1. Background
The feeling of dry mouth is not directly related to systemic diseases or use of drugs, and the flow of saliva is completely normal; so, the main cause of dry mouth can be a change in the quality of the saliva (1, 2).
Saliva is secreted from the salivary glands and contains bacteria shed from adhering microbial communities on tooth surfaces, gingival crevices, tongue dorsum, and buccal mucosa (3). On the other hand, saliva has mucins and proteins that can protect mucus and dental surface (4, 5). Comparing with serum, saliva collection is easy and non-invasive method, requiring relatively simple instructions for collection and possesses lower protein content and less complexity (6, 7). Nowadays, saliva has important role in monitoring the different disease such as Sjogren’s syndrome (SS), human immunodeficiency virus (HIV) infection, immune responses to viral infections (e.g., hepatitis A, B, and C), systemic levels of drugs, and the detection of illicit drug (8).
It is known that the caries and dental abrasions are caused by mineral decomposition, which is mainly due to a decrease in salivary pH and changes in salivary pH and leads to dry mouth that is one of the main side effects of the action of chemotherapeutic drugs on oral tissues (9, 10). The characteristics of complete saliva and gingival fluid can affect the severity of oral and dental diseases, such as dental caries (11-13) and periodontitis (14).
To determine the clinical risk of caries, it is important to study the effect of various factors such as enamel solubility, pH, bicarbonate buffer, salivary micro flora, diet, and oral hygiene, so that the role of buffering saliva is very important and critical (15).
The ability of human saliva to stabilize the level of acidity to maintain a suitable pH for the oral environment is important in terms of providing sufficient amount of hydroxyapatite in the tooth structure (16); however, the sodium bicarbonate is much more important (17). Buffer capacity means that resistance to pH changes and there is reasonably strong evidence that the salivary buffering capacity protects the tooth from dental caries (18). An association between low caries tendency and high salivary buffering capacity has also been demonstrated. Individuals with a high salivary buffer capacity are often low dental caries (19). Equilibrium and ecological stability of the oral environment can also be related to systemic diseases or drug use, which can all contribute to a qualitative and quantitative change in saliva (20, 21).
Clinical studies have shown that salivary characteristics can be related to the characteristics of the blood (22). In addition, the comparison between blood and saliva has shown that the most important advantage of using saliva samples is its ability to be used in difficult conditions and clinical complexities, for example, in patients with severe depression, low-income children, etc. Moreover, saliva is easy to obtain in comparison with taking blood samples (23).
Cancer, in turn, creates a series of complications in the body, especially in the affected area, which prevents a person from having a normal life (24).
Acute myeloid leukemia (AML) is a cancer of the myeloid line of blood cells, characterized by the rapid growth of abnormal white blood cells that accumulates in the bone marrow and interferes with the production of normal blood cell (25). Such a disease in healthy hematopoiesis is an invasive aspect of this malignancy, which produces undesirable clinical features in most subtypes of the disease (26). AML can be affected by genetic or non-genetic factors, in either an uncontrolled proliferation, or blocking program interfere with the differentiation of bone marrow progenitor cells that, in turn, causes clinical manifestations of the disease (27).
In the present time, it is believed that a variety of cancers, including leukemia, is more incident than before, and health and the oral and dental condition are of the great importance as it profoundly affects patient’s quality of life (28, 29).
2. Objectives
This study aimed at investigating the changes in pH and sodium bicarbonate in saliva of patients with AML before and after chemotherapy. This goal of the study was to evaluate quantitative and qualitative changes in the saliva of individuals with AML after chemotherapy; and if any change is recorded, we could lessen the dental complications through special care and thorough examinations of teeth and oral cavity and coming up with the best treatment plans to be carried out before and during chemotherapy and hopefully promote these individual’s quality of life.
3. Methods
This is a pre- and post-observational-analytic study. The study population was selected by simple random sampling method among the patients with the diagnosis of AML referred to the hematology department of Vali-e-Asr Division of Imam Khomeini Hospital during September 2012 to May 2013.
By analyzing the data from the pilot study, using the formula
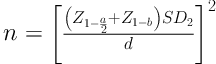
and by considering that the type 1 error equals to 0.05 and the second type error equals to 20% (standard values), the sample size was ultimately calculated to be at least consisting of 40 cases.
The inclusion criteria were all patients aged 18, who were referred to hematology department of Vali-e-Asr Division of Imam Khomeini Hospital with the diagnosis of AML in the absence of active caries or evidence of gingivitis and periodontitis.
After initial oral examination, the patients were informed to sing the informed consent forms. These patients were eligible for chemotherapy with a 7 + 3 regimen.
For sampling, saliva was obtained in the first session of treatment, after clinical examination for a dry mouth, using a questionnaire, while patient was sitting in a comfortable and direct position (rest position). Then, the participants were asked to, first, gulp their saliva and, then, discharge it in a measured tube, every 30 seconds.
The saliva volume was read from the tube after 30 second (1 minute) and divided by time for calculation of the saliva flow. The patient was, then, asked to produce about 5 mL of saliva in a special container by continuing the above procedure. Patients should avoid eating, drinking, and smoking for at least 90 minutes before sampling. This sampling was, then, performed at the last treatment session again (on the 7th day after starting treatment).
3.1. Exclusion Criteria
The following patients were excluded from the study:
-People who died of disease complications within study time.
-Patients who, despite the previous examination, were not able to cooperate with further sampling due to any reason such as the severe complications of the treatment.
-Patients who used radiotherapy or drugs that could affect saliva secretion, such as antihistamines, anticholinergics, antihypertensive medications, Parkinson drug, anticonvulsants and muscle relaxants, tranquilizers and hypnotics, other cytotoxic drugs, and Tricyclic antidepressants.
