1. Background
Spinal cord stimulation (SCS) is an effective treatment option for pain relief in patients with intractable chronic neuropathic leg(s) and back pain, commonly including failed back surgery syndrome (FBSS), complex regional pain syndrome (CRPS), and ischemic pain, like refractory angina pectoris (rAP), and peripheral vascular disease (PVD) (1-4).
The cost-effectiveness of non-rechargeable spinal cord stimulators (NR-SCS) was studied in a health technology assessment (HTA) in the National Institute of Health and Clinical Excellence (NICE) in the UK and was published by Simpson et al. (4), where it was compared to reoperation and conventional medical medicine (CMM). In this HTA, they found that SCS was more cost-effective than both CMM and reoperation.
In 2010, Taylor et al. (5) extended the NICE analysis, comparing NR-SCS and more costly rechargeable spinal cord stimulation (R-SCS) systems with CMM. They concluded that R-SCS was more cost-effective than NR-SCS as long as the longevity of NR-SCS was 4 years or less, confirming the earlier findings by Hornberger et al. in the U.S (5, 6).
In the meantime, new stimulation designs have entered the neuromodulation arena including high-frequency SCS (HF-SCS) and burst SCS (B-SCS). Various studies have consistently shown that they are at least as good as traditionally applied tonic stimulation waveforms. What is even more is that the development of these waveforms has led to paresthesia-free stimulation and can even suppress the pain better than classical tonic stimulation does (7-10). Furthermore in a recent multi-center study, they found that burst stimulation further improved the result in responders using tonic stimulation and it had the potential to rescue non-responders to keep the benefits of their implant (11).
In a study by Annemans et al. (12), they suggested that HF-SCS was better than both NR-SCS and R-SCS with tonic stimulation concerning the cost-effectiveness and to obtain a greater number of quality-adjusted life-years (QALYs). In a study regarding response comparison and budget impact modeling, Vancamp et al. (13) found that burst stimulation is cost-effective in comparison to tonic stimulation (with NR-SCS and R-SCS) and conservative medical management.
In the healthcare environment we are currently in, comparative clinical effectiveness and cost-beneficial administration of applied therapies have attracted increasing interest, as allocated public money needs to be spent wisely. Therefore, it is wise not only to investigate the clinical effectiveness and safety but also to estimate the potential cost-effectiveness of these devices and novel therapy options (12).
2. Objectives
In this study, we did not aim to study the cost-effectiveness, but rather the cost-benefit and consequences of NR-SCS versus R-SCS.
3. Methods
The study was designed to compare the cost reductions between R-SCS and NR-SCS systems in patients implanted with either system between 2005 and 2011. Calculations were based on a population of 86 patients with SCS implants. Ethical Committee approval for this study was obtained from the “Comité de Ética de la Investigacion de la Fundacion Jimenez Diaz”, Madrid, Spain.
The average age of the patients was 56 years (SD = 14 years; range = 32 - 84) and the gender distribution in the sample was 69.8% (n = 61) females and 30.2% (n = 27) males. All patients in the sample were diagnosed with FBSS and underwent pain management therapies according to the best clinical practices before being considered as candidates for implantation of a neuromodulation device, like conventional treatment, rehabilitation, and interventional approach. All patients followed a rigorous clinical investigation and screening process to ensure and confirm the diagnosis of therapy-refractory FBSS, as well as to rule out any exclusion criteria (e.g. coagulopathy, neuropsychiatric disorders, cardiac pacemakers, pain medication abuse, and the more).
After a trial period of 15 days, patients received their NR-IPG implants and were further followed up at the pain clinic as per standard practice.
In this study, 55 patients were implanted with a dual quattrodeTM and GenesisTM implantable pulse generator (IPG) (St. Jude Medical, Inc., Minneapolis, MN). The remaining 31 patients received either a dual Pisces QuadTM (n = 18) with SynergyTM NR-IPG or a single Pisces QuadTM connected to a VersitrelTM (n = 11) or Itrel 3TM NR-IPG (n = 2) (Medtronic, Inc., Minneapolis, MN).
The life expectancy of patients was calculated according to the National Statistical Institute and the sample was analyzed at 10-year intervals from birth to 100 years of age, determining, according to the life of the device implemented, the number of replacements that each patient would require, bearing in mind that the life expectancy of a male is 77.8 years and of a woman is 84.1 years (14).
