1. Background
Primary progressive aphasia (PPA) refers to a group of neurodegenerative disorders that slowly and progressively impair language functions while other aspects of cognitive processing such as memory, attention, visuospatial skills, and executive functions remain unaffected in the initial stages of the condition (1). Recently, three clinical variants of PPA have been described including Semantic variant (svPPA), non-fluent variant (nfvPPA), and logopenic variant (lvPPA), differentiated based on the atrophy pattern and profile of speech and language features occurring in each one. The core criteria of non-fluent variant include agrammatism, motor speech disorders in language production, and effortful speech with inconsistent sound errors and distortions. Although the comprehension of single words and object knowledge are intact in this variant, the comprehension of complex grammatical sentences may be impaired. Since the word retrieval impairment arises in each of the three variants of PPA, anomia is the first and debilitating defect and symptom of PPA (1).
Few studies in the literature on word retrieval therapy and language rehabilitation have focused on naming deficits in PPA, especially on lvPPA and nfvPPA variants. The studies focused on naming ability in nfvPPA have applied multimodalities cueing and semantic-based anomia therapies and their results demonstrated a significant improvement in naming ability. In these studies, while some maintenance and generalization of the results have been reported to some extents, the generalization of the target word to the conversation has not been found (2-4). These studies indicated that the individual with PPA could learn and re-access words following the treatment despite progressive damage to the regions related to language network. In addition to learning treated items, in some cases, the generalization and maintenance of the results have also been reported (2, 5-7). However, the generalization of learning to untrained words has not been consistently demonstrated and positive improvement has usually been restricted to picture naming and treated items.
Most interventional studies in the field of word retrieval treatment in PPA have concentrated predominantly on the single-word level and picture-naming task, with the limited generalization of therapy gain. However, the ultimate goal of anomia therapy for PPA is to improve the naming abilities that would generalize to the individual’s daily communication and be maintained for some time. Since recent discourse-based treatments in post-stroke aphasia have provided more generalization to untrained items and everyday communication (8, 9), it could be an opportunity to investigate whether the same benefits may be found in the PPA population.
2. Objectives
The present study aimed to examine the effectiveness of word retrieval treatment in the individual with PPA to determine whether significant improvements are seen in word retrieval, as well as to compare the effects of cueing hierarchy and integrated treatment (cueing hierarchy integrated with discourse) on maintenance and generalization.
3. Methods
3.1. Design
A participant was randomly selected for this single-case experimental ABAB design. The participant received both cueing hierarchy therapy and integrated intervention in two consecutive phases with a break period between the phases.
During the two consecutive therapy phases, the participant received eight sessions of cueing hierarchy therapy (A) (two times a week for four weeks). After that, there were two break weeks (B) to examine maintenance/generalization of the cueing therapy phase. After completing the first phase and the break period, the participant then underwent a second phase of integrated therapy (A) (cueing in a story-retelling context) with the same duration as the first phase. After that, there were two break weeks as a follow-up phase (B). The study design involved repeated assessments made at weekly intervals, three times before treatment in order to provide the baseline status (before treatment) and once immediately following each four-week long treatment phase. The 150 line-drawings pictures were used in treatment; they were applied as a measurement tool for tracking the change of naming ability during the intervention. Correct answers were scored as 1 and no answer or non-target response was scored as 0, to increase the experimental control. The design also included the assessment of items treated in the therapy period and a matched set that was untreated.
It should be mentioned here that the assessor was the same person who provided the intervention programs; so, she was not blind to the intervention allocation.
For reporting and writing this paper, we used the single-case reporting guideline In Behavioural interventions (SCRIBE) (8).
