1. Background
Effective self-care depends on the knowledge and understanding of individuals and their self-control abilities (1). Improvement of perceived self-care ability can extend the life expectancy of patients with chronic diseases and promote the quality of life, active lifestyle, and independence (2). Generally, perceived self-care ability depends on various social determinants and health factors (1).
Stroke is recognized as an important health problem, which has spread throughout the world. It is described as one of the main causes of early morbidity and mortality, especially in low-income and middle-income countries (3). The number of elderly people with chronic diseases is speculated to rise rapidly by 2050 (4). Self-care is an important tool in the prevention of stroke. With the increase in the elderly population around the world, the incidence of stroke is also increasing. In fact, stroke is the second leading cause of mortality worldwide (2).
The long-term lifestyle study of stroke patients suggests complex issues in their daily lives (5). In healthy people, self-care focuses on health promotion, while in people with chronic diseases, it emphasizes self-care behaviors, compliance with treatment, and healthy lifestyle (6). Today, given the increased economic burden of chronic diseases, health service providers are trying to direct care from hospitals to the patient’s home (4).
Generally, the quality of provided care in hospitals is much higher than that provided at home (7). Therefore, attention to self-care in patients with chronic diseases and their participation in self-care activities are essential for disease management (8). Moreover, understanding the patient’s self-care ability is important for determining his/her needs during discharge. In fact, by understanding the patient’s perceived self-care ability, nurses and care providers can design and implement proper therapeutic interventions (9).
The patient’s understanding is fundamental to his/her perceived self-care ability and independent performance. Also, therapists, by understanding the perceived self-care ability of stroke patients, can promote accurate resource allocation and planning during hospital discharge and follow-up (10). Rehabilitation centers provide nurses with the opportunity to develop interventions, which can help stroke victims cope with their chronic disease and make appropriate self-care decisions (11). Therefore, a thorough understanding of the perceived self-care ability of stroke patients living at home is very important, which can help predict the outcomes, as a significant part of the patient’s performance is influenced by self-care ability.
So far, no major attempts have been made to portray the care needs of stroke patients at different stages of the disease. Also, no sufficient evidence has been presented in this area and the experiences of patients have not been discussed (12); therefore, further research is necessary. In this qualitative study, we aimed to determine the implications of understanding the perceived self-care ability of stroke patients living at home via content analysis.
2. Objectives
The current study aimed at determining the consequences of perceived self-care ability in stroke patients living at home in Iran.
3. Methods
This qualitative study was conducted using the content analysis approach in Iran in 2018. Ten independent home-dwelling patients in the sub-acute and chronic phase of stroke were included in this study. One patient was interviewed at home, while nine patients were interviewed at the rehabilitation centers of Tehran, Iran. The sub-acute and chronic phase of stroke lasts more than one month.
Patients with a history of a sub-acute and chronic phase of stroke (more than one month after it) were eligible if having the ability to express oneself and willing to participate. Patients with cognitive status survey score of < 21 and the functional independence measure (FIM) score of < 22 were excluded. Patients with hemiparesis or hemiplegia, who could walk to the bathroom with a cane or walker and live at home independently, were also eligible.
In this study, the individual patient was the unit of analysis. The setting for interviewing the patients was their homes. However, most (except one) participants were reluctant to conduct interviews at home. Therefore, by referring to reputable rehab centers in the city of Tehran, the patients diagnosed with stroke were identified according to the inclusion criteria. Patients referred to the rehabilitation centers who met all inclusion criteria were selected. The researcher arranged to interview eligible patients at their convenience.
For data collection, semi-structured interviews were conducted. The researcher communicated with the participants and obtained their oral consent to participate in the study. After obtaining consent, the researcher proceeded with the interviews. The questions in the interview guide were as follows: “What is your experience of day-to-day living with the disease at home?” and “What do you do in terms of self-care when you are at home?” Also, the researchers asked exploratory questions during the interviews for deeper analysis (e.g., “Can you explain more?”). The duration of each interview varied from 20 to 30 minutes on average; if necessary, prolonged interviews were conducted in two stages.