In the cost reduction study, the average life of the implanted device was valued depending on the type of non-rechargeable device implanted to make a comparison between the use of a rechargeable system during the patient’s lifetime (based on the starting age and life expectancy), compared to the use of a non-rechargeable system.
To calculate the average life of each device, we used the tables published by the two companies St. Jude Medical, Inc. (Minneapolis, MN) and Medtronic, Inc. (Minneapolis, MN) found in their implant manuals; this was the only way to empirically calculate the estimated duration of the NR-SCS systems (15, 16). Costs were considered both the cost of the device and the cost of necessary accessories for its correct operation, such as the cost of the intervention and the cost of possible adverse effects.
For the economic analysis, we valued costs according to the expenses caused by the procedure. The expenses were associated with both the devices and the intervention necessary to carry out the implants. Concerning the expenses associated with the surgery, the human and physical resources needed to carry out the intervention were analyzed. The operating room staff included one attached pain unit, one anesthesiologist, one assistant, one radiodiagnostic technician, one nurse, one nursing assistant, and one caretaker; operating room material; stay in day hospital care; day hospital staff: 1 attached pain Unit, 2 nurses, 1 nursing assistant and healing material in day hospital; we have to take into account the expenses of surgical complications and in NR-SCS the expenses of a replacement reoperation in each patient.
All expenses were considered with the estimated time for the intervention of one hour so that in all cases we could do the calculation over time. The procedure was analyzed with the costs incurred in an hour of work.
Indirect costs of loss of salaries or productivity and the time spent with careers were omitted because there is a general consensus that there will be little difference in the loss of work and the use of indirect careers. For the analysis, data obtained in the publications of the Sanidad Publica bulletins and all economic values were expressed in Euro (€).
4. Results
Gender distribution analysis showed no differences between the groups regarding the average age. The average life expectancy (life years left of the patient according to the life expectancy in Spain) was 33 ± 13.3 years, without differences between the two groups in the study. The gender distribution analysis predominated the female gender (69.8%) over the male gender (30.2%), without differences between the groups.
The average duration of non-rechargeable generators was 58 months (M) (range = 5.9 - 163.1 M; SD ± 40.4 M), as commented on this value, it is an approximation using the parameters applied in the device for each patient. The assessment of the duration of the systems considers in each case the impedance, the pulse width, the frequency and the amplitude that was programmed, as noted during the performed telemetries.
About 40% (39.5%) of the patients using a non-rechargeable implant presented a system duration of more than 60 months. When we analyzed the results by intervals, we found that 12.8% of the sample had a duration equal to the duration determined by the FDA for a rechargeable system of St. Jude Medical (a 10-year-old device should operate at least 24 h between each recharge) and 18.6% had a duration equal to a rechargeable Medtronic system (a nine-year-old device will cease to function automatically after this period) (15, 16).
In comparison with life expectancy, 98% of the sample patients were candidates for a rechargeable generator when the study was conducted. When the duration of the rechargeable generator was considered (considering a life cycle of the device limited to 120 months), 86% of the sample patients were candidates for a rechargeable generator. Once these two criteria, i.e., life expectancy and estimated battery life, were applied, 14 patients were not candidates for a rechargeable generator. The main reason was that the life of the non-rechargeable battery life was longer than that of the FDA’s approved average battery duration for a rechargeable system in 12 patients (12 of 14 patients; 86%). In the other two patients (14%), the reason was to have a life expectancy below the duration of the device at the time of the analysis.
When we analyzed the distribution of the population according to age and gender, no conclusions could be drawn from the total study population. It can be highlighted that in the 30 - 39 years’ range (10 patients), a cost reduction would be obtained compared to two patients in which expenditure would be higher. In the 40 - 49 years’ interval, nine patients generated savings compared to 13 in which no cost reduction would be achieved and in the 50 - 59 years’ interval, four patients would reduce expenditure by implementing a rechargeable system, compared to seven who would not. When the costs arising from the replacements were met, the percentage of the sample studied was 59% (Table 1).
