1. Background
Cytokines, including tumor necrosis factor-alpha (TNF-α), interleukin-6 (IL-6), and interleukin-10 (IL-10), are systemic inflammatory and anti-inflammatory immune responses. They are key modulators of inflammatory reactions and are closely related to the extent of tissue damage secondary to the activity of the immune system. Anti-inflammatory cytokines, such as IL-10, can inhibit the release of TNF-α and IL-6. Cytokines are released following any tissue damage by immune cells (macrophages, lymphocytes, and mast cells) and non-immune cells (endothelial cells and fibroblasts) and play an important role in defense mechanisms, wound healing, and posttraumatic pain.
The concentrations of circulating cytokines are normally low and may be undetectable within 30 - 60 minutes after the start of surgery. The level of IL‐6 increases significantly at 2 - 4 hours after surgery. Under physiological conditions, cytokines act as immunomodulatory components, which limit potential damages or excess inflammatory reactions. Under pathological conditions, such as major surgery, trauma, hemorrhagic shock, pancreatitis, burns, and ischemia-reperfusion injury, cytokine excess may lead to systemic inflammatory response syndrome (SIRS) or immunosuppression. The exaggerated release of cytokines in the perioperative period may have disturbing effects on the central nervous system, cardiovascular system, lungs, liver, and kidneys. The cytokine concentrations are maximal at 24 hours after major surgeries and remain elevated for 48 - 72 hours postoperatively (1-4).
Minimally invasive techniques and laparoscopic methods are preferred over open surgeries to improve the preservation of immune function (5). The greatest increase in the IL‐6 level occurs after major procedures, such as joint replacement and major vascular and colorectal surgeries. A high IL-6 level is associated with postoperative complications and is recognized as a predictor of morbidity after surgical interventions (6, 7). Inhibition of the production of cytokines, including IL-6, can protect the body against traumatic injuries and infections under pathological conditions; therefore, cytokine inhibitors or antagonists may have the capacity to reduce tissue/organ dysfunction (8, 9).
Besides surgery, modification of the anesthesia-related immune response may decrease perioperative morbidities by reducing the proinflammatory cytokine expression (1). However, there are conflicting findings about the effects of anesthetics (5, 10, 11) and the type of anesthesia (12, 13) on cytokine release and postoperative immune responses. Cesarean section is one of the most frequently performed surgical procedures worldwide, with an increasing trend (14). Recent studies have shown that a normal pregnancy is associated with a controlled inflammatory process (15), while cesarean section, as a major surgery, may aggravate the previously increased level of cytokines in pregnant women (16). Nevertheless, studies on cytokines in the cesarean section population are limited, and the results are contradictory.
2. Objectives
Therefore, this study aimed to compare the serum levels of cytokines after general anesthesia (GA) and spinal anesthesia (SA) in cesarean section.
3. Methods
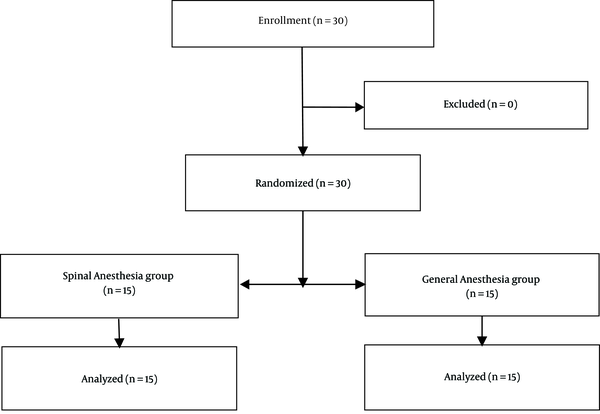
This prospective, single-blind, randomized controlled clinical trial was registered at the Iranian Registry of Clinical Trials (code: IRCT20200930048887N1). It was approved by the Research Ethics Committee of Shahid Beheshti University of Medical Sciences, Tehran, Iran (code: IR.SBMU.MSP.REC.1398.169) and conducted between June 2018 and February 2019. After obtaining informed consent from the participants, 30 American Society of Anesthesiologists (ASA) class I and II parturients, scheduled for cesarean section, were included in the study. They were randomly assigned into two equal groups of SA and GA (15 patients per group) (Figure 1).
Randomization was carried out using a table of random numbers. The names of the groups were written on cards and placed in sequentially numbered and sealed envelopes. When an eligible woman entered the study, an envelope was opened in sequence by a person who was not involved in the study, and the participant’s group was assigned. Patients with coagulation disorders, phospholipid syndrome, and difficult intubation criteria were excluded. Also, women with a surgery duration < 60 minutes and > 2 hours were excluded from the study since a longer surgical duration might result in the greater manipulation of the viscera, the greater complexity of the procedure, and therefore, a higher release of inflammatory factors.