3.2. Participant
The participant, FK, was a 56-year old, right-handed, Persian speaking housewife with three years of formal education. She had been experiencing a decline in the language performance over a period of approximately one year prior to this study and complained of increasing problems in word finding and names remembering of familiar people. FK was examined and diagnosed at the specialized memory clinic of Rozbeh hospital (Tehran University of Medical Sciences). The criteria for selection of the participant include having early to moderate language difficulties associated with a working diagnosis of PPA which were determined by multidisciplinary team including an expert cognitive neurologist, a neuropsychologist, and speech-language pathologists, based on Mesulam’s cores that are as follows: 1) predominance of language impairments over other clinical features (including word-finding deficits, paraphasia, halting speech, grammatical and/or phonological deficits in speech); 2) prominence of aphasia during the initial phase of the disorder (relative absence of memory, visuospatial, behavioral and affective deficits and disorders at the onset); 3) embodying a neurodegenerative nature, hence being progressive such that the observed deficits cannot be attributed to any other pathologies (9, 10), speak conversational Persian, word finding difficulties and having adequate hearing and vision. The exclusion criteria included an inability to give informed consent and a history of other neurological diseases (e.g., stroke, head injury, Parkinson’s disease), and severe psychiatric and cognitive disorders. Demographic information of FK is described in Table 1. FK was diagnosed with a non-fluent variant of PPA associated with apraxia of speech. Her language was effortful with halting speech, impaired word retrieval, and spared comprehension. In addition, there were many phonological errors in her repetition and her spontaneous speech was described as poor and interrupted with word retrieval difficulties. A working diagnosis of the PPA sub-type was agreed with the consensus criteria suggested by Gorno-Tempini et al. (9), and finally, the diagnosis was confirmed by structural brain magnetic resonance imaging (MRI) in which frontal and left perisylvian atrophy was confirmed.
| Test | Score Achieve | Norm (Cut-Off) |
|---|---|---|
| MMSE | 14 | 21 |
| Orientation | 8 | |
| Registration | 1 | |
| Attention and calculation | 0 | |
| Repetition and memory | 1 | |
| Language | 1 | |
| Visuospatial | 3 | |
| Parallel picture naming test | 45 | 86 |
| P-DAB | - | |
| Auditory comprehension | 8 | |
| Sequential commands | 6 | |
| Repetition | 8 | |
| Naming | 9 | |
| Fluency of spontaneous speech | 1 | |
| The content of spontaneous speech | 1 | |
| Total | 33 | |
| AQ | 55 | |
| Word-picture Matching test | - | |
| Phonologically related distractors | 47 | - |
| Semantically related distractors | 52 | |
| Word repetition test | 28 | - |
| Nonword repetition test | 18 | - |
Demographic Information of the Participant a
This study was approved by the ethics committee of Tehran University of Medical Sciences (approval number: IR.TUMS.REC.1394.2149) and written informed consent was obtained from both the participant and her husband prior to the inclusion in the study.
3.4. Stimulus Selection
First, 150 pictures assigned to concrete Farsi words including 130 names and 20 verbs were selected from available Farsi-speaking data sets (12, 14). These pictures were divided into three sets of 50 words that were matched according to psycholinguistic parameters (frequency, length of the word, number of syllables, imageability, the age of acquisition, and accuracy of naming at pre-treatment baseline assessments). These three lists were randomly assigned to three conditions: set (A); cueing hierarchy therapy (Phase1), set (B); integrated treatment (Phase 2) and set (C); untreated set.
Three parallel stories were designed based on the three-word sets and were controlled for the number of words (each story including 50 homogenous words according to three sets), number of sentences, and mean sentence length. Each story was also illustrated by an artist with a six-plate black and white drawing. In the integrated therapy phase, the story related to the word set was selected. In each treatment phase, only a one-word set was the treated stimulus and the other sets acted as control lists.
3.5. Intervention
The word retrieval intervention included two phases: semantic and phonological cueing at the single word level and the integration of these methods in narrative discourse context. Each treatment program consisted of two 60-minute sessions per week for four weeks.