| Life Expectancy | Duration of R-SCS of the Same Company | Replacement Costs During the Battery Lifetime of R-SCS | Replacement Costs During the Patients’ Life | |
|---|---|---|---|---|
| Total candidates (n = 86) | 84 (98) | 74 (86) | 47 (55) | 51 (59) |
| No candidates | 2 (2) | 12 (14) | 39 (45) | 35 (41) |
Patient Candidates for an R-SCS System When the Three Parameters Were Applied: Life Expectancy, Battery Lifetime, and Costs of Battery Changesa
In the comparison of the use of a rechargeable system against a non-rechargeable system in the total studied sample (n = 86), depending on the life expectancy of the patients, it was noted that the use of rechargeable devices would result in an average savings of €56,322 per patient over their lifetime. This accounts for a 43% reduction of costs using a rechargeable system versus a non-rechargeable system, taking into account that the price of the non-chargeable system was €131777,62 and that of the rechargeable system was €75445,47 during the lifetime of a patient.
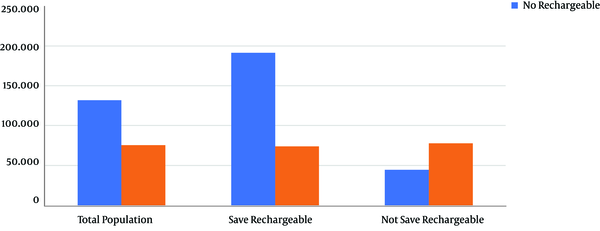
In this study, we found that in the total sample, there were 41% of the patients in whom the rechargeable device not only did offer no economic benefit but added the expenditure to the process (an added cost of 74%) while 59% of the sample showed the reduced costs of the procedure, with savings of 61% of the costs (Figure 1).
The total cost of the procedure when the cost of the device was included was €9,150,411.19 in patients with an NR-SCS device compared to €3,415,076.96 with savings of €5,735,334.23, representing a total saving of 63% to the public health system over the life of a patient implanted. When the analysis was made based on the life of the R-SCS device, savings were 60% in favor of the rechargeable system [€2,527,555.93 versus €1,019,269.76 (Table 2)].
| Group (N = 51) | Final Cost of Replacements During the Lifetime of R-SCS, € | Final Costs During the Lifetime of Patients, € |
|---|---|---|
| NR-SCS | 2,527,555.93 | 9,150,411.19 |
| R-SCS | 1,019,269.76 | 3,415,076.96 |
| Difference | -1,508,286.17 | -5,735,334.23 |
| Savings, % | -60 | - 63 |
Final Costs of Replacements During the Lifetime of Patients with R-SCS and NR-SCS
As commented, there are cases in which the direct implant of a rechargeable system implies an added expense to the procedure. The cases in which it does not generate savings are those cases in which the number of replacements of the R-SCS device is similar to the number of replacements of the NR. This happens when the battery life of the non-rechargeable device is very long because of the patient’s characteristics and/or energy needs. This situation occurs when the batteries of non-rechargeable systems last: VersitrelTM > 40 months (3.3 years), SynergyTM > 63 months (5.25 years), Itrel 3TM > 40 months (3.3 years), and GenesisTM > 53 months (4.4 years).
The final population of economic impact analysis was 51 patients with an elevated output energy need: 34 patients with Genesis, four patients with VersitrelTM, and 13 patients with SynergyTM. Within these 51 patients, the economic figures were analyzed in two different assumptions: 1) A NR-SCS patient requiring replacement surgery with a NR-SCS system and 2) a patient with a NR-SCS system who underwent a R-SCS system replacement surgery. Integral costs for battery changes included NR-IPG, personnel in the OR, personnel in day hospital, materials used in the OR, the hourly cost of the OR, and hourly cost of the day hospital. Similar costs are used for battery changes of an R-IPG; the price of an NR-IPG generator would be €8,491.5 compared to €17,031.8 of an R-IPG; the rest of the costs was the same in both cases, corresponding to the overall of both surgeries; depending on whether the implant was NR-IPG or R-IPG, the final difference was €11,289.5 versus €19,829.8.
