Abstract
Introduction:
Coexistence of horseshoe kidney and ureterocele abnormalities in one patient is a complex and rare condition. The role of heredity in this disease has not yet been proven. Moreover, its diagnosis requires various paraclinical methods.Case Presentation:
A middle-aged male was known to have horseshoe kidney, bilateral ureteroceles and a stone, 1 cm in diameter, in his right ureter. He also had severe hydronephrosis in his left kidney, whereas mild hydronephrosis was detected in his right kidney. Unlike other similar cases, we performed a transverse incision on the ureterocele with no surgery on the horseshoe kidney. Similar cases to date have been treated with partial nephrectomy. Urinary complications and flank pain did not occur during the one-year follow up.Conclusions:
Precise evaluation of patients with one renal abnormality could lead to detection of other associated anomalies. Application of minimally invasive procedures such as ureteroscopic incision is highly recommended in ureterocele treatment.Keywords
1. Introduction
Ureterocele is an anomaly marked with a sac-like pouch in the distal part of the ureter, which can be either intravesical or ectopic. Ectopic ureteroceles are four times more common than intravesical ones and usually coexist with duplicated ureters (1). Bilateral ureterocele in combination with other congenital anomalies is a rare entity and its mismanagement due to misdiagnosis can lead to renal failure (2). Horseshoe kidney is a congenital disorder that involves one in 400 individuals and is more frequent in males (3). At least 50% of cases with horseshoe kidney are asymptomatic. Symptoms are typically related to hydronephrosis, infection or calculus (4). Combination of these two conditions is extremely rare and one stone in a ureterocele is common (4% to 39%); however, our patient had bilateral stenotic ureterocele due to a unilateral stone (3). Taken together, this case is extremely rare and misdiagnosis due to anyserious symptoms could lead to renal failure in such patients.
2. Case Presentation
A 42-year-old man with dysuria and occasional flank pain for 3 - 4 years presented to our clinic. He had no history of kidney complications and received no type of medical treatment except NSAIDS (Nonsteroidal anti-inflammatory drug) due to occasional flank pain.
His family history had nothing remarkable. Physical examination of abdomen and external genitalia revealed normal findings. Regarding laboratory tests, complete blood count, blood urea nitrogen and creatinine had normal results, except for the presence of microscopic hematuria (RBC: 4 - 5, Blood: 1+). In ultrasound study, severe hydronephrosis of the left kidney and a 1 cm stone in the distal segment of the right ureter were reported. The special condition of patient encouraged us to step beyond routine evaluations.
In intravenous pyelography (IVP), the patient had severe hydronephrosis of the left kidney and tortuosity of the left ureter. A large ureterocele was also found in the left ureter resulting in an intravesical filling defect (Figure 1). In the right side mild hydronephrosis, large stone of the distal ureter and a typical ureterocele were observed (Figure 2). In addition, the lower poles of the kidneys faced each other and the ureter crossed the lower poles of both kidneys, indicating a horseshoe kidney (Figures 1 and 2). In KUB (Kidneys, Ureters and Bladder) performed for the patient, a stone in the distal segment of the right ureter was clearly observed. For treating the ureterocele, we used the transverse incision method in 1 cm length according to the textbook of urology (Campbell Walsh) (4) and two papers on ureterocele treatment (5, 6). The stone at the distal segment of the right ureter underwent lithotripsy and its fragments were removed using a basket. The patient was hospitalized for one day and then discharged.
