1. Background
Currently, laparoscopy is the technique of choice for living kidney donors. Laparoscopy is best to reduce the incidence of postoperative pain (1). Good postoperative pain management is essential to reduce anxiety, sleeping disturbances, mental disturbances, infection, and social issues, hence, preventing a prolonged hospital stay.
Using effective analgesia may decrease morbidity and mortality due to immune system problems, such as infection, delayed wound healing, and sepsis. Living kidney donors are often healthy people; therefore, optimal pain management is essential to have a short recovery period (2-4). In Cipto Mangunkusumo Hospital in Jakarta, Indonesia, the continuous epidural blockade is the standard postoperative management for living kidney donors. However, this technique is limited to patients with no coagulopathy issues with numbness and tingling sensation as its side effects. Additionally, patients undergoing epidural blockade might require longer urinary catheter duration and mobilization period.
Blanco first introduced quadratus lumborum blockade (QL block) in 2007 and found it effective in cesarean sections (5, 6). Further studies proved QL block as an effective, safe postoperative pain management technique for abdominal surgery (7-9). This technique is an alternative to the epidural blockade to decrease intraoperative stress response among living kidney donors.
Intraoperative stress response could be measured by inflammatory mediators, such as interleukin-6 (IL-6), interleukin-10 (IL-10), C-reactive protein (CRP), and tumor necrotizing factor-α. Based on the literature, IL-6 is the most sensitive marker to represent surgical stress responses. The release of IL-6 might indicate an acute stress response. This protein in the acute stress response might play the role of an inflammatory mediator, anti-proteinase, and wound healing agent. Meanwhile, CRP is often linked with pain transmission and inflammation postoperatively. CRP concentration increases within 4-6 hours after stimuli, such as incision, and reach its peak within 48 - 72 hours. Therefore, both IL-6 and CRP might represent stress response following surgery (2, 10).
2. Objectives
This study aimed to compare IL-6 and CRP concentrations between QL and epidural blocks among living kidney donors.
3. Methods
This randomized clinical trial was conducted among living kidney donors in Cipto Mangunkusumo Hospital in Jakarta, Indonesia from May to December 2018. The inclusion criteria were living kidney donors undergoing laparoscopic surgery, signing the informed consent form, and having a body mass index of less than 30 kg/m2. The exclusion criterion was a history of an allergic reaction to local anesthetic agents, including anaphylactic shock and cardiac arrest. The drop-out criteria included patients with failed epidural insertion or QL block and those who had intraoperative problems, such as severe hypotension and bleeding. Ethical clearance for this study was obtained from the Ethics Committee of the Faculty of Medicine Universitas Indonesia (0211/UN2.F1/ETIK/2018). This study was registered at ClinicalTrials.gov (NCT03520205).
Randomization was conducted through www.randomizer.org with the first group receiving the continuous epidural block and the second group receiving QL block as intraoperative and postoperative analgesia techniques. There were 31 patients for each group. Preoperatively, all patients received education regarding the type of intervention they would receive, how to use the numeric rating scale (NRS) for pain, and how to operate patient controlled analgesia (PCA). All patients underwent general anesthesia with endotracheal intubation. Anesthetic maintenance was done using Sevoflurane, oxygen, and compressed air.
The control group utilized continuous epidural block with epidural insertion in the left lateral decubitus position after intubation under general anesthesia. The epidural catheter was inserted in the vertebral interspace Th11-Th12 and catheter was advanced 4 - 6 cm in length within the epidural space. The position was confirmed using the aspiration technique and administering the test dose (3 mL of bupivacaine 0.25% and 1:200,000 epinephrine). The regimen was bupivacaine 0.25% at the speed of 6 mL/hour.
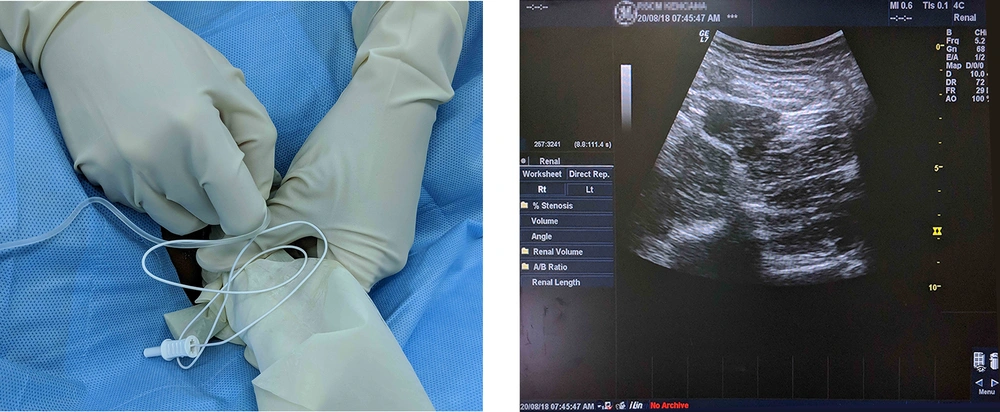
The other group received bilateral QL block after general anesthesia. The QL block was conducted with anterior approach guided by ultrasound (Figure 1). Patients were in the lateral position with the site of the block facing upward by a pillow underneath it and table tilting. After ensuring skin asepsis of the site, a 2.0 - 5.5 MHz convex transducer (4C-RS, Logic E, GE Healthcare, USA; C5-1E, DC-70, Mindray, Shenzen, China) covered with sterile drapes was vertically attached above the iliac crest. After QL and major psoas muscles were identified, Contiplex® was inserted 1 - 2 cm away from the probe. One mL of NaCl 0.9% was injected for hydrodissection; then, 20 mL of bupivacaine 0.25% was injected through the catheter until the anterolateral part of QL muscle was surrounded by the local anesthetic agent.