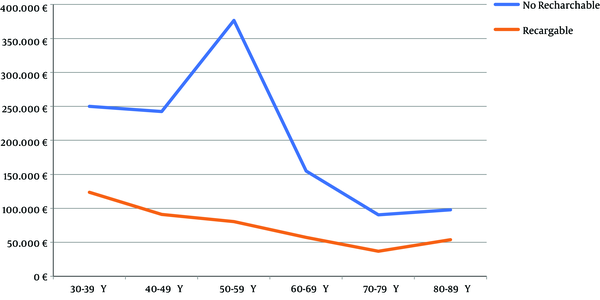
In the analysis of patients with high energy needs (n = 51), a more detailed study was conducted and the average cost of R-SCS systems relative to NR-SCS systems was analyzed over the lifespan of the patients per age-group. It was observed that the percentage of savings obtained was proportional to the average duration of the NR-SCS device in these age groups. Patients with an R-SCS device who generated higher savings (79% savings) were those with higher energy needs: 16 months’ battery duration and 50 - 59 years of age (Figure 2).
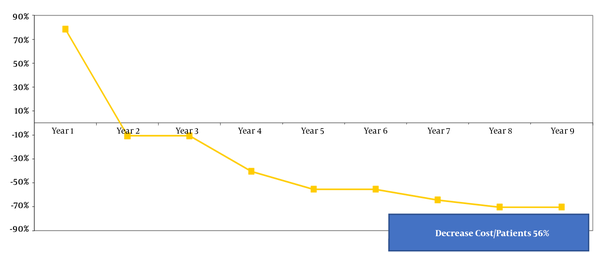
Finally, a comparative analysis was carried out in which we obtained the difference in costs generated by the use of the R-SCS device compared to the NR-SCS during the life of a rechargeable device. We considered a minimum of nine years. The analysis was carried out for the energy profile of the sample of patients with high needs: an average of 30 months duration of the NR-SCS device. The analysis only considered the cost of the devices and the cost of replacement surgery. No adverse effects were included. The negative percentages represented savings when using the R-SCS system rather than the NR-SCS system.
It was observed that, throughout the life of the device (nine years), the average saving would be 56%, equal to €26,512, per patient for the analyzed population (Figure 3).
The average replacements during the calculated lifetime of patients would be 9.2 replacements in our study when using NR-SCS systems versus 2.2 replacements when using R-SCS systems. Considering the average costs, a simplified calculation showed that the replacement surgery costs would be €25,741.6 for NR-SCS systems and €6,155.6 for R-SCS systems over the expected lifetime of a patient. This results in €19,586.00 savings on procedural costs per patient when using R-SCS systems. In our study, we also calculated an average of 3% complication rate (procedural complication with replacements, infections, etc.) that resulted in an average complication cost of €1,220.35 over the lifetime of a patient when using R-SCS versus €2,872.36 when using NR-SCS.
5. Discussion
Cost studies appear to be an essential part when involving any high-level medical work or performing medical material. Where such studies are conducted in reference to stimulation systems, they add a difficulty: the alleged tolerance to treatment or the lack of functional recovery or improvement that a patient reaches when dealing with these devices.
The study is not about the effectiveness of the system, we performed a cost-benefit because we need to analyzed the benefit of implanting a R-SCS vs NR-SCS. We assumed that the system was effective given the time it was implanted in our patients. The objective of this study was to verify if it was more cost-effective to implant an R-SCS system versus an NR-SCS system at our center.
In all the analyses carried out, according to the life of the patient, the average life of the generator and the expenses derived from the replacements in response to the life expectancy of the patients, in a real sample of patients, the result is favorable to implant immediately an R-SCS system. Although when the focus is only put in the expense caused by the replacements of an R-SCS system compared to an NR-SCS system, only 51 patients (59.3%) would be the candidates. When the economic difference is taken into scope, it seems that it would be advisable to implanting R-SCS systems, with a long-term benefit of €56,322.15. But, when it is taken into account with the expense caused in the patients who were candidates for an R-SCS system, the saving was greater than €115,000, with a saving percentage of greater than 61%.
On the other hand, although the half-life of the systems is four years, it seems that the most repeated value was 2 - 3 years, seen in most recent studies of the economic benefit of implanting a rechargeable system when the non-rechargeable system lasts less than four years; therefore, at this point, the implantation of this type of devices also seems favorable compared to the implant of a conventional system.
When a more detailed analysis was performed for the population with high energy needs (n = 51), considering the average cost of R-SCS systems versus NR-SCS systems looking at the different age groups of the patients, it was noted that the percentage of savings obtained was proportional to the average duration of the NR-SCS device in these age groups. Patients in which the R-SCS device would generate higher savings, with 79% savings amounting to almost €300,000, are those with higher energy needs; in these patients, the average battery duration of NR-SCS systems was found to be averaging 16 months. One important finding is that most of them were in the age range of 50 - 59 years, taking into account the fact that the average age of the population was 58 years.