3.5.1. Phase 1: Cueing Hierarchy Therapy
In the first phase of the intervention, cueing hierarchy including semantic and phonological cues, each of which with six levels, were applied in an increasing direction for semantic and phonology. The cueing hierarchy started with training semantic cueing techniques and progressing through phonemic cues. At first, the participant was guided through the semantic cueing hierarchy including superordinate, definition, semantic closure phrase, and repetition of the target word. The phonological cueing was then completed by the number of syllables, first sound, first syllable (multi-syllable words) or sounds (single-syllable words), and repetition. If the participant named a picture correctly, the next item was shown. During the treatment sessions, she was guided through the cueing therapy for each item in the targeted set.
3.5.2. Phase 2: Integrated Therapy
In the second phase, the six black and white line-drawing pictures corresponding to the treated story were shown to the participant and the story was read aloud to familiarize her with the information. First, a question with minimal semantic information was asked, to attempt to elicit the targeted word. If an incorrect response was given, semantic and phonological cues, same as phase A, were provided to the patient until she expressed the word or repeated it and then, a sentence completion cue was used. This step was included in order to place the targeted word back into the context of the story and to give the participant an opportunity to produce the word within a more complex context.
3.6. Analysis
For analyzing the data, we used traditional visual analysis and supplemented it with weighted statistics (WEST) analysis, first by evaluating the change across the whole study using WEST-Trend. In addition, to determine whether the change could be unambiguously attributed to the effects of treatment, we used WEST-Rate of change (WEST-ROC) (15), which examines whether the change in performance is significantly greater during the treatment phase compared to the no treatment (baseline) phase of the study. For both analyses, the accuracy of each item is multiplied by the appropriate coefficient for that time point and summed. The resulting weighted scores are compared to the null hypothesis (no change for WEST-Trend, and no difference between the phases for WEST-ROC) using a one-sample t-test. Only when both the WEST-Trend and WEST-ROC are significant, it can confidently be concluded that treatment has resulted in the improved performance.
4. Results
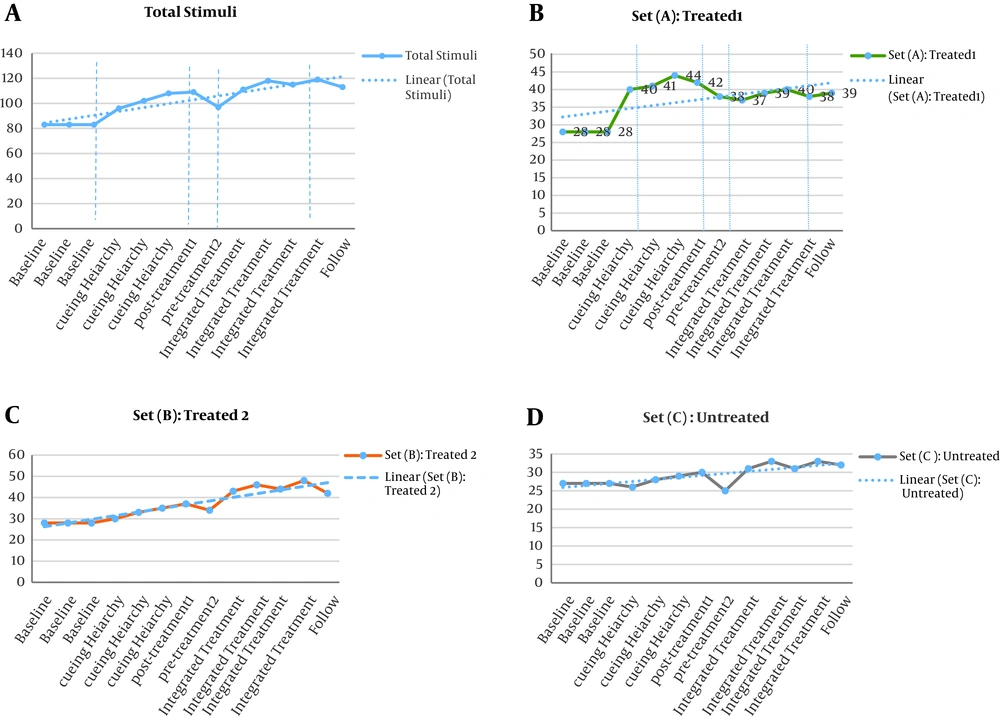
The results from the repeated measures task (the naming ability of 150 stimuli) for the participant are represented in Figure 1 and the effect sizes of intervention programs on these repeated measures estimated by WEST-TREND and WEST-ROC are shown in Table 2.
