]. https://doi.org/10.1016/j.csm.2015.06.005.
-
9.
Performing Arts Physical Therapy. Os Trigonum. [cited 07 February 2016]. Available from: http://www.performingartspt.com/Diagnosis/os%20Trigonum%20Syndrome%20and%20post%20impingement.pdf.
-
10.
Lopez Valerio V, Seijas R, Alvarez P, Ares O, Steinbacher G, Sallent A, et al. Endoscopic repair of posterior ankle impingement syndrome due to os trigonum in soccer players. Foot Ankle Int. 2015;36(1):70-4. [PubMed ID: 25249322]. https://doi.org/10.1177/1071100714552078.