It is important to note that the comparative analysis was made in a way to assess the difference in costs obtained by the use of the R-SCS device versus NR-SCS device, during the life of an R-SCS device. The study considered nine years for R-SCS systems since two of the commercial houses had this period of time accepted by the FDA, and that it was performed on the energy profile of the sample of patients with high needs that had an average of 30 months’ duration of NR-SCS device. This study also observed that the length of the device's life of nine years would be expected to result in average savings per patient for 56% of the population (about €30,000). The savings of the R-SCS implant versus NR-SCS systems appeared before the second year, with saving close to 10%, resulting in savings up to 70% in nine years.
When all these data are analyzed, it seems that the R-SCS implants would result in a significant reduction in costs compared to NR-SCS systems at all points analyzed. According to these data, it seems clear that the first system to be implemented is an R-SCS system although before the conclusion of this assertion, certain aspects must be considered: the initial cost of the R-SCS system versus NR-SCS, patients who fail therapy due to lack of effectiveness at two years or earlier, and the energy needs of each patient and pathology.
These three points must be analyzed before venturing to make sure that an R-SCS system is to be implemented in all patients and for every pathology and that they can be corrected before the start of treatment. A good selection of patients, with a correct analysis of anatomical, clinical, and psychosocial criteria, could clarify the second point and remove those patients who are not actually the candidates for neurostimulation in general. A good patient selection would also allow countering the initial cost of therapy, with medication adjustment and visits to consultation and emergency, which in some cases may also match this initial cost. The other cardinal point that must be performed correctly and thoroughly to avoid an economic loss is a correct staging of a test phase. During the test period, the patient and the physician must pursue realistic expectations with the benefit that can be obtained from this treatment and if the result is expected to be sustainable while at the same time trying to avoid patients would get discouraged and require the system’s to be explanted. During this phase, the energy needs of each patient must also be calculated, as well as the life expectancy of the system, so as to make a selection for the appropriate device, taking into account the energy needs and the pathology and evolution hereof, as well as the abilities of the patient to properly function and take care of the device and of course environmental factors and compliance issues inherent to each patient. An overview of considerations to choose NR-IPG versus R-IPG is based on the initial cost and maintenance cost, as well as on other variables, the patient’s life expectancy, the type of pathology in the diagnosis, the energy requirements such as the parameters used, the time of use, the type of programming (cyclic or continuous), and the estimated half-life of the system once the trial period is carried out. The physical constitution of the patient must also be taken into account, especially in patients who are thinner or without much adipose tissue an R-IPG system must be implanted, compared to more obese patients in whom the size of the system does not matter. The patient’s compliance must be analyzed; finally, a vital importance today is the type of wave (burst, HF, high density, etc.) that we want to use; if our patients needed a new waveform, like HF, or Burst, energy requirements would make it impossible to use a NR-SCS.
The results showed that using R-SCS, the number of replacements was 2.6 to 4.2 times less compared to when using NR-SCS (6). With an average of 4.2 times, fewer replacements were needed when using R-SCS in our study; thus, we confirm the findings by Hornberger et al. (6).
With the introduction of novel waveforms, as mentioned in the introduction, a multi-waveform capable IPG may be not only more clinically beneficial for patients’ therapeutic outcomes, but also more cost-beneficial and cost-effective, as there will be less need for replacements (12, 13) The reduced need for replacements lays in the fact that treatment modalities may be switched right on the implanted device (stimulation designs) without the need for physical intervention. Furthermore, it has been shown in several studies that the way stimulate patients can move from non-responders to responders has changed, showing that the change of mode of stimulation, can bear a significant improvement in patients (11, 17, 18). Therefore, these multi-modality generators should be not only more efficacious clinically but also more cost-efficient than standard single-waveform IPGs. Upgradability will further augment this positive effect as updates may be downloaded into the implants through an app-based solution. In the future, we plan to do a cost-effectiveness analysis to include novel stimulation designs and compare them with more traditional pain treatment paradigms.
Despite the data we obtained from this cost-benefit study, we still believe that a general recommendation should not be made, but a detailed study of each patient and each case should be done, taking care of not only coats, but also medical and social reasons in each environment.