| Treatment Phase | West-Trend | West-Roc | Treatment-Specific Improvement? | ||
|---|---|---|---|---|---|
| t (49) | P | t (49) | P | ||
| Set (A) | |||||
| Cueing hierarchy | 4.5 | 0.00 | 1.95 | 0.02 | Yes |
| Integrated therapy | 0.6 | 0.27 | -0.87 | 0.8 | No |
| Set (B) | |||||
| Cueing hierarchy | 2.62 | 0.00 | 1.32 | 0.09 | No |
| Integrated therapy | 3.63 | 0.00 | 3.17 | 0.00 | Yes |
| Set (C) | |||||
| Cueing hierarchy | 0.96 | 0.17 | 0.69 | 0.24 | No |
| Integrated therapy | 2.6 | 0.00 | 1.76 | 0.04 | Yes |
Visual analysis of the data showed an improvement in the total stimuli and for each set separately during the study (Figure 1). In addition, the overall trend across the study (WEST-trend) was significant (P < 0.001). Overall, there was a significant improvement over the course of the study (WEST-trend) for all sets combined and this was significantly greater during the treated periods than during the untreated periods (WEST-ROC, P < 0.001). Therefore, it can be concluded that the treated period resulted in a remarkable improvement.
In Table 2, column ROC uses coefficients designed to ask the question of whether there is a significantly greater improvement in the treated periods than in the untreated periods, independent of the overall trend (WEST-ROC). For all the items, there was a greater improvement in the treated periods than in the untreated ones (P < 0.001). The results for each set separately during each phase indicated that in set (A): t (49) = 6.41, P < 0.001, representing that there was a significant trend in cueing treatment and there was a greater improvement in cueing therapy than in untreated periods (P = 0.02). However, there was no significant improvement during the integrated phase for set (A). The results showed no significance across the course of the study (WEST-Trend), a greater improvement in the treatment phase, and no evidence of improvement during this set over phase 2.
Set (B) with t (49) =0.05, P < 0.001 showed a significant trend for improvement in phase 1 without any significant difference in the rate of change across cueing therapy for set (B) (Table 2). Therefore, the improvement in set (B) across the cueing phase was most likely due to “practice effects” on naming task. Nevertheless, there was a significant trend in WEST-ROC during the integrated therapy for the set (B) and hence, the effect of treatment was significant for this set. In the untreated set, set (C), no significant improvement was shown in the cueing therapy phase, but there was a significant trend in WEST-ROC in the integrated therapy.
Overall, the participant showed a significant treatment-related improvement across the course of the study in WEST-trend and a greater improvement in the treatment phase (WEST-ROC). Nevertheless, there was no significant difference in performance between the two therapies phases (t (149) = -1.04, P = 2.6, 2-tailed).
5. Discussion
Word retrieval difficulty is a common problem for PPA patients. Therefore, it is important to improve naming ability despite the progressive nature of PPA. The purpose of this single-subject study was to assess the effect of word retrieval therapy in PPA within single word level and discourse context. To the best of the authors’ knowledge, this is the first report demonstrating beneficial effects of word retrieval therapy in the narrative context on PPA.
