1. Introduction
One-lung ventilation (OLV) is increasingly performed in thoracic surgeries to prevent soiling from the contralateral lung and provides the surgeon with a better view. Double-lumen endobronchial tubes (DLTs), bronchial blockers (BBs), and single-lumen endobronchial tubes, which have been increasingly used in recent years (1, 2), are standard methods for lung isolation procedures. However, the size and weight of DLTs can cause trauma to the tracheostomy stoma in patients with tracheostomy; thus, BBs and Fogarty catheters are considered as better options for these patients (3, 4). Because airway management, particularly OLV, is unusual in patients with tracheostomy, there is limited information about this topic in the literature. In this case study, a new method was used when two separate small-sized tubes were inserted by using a fiberoptic bronchoscope. Thus, this method can be used for bilateral ventilation, proper suction, and lung isolation in specific cases or in the absence of certain equipment.
2. Case Presentation
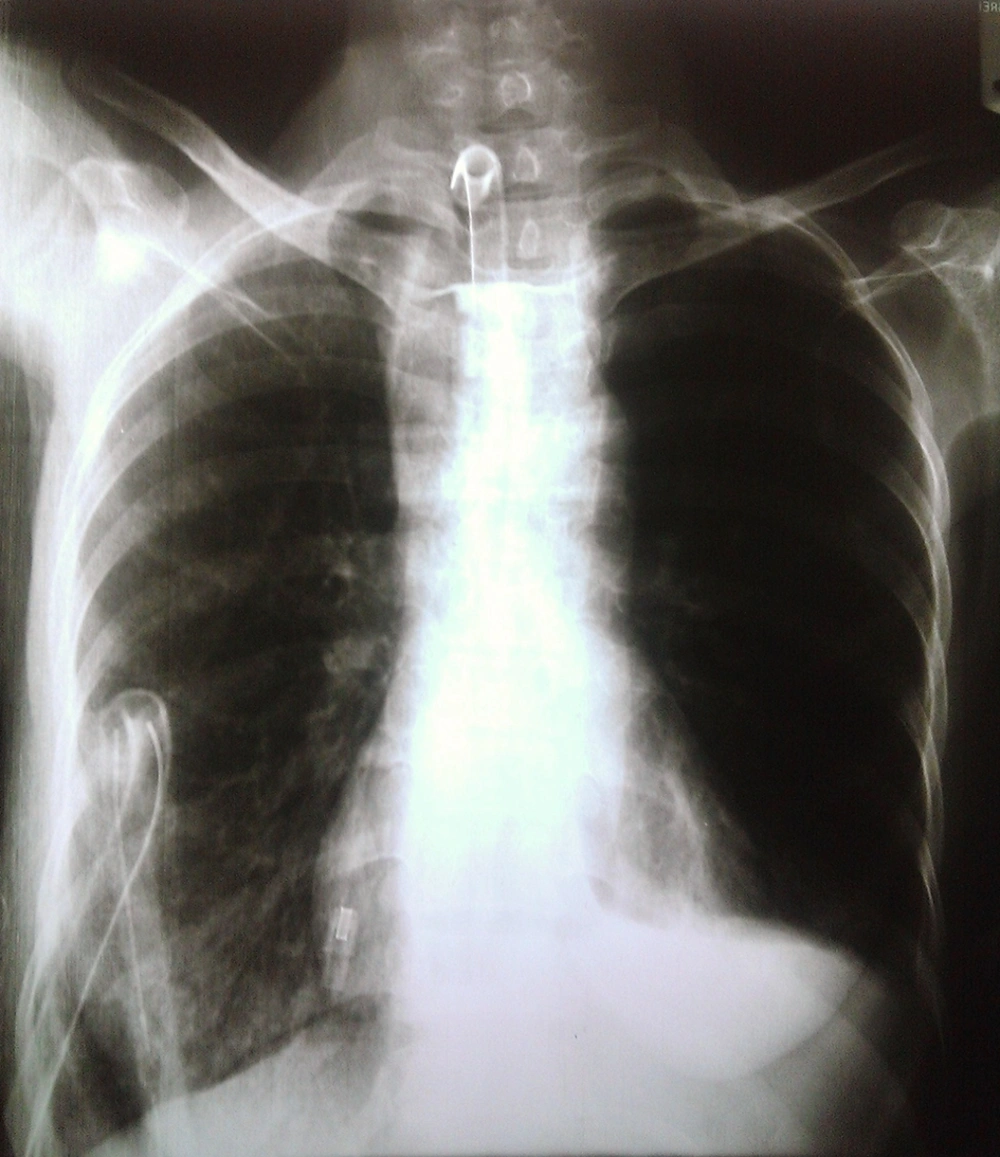
A 41-year-old woman with advanced esophageal cancer who underwent pharyngo–laryngo–oesophagectomy (PLO) 21 days ago was selected for thoracic duct ligation because of chylothorax. She received radiotherapy 8 times and chemotherapy 3 times before PLO, as well as she had a right chest tube with lymphatic secretions, and a jejunostomy feeding tube. Blood tests showed that the patient had hypocalcemia and hypoalbuminemia. ECG revealed a reversed T wave in leads I, II, and aVF and a long-QT interval. In addition, arterial blood gas values were PH = 7.35, PCO2 = 45 mmHg, HCO3 = 25 mEq/L, PO2 = 88 mmHg, and SaO2 = 92%. Chest X-ray showed that the left costophrenic angle was obscured with an infiltration pattern in the right lower lobe (Figure 1).
