1. Introduction
The incidence of tracheal stenosis in pregnant women requiring laryngotracheal resection and reconstruction is limited. There is a high probability that conservative management is proposed until the end of gestation. However, the physiologic changes in pregnancy, such as diaphragmatic elevation, capillary congestion of the larynx, upper airway edema, increased minute ventilation, and carbon dioxide (CO2) production, are challenging for the anesthetic approach of patients with tracheal stenosis. Therefore, we present two successful cases of transnasal humidified rapid insufflation ventilatory exchange (THRIVE) in pregnant patients diagnosed with tracheal stenosis, which required surgery to resection the stenotic segment and terminal-terminal anastomosis.
2. Case Presentation
Written informed consent was obtained before patients’ inclusion. This case report was approved under the ethical approval code by Fundación Valle del Lili’s Institutional Review Board (in letter no. 171 of 2021, Act no. 11 of 2021, and submission no. 535).
2.1. Case 1
A 19-year-old female patient, Gesta1 parturition 0, at 37.5 weeks of pregnancy, with a history of sickle cell anemia managed with ferrous sulfate, folic acid, acetylsalicylic acid, and calcium carbonate was consulted due to moderate to severe hypogastric pain, associated with regular uterine activity and light vaginal bleeding. She was admitted to the high obstetric care unit.
The patient reported a history of severe community-acquired pneumonia that led her to develop septic shock with multiorgan failure and required transfusion of two packed red blood cell units. As a complication, she presented transfusion-related acute lung injury, which manifested as acute type one respiratory failure requiring endotracheal intubation to ensure gas exchange. The case was on invasive mechanical ventilation for 16 days; since then, the patient reported dyspnea, dysphonia, and stridor. Nasofibrobronchoscopy was performed, which showed three areas of tracheal stenosis, the most severe of which compromised 80% of the lumen with characteristics of tracheomalacia.
In the obstetric high care unit, the patient received analgesia, oxygen support with a nonrebreathing mask, and fluid therapy with significant clinical improvement. Subsequently, a multidisciplinary meeting was held involving the gynecological-obstetric intensive care, head and neck surgery, and anesthesiology teams. The consensus was reached; since the patient was in the latent phase of labor and the regularity of contractions decreased, priority was given to managing the airway pathology. The multidisciplinary team decided to resect the tracheal segment and terminal-terminal anastomosis with a surgical technique that allowed Valsalva maneuvers to complete the pregnancy vaginally. However, a plan was prepared if a cesarean section was required to terminate the gestation.
On the day of surgery, the patient was in good general condition. The case was admitted with several vital signs, including a blood pressure of 132/78 (96) mmHg, a heart rate of 121 beats per minute, and peripheral arterial oxygen saturation of 98%. She had venous access #18 G in the right upper limb. The patient was monitored with a continuous electrocardiogram on the visoscope to visualize the DII lead, noninvasive blood pressure, peripheral arterial oxygen saturation, and bispectral index. The surgeon performed the surgical safety checklist recommended by the World Health Organization (WHO). The patient was induced after administration of lidocaine at 1 mg/kg with propofol in target-controlled infusion (TCI) according to the Schnider model with a site-effect concentration of 3 mcg/mL and remifentanil in TCI according to the Minto model at an site-effect concentration of 1 ng/mL. A high-flow nasal cannula with the AirvoTM 2 device was used, with the fresh gas flow at 40 L/minute, relative air humidity of 100%, a gas temperature of 37°C, and an inspired oxygen fraction of 0.80. After induction, an anatomically guided bilateral superficial cervical plexus block was performed. The left radial artery was cannulated for continuous blood pressure monitoring and arterial gas sampling during the transoperative period.
The anesthetic maintenance was performed with propofol in TCI with an site-effect concentration of 3 mcg/mL and remifentanil in TCI with an site-effect concentration of 1 ng/mL. Analgesia was given with diclofenac at 1 mg/kg plus morphine at 0.1 mg/kg. Prophylaxis for postoperative nausea and vomiting was performed with ondansetron 4 mg. A volume of 700 mL of Ringer’s lactate was administered throughout the surgery, and the estimated blood loss was approximately 100 mL.