At the end of the surgery, subjects in the epidural group received bupivacaine 0.125% with the speed of 6 mL/hour for 24 hours postoperatively and subjects in the QL block group received bupivacaine 0.25% with a total volume of 20 mL before the catheter was discarded. Blood tests were conducted directly after surgery and 24 hours postoperatively. PCA morphine was set with a bolus dose of 1 mg, lockout time of 10 minutes, and a maximal dose of 6 mg. The amount of PCA morphine use in the first 24 hours was recorded. Pain scores at rest and movement were recorded using the NRS at 2, 6, 12, and 24 hours postoperatively. Motor ability was measured using the Bromage score within 24 hours. Any side effects such as nausea, vomiting, and paresthesia were noted within 24 hours postoperatively.
Data analysis was conducted by statistical package for social sciences (SPSS) program with unpaired t-test for normally distributed numerical variables, Mann-Whitney test for non-normally distributed data, and the general linear model test for multivariate analysis. Normally distributed data were displayed as means and standard deviation while data with non-normal distribution were expressed as median with minimal and maximal values. The P values of < 0.05 showed statistically significant differences.
4. Results
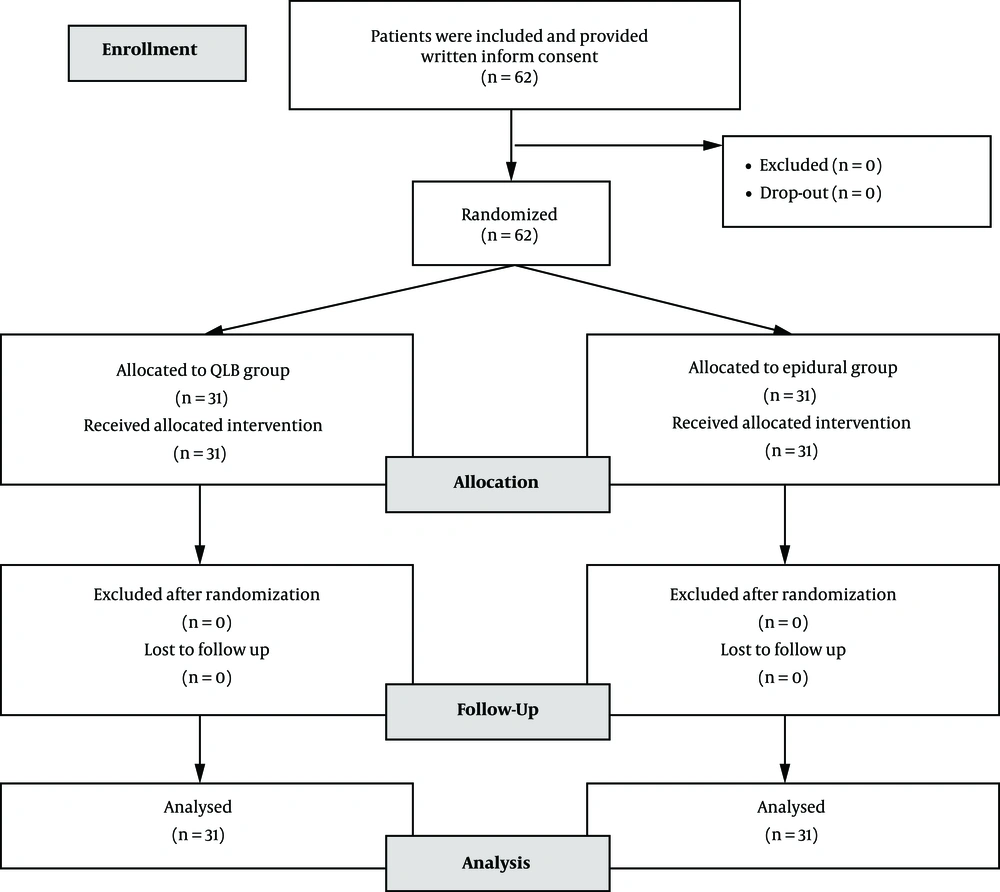
The subject selection process is shown in Figure 2. The demographic characteristics of patients in continuous epidural and QL block groups are shown in Table 1. Comparable characteristics were found between the two groups.