Overall, 10 interviews were conducted in this study. The interviews were recorded in a quiet place and sampling continued until data saturation (13). Simultaneously, Graneheim and Lundman’s five-step approach was applied to analyze the data. The interviews were immediately transcribed and entered in MAXQDA. All interviews were read to reach a thorough understanding of their content and to define the semantic units and primary codes. Next, similar primary codes were classified in larger groups and content analysis was performed (14).
In order to confirm the accuracy and reliability of data, the validity and reliability criteria proposed by Lincoln and Guba were followed. The researcher established a long-term relationship with the participants to gain their trust. After extracting the primary codes, their accuracy was confirmed by asking the participants’ opinions; in the event of any conflict or inconsistency, the codes were revised. Also, the control method was implemented by two faculty members and experts in the field of qualitative research, and agreements were obtained on the selected codes and classifications.
We tried to consider the diversity of the sample in terms of age, gender, education, and marital status. Regarding ethical considerations, all participants were informed about the purpose and method of the study. After reaching an agreement, informed consent forms were obtained for participation in the study. The participants were assured of the anonymity and confidentiality of their information and audio files. They were also allowed to withdraw from the study at any time during the study.
This study was approved by the Ethics Committee of Tehran University of Social Welfare and Rehabilitation Sciences (code: IR.USWR.REC.1396.208).
4. Results
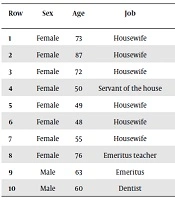
The participants included 10 patients with chronic stroke (two males and eight females), aged 48 - 87 years (average age, 63.7 years) (Table 1).
| Row | Sex | Age | Job | Education Degree | Setting | Marriage | Duration After Stroke | Number of Stroke Attacks |
|---|---|---|---|---|---|---|---|---|
| 1 | Female | 73 | Housewife | Elementary | Besat | Husband died | One month | First |
| 2 | Female | 87 | Housewife | Elementary | Besat | Husband died | Three years | Second |
| 3 | Female | 72 | Housewife | High school | Khanevadeh | Abandoned | One year | First |
| 4 | Female | 50 | Servant of the house | Diploma | Rofeideh | Living with Husband | Three months | First |
| 5 | Female | 49 | Housewife | Diploma | Rofeideh | Living with Husband | Seven months | First |
| 6 | Female | 48 | Housewife | Diploma | Rofeideh | Living with Husband | Three years | Third |
| 7 | Female | 55 | Housewife | Illiterate | Besat | Living with Husband | 20 days | First |
| 8 | Female | 76 | Emeritus teacher | Diploma | Home | Husband died | Seven months | First |
| 9 | Male | 63 | Emeritus | Diploma | Rofeideh | Living with wife | Seven years | Second |
| 10 | Male | 60 | Dentist | Doctor | Rofeideh | Living with wife | Seven months | First |
We reached data saturation by conducting 10 interviews with 10 participants and identified the primary categories. After identifying the primary themes, the primary codes were extracted from the interviews. These codes were classified after several reviews and summarized, based on their similarities. With further review and comparison, the main themes were identified as the primary categories. Two main categories and three subcategories were identified, including “promotion of adaptive strategies” (self-efficacy and adaptation to disability) and “maintaining a healthy lifestyle” (maintaining individual autonomy) (Table 2).
| Main Category | Subcategories |
|---|---|
| Promoting adaptive strategies | Self-efficacy |
| Adaptation to disability | |
| Maintaining a satisfying lifestyle | Maintaining individual autonomy |
4.1. Promotion of Adaptive Strategies
The main extracted theme in this study was the promotion of coping strategies, which included two main subcategories of self-efficacy and adaptation to disability.
4.1.1. Self-Efficacy
From the point of view of the participants, the ability to perform everyday life activities, social participation, self-care, self-help, autonomy, return to work, personal hygiene, and compliance with pharmaceutical and nutritional recommendations are all the examples of perceived self-care ability. In this regard, one of the participants (male, married, 63-year-old) stated:
“After the stroke, despite hemiplegia, I was able to walk again, swim, and drive. I’m taking my medications on time, and I can bear a major share of my responsibilities on my own. Of course, I helped myself a lot to feel better.”
4.1.2. Adaptation to Disability
From the participants’ point of view, this subcategory includes accepting one’s disability, use of adaptive strategies, acknowledging one’s problem, feelings of helplessness and defeat related to the disease, eagerness to repeat, practice, and learn to communicate despite disability, one of the participants (male, married, 60-year-old) said:
“God has created man in a way that he can endure any difficulty. For example, it was very hard for me at first to go to the bathroom alone with only one hand... Someone had to open my belt, which was really difficult for me. I learned to do it myself over time and tried to walk on my own. Now, I can zip and unzip my pants with one hand!”
4.2. Maintaining a Healthy Lifestyle
This category includes one major subcategory, i.e., individual autonomy.
4.2.1. Individual Autonomy
From the participants’ point of view, this category includes the development of self-care skills, understanding the level of dependence or independence, interest in home-based rehabilitation, and a positive outlook for maintaining independence. In this regard, one of the participants (male, married, 60-year-old) said:
“I am a dentist. After my illness, I decided to return to work, but the function of one of my hands was impaired. It was pointless to stay at home. Now, I can do simple things, like wringing prescriptions, molding, and removing dental plaques; I feel quite happy.”
5. Discussion
The aim of this study was to describe the consequences of perceived self-care abilities of stroke patients living at home. The results showed that the most prominent theme is the promotion of coping strategies in stroke patients. Researchers believe that patients with high perceived self-care ability are able to understand their disease and know how to cope with it. Individuals with high perceived self-care ability can take the necessary measures in the event of any changes (8). Folden showed that the improvement of self-care skills can help a person cope with functional disabilities; therefore, the sustainability of stroke rehabilitation and self-care skills is important (11). Kristensen et al. believe that self-care has a very dynamic nature in patients with a chronic disease, and there is no holistic view of this concept (8). Lou et al. believe that the patient’s home is the best place to continue learning and relearning the necessary skills and functional approaches for living in that environment (15).
The main theme, i.e., promotion of adaptive strategies, consists of two subcategories, self-efficacy and adaptation to disability. Self-efficacy is a psychological construct, which refers to a person’s beliefs about his/her ability to produce a certain level of performance that affects his/her life (5). Robinson described four components of self-efficacy and their application in patients with stroke in the rehabilitation stage, including assuring patients, providing social support, having self-confidence, and showing adequate self-efficacy for rehabilitation at home (16).
Some studies have examined self-efficacy, as well as other constructs related to perceived self-care ability (17). Rabie et al. believe that if patients with chronic diseases do not have adequate knowledge of self-care, health, and autonomy-related problems, they will not be able to take care of themselves and will lose the ability to cope with their disease (18). In a combined study by Sun et al., it was found that multiple factors may influence perceived self-care ability and adaptation to disability. Some of these factors included the patient’s knowledge, competence, self-esteem, education, support system, collaborative effort in home-based rehabilitation, problem-solving ability, stress management, caregiver’s understanding, patient’s physical condition, the patient’s understanding of his/her health condition, and understanding the implications of self-care behaviors and perceived self-care ability (19). The results of these studies are consistent with the present results.
Another important theme, which is one of the implications of perceived self-care ability in patients with stroke, is maintaining a healthy lifestyle, which includes one major subcategory, i.e., individual autonomy. Based on the results of previous studies, patients who are able to maintain their individual autonomy in daily life activities and are less dependent on others feel more satisfied with their lives (7, 20-22). In addition, in a study by Casey et al., the level of dependence or independence was defined as a determining factor for perceived self-care ability. They claimed that understanding the experiences of stroke patients is critical for designing, revising, and implementing healthcare plans and policies to meet the needs of stroke patients (23). The findings of these studies are also consistent with the results of the present study.
5.1. Conclusions
A person’s perceived self-care ability and autonomy are immediately evaluated by clinicians after a stroke. Stroke affects the person’s ability to participate in everyday life activities, disrupts the normal course of life and consequently, reduces the quality of life. The results of previous studies show that these patients do not have a high quality of life. According to the present results, the higher the patients’ understanding of their abilities and limitations is, the greater their adaptation to disability will be during the transition from the acute to chronic phase. In fact, patients with a greater understanding can adopt more suitable strategies. Therefore, the development of appropriate strategies and behaviors, such as accepting disability, self-efficacy, perseverance, spiritual practice and beliefs, cooperation of family members in the patient’s adaptation, and reliance on family support can help patients better cope with their problems.