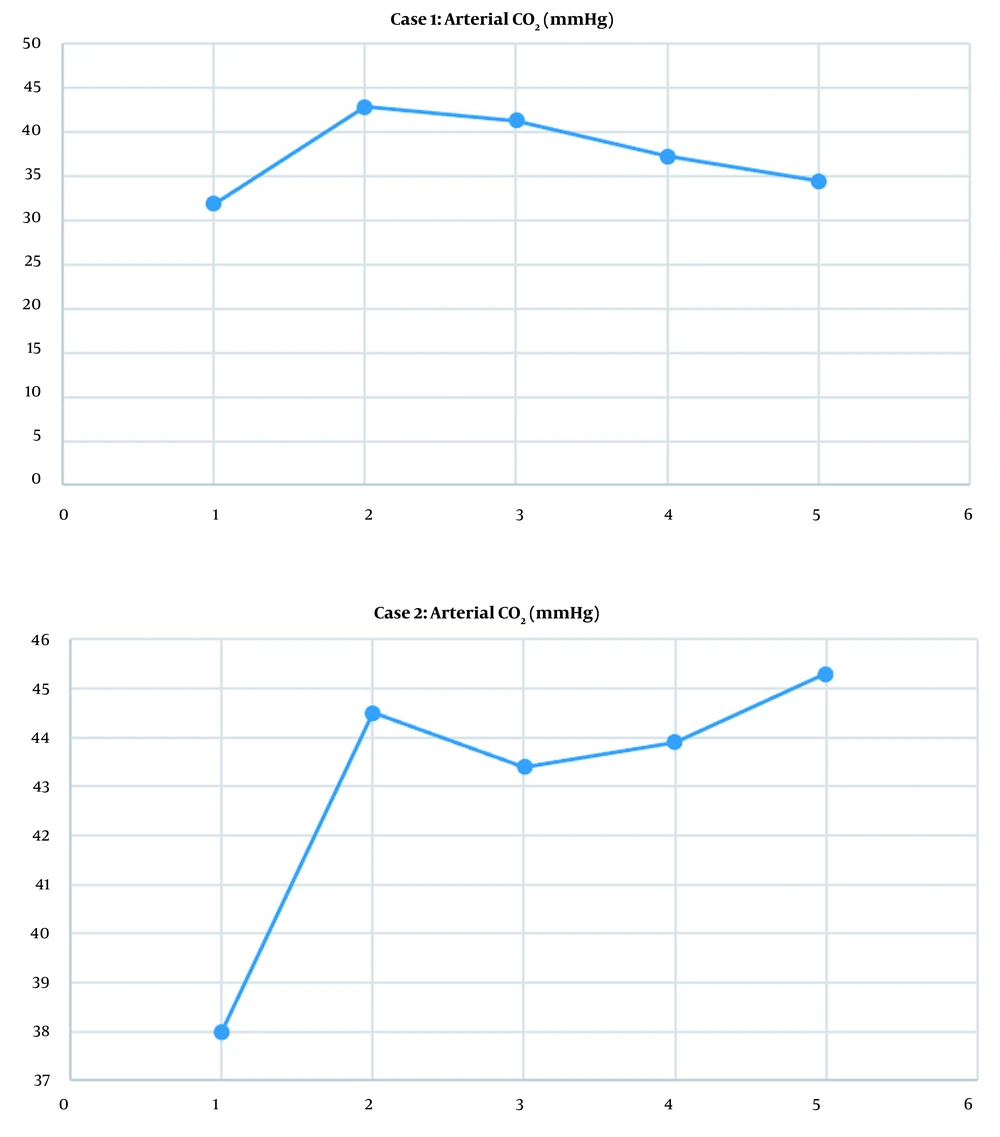
The duration of anesthesia was approximately 2 hours, and the surgery took 1 hour 30 minutes. The surgical procedure went without complications, and the patient required no vasopressor or vasodilator support. Oxygenation was adequate as measured by peripheral oxygen saturation, which remained above 90% during the event. Likewise, spontaneous ventilation was adequate and maintained throughout the procedure, evidenced by an arterial partial pressure of carbon dioxide (PaCO2) within 30 to 45 mmHg (Figure 1A).
