1. Background
At the end of 2019, an outbreak of a new respiratory infectious disease, later called Coronavirus disease 2019 (COVID-19), was identified in Wuhan city, Hubei Province, China (1). The World Health Organization (WHO) declared COVID-19 as a global pandemic on March 11, 2020 (1, 2). By late 2020, all countries worldwide were affected by this pandemic. On March 2, 2020, the first COVID-19 case was detected in Indonesia. By the end of 2020, 735,124 COVID-19 cases and 21,944 deaths had been reported in all 34 provinces of Indonesia (3, 4).
Although the incidence of COVID-19 infection is lower in children than adults, the number of pediatric cases in Indonesia has been increasing rapidly (2). In general, children with COVID-19 experience milder symptoms with a better prognosis than adults, although severe or critical cases and several deaths in children have been documented in China and other countries (1, 5, 6). Few studies have investigated children infected with COVID-19, and most published studies are case reports, case series, or include a small number of children. Data on symptoms, laboratory, and radiology findings from children with COVID-19 are limited.
West Nusa Tenggara province is one of 34 provinces in Indonesia and has an estimated population of 5,070,385 and includes 10 districts (7). The first COVID-19 case in children was found in March 2020, and the number of cases is still increasing until now.
2. Objectives
This study was conducted to describe the demographics, clinical characteristics, and outcomes of children with COVID-19 in West Nusa Tenggara Province of Indonesia.
3. Methods
We conducted a retrospective review study of children with laboratory-confirmed COVID-19 using a registry collected by the Indonesian Pediatric Society (IPS), West Nusa Tenggara Branch, which served as the data coordinating center for this study. Almost all members of IPS from the province and several district hospitals contributed data to the registry. Patient data included age, gender, district, comorbidities, mode of presentation (asymptomatic or symptomatic), clinical manifestations, laboratory and radiology findings, and clinical outcomes at the time of study closure. We recognize that there were substantial differences in practices and facilities across the participating hospitals.
We reviewed the registry of children with COVID-19 from provincial, private, and district hospitals as well as district central quarantines (i.e. facilities operated by the Province Health Office that provide temporary accommodation for people exposed to COVID-19 during their quarantine period) in West Nusa Tenggara Province. Cases identified between March 1 and July 12, 2020, were included in this study. We selected this period because the first COVID-19 case was detected in Indonesia on March 2, 2020, and a new guideline for prevention and management of COVID-19 was published by the Ministry of Health on July 13, 2020 (8).
The inclusion criterion was children aged 0 to less than 18 years old with confirmed COVID-19, diagnosed by real-time reverse-transcriptase polymerase chain reaction (RT-PCR) detection of SARS-CoV-2 from March 1 to July 12, 2020. Subjects with missing data (demographic, clinical, or outcome) in the registry were excluded.
RT-PCR tests were performed for children suspected of COVID-19 based on clinical manifestations, with or without a history of exposure. Tests were also performed on asymptomatic children with a history of exposure to a COVID-19 confirmed case as part of contact tracing activities. A COVID-19 confirmed case was defined as detection of SARS-CoV-2 by RT-PCR.
The identification of the SARS-CoV-2 virus by real-time RT-PCR assay was obtained from nasopharyngeal swab specimens following the national guidelines (8, 9). The RT-PCR test was performed in five different laboratories: General Hospital of West Nusa Tenggara Province, Mataram University Hospital, Mataram Regional General Hospital, Dr. Soedjono Selong East Lombok District Hospital, and Manambai Abdulkadir Sumbawa General Hospital. Post mortem nasopharyngeal swabs were collected for suspected COVID-19 patients who died before performing specimen collection. Laboratory staff performing nasopharyngeal swab collection and RT-PCR testing had been trained by the West Nusa Tenggara Province Health Office before they were approved to perform the procedures. We used the Novel Coronavirus (2019-nCoV) Nucleic Acid Diagnostic Kit (Sansure Biotech Inc, Changsa, China), Nest Scientific Viral Transport Media and swabs from NEST Biotechnology Co Ltd, Wuxi, China, and Biocomma virus transport and preservative medium (inactivated) (Biocomma Ltd, China) provided by Ministry of Health. External quality control of testing laboratories was performed regularly by the Agency of Health Research and Development, Ministry of Health.
The severity of COVID-19 infection was classified based on clinical features, laboratory testing, and chest X-ray as according to the National Guidelines by the Indonesian Ministry of Health. An asymptomatic case was defined as a case without any symptoms. Mild symptomatic cases had non-specific symptoms such as fever, cough, sore throat, rhinorrhea, anosmia, or malaise. Moderate symptomatic cases were in patients who had mild pneumonia symptoms, i.e. cough or dyspnea. A patient was categorized as a severe symptomatic case if at least one of the following was present: central cyanosis or SpO2 < 90%, severe respiratory distress characterized by profound chest retraction, feeding difficulty in infants, decreased consciousness, or seizure. Cases with the criteria for acute respiratory distress syndrome were categorized as critical symptomatic (8).
Based on national guidelines, the COVID-19 RT-PCR test should be repeated a week after the first positive result, and patients should have two negative results before finishing isolation. Duration of conversion was defined as the number of days from the first positive PCR result until the first negative result of two consecutive negative PCR results. Completed isolation was defined by two consecutive negative PCR results.
Because not all subjects had body length/height data, nutritