1. Background
Pain is a multi-faceted phenomenon, which is composed of physical, psychological, social, and spiritual components. In fact, pain is an unpleasant psychological and physical experience, which is associated with real tissue injury. Those, who experience pain try to express their feeling by different words (1-3). Headache is one of the most common causes of physical pain, which results in problems for the patients, especially if it is persistent, recurrent, and severe (4-6). Migraine is just one type of pain, which has several negative effects on the patients’ health (6, 7).
Migraine is the most common cause of headache, which accounts for 15% and 6% of pain in females and males, respectively (8). Migraine is a traumatic headache that can be categorized to three groups, known as classic migraine, common migraine, and variant migraine (9, 10). Headaches caused by migraine are one of the most common headache disorders, which are characterized as severe, recurrent and occasional pain, sensitivity to sound and light, dizziness, and nausea. Disability is also reported in the later stages of this disorder (11-13). Accordingly, migraine is recognized as one of the most frequent and common causes of disability (14, 15), which influences functional tasks in patients (16).
Migraine changes the health of patients, so that the problems that are caused by migraines can reduce quality of life. The prevalence of migraine has been studied by several studies. In the study of Monfared et al. (17), 11.2% of headaches was related to migraine, and in the study of Fallahzadeh et al. (18), 12.3% were related to tension headaches, and in Khazaie et al.’s study migraine prevalence was 6.4% in males and 7.6% in females (19). Therefore, it is very important to these patients (20, 21).
Nurses are supposed to manage pain in patients (22). Of the several methods for alleviating pain in patients, pharmacological and non-pharmacological methods are frequently used (23). Pharmacological methods are not considered economical methods as they are high-priced and have several side effects. However, non-pharmacological methods are recognized as the most effective methods for alleviating pain, some of which include nursing interventions (24), massage therapy (25), psychological interventions (26), tailored Web-based interventions (27), integrative nursing intervention (28), and music therapy (29). These are not highly priced methods and have no special side effects (30).
The adaptive stability model is one of the non-pharmacological nursing models, which has had positive effects on the patients’ health in previous studies (31). The indigenous adaptive stability care model was developed by Radfar et al (32). This model aimed at helping the family of depressed patients in order to reach maximum consistency with minimum damage to the patient and his/her family. The adaptive stability model includes four stages, namely family status detection, desensitization, collaboration, and continuous exploration. In this model, family is the main contributor and interventions and care procedures are based on change in family attitudes and motivation (31, 32). Given the importance of migraine headaches and their role in patients’ health, it is necessary to make the required interventions. For this purpose, the present study was conducted with the aim of evaluating the effect of adaptive stability model on patients with migraine in the city of Ilam.
2. Methods
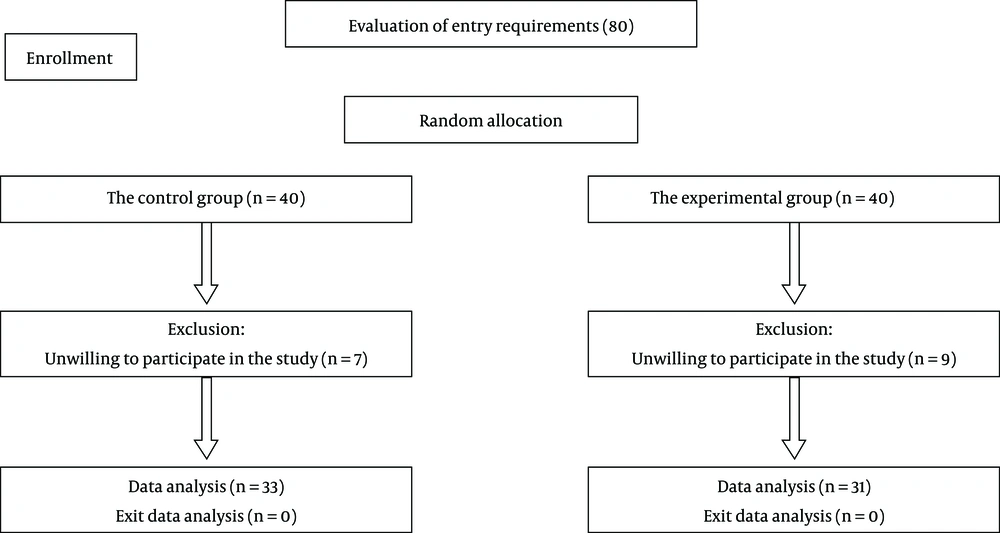
This is a semi-experimental study with pre- and post-test groups. The sample size composed of patients with migraine in the city of Ilam, who were assigned randomly to experimental (31 patients) and control groups (33 patients). The entry criteria for the study included written consents provided by the patients, having migraine based on a neurologist’s report, not having other physical and psychological diseases, and not taking other pharmacological and non-pharmacological treatments for pain management. The exit criteria encompassed causing any sort of crisis within the family and having any other disease affecting acceptance, such as trauma, etc.