Once the surgery was completed, the high-flow nasal cannula was removed, and the patient was transferred to the intensive care unit for airway surveillance. On the 1st postoperative day, the patient presented adequate evolution, with no dyspnea, no signs of respiratory distress, and saturated 99% with oxygen support by conventional nasal cannula at 2 L/minute. Her arterial gases showed a PaCO2 of 33.6 mmHg and partial pressure of oxygen of 137 mmHg. Given stationary labor and a progressive decrease in platelet count on the 2nd postoperative day, the obstetrics decided to terminate the pregnancy surgically.
2.2. Case 2
A 29-year-old female patient, Gesta 1 parturition 0, at 17.3 weeks of pregnancy, had a history of prolonged hospitalization for organophosphate poisoning and required prolonged endotracheal intubation in the intensive care unit (with no data in the clinical history of the exact days of invasive mechanical ventilation). After extubation, the patient presented laryngeal stridor on exertion and reported having dyspnea of progressive severity since the beginning of gestation. Therefore, the case was evaluated using pulmonology, and hospital admission was ordered for a comprehensive assessment.
Nasofibrobronchoscopy was performed with evidence of 80% tracheal stenosis on admission. In addition, a computed tomography scan of the neck was performed, which reported 70% tracheal stenosis of 4.1 cm in length, whose proximal end was 3.1 cm from the vocal cords and its distal end was 6.3 cm from the carina. The patient was admitted to the obstetric high care unit with several vital signs, including a blood pressure of 100/60 (73) mmHg, a heart rate of 75 beats per minute, and peripheral arterial oxygen saturation of 98%, without oxygen support. She was evaluated by a head and neck surgery that indicated the resection of the stenotic segment and terminal-terminal anastomosis after evaluation by the anesthesiology service and approval of the specialists in gynecological-obstetric intensive care.
On admission to the operating room, the patient was in an acceptable general condition, with no signs of respiratory distress, without the presence of stridor at rest. She was monitored with a continuous electrocardiogram on the visoscope to visualize the DII lead, noninvasive blood pressure, peripheral arterial oxygen saturation, and bispectral index. Initial vital signs included a blood pressure of 113/72 (85) mmHg, a heart rate of 80 beats per minute, and 99% peripheral arterial oxygen saturation. The case had a left upper limb peripheral venous access #22 G.
The surgical safety checklist recommended by the WHO was performed, and the high-flow nasal cannula was positioned with the AirvoTM 2 device with the same parameters used in the first case. The patient was induced after administration of lidocaine 40 mg with propofol by TCI according to the Schnider model with an site-effect concentration of 1 mcg/mL and remifentanil by TCI according to the Minto model with an site-effect concentration of 1 ng/mL. The site-effect concentration of propofol was increased 10 minutes after induction to 3 mcg/mL. Subsequently, an anatomically guided bilateral superficial cervical plexus block was performed and cannulated ulnar arterial line.
The anesthetic maintenance was performed with propofol in TCI with an site-effect concentration of 3 mcg/mL and remifentanil in TCI with an site-effect concentration of 1.2 - 1.4 ng/mL. Analgesia was given with diclofenac at 1 mg/kg and dipyrone 30 mg/kg plus morphine at 0.1 mg/kg. Prophylaxis was performed for postoperative nausea and vomiting with 4 mg of dexamethasone and 4 mg of ondansetron. A volume of 750 mL of Ringer’s lactate was administered throughout the surgery, and the estimated total bleeding was approximately 150 mL.