| Variables | Epidural Block Group (N = 31) | QL Block Group (N = 31) |
|---|---|---|
| Sex, No. (%) | ||
| Male | 20 (64.51) | 21 (67.74) |
| Female | 11 (35.49) | 10 (32.26) |
| Age, y | 36 (23 - 66) | 35 (22 - 68) |
| Body weight, kg | 62.72 ± 10.06 | 64.34 ± 10.10 |
| Body height, cm | 162 (140 - 183) | 165 (148 - 180) |
| BMI, kg/m2 | 24.13 ± 4.06 | 24.06 ± 3.82 |
| ASA, No. (%) | ||
| ASA 1 | 20 (64.51) | 18 (58.06) |
| ASA 2 | 11 (35.49) | 13 (41.94) |
| Surgical duration, h | 4,75 (4 - 6) | 4,5 (4 - 6) |
| Anesthesia duration, h | 6 (5 - 7.25) | 6 (5 - 7.25) |
The IL-6 concentration directly after surgery and 24 hours postoperatively did not show significant differences between the groups although the IL-6 concentration 24 hours postoperatively was slightly higher in the epidural group than in the QL group (Table 2).
| Time | Mean (95% CI) | P Valueb | Mean Difference (Upper - Lower 95% CI) | P Valuec | |
|---|---|---|---|---|---|
| Epidural Block (N = 31) | QL Block (N = 31) | ||||
| Interleukin-6 | 0.454 | ||||
| Preoperative | 1.89 (1.63 - 2.20) | 2.06 (1.72 - 2.46) | 0.459 | 1.11 (0.86 - 1.36) | |
| Postoperative | 35.32 (28.39 - 43.66) | 36.66 (29.58 - 45.44) | 0.785 | 1.04 (0.77 - 1.40) | |
| 24 hours postoperatively | 52.82 (41.36 - 67.45) | 45.98 (38.15 - 55.41) | 0.361 | 0.87 (0.64 - 1.17) | |
| C-reactive protein | 0.201 | ||||
| Preoperative | 1.60 (1.15 - 2.22) | 1.93 (1.28 - 2.92) | 0.466 | 0.82 (0.49 - 1.38) | |
| Postoperative | 1.80 (1.30 - 2.49) | 1.70 (1.20 - 2.40) | 0.805 | 1,05 (0.66 - 1.68) | |
| 48 hours postoperatively | 108.76 (95.12 - 124.36) | 99.08 (67.99 - 144.37) | 0.636 | 1.09 (0.74 - 1.62) | |
aData served as geometric data.
bUnpaired t-test, significant at P < 0.05.
cGeneral linear model test, significant at P < 0.05.
Similarly, the CRP concentration did not show significant differences between the two groups. The changes in the CRP concentrations did not differ significantly, as well (Table 2).
The pain score at rest and during movement did not show significant differences between the epidural and QL block groups (Table 3). Similarly, morphine requirement was not different between the epidural and QL block groups (Table 3).
| Time | Median (Minimum - Maximum) | P Valuea | |
|---|---|---|---|
| QL Block (N = 31) | Continuous Epidural Block (N = 31) | ||
| NRS at rest | |||
| At recovery room | 1 (0 - 5) | 2 (0 - 7) | 0.313 |
| Two hours postoperatively | 2 (0 - 5) | 2 (0 - 6) | 0.785 |
| Six hours postoperatively | 1 (0 - 5) | 2 (0 - 4) | 0.708 |
| Twelve hours postoperatively | 2 (1 - 6) | 2 (0 - 5) | 0.659 |
| Twenty four hours postoperatively | 2 (0 - 4) | 2 (0 - 5) | 0.878 |
| NRS during movement | |||
| At recovery room | 3 (0 - 6) | 3 (0 - 8) | 0.617 |
| Two hours postoperatively | 3 (0 - 6) | 3 (1 - 7) | 0.863 |
| Six hours postoperatively | 3 (1 - 6) | 3 (1 - 6) | 0.868 |
| Twelve hours Postoperatively | 3 (2 - 8) | 3 (1 - 6) | 0.895 |
| Twenty four hours Postoperatively | 3 (1 - 5) | 3 (1 - 6) | 0.873 |
| Morphine requirement postoperatively | |||
| Two hours postoperatively | 0 (0 - 3) | 0 (0 - 4) | 0.857 |
| Six hours postoperatively | 1 (0 - 6) | 1 (0 - 6) | 0.764 |
| Twelve hours postoperatively | 1 (0 - 8) | 1 (0 - 6) | 0.750 |
| Twenty four hours postoperatively | 1 (0 - 10) | 1 (0 - 5) | 0.965 |
aMann-Whitney test, significant at P < 0.05.
