1. Background
2. Objectives
3. Methods
3.1. Statistical Analysis
4. Results
| Variables | EVDs Infection | P-Value | OR (95% CI) | |
|---|---|---|---|---|
| Yes | No | |||
| Sex | 39 (48.1) | 42 (51.9) | 0.1 | 2 (0.76 - 5.76) |
| Male | 25 (55.6) | 20 (44.4) | ||
| Female (reference) | 14 (38.9) | 22 (61.1) | ||
| Age | 44.33 ± 19.5 | 44.88 ± 20.57 | 0.9 | 1.7 (0.9 - 4.2) |
| Diagnosis | 0.3 | 0.7 (0.3 - 1.85) | ||
| Vascular | 23 (46.9) | 26 (53.1) | 0.4 (0.2 - 3.23) | |
| Brain tumor | 11 (47.8) | 12 (52.2) | 0.5 (0.4 - 1.45) | |
| Shunt and malformation (reference) | 5 (55.6) | 4 (44.4) | ||
| Past medical history | 0.8 | |||
| Diabetes (DM) | 2.9 (0.7 - 7.37) | |||
| Yes | 6 (50) | 6 (50) | ||
| No (reference) | 33 (47.8) | 36 (52.2) | ||
| Hypertension (HTN) | 0.3 | 0.6 (0.1 - 2.4) | ||
| Yes | 7 (389) | 11 (61.1) | ||
| No (reference) | 32 (50.8) | 31 (49.2) | ||
| Hyperlipidemia (HLP) | 0.1 | 0.7 (0.1 - 3.4) | ||
| Yes | 0 (0) | 2 (100) | ||
| No (reference) | 39 (49.4) | 40 (50.6) | ||
| Ischemic heart disease (IHD) | 0.1 | 0.3 (0.02 - 3.08) | ||
| Yes | 1 (20) | 4 (80) | ||
| No (reference) | 38 (50) | 38 (50) | ||
| Cerebrovascular attack (CVA) | 0.4 | 0.5 (0.07 - 3.71) | ||
| Yes | 2 (28.6) | 5 (71.4) | ||
| No (reference) | 37 (50) | 37 (50) | ||
| APACHE II score | 0.4 | 0.9 (0.1 - 1.5) | ||
| 0 - 15 | 13 (40.6) | 19 (59.4) | 0.8 (0.41 - 1.73) | |
| 16 - 19 | 12 (57.1) | 9 (42.9) | ||
| 20 - 30 (reference) | 14 (50) | 14 (50) | 0.6 (0.3 - 2.43) | |
| Number of EVD | 0.3 | |||
| One time | 35 (89.7) | 38 (90.5) | 0.8 (0.3 - 4.2) | |
| More than one time (reference) | 4 (10.3) | 4 (9.5) | ||
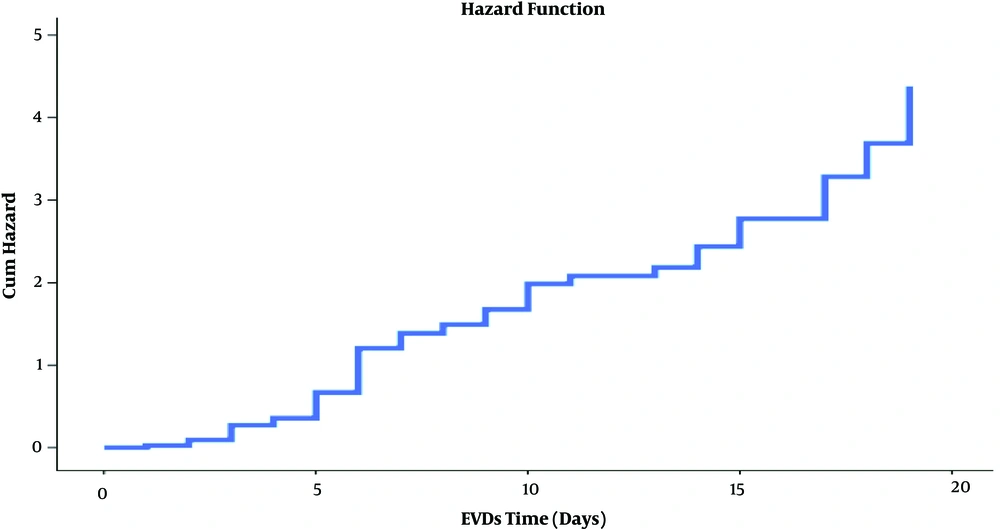
| Time of EVDs, d | 7.34 ± 4.68 | 4.95 ± 3.86 | 0.09 | 1.2 (0.4 - 3.6) |
| > 6 | 15 (62.5) | 9 (37.5) | ||
| ≤ 6 (reference) | 23 (41.1) | 33 (58.9) | ||
| Type of airway | 0.4 | |||
| Intubation | 34 (50) | 34 (50) | 1.3 (0.6 - 2.5) | |
| Awaked and spontaneous (reference) | 5 (138.5) | 8 (61.5) | ||
| Duration of surgery, h | 4.22 ± 1.20 | 4.12 ± 2.1 | 0.2 | 1.3 (0.7 - 1.86) |