The duration of anesthesia was approximately 2 hours 30 minutes, and the surgery lasted 2 hours. The surgical procedure went smoothly, requiring a single dose of 8 mcg of norepinephrine. Oxygenation was adequate as measured by peripheral oxygen saturation, which remained above 90% throughout the event. Likewise, spontaneous ventilation was adequate and was maintained throughout the procedure, evidenced by an arterial PaCO2 within 30 to 45 mmHg (Figure 1B).
At the end of the surgery, the patient was transferred to the obstetric intensive care unit for airway surveillance. The case was hospitalized seven days after the procedure with no signs of respiratory distress or uterine activity. On the 6th postoperative day, control nasofibrobronchoscopy was performed, and no airway stenosis or edema was observed.
2.3. Description of the Anesthetic Technique
2.3.1. First
The high flow nasal cannula was positioned with the AirvoTM 2 device, with the fresh gas flow at 40 L/minute, relative air humidity of 100%, a gas temperature of 37ºC, and an inspired oxygen fraction of 0.80.
2.3.2. Second
After administering lidocaine 40 mg, anesthetic induction was performed with propofol in TCI according to the Schnider model at an site-effect concentration of 3 mcg/mL and remifentanil in TCI according to the Minto model at an site-effect concentration of 1 ng/mL.
2.3.3. Third
A bilateral superficial cervical plexus block was performed guided by anatomy at the level of the midpoint of the posterior border of the sternocleidomastoid muscle and 5 mL of bupivacaine at 0.5% was injected. The needle was changed for a 22 G Spinocan needle and punctured from toward the mastoid infiltrating 2.5 mL of 0.5% bupivacaine and again from that initial point toward the clavicle infiltrating 2.5 mL of 0.5% bupivacaine. Bupivacaine 0.5% with epinephrine 1: 200000 plus simple bupivacaine 0.5% was used.
2.3.4. Fourth
Once the patient loses consciousness, the nasal cannula flow was increased to 60 L/minute, and an arterial line was cannulated for continuous blood pressure monitoring and serial arterial gas sampling. Anesthetic induction lasted approximately 20 - 25 minutes, and during this time, the airway was topicalized with 1% lidocaine spray. The surgery started with the trachea dissection distal to the stenotic rings. An incision was made, and a pediatric venous cannula of extracorporeal circulation attached to a connector of an endotracheal tube connected to the high flow nasal cannula was positioned. Adequate oxygenation and ventilation were confirmed, and the surgeon continued the dissection until the resection of the stenotic segment.
2.3.5. Fifth
With the pediatric venous cannula, the flow of fresh gases was decreased to 40 L/minute. When the surgeon had resected the stenotic segment and reconstructed the tracheal wall, the venous cannula was removed, returning the system to the high flow nasal cannula.
2.3.6. Sixth
The fresh gas flow was again increased to 60 L/minute. Subsequently, the tissues were closed in planes, and a chin-sternum stitch was placed to protect end-to-end anastomosis. The presence of airway edema was checked with nasofibrobronchoscopy, and if edema was observed, the airway was protected with orotracheal intubation. Otherwise, spontaneous ventilation was continued in the postoperative period. Transitional analgesia was performed with diclofenac 1 mg/kg, dipyrone 30 mg/kg, and morphine 0.1 mg/kg. Prophylaxis with 4 mg of dexamethasone and 4 mg of ondansetron at the beginning and at the end of the surgery, respectively, were administered
3. Discussion
Tracheal stenosis is a rare diagnosis during pregnancy, and information on the anesthetic management of this pathology is limited to case reports (1). In this context, the anesthetic management in the pregnant patient is challenging given the physiological variations associated with pregnancy and the implications on maternal-fetal well-being. In addition, tracheal stenosis is an entity with multiple treatment options, including tracheostomy, balloon dilatation, laser resection, and laryngotracheal reconstruction surgery, all with different considerations for anesthesiologists in the perioperative management of these patients.