On IVP, Tortuous of the Left Ureter and a Big Ureterocele in the Left Ureter Are Seen
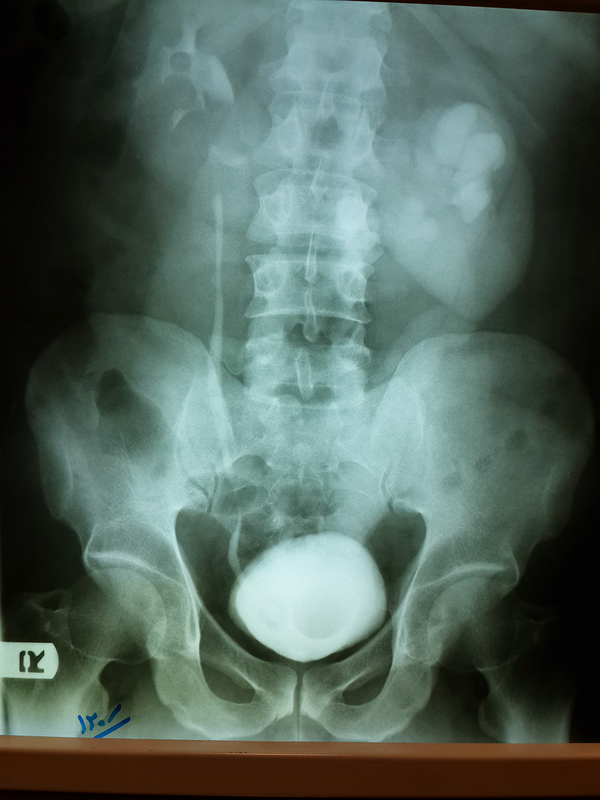
On IVP, Intravesical Cobra Head and Filling
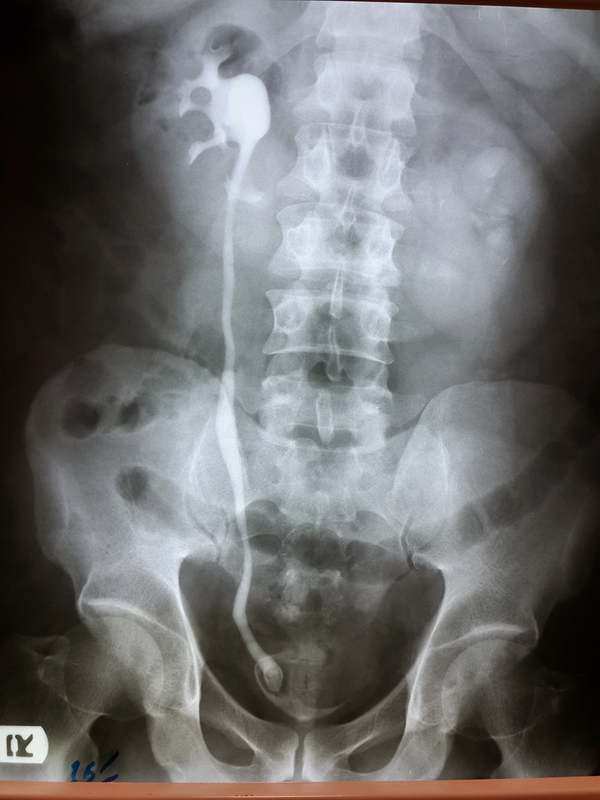
One month later, to remove the Double J (DJ) stent, both ureters were examined with a ureteroscope, indicating no evidence of stenosis. At his 3-month follow up, MRU (Magnetic Resonance Urography) was performed which reported a normal right urinary system, while the left kidney had moderate hydronephrosis and the kidneys connection at the lower poles confirmed as a horseshoe kidney. After one year, the patient experienced no urinary complications, infection or flank pain and his laboratory tests had normal results.
3. Discussion
Ureteroceles are diagnosed in one of 4000 individuals and are more common in females than males (1). The case presented here had bilateral stenotic ureterocele. The prevalence of bilateral ureteroceles is 10% and most previous similar cases were unilateral ectopic ureteroceles (7). Bilateral ureteroceles in a non-duplicated urinary system are very rare, especially along with renal stones; only 9 such cases have been reported so far (8). Ureteroceles are categorized into stenotic ureteroceles with unduplicated ureters and ureteroceles associated with duplex ureters (9). Clinical findings in patients with ureteroceles include infection, obstruction of vesical outlet, hematuria and incontinence (1). Today, many ureterocele cases are diagnosed prenatally using ultrasound techniques. Worth noting, the preferred type of treatment differs for each individual.
