1. Introduction
PHN (postherpetic neuralgia) is associated with severe neuropathic pain syndrome. It can impair the quality of life of the patients, and may have serious effects on medical services and society (1, 2). The neuropathic pain is defined as “pain arising as a direct consequence of a lesion or disease affecting the somatosensory system”. The neuropathic pain is characterized by spontaneous ongoing or shooting pain and evoked amplified pain responses after noxious or non-noxious stimuli (3). PHN is caused by degeneration and destruction of the motor and sensory nerves as the neuron in the dorsal root ganglion (DRG) is injured or necrotized; however, the exact mechanism of pain is unknown. The treatment of PHN can include pharmacotherapy and interventional therapy. The 1st line pharmacotherapy of PHN comprises tricyclic antidepressants (TCAs), antiepileptics, and topical lidocaine. Opioids and tramadol are considered as 2nd line pharmacotherapy, while topical capsaicin and valproate are in 3rd line treatment. Interventional therapies such as sympathetic and epidural block, intrathecal injections, pulsed radiofrequency (PRF), spinal cord stimulation, and invasive surgical procedure are also considered for PHN treatment (4-6). Although several therapeutic options are known, still there are no precise therapeutic options and this causes difficulties (4-7). Watson et al. (6) demonstrated that at least 30% of PHN patients show refractory or unsatisfactory relief of pain. Hence, this study was performed on patients with intractable PHN, who had not responded to the standard treatments and had an uncontrollable anterior abdominal pain. We performed a transversus abdominis plane (TAP) block to reduce the dose of medication and enable effective pain control.
2. Case Presentation
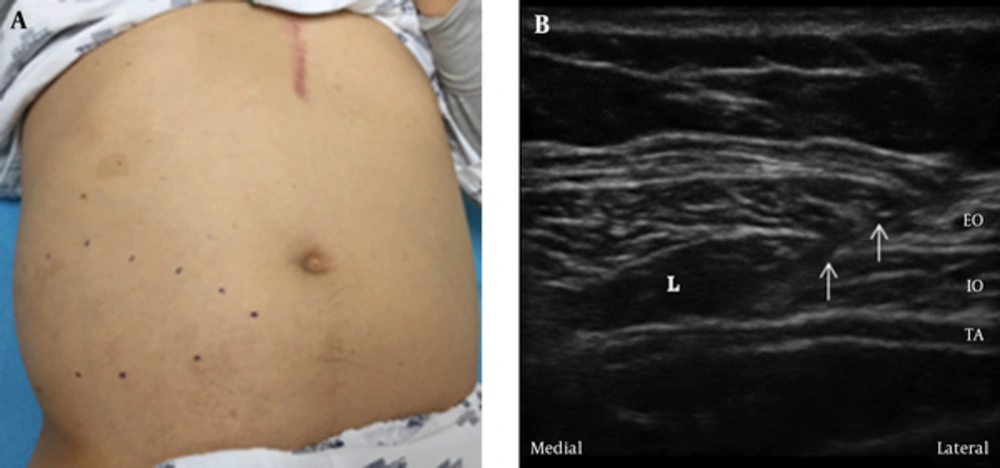
The TAP block was performed as follows. After sterile prep and draping, TAP block was performed under ultrasound (SonoSite M turbo, SonoSite, Inc., Bothell, WA, USA) guidance using a linear ultrasound probe placed in the midaxillary line in a transverse plane to the lateral abdominal wall between the lower costal margin and the highest point of iliac crest. A 22-gauge Quincke needle was advanced until it reached the plane between the internal oblique and transversus abdominis muscles (Figure 1A). After negative aspiration, 10 mL of 1% lidocaine was injected in this plane and then the needle was removed (8). The patients’ pain intensity was measured based on the NRS (numerical rating scale), where 0 = no pain and 10 = worst possible pain. The NRS is a standard instrument and represents the degree of clinical improvement in chronic pain (9).
2.1. Case 1
The first case was a 59-year-old and 75 kg weighted male patient who was diagnosed with PHN in the right T9-11 dermatomes 4 years ago and he was taking gabapentin 900 mg, acetaminophen 650 mg tid, pregabalin 300 mg bid, and prednisolone 5 mg qd. He was treated 3 years ago with right thoracic epidural steroid injections (T-ESI), T9-11 root block (RB), T11, T12 PRF, and intercostal nerve block; the pain was controlled by medication for 2 years. But, he complained of aching pain and allodynia again in spite of taking same dose of medications; when visiting pain clinic, the NRS was 8. The patient had a medical history of diabetes mellitus, and was taking warfarin 10 mg qd after undergoing prosthetic valve surgery 23 years ago. The most severe painful area was on the right side of the umbilicus (Figure 1B). Considering the patient was taking warfarin, he was hospitalized for heparin bridging therapy and a TAP block was performed. His international normalized ratio (INR) was 2.16 before performing TAP block. After bridging therapy with low molecular weighted heparin (LMWH), at first block, INR was 1.59. After the TAP block, the NRS of 1 was maintained during hospitalization. Two weeks after discharge, the NRS increased to 3 under taking reduced dose of medication (gabapentin 900 mg tid alone), but the satisfaction level of the patient with respect to the treatment was deemed to be “very satisfactory” according to a four-point Likert scale (unsatisfactory/normal/satisfactory/very satisfactory), which was higher than that with other treatments (i.e., “normal”). Six months after discharge, the NRS was maintained as the same.