The physiological changes that an anesthesiologist should consider in the surgical management of pregnant patients with tracheal stenosis are the changes in the respiratory system. From the first trimester of pregnancy, capillary congestion in the upper airway (2) predisposes patients to bleeding and edema. The diaphragm rises, and the vertical diameter of the thoracic cavity decreases by 4 cm, which, associated with the growth of the uterus, generates a decrease in the residual functional capacity (3). Minute ventilation increases mainly due to the increase in tidal volume and in response to the increase in resting CO2 production (3). Despite increased CO2 production from the 12th week of gestation, the PaCO2 decreases due to the reduction of alveolar dead space. In addition, there is an increase in oxygen consumption secondary to uterine and fetal growth (3).
Regarding the case reports found in the literature, only one describes the case of a pregnant patient with tracheal stenosis who underwent surgery for the resection of the stenotic segment. Naqvi et al. (4) reported that the patient was at 28 weeks of pregnancy and presented with tracheal stenosis after prolonged intubation due to benzodiazepine overdose in the first trimester of pregnancy. The patient was managed with three dilatations; however, the improvement was only transitory, and they considered it necessary to perform a tracheal resection. Unlike the patients in the current report, the authors used general anesthesia with neuromuscular relaxation and endotracheal intubation with a number 5.5 tube; the patient was extubated at the end of the procedure. Similar to the second case reported herein, the patient had a follow-up bronchoscopy with a good surgical outcome and was discharged seven days after surgery. Both results suggest that laryngotracheal resection and reconstruction are effective treatment options in pregnant patients.
Spontaneous ventilation in pregnant patients with this diagnosis has been described in three case reports (5-7). Ratner et al. (5) published an article in 2001 describing a patient at 32 weeks of gestation who underwent laryngoscopy, bronchoscopy, and tracheal biopsy after induction with sevoflurane on spontaneous ventilation. However, Ratner et al. only used spontaneous ventilation for induction; succinylcholine and rocuronium were used after the patient lost consciousness. In 2008, Scholz et al. (6) published a case report of a patient at 29 weeks of gestation who underwent laser resection and for whom total intravenous anesthesia was used without intubation. Scholz et al. reported that the anesthesia passed without eventualities, the airway device was a nasal route, and topicalization with lidocaine was performed. Scholz et al. did not describe the dose, type of device, or ventilatory management during the procedure (6). In the same year (2008), Parsa et al. (7) published an article describing a patient at 31 weeks of gestation who underwent bronchoscopy for dilatation and laser resection. Parsa et al. (7) used halothane by face mask to preserve ventilation and, after starting dilatation, discontinued halothane, started remifentanil infusion and switched to controlled ventilation. The results of the current case report add to previously described case reports as evidence of the successful use of spontaneous ventilation in pregnant patients with tracheal stenosis.
It is essential to highlight using a high-flow nasal cannula oxygenation system and spontaneous ventilation. The use of a high-flow nasal cannula guarantees the oxygenation of an individual even when apnea is present due to the principle of aventilatory mass flow. This principle explains that when there is a high flow of oxygen to the upper airway and since oxygen diffuses more rapidly than CO2 in the alveoli, a negative pressure gradient between the upper airway and the alveoli occurs, this gradient generates a flow of gases from the point of higher pressure to the point of lower pressure (8). However, a disadvantage of this principle might be the low excretion of CO2, leading to the accumulation of this gas in the blood and the presence of respiratory acidosis. Contrary to expectations, there was no elevation of arterial PaCO2 above 45 mmHg in our patients due to spontaneuos ventilation. Using a high-flow nasal cannula in this type of patient avoids airway manipulation, which can be associated with edema and bleeding more frequently than in the general population. Additionally, the absence of an endotracheal tube allows for a free surgical field, thereby reducing surgery duration.
3.1. Conclusions
The current two cases add to the growing evidence on the successful use of high-flow nasal cannula with spontaneous ventilation in tracheal surgery. These are the first reported cases of this technique in pregnant patients taken to laryngotracheal reconstruction. The results of the patients in this report seem to suggest that it is a safe technique for both the pregnant woman and the fetus, decreases airway manipulation, optimizes the surgical field, and maintains adequate ventilation.