In this study, the questioners attended the office and public health centers on a daily basis. In order to assign patients to experimental and control groups, the patients, who were willing to participate in the study were listed. Patients in the odd row were assigned to the control group, while those in the even Paired row were assigned to the test group. In order to prevent bias, the data were inserted by someone other than team members. Then, the information (A and B) was inserted in the SPSS V. 16 software.
The tools used in this study included demographic features questionnaire, a checklist showing the duration and frequency of pain, and a pain evaluation tool. These are recognized as the simplest and the most authentic tools for pain evaluation. Given the simplicity of these tools, the patients and their families were trained on how to use it and then the tools were completed by the patients (33). Validity and reliability of the tool were approved. All interventions were performed for 10 weeks. Additionally, the patients’ families were contacted to inform them about the tool completion process (after a two-month intervention). The patients and their families were allowed to pose their questions, if they had any.
Having assigned the patients to control and experimental groups, the intervention was performed based on the adaptive stability model, which was developed in Iran. This model constitutes of different stages, which is shown in Table 1. Written consent provided by the patients with no intention to impose costs on patients and following the ethics code related to the study were among the most prominent ethical considerations. According to previous studies, 80 patients entered the study, while 16 patients were excluded.
SPSS V. 16, descriptive statistical tests (mean and standard deviation) and inferential tests (T-test and ANOVA) were used to analyze the data.
| ASM Stages | Interventions Based on ASM Model |
|---|---|
| 1) Family status detection | While the family members of the patients were around, different stages of ASM model was fully explained. |
| The patients were willing to complete the study. | |
| The tools were also completed by the patients. | |
| This session, in which patients’ families participated took 30 to 45 minutes. | |
| Patients were divided to groups of 5 to 6 people. | |
| 2) Desensitization | |
| A) Melting | Having informed the families, their attitudes towards the pain and alleviation was shifted from simple rules to better ones. |
| These families were willing to change their attitudes. | |
| The nature of migraine was explained to the patients and their families. It was also emphasized that migraine pains are controllable provided that they cooperate with specialists. | |
| This session lasted for 30 to 45 minutes. | |
| B) Changing | Families changed their attitudes. |
| They believed that they could adapt themselves to the existing beliefs. | |
| The necessity of follow-up treatment was explained to them. | |
| This session also took 30 to 45 minutes. | |
| C) Frosting | A new attitude was developed for pain management. |
| This new belief was stabilized by the families. | |
| This new attitude became part of their beliefs. | |
| This session lasted for 30 to 45 minutes. | |
| 3) Collaboration | This process aimed to encourage the families to participate in patient care. |
| The researcher helped the families provide the patients with appropriate care at home. | |
| They were also trained on how to speak to the patient, how to manage the pain and promote health. | |
| The researcher contacted the families and asked questions about the patient's health status. | |
| The families were also allowed to contact the researcher and ask their questions. | |
| 4) Continuous monitoring | The patients' families were continuously investigated. |
| The researcher contacted the families once a week for a month in order to follow the training. |
3. Results
The findings of the present study showed that in the experimental group, 20 (64.5%) were male and 11 (35.5%) were female, while in the control group, 23 (69.7%) were male and 10 (30.3%) were female. In terms of employment status, six (19.4%) were students, three (9.7%) were employed, 13 (41.9%) were unemployed, five (16.1%) were employees, and four (12.9%) were housewives. In the control group, three (9.1%) were students, nine (27.3%) were employed, 17 (51.5%) were unemployed, two (6.1%) were employees, and two (6.1%) were housewives. In marital status, 19 (61.4%) were single and 12 (38.7%) were married, yet 23 (69.7%) were single and 10 (30.3%) were married. Regarding the educational status of patients, four (12.9%) had graduate degrees, 23 (74.2%) had Bachelor’s degrees, four (12.9%) had higher education, yet in the control group two (6.1%) had diploma education, 22 (66.7%) Bachelor’s degree, and nine (27.3%) were educated. The mean age of the patients in the experimental group was 34.90 (5.28) and that of the control group was 34.30 (6.19). There was no difference between the demographic characteristics of the patients in the experimental and control groups (P > 0.05).