In the SA group, 2.8 mL of 0.5% bupivacaine (Mylan, Saint Priest, France) was injected intrathecally into the L3-L4 or L4-L5 interspace with a 25 Quincke spinal needle. In the GA group, anesthesia was induced with 4-6 mg/kg of thiopental and 1 - 1.5 mg/kg of succinylcholine, and endotracheal intubation was performed while using the Sellick maneuver. Anesthesia continued with oxygen, 50% nitrous oxide, 0.8% isoflurane, and 0.15 mg/kg of atracurium. After delivery, 200 µg/70 kg of fentanyl and 2 mg/70 kg of midazolam were administered. The muscle relaxant was reversed with atropine and neostigmine, and the subjects were extubated and transferred to the recovery room. All subjects also received intravenous oxytocin after delivery and were given two 100-mg diclofenac suppositories at the end of surgery to control postoperative pain.
The anesthesia and surgery were uneventful in women. None of the subjects received transfusion during surgery. Venous blood samples were taken for measuring the levels of IL-6, IL-10, and TNF-α before induction of anesthesia and 30 minutes after entering the recovery room. The serum levels of cytokines were measured using an enzyme-linked immunosorbent assay (ELISA) (Mabtech, Nacka, Strand, Sweden) in the laboratory of our hospital. The laboratory staff and data analyzers were unaware of the assignment of the study groups.
SPSS version 22.0 (SPSS Inc., Chicago, IL, USA) was used for data analysis. Based on previous studies, at a power of 80% and significance level of 5% (delta = 6.6, SD = 9.8), a sample size of 15 patients was calculated for each anesthesia group. The student’s t-test or Mann-Whitney U-test was used to compare quantitative variables. Chi-square and Fisher’s exact tests were also used to compare categorical variables. First, a t-test was performed for intergroup assessments. The age difference between the two groups was found to be significant. Therefore, assessments were performed in the two groups using the ANCOVA test. Also, covariance analysis allowed us to remove the effect of age as a confounding factor from the analysis. A P-value less than 0.05 was considered statistically significant. Data are presented as mean ± SD.
4. Results
Thirty patients in the age range of 18 to 36 years were included in this study. The mean age of the patients in the SA group was significantly lower than the GA group. There was no significant difference in terms of other characteristics (Table 1). In the GA group, the serum levels of IL-6 and TNF-α significantly increased after surgery as compared to the preoperative levels. In the SA group, no significant difference was observed in any cytokines (Table 2). However, there were significant differences in the preoperative and postoperative levels of TNF-α between the two groups. The levels of IL-6 and IL-10 were similar in the SA and GA groups (Table 3). Changes in the IL-6 and TNF-α concentrations were significantly higher in the GA group compared to the SA group, while changes in the IL-10 level were not significant (Table 4). There were no significant differences in the ratio of IL-6 change to IL-10 change or TNF-α change to IL-10 change between the two groups (Table 5).
| Variables | SA Group (N = 15) | GA Group (N = 15) | P-Value |
|---|---|---|---|
| Age, y | 26.3 ± 4.9 (18-34) | 29.7 ± 3.1 (26-36) | < 0.03b |
| Number of pregnancies | 2.2 ± 0.7 | 2.3 ± 1.5 | 0.595 |
| Number of abortions | 9 (60) | 13 (87) | 0.265 |
| Weight, kg | 80 ± 9.3 | 79.1 ± 9.8 | 0.28 |
| Height, cm | 164.4 ± 3.4 | 164.1 ± 3.5 | 0.31 |
| BMI, kg/m2 | 29 ± 3.3 | 29.2 ± 2.5 | 0.35 |
| Surgery duration, min | 85.7 ± 11.3 | 84 ± 11 | 0.42 |
The Patients’ Characteristicsa
| Cytokines | Time | SA Group (N = 15) | GA Group (N = 15) | P-Value |
|---|---|---|---|---|
| IL-6, pg/mL | Before surgery | 7.6 ± 12.5 | 2.1 ± 0.8 | 0.11 |
| After surgery | 5.0 ± 6.6 | 6.0 ± 3.1 | 0.92 | |
| IL-10, pg/mL | Before surgery | 4.4 ± 5.3 | 3.0 ± 2.1 | 0.442 |
| After surgery | 4.8 ± 3.8 | 3.2 ± 0.3 | 0.089 | |
| TNF-α, pg/mL | Before surgery | 3.6 ± 0.3 | 3.3 ± 0.3 | 0.023* |
| After surgery | 3.4 ± 0.3 | 4.0 ± 0.6 | 0.00* |
Comparison of Serum Cytokine Concentrations Between the Two Groups
5. Discussion
In the current study, we found that the levels of IL-6 and TNF-α significantly increased after surgery compared to their preoperative levels in the GA group in comparison with the SA group. Moreover, the postoperative concentration of TNF-α, as well as changes in the IL-6 level, was significantly higher in the GA group as compared to the SA group. However, changes in the IL-10 levels were not significant throughout the study. We did not find any significant difference in the concentration of IL-10; also, no significant difference was found in the ratio of IL-6 changes to IL-10 changes or TNF-α changes to IL-10 changes between the two groups. The reason may be that the IL-10 level usually rises hours after the operation, while we measured postoperative cytokines only 30 minutes after surgery (12, 17).