The most common type of fused kidneys is horseshoe kidney (1). It seems that the main etiology is adhesion of two metanephrons in the embryonic stage; this happens when the kidneys are still at the pelvic level (10). In horseshoe kidney, the lower poles are stuck together (Isthmus). Presence of non-localized pain that spreads into the lower lumbar parts is a common symptom. In rare cases and in the presence of a large isthmus, the patient may experience abdominal pain, nausea and vomiting (the Rovsing sign). Our case did not complain any of these symptoms and therefore no surgical change was performed on the kidneys (1).
Presence of bilateral ureterocele along with horseshoe kidney in a patient is a rare and uncommon finding. This anomaly has been reported in a few cases so far and the treatment of choice differs among such patients.
In the case reported by Mikuma et al. upper pole ureteropyelostomy was performed with ligation of the distal ureter and unroofing the ureterocele. This is an open surgical technique accompanied with certain morbidity (11). In another case report, ureterocele endoscopic puncture was performed on a two-month girl (12). The treatment performed on our patient was minimally invasive resulting in minimum morbidity for the patient. It consisted of breaking and removing renal stone with a ureteroscope and a transverse incision of the ureterocele floor besides placing a Double J (DJ) stent for one month. He experienced no complications during his one-year follow-up.
Nevertheless, this treatment had one limitation; megaureter dilatation cannot be corrected by this technique and this goal can only be achieved with open surgery. Yet, endoscopic management has lower morbidity and shorter hospital stay for the patient which is considered a priority.
In conclusion, precise evaluation of patients with one renal abnormality is highly recommended as it can result in detection of other associated anomalies. MRU is also highly beneficial in the diagnosis of congenital anatomic abnormalities. Application of minimally invasive procedures such as ureteroscopic incision is the preferred approach in ureterocele treatment.
References
-
1.
Donald Ridgeway S. General urology. New York: Lange Medical Publications; 1975.
-
2.
Dada SA, Rafiu MO, Olanrewaju TO. Chronic renal failure in a patient with bilateral ureterocele. Saudi Med J. 2015;36(7):862-4. [PubMed ID: 26108593]. https://doi.org/10.15537/smj.2015.7.11786.
-
3.
Hicks CC, Boehm GA, Sybers RG, Stone HH, O'Brien DP. Traumatic rupture of horseshoe kidney with partial ureteral duplication associated with supernumerary kidney. Urology. 1976;8(2):149-52. [PubMed ID: 960346].
-
4.
Walsh PC, Campbell MF, Wein AJ. Campbell-Walsh Urology. 10 th ed. Philadelphia: Saunders Elsevier; 2007.
-
5.
Cichon W, Malik L, Maciukiewicz P, Kotula J. Bilateral ureterocele in adult--a case report and review of literature. Przegl Lek. 2014;71(8):460-1.
-
6.
Sen V, Aydogdu O, Yonguc T, Bozkurt IH, Polat S, Basmaci I. Endourological treatment of bilateral ureteral stones in bilateral ureteral duplication with right ureterocele. Can Urol Assoc J. 2015;9:7-8.
-
7.
Schlussel RN, Retik AB. Campbell-Walsh Urology. 9 th ed. Philadelphia: Saunders; 2007. 3398 p.
-
8.
Shamsa A, Asadpour AA, Abolbashari M, Hariri MK. Bilateral simple orthotopic ureteroceles with bilateral stones in an adult: a case report and review of literature. Urol J. 2010;7(3):209-11. [PubMed ID: 20845303].
-
9.
Stephens FD, Smith ED, Hutson JM, Fernbach SK. Congenital anomalies of the urinary and genital tracts. AJR-Ame J Roentgenol. 1996;167(5):1114.
-
10.
Knutson T, Hawas B. Horseshoe kidney with a circumcavalureter. Scand J Urol Nephrol. 2004;38:3.48E+52.
-
11.
Mikuma N, Adachi H, Takatsuka K, Yokoo A, Wada H, Takahashi A. Ectopic ureterocele with a horseshoe kidney in an adult. Int J Urol. 1996;3(3):243-4. [PubMed ID: 8776627].
-
12.
Chiang G, Kaplan G. Management of ectopic ureterocele with horseshoe kidney. J Pediatr Urol. 2009;5(5):400-1. [PubMed ID: 19328741]. https://doi.org/10.1016/j.jpurol.2009.02.208.