| Variable, Time | Experimentala | Controla | P Value |
|---|---|---|---|
| Headache severity | |||
| Pre-test | 7.97 ± 0.75 | 7.94 ± 1.02 | 0.91 |
| Post-test | 3.93 ± 1.06 | 6.12 ± 1.39 | 0.000 |
| P value | 0.001 | 0.001 | - |
| Duration | |||
| Pre-test | 5.29 ± 1.06 | 5.79 ± 1.38 | 0.10 |
| Post-test | 3.29 ± 1.21 | 5.69 ± 1.40 | 0.000 |
| P value | 0.001 | 0.72 | - |
| Frequency of headache | |||
| Pre-test | 11.58 ± 3.89 | 11.52 ± 2.97 | 0.94 |
| Post-test | 6.09 ± 1.42 | 10.24 ± 4.41 | 0.000 |
| P value | 0.001 | 0.18 | - |
aValues are expressed as mean ± SD.
According to the findings presented in Table 2 before the intervention, there was no significant difference between the mean severity, hours, and frequency of headache in the experimental and control groups. However, after the intervention, severity and duration of headache in the experimental group was reduced compared to the control group after the intervention and the reduction was statistically significant (P < 0.001). Also, in the control group after the intervention, mean headache severity had a significant decrease compared to before the intervention (P < 0.001).
4. Discussion
Patients with migraine always suffer from pain (34-36). For this purpose, the present study aimed at investigating the effect of adaptive stability model, as an indigenous model developed in Iran, on the headache of patients with migraine. The findings showed that this model can reduce pain in patients with migraine to a great extent. The only study, in which the ASM model has been used, is a study by Esazadeh et al. (31), who aimed at evaluating the effect of ASM to reduce readmission alleviation in patients with depression. In the present study, the patients were assigned to experimental and control groups. The adaptive stability model includes four stages, namely family status detection, desensitization, collaboration, and continuous exploration. The findings indicated that the number of hospitalized patients decreased significantly six months after the implementation of ASM, which shows the high efficacy of this model (32). This is in good agreement with the results of this research.
Different nursing interventions have been performed in order to reduce pain in patients. For instance, Ali showed that nursing interventions reduce pain in patients undergoing spinal anesthesia (37). In their study, Leroux et al. attempted to investigate the effect of nursing intervention on the quality of life and self-efficacy of the patients with migraine. They showed that these interventions proved useful and positive (38). In a systematic review study, Castillo-Bueno et al. emphasized that nursing interventions can reduce pain (23), which is consistent with the results of the current study.
In another non-pharmacological study on pain reduction, Hamedanizadeh et al. investigated the effect of a self-care program on headache indices in patients with migraine. In this study, four sessions were held based on the patients’ self-efficacy needs. After the intervention, the number, duration, and severity of headache attacks in the control group decreased significantly compared to the experimental group, which is consistent with the results of this study (39).
One of the limitations of this study was the difficulty of collecting data and not collaboration with patients. To address this limitation, the benefits of this model were explained to patients and their participation was completely optional. One of the strengths of this study was the fact that the study used a new non-pharmacological intervention. This intervention is new and has many benefits for patients, as well as the construction of the country and is a completely natural model, in accordance with the cultural conditions of Iran.
4.1. Conclusion
Given the fact that the implementation of the ASM model has had significant effects on the pain indices in patients with migraine, it is highly recommended as an affordable and non-pharmacological intervention to reduce pain. Since this model has not been widely used in different studies, it is recommended that researchers use this model as an indigenous model in researches and evaluate it on different diseases with various variables.

.png)