Saliva samples were centrifuged at a speed of 2200 rpm for 10 minutes (to remove the sputum from the non-stimulated saliva) and, then, transferred with the sampler to the new tubes. Consequently, samples had been stored at -70°C in the Oncology Laboratory of Vali-e-Asr Division of Imam Khomeini Hospital, until they were transferred to the laboratory to test for the study items. Then, by using a PCLM-3 Chloride Meter, the sodium bicarbonate concentration was evaluated. We used coulometric system, which is based on measuring the amount of electricity that passes through the solution and, then, on body weight.
A pH meter (Metrom, Swiss) was also used to show the pH values. This digital device detects the pH levels of the environments based on the electrical voltage generated around the electrodes inside the tested fluids.
After all, the collected information were coded and analyzed, using SPSS (ver. 16.0) and paired t test. The statistical significance for this information was considered to be less than 0.05.
This article has been submitted and authorized at the dental research center by the ethical code number 92-01-70-20863.
4. Results
The average age of the participants was 39 years, of whom 60% were male. Records showed that no history of previous chemotherapy was reported before the current chemotherapy, while after chemotherapy finished, 100 patients complained about a sense of dry mouth.
Based on paired t test analysis, the mean non-arterial flow of saliva before the onset of chemotherapy was 1.647 ± 0.46 mL/min, while the salivary flow rate in the patients after chemotherapy was 1.41 ± 0.49 mL/min, which indicates a significant decrease in the flow rate of saliva after chemotherapy (P < 0.05).
Based on paired t test analysis, the mean untreated saliva pH of patients before the onset of chemotherapy was 7.108 ± 0.35, while the mean salivary pH of them after chemotherapy was 7.015 ± 0.32.
Significant decrease in salivary pH was observed after chemotherapy (P < 0.05).
The mean amount of sodium bicarbonate was 2.622 ± 1.54 mol/mL from the results of paired t test analysis on the data of sodium bicarbonate in unstimulated saliva before starting chemotherapy, while the mean value for saliva after chemotherapy was 1.868 ± 1.33 mol/mL.
Significant decrease in saline sodium bicarbonate after chemotherapy was observed with P < 0.05.
5. Discussion
The results of this study showed that the pH and sodium bicarbonate in the saliva of patients with AML after treatment with the 7 + 3 regimen significantly decreased. Also, a significant decrease in the salivation of these patients happened after chemotherapy compared to that before treatment.
Dry mouth is one of the earliest and most common complaints of patients undergoing chemotherapy. The salivary changes happens in the form of reduction or no secretion, which may occur a week after the onset of chemotherapy (30). The most important cause of dry mouth in patients undergoing chemotherapy/radiotherapy is the involvement of the main salivary glands that reduces the flow rate of the saliva, followed by other consequences such as floral changes of oral cavity, damages to the dental tissues, increased risk of caries, difficulty in swallowing and speaking, and reduced tolerance for dental prostheses (31, 32).
Parenchymal tissue of salivary glands is very sensitive to chemotherapy and radiotherapy drugs, so that dry mouth is the first complication of such treatments (31). The results of this study showed that 100% of the patients would complain a dry mouth during chemotherapy sessions.
The stability of the oral flora may be affected by systemic diseases or the use of certain medications that alter the properties of saliva (20). Research results show that the causes of dry mouth do not significantly change the flow of saliva.
As mentioned, one of the most common causes of dry mouth is medication, which acts through preventing the binding of neurotransmitters and membrane receptors of the salivary glands, or by disturbing the transfer pathway of ions in salivary glandular acinar cells. So, medications affect the quality and quantity of saliva; however, recent studies have shown that this effect is not associated with the majority of drugs (33, 34).
Rojas-Morales et al. showed that there was no positive relationship between pH and sodium bicarbonate in saliva and it is mostly affected by factors such as oral hygiene, quality and quantity of oral microorganisms, diet, and medications (35), which contradicts the results of other studies, including ours. These differences may be because of the nature of drugs used in 2 studies.
There is a minimum secretion of methotrexate or cyclophosphamide in corporal fluids, such as heces and urine after the intravenous administration due to the forced hyperhydration.
The effects of various factors such as solubility of enamel, pH, bicarbonate buffer, bacterial species in saliva, diet, and oral hygiene are important to determine the clinical risk of caries, but the salivary role of saliva is more important than them (15).
In another study by Rojas-Morales et al. in 2006 titled “pH and sodium bicarbonate saliva during treatment for children with leukemia with methotrexate” patients’ saliva were collected in the first treatment session and 10, 20, 24, 31 weeks (a) before treatment commences, (b) 12 hours after receiving intravenous sodium bicarbonate, and (c) 3 hours after receiving the methotrexate. Their results showed that changes in pH and sodium bicarbonate was not seen with the pre-treatment use of sodium bicarbonate (16).
It is believed that the ability of saliva to stabilize the pH of the oral environment in order to maintain the hydroxyapatite of the tooth is important; however, the sodium bicarbonate system is much more important (17).
In a study conducted by Vuotila et al. it has been shown that the flow, pH, and buffering capacity of saliva significantly decreased during radiotherapy; however, in contrast, the risk of bacterial and fungal colonization was significantly increased when the treatment was half through. They also reported the grading of MMPs and its dependency coefficients (15).
5.1. Conclusions
In this study, Our aim was the evaluation of changes in pH and sodium bicarbonate in saliva of patients with AML before and after chemotherapy and we did not find any significant decrease in stimulated saliva flow, salivary pH, and sodium bicarbonate before and after chemotherapy in all patients; however, more researches with larger sample sizes are needed to absorb therapists’ attention to this aspect of the complications of chemotherapy, which affect the patient’s quality of life.