2.2. Case 2
The second case was a 43-year-old male patient weighted 70 kg who was diagnosed with PHN 1 year ago in right T12, L1 dermatomes leading to hospitalization. He was taking pregabalin 150 mg, nortriptyline 10mg, tramadol 75 mg, and acetaminophen 650 mg bid. Several months ago (prior to this admission), T-ESI, T12, L1 RB and T12, L1 PRF had been applied twice leading to disappeared burning and aching pain, but the patient complained of allodynia and hyperalgesia with NRS 7. The main painful area was below the umbilicus on the right side and near the iliac crest; therefore, a right TAP block was performed. We performed a total number of 5 blocks in an interval of one week. At an early stage, the analgesia persisted for one or two days. After that, the duration of pain relief gradually increased, and while the sensation was maintained, allodynia and hyperalgesia disappeared. The medication was changed to pregabalin 150 mg bid. One month after the treatment, the NRS was 3; hence, the medication was stopped.
3. Discussion
The TAP block involves injection of local anesthetics into the interfascial plane between the internal oblique and transversus abdominis muscles. The method of using an anatomical landmark was introduced in the past by Rafi. However, the technique was modified because of the development of ultrasound which is commonly used (10-12). The TAP block is a treatment option that is mostly used to control the postoperative pain after laparoscopic surgery as well as open abdominal surgery. Additionally, there are case reports suggesting that the TAP block not only is useful in acute pain, but also in postsurgical pain or cancer pain. However, there are no reports on the treatment of PHN with ultrasound-guided TAP block indicating that it is an easy and safe treatment. The toxicity of local anesthetics and injection in wrong structures such as vessel or peritoneum are some drawbacks of TAP block. However, using ultrasound can lead to the decreased volume of local anesthetics and the injection into appropriate anatomical structure (10).
In some PHN cases, the main route for pain is known to be damaged abnormal functioning or sensitized cutaneous nerve endings that send increased nociceptive stimuli to the dorsal horn of the spinal cord. The use of local anesthetics to control the pain of PHN has a history dating back to the report by Watson and Oaklander (6). Damaged and regenerating nerve endings can express changes in the number and location of sodium channels, the target of local anesthetic drugs. A damaged peripheral nerve is particularly susceptible to local anesthetics, so that abnormal tonic evoked and ectopic activity is suppressed by local anesthetic concentration far below that required to block nerve impulse conduction (6). As the region of pain in the patients described in this case report was limited to anterior abdominal area rather than the band shape, a TAP block was considered. Because the local anesthetics acted via the cutaneous nerve ending of abdominal wall, a TAP block is thought to show unexpectedly a long-lasting therapeutic effect. Furthermore, PHN causes damage to all sensory nerve groups (C, Aδ, and Aβ fibers) and results in a sharp and burning pain, and also allodynia and hypersensitivity (13). A TAP block is known to block the motor and sensory nerves of the anterior abdominal wall; thus, it is effective in relieving the sharp and burning pain, allodynia, and hypersensitivity of the anterior abdominal wall. PHN is known to start from the lesion in one segment on the DRG, but over chronic duration, the peripheral DRG changes and extends to the upper and lower segments (13). Rather than performing RB at several levels, the TAP block has an advantage of controlling the abdominal wall pain at several levels. TAP block in the midaxillary line is known to block the nerve part extending from T7/8 to L1 (8, 14). However, the conventional TAP block was extended to T9-T10 in the first case, which we believe that it can be attributed to the patient’s anatomical variation (15). There is a direct association in the frequency and level of pain with age in patients with PHN (16), and if the patient is elderly, there might be several underlying diseases; however, there are many kinds of antithrombotic and antiplatelet medications to control these underlying diseases. In patients taking antithrombotic and antiplatelet medications, the medication must be stopped for a certain period of time prior to neuraxial block, and in high-risk patients, bridging therapy might be required. Also, hospitalization may be required for performing the neuraxial block and the risk of complications is high before and after the neuraxial block (17). However, TAP is a plane block that involves injection of the drug between the spaces in the abdominal wall; thus, it has the advantage of being well-suited for patients taking antithrombotic and antiplatelet drugs, and it is relatively safer than the deep peripheral block or neuraxial block.
3.1. Conclusion
The TAP block seems to be an alternative for patients with PHN who suffer from anterior abdominal wall pain accompanied by allodynia and hyperalgesia, and do not respond to the existing conservative treatment and medication, or those who have a low response to interventional therapies such as RB and PRF, especially those undergoing anticoagulation therapy.