Because of improper hygiene, tracheostomy stump was almost occluded and the patient presented with mild respiratory distress, tachypnea with hyperactivity of the accessory muscles. The patient was conscious, but weak. She weighed 42 kg, and before induction, her vital signs were RR = 18, BP = 90/62 mm Hg, HR = 94 bpm, T = 37°C, and SpO2 = 91%. Initially, intravenous access was established for the patient using two 20-gauge catheters and underwent standard monitoring. She was infused with 500 mL saline. A green 14 French suction tube was inserted in the trachea to examine the tracheotomy, and suction the excessive secretions. One milligram midazolam, 150 μg fentanyl and 80 mg propofol were slowly injected, and 100 μg/kg/min propofol was infused.
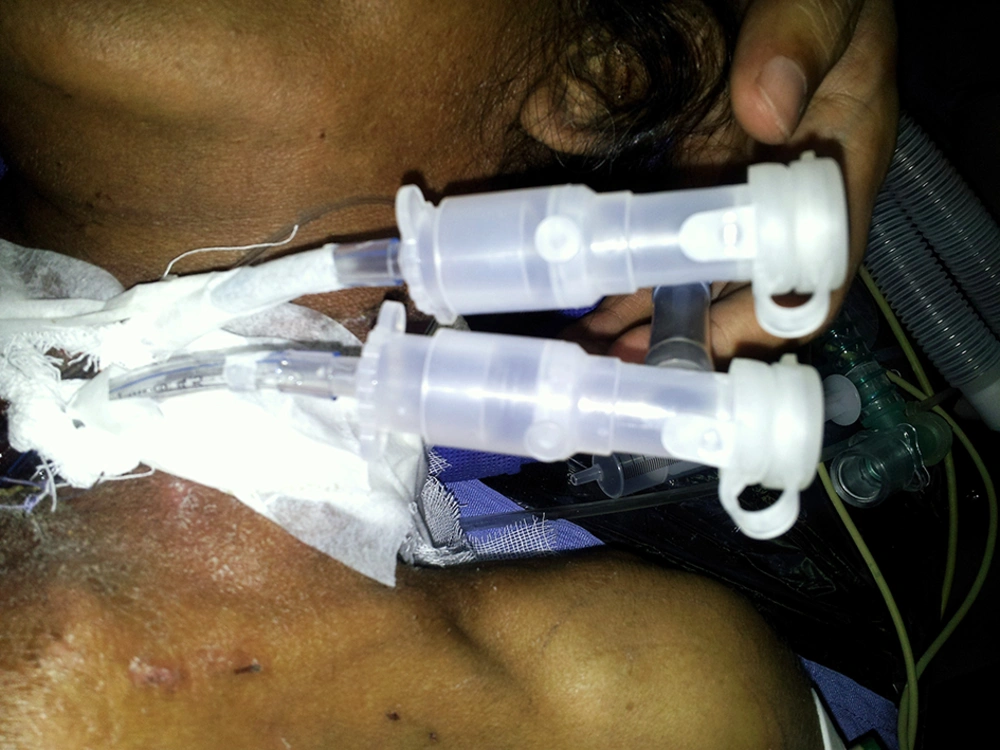
After the patient was anesthetized, a cuffed tracheal tube number 4.5 (internal diameter of 4.5 mm and external diameter of 6.2 mm) was inserted from a narrow tracheostomy tube and fixed in the trachea. The cuff was filled, then 20 mg atracurium was injected, and the patient was ventilated manually. Next, the cuff deflated and by a narrow child-sized fiberoptic bronchoscope, the tracheal tube was directed to the right bronchus. After pulmonary ventilation of the right lung was confirmed, another 4.5 cuffed tube was slowly inserted through the tracheostomy; this caused minor trauma and mild bleeding. Then the tube was directed to the left bronchus, the cuff was inflated, and ventilation of the left lung was verified. Both lungs were ventilated via a Y-piece connection (Figure 2), and a leak test was applied to ensure that no air leaked out of the lungs.