5. Discussion
Optimal postoperative pain management is essential for all patients undergoing surgery. Good pain management may create comfort during the recovery period (11). This study compared IL-6 and CRP as the main parameters of stress response between continuous epidural and QL block among living kidney donors. There were 31 subjects in each group. Demographic data showed no significant difference between the two groups. In order to limit a large biometric variation, the study recruited only patients with a BMI of less than 30 kg/m2. Surgical duration, bleeding, and the position were considered as non-confounding factors since all subjects underwent a similar technique.
Laparoscopic nephrectomy generates extra intra-abdominal pressure, which, in turn, creates pressure in the inferior vena cava. This will lead to decreased preload followed by reduced stroke volume and cardiac output. The compensation for decreased cardiac output includes the release of stress hormones, such as catecholamines. These agents will increase systemic vascular resistance, heart rate, and cardiac contractility (12). However, epidural block inhibits the sympathetic nervous system, hence reducing pain and temperature sensation. Epidural block also inhibits the motoric aspect. If the epidural block is conducted in the thoracal section, this effect will be amplified, especially with the sympathetic block. Bradycardia and hypotension due to vein dilation and pooling are commonly found (13, 14).
IL-6 as a pro-inflammatory and anti-inflammatory mediator increases in traumas, burns, and sepsis condition. It also increases following surgical traumas and increases the risk of postoperative complications, including infections. The current study found that the IL-6 concentration was not significantly different between the epidural and QL block groups. However, its concentration 24 hours postoperatively was higher in the epidural block than in the QL block group. This finding might be due to that the analgesic effect of epidural block inhibited the sympathetic response, thus, decreasing the release of catecholamines. Additionally, in the QL block group, the distribution of local anesthetic might spread to incision parts to suppress the sympathetic response.
Kvarnstrom et al. and Li et al. showed that laparoscopic surgery led to lower levels of stress response mediators, such as IL-6, than conventional open surgery (15, 16). However, Almagor et al. found contradictory results indicating that the postoperative stress response in open appendectomy and laparoscopic appendectomy was not reflected by the IL-6 concentration. The current study did not find any significant difference in the IL-6 concentration between the two intervention groups. Both epidural and QL block showed similar analgesic properties in terms of IL-6 concentration among living kidney donors.
CRP concentration increases in response to increasing IL-6 concentration in the plasma. This is in accordance with the acute phase response during surgical traumas (15, 16). This study found no significant difference in terms of CRP concentration between subjects undergoing epidural block and QL block. However, Kvarnstrom et al. and Li et al. found significant differences in terms of CRP concentration between patients undergoing laparoscopic surgery and conventional surgery (15, 16). IL-6 stimulates hepatocyte to release CRP; hence, since there was no significant increase in the IL-6 concentration in this study, no significant increase was observed in the CRP concentration, as well.
Pain intensity was measured in this study using the NRS at rest and movement. This study found no significant difference in terms of pain score at rest and movement between subjects in the epidural and QL block groups at any time-point. Ishio et al. reported that QL block was associated with a low NRS score within 24 hours postoperatively (17). Meanwhile, another study found no pain at rest and movement within 24 hours postoperatively among patients undergoing partial laparoscopic nephrectomy with a continuous epidural regimen with Ropivacaine 0.2% (12). Therefore, both continuous epidural and QL block had comparable analgesic properties for postoperative pain management.
Similar analgesic properties of both interventions might be due to the spread of local anesthetic agent to cover the incision location. The largest incision area was Pfannenstiel incision located in the lower abdominal area and the other surgical field consisted of Th8-L1 dermatomes for trochar insertions (13, 14). Both epidural and QL block covered a similar area of surgery; hence, there was no difference in terms of analgesic properties. This finding was reflected in morphine requirement between the two groups such that no significant difference in morphine requirement was seen at all times between epidural and QL block groups.
This study has several limitations; it did not measure the CRP concentration at the first 24 hours; so, there was no linearity between CRP and IL-6 concentrations at that time. Further study should measure both markers at similar times in order to determine the linearity.
5.1. Conclusions
There was no significant difference in IL-6 and CRP concentrations between continuous epidural and QL block among living kidney donors. Both continuous epidural and QL block techniques showed comparable postoperative analgesic properties among living kidney donors undergoing laparoscopic nephrectomy.