Our patient showed treatment-related improvements following both therapies regardless of the type of therapy. The performance evaluation of the participant showed that the percentage of correct answers after integrated therapy increased compared to after cueing therapy alone. However, this difference was not significant. Other studies on all PPA variants also indicated that behavioral therapies yielded positive results regardless of the type of therapy (16-19). Thus, it seems that applying words in a story context plays a more facilitating role than a single word therapy in processing and retrieving the words. This result is consistent with the results of studies that have used this paradigm in aphasia due to stroke (3, 20, 21). However, regarding the fact that word retrieval at discourse level needs more cognitive abilities and active memory capacities than single word level, it seems necessary to add some cognitive elements to therapy for strengthening the defect and the limitation mentioned in such patients in order to achieve the better result at this level.
The main goal of word retrieval therapy in the patients with aphasia is to generalize the results to untreated items that can finally provide positive communicative sufficiency. In the current study, naming ability increased in the untreated list with a positive slope (Figure 1). This difference was statistically significant after the integrated therapy. It seems that using the tasks related to daily context like storytelling may increase the possibility of generalization of the results (3, 21, 22). This significant difference obtained in the present study is consistent with some results in other studies (9, 21). Henry et al. reported generalization to untreated items and routine discourses following a semantics-oriented intensive therapy on PPA (22). Following a computer-based therapy in two nfvPPA, Jokel et al. observed no generalization to untreated items, but they were successful in the generalization of the results to syntax or verbal fluency tasks (16). Another study reported an increased accuracy in naming objects and verbs after the word retrieval therapy while no generalization to untreated items was observed (23). Since a few studies have been conducted in PPA, especially in nfvPPA, there is limited information about the potential of the generalization of results obtained by naming therapy in nfvPPA. Although findings are limited, the literature suggests that generalization to untrained tasks is possible following speech therapy in a person with PPA. Further work is needed to determine whether generalization is a reasonable expectation for therapy in nfvPPA.
In order to examine the maintenance, the patient’s naming ability was reassessed two weeks after the completion of the intervention. The results showed the maintenance of treated items, although there was a decreasing trend to some extents, compared to baseline. Thus, it seems continuous training and involving multiple levels of language processing may be important elements for the maintenance of the results. In addition, in most studies, the follow-up period varied from 1 week to 9 months and most studies reported some extents of maintenance of the results in different variants of PPA (5, 16, 19, 23-25), while no maintenance of the results was observed in other studies (23).
Some nfvPPA studies examining the maintenance of naming ability following therapy observed that the naming ability was in a higher level compared to baseline (3, 16). Therefore, the results of this study and other studies support the fact that the learned skills will probably be maintained for a short period. However, this extent of maintenance is, in fact, impressive considering the progressive nature of the disorder (13)
Some limitations are present in the study that must be acknowledged. For instance, no pre-post assessment for discourse was taken. As discourse production was related to familiarity with everyday communication, discourse assessment would increase confidence in the findings. The changes in the brain activity associated with anomia treatment were not examined in this study. Using the functional magnetic resonance imaging data may show greater benefits from anomia intervention. Furthermore, the maintenance of training effects beyond the immediate treatment period should be considered in further research. Having one follow-up to examine the changes in the participant’s performance after the intervention is another limitation of this study. More follow-up survey should not be ignored in future research. The inclusion of only one individual in the study is a further limitation with regard to the generalizability of findings. The promising results, however, suggest that trialing the intervention with a larger number of participants is warranted.
The present study aimed to examine the effectiveness of word retrieval therapy in a patient with primary progressive aphasia. Positive results achieved from the therapy program provided additional evidence supporting the importance of rehabilitation of speech and language defects in patients with the progressive disorder. Using semantic-phonological cueing in a discourse context was effective in increasing word retrieval and the patient obtained higher results following the integrated therapy. However, considering the fact that the present study was one of the first studies examining the efficacy of naming therapy at the discourse level in this group of patients, more extensive studies with more accurate research designs and more subjects are needed to obtain accurate and generalizable results and increase the effectiveness of therapy plans in the maintenance and generalization of the results by modifying and manipulating different methods.