Approximately 10 minutes after the insertion of the tracheal tube, oxygenation remained stable and the vital signs were as follows: BP = 110/78 mm Hg, HR = 94 bpm, SpO2 = 96%–98%. After the bronchial tubes were inserted, the end-tidal CO2 was monitored, and a catheter was embedded on the left radial artery for invasive monitoring of BP. The patient was ventilated mechanically with F = 10 breaths per minute, Vt = 420 mL, and also 50% O2/N2O, then thoracic surgery began. After thoracic incision, the patient was given 100% O2, the right-sided tracheal tube was clamped, and the right lung was collapsed. Ventilation parameters were set again (F = 15, Vt = 300, PEEP = 3 mm Hg) with measuring and controlling of ETCo2.
The surgery lasted for 3.5 hours and during this time, there was not a significant hemodynamic change (BP = 90-132/60-82 mm Hg, HR = 88-142 bpm, ETCo2 = 30-42 mm Hg) and peripheral oxygenation was preserved between 91%- 93%. One hour after bronchus clamp, arterial gas was PH = 7.32, PCO2 = 42 mmHg, Hco3 = 19.2 mEq/L, PO2 = 88 mm Hg. After the thorax was closed; the bronchus was suctioned and first the patient was ventilated manually with high inspiratory pressure and then mechanically with F = 12, Vt = 400 ml; then tracheal tubes were removed. A 65 mm tracheostomy tube was placed, and atropine, neostigmine, and 60 mg lidocaine were injected.
The patient was transferred to the recovery room while she was conscious and her vital signs in the recovery room were BP = 90/60 mm Hg, HR = 140 bpm, SpO2 = 96%-98%. One-hour later, the patient was transferred to the intensive care unit, and her arterial blood gas values were PH = 7.28, PCO2 = 36.5 mmHg, HCO3 = 17.3 mEq/L, PaO2 = 124 mm Hg, and SaO2 = 96%.
3. Discussion
In thoracic surgeries, lung isolation is sometimes a necessary technique. OLV can be accomplished by using DLTs, BBs, or single-lumen endobronchial tubes; however, previous studies have not shown a specific preference and there was no exclusive choice between BB and DLT in patients' tracheostomy. Use of double-lumen tubes instead of single-lumen, and BBs have not been approved in children, patients with airway problems, or with tracheostomy (5). However, Coe et al. have shown that DLT has been used in patients with tracheostomy (6). Furthermore, Leinbakh Yaney used a double-lumen tube for a patient with a fresh tracheostomy that was a candidate for esophagectomy and underwent ventilation for 4 hours (7).
In recent years, it has been increasingly suggested that BBs be used in patients with airway problems and patients with tracheostomy (1, 2, 6). However, several complications such as BB displacement, dislodging BB tip, blockage of the airway, and collapse of the upper right lobe have been reported (8). In this study, a DLT tube was not used because of its long length, a narrow tracheostomy stoma, trauma probability, and bleeding. Also, the probability of a prolonged surgery, stomal stenosis, trauma, and the rare complications associated with BBs such as displacement, blockage of the airway, and inaccessibility to appropriate BB and a univent type BB prevented us to use it.
Instead, a new method was used in this study that involved the insertion of two tracheal tubes for one-lung ventilation. Two cuffed tracheal tubes (4.5 mm internal diameter) were inserted in the right and left lungs using a fiberoptic bronchoscope. After the isolation, the right lung was collapsed. At the end of surgery, all the lung tissues, including the upper lobe, were ventilated and the patient did not have any pulmonary complications. In certain cases and inaccessibility to appropriate device, lung isolation may be performed using this method. The only limitation for this method is the need for child-sized fiberoptic bronchoscope.