Interestingly, Malamitsi-Puchner et al. (15) found that the serum level of IL-6 in pregnant women who had a vaginal delivery was higher than in those with caesarian sections. Their findings may be attributed to the severity of labor pain in parturients with a vaginal delivery. However, their study did not determine whether patients in the vaginal delivery group received analgesia; also, the type of anesthesia used for the caesarian section was not mentioned. It is noteworthy that TNF enhances the production of IL-6 in the amniotic fluid and plasma during labor, which affects the ripening of the cervix, stimulation of uterine contractions, and rupture of the amniotic membrane (18).
Oscan et al. (12) investigated the effects of GA combination with thoracic epidural analgesia on the cytokine response after laparoscopic cholecystectomy. They found that the level of interleukins increased significantly in the epidural saline administered group, compared to patients who received levobupivacaine and fentanyl via an epidural catheter. The IL 6, IL 8, and IL 10 levels started to increase at two hours and returned to the basal level at 24 hours in the groups. The anti-inflammatory effects of local anesthetics may be important in modulating the release of cytokines following regional anesthesia (19).
On the other hand, Buyukkocak et al. (13) found no significant difference in the effects of GA and SA on the IL-6, TNF-α, C-reactive protein (CRP), cortisol, and leptin levels at 24 hours after hemorrhoidectomy as a minor surgery. Similarly, in a study by Zura et al. (20), IL-6 was elevated in both GA and SA groups for transurethral resection of the prostate (without any significant differences), which may indicate the lower level of tissue damage in this type of procedure. GA appears to have little effect on the immune system in healthy cases and patients undergoing short-term minor surgeries; in other words, changes in the immune system are associated with major surgeries (21).
In our previous study (22), we compared the effect of SA versus GA on attenuating the increased cytokine levels in preeclampsia patients undergoing a caesarian section and observed a greater increase in the cytokine level of the GA group compared to the SA group. We suggested that the use of SA for cesarean section in preeclampsia patients may slow the increase in cytokines after surgery. Contradictory to our results, Mohammed Ashery et al. (17) showed that at 30 minutes after anesthesia induction and at four hours postoperatively, the levels of IL-6 and TNF were significantly higher in the SA group compared to the GA group in benign abdominal hysterectomy. The level of anti-inflammatory IL-10 also significantly increased in the GA group at four hours after surgery as compared to the SA group. A probable explanation for our results may be the prohibition of opioid administration before delivery in the GA group.
Moreover, Dermitzaki et al. (23) compared GA with epidural anesthesia in cesarean section. They found that the serum concentration of IL-6 was significantly higher at 24 hours after cesarean section as compared to the corresponding levels immediately before anesthesia, after uterine incision, and before umbilical cord clamping. However, the concentration of IL-6 was similar in both anesthesia techniques. The reason for the discrepancy between our findings and their results could be the better control of postoperative pain in their study. In their study, in the GA group, the surgical incision was infiltrated with ropivacaine, and mothers received intravenous meperidine and paracetamol upon admission to the post-anesthesia care unit. In the epidural group, postoperative analgesia was achieved by combining local anesthetics with narcotics through an epidural catheter.
Besides, Mohammed et al. (24) measured the levels of IL-1β and TNF-α before anesthesia and at 12 and 24 hours postoperatively in the GA and SA groups of women with cesarean section. They revealed that the mean serum level of IL-1β in both groups significantly increased after 12 and 24 hours of anesthesia; however, there were no significant differences between the two anesthesia groups. This study did not provide a clear explanation about GA and regional anesthesia techniques and did not mention the method of postoperative pain control.
Perioperative pain may play an important role in modulating cytokines (25). For example, postoperative analgesic modalities after laparoscopic colorectal surgery attenuated the cytokine response as IL-6 expression (26). Although our patients received 200-mg diclofenac suppositories for postoperative pain management, the pain scores were not assessed at the time of sampling in the recovery room, which may be a limitation of our study. Moreover, measurement of cytokines at 30 minutes after admission to the recovery room may prevent the possible effects of pain and related medications on cytokines.
Another limitation was the measurement of cytokines in both elective and emergency cesarean patients; therefore, some women entered the operating room after enduring labor pain, which might have affected the production of cytokines. It might also be the reason for heterogeneity in the SD of cytokine levels in our study. Therefore, further studies are needed to investigate the effect of perioperative analgesia on cytokine release using both anesthesia methods. It is also recommended to evaluate the level of cytokines in women who endure labor pain before surgery in future studies. Another limitation of this study was that the serum levels of cytokines were measured once in the recovery room due to budget restrictions and staff shortage.
In conclusion, the concentrations of IL-6 and TNF-α were significantly lower in the SA group as compared to the GA group in healthy parturients after cesarean section. Therefore, we suggest SA as a better option for women undergoing cesarean section.