| CSF lactate ≥ 36 | 0.9 | 1.5 (0.9 - 3.2) | ||
| Yes | 21 (48.8) | 22 (51.2) | ||
| No | 18 (47.4) | 20 (52.6) | ||
| Mechanical ventilation (MV) | 0.3 | 1.6 (0.9 - 2.5) | ||
| Yes | 34 (50.7) | 33 (49.3) | ||
| No (reference) | 5 (35.7) | 9 (64.3) | ||
| Length of time MV, d | 12.87 ± 12.18 | 8.57 ± 10.40 | 0.04b | 2.3 (1.4 - 3.56) |
| > 6 | 23 (60.5) | 15 (39.5) | ||
| ≤ 6 (reference) | 16 (37.2) | 27 (62.8) | ||
| Use of antibiotic prophylaxis | 0.04b | |||
| Ceftazidim + vancomycin | 17 (39.5) | 26 (60.5) | 0.3 (0.08 - 0.78) | |
| Vancomycin + meropenem ( ± other antibiotics) (reference) | 22 (57.9) | 16 (42.1) | ||
| Length of tunneling, cm | 0.01b | 2.5 (1.87 - 4.76) | ||
| > 5 | 9 (69.2) | 4 (30.8) | ||
| ≤ 5 (reference) | 36 (44.1) | 38 (55.9) | ||
| Length of time antibiotic prophylaxis, d | 15.69 ± 3.71 | 13.68 ± 8.37 | 0.5 | 1.2 (0.76 - 8.23) |
| > 9 | 21 (55.3) | 17 (44.7) | ||
| ≤ 9 (reference) | 18 (41.9) | 25 (58.1) | ||
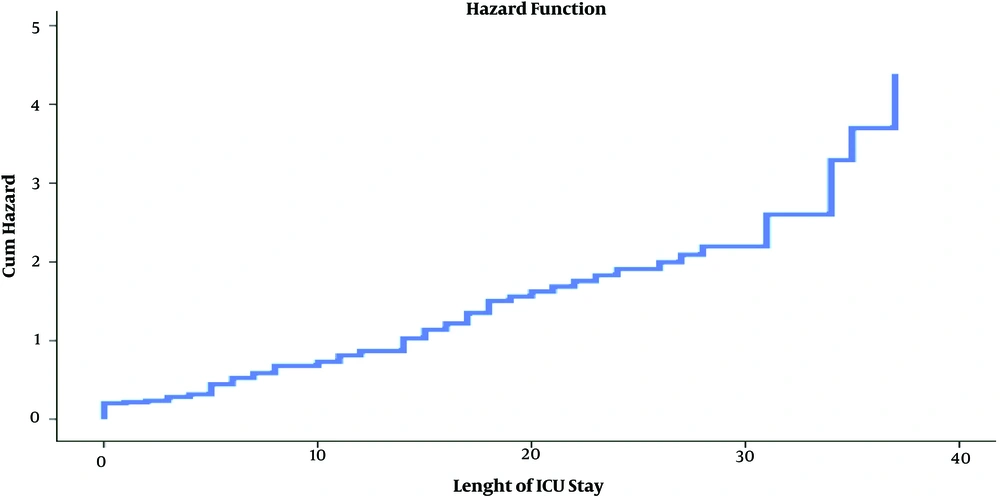
| Length of time ICU stay, d | 13.87 ± 3.67 | 10.55 ± 2.27 | 0.1 | 1.04 (0.6 - 1.98) |
| > 10 | 22 (56.4) | 17 (43.6) | ||
| ≤ 10 (reference) | 17 (40.5) | 25 (59.5) | ||
| Length of time hospital stay, d | 22.33 ± 9.61 | 21.1 ± 12.22 | 0.1 | 1.8 (0.8 - 3.21) |
| > 14 | 23 (57.5) | 17 (42.5) | ||
| ≤ 14 | 16 (39) | 25 (61) | ||
Abbreviations: CI, confidence interval; OR, odds ratio.
aValues are expressed as No. (%) or mean ± SD.
bIndicates statistical significance.
| Variables | OR (95% CI) | P-Value |
|---|---|---|
| Time of EVDs, d | 0.08 | |
| > 6 | 1.1 (0.4 - 3.6) | |
| ≤ 6 (reference) | ||
| Length of time MV, d | 0.04* | |
| > 6 | 2.5 (1.6 - 3.56) | |
| ≤ 6 (reference) | ||
| Use of antibiotic prophylaxis | 0.04* | |
| Ceftazidim + vancomycin | 0.4 (0.08 - 0.84) | |
| Vancomycin + meropenem (± other antibiotics) (reference) | ||
| Length of tunneling | 0.02* | |
| > 5 | 1.98 (1.87 - 4.76) | |
| ≤ 5 (reference) |
aThe adjusted odds ratio in multiple logistic regression analysis to predict EVDs infection. Statistical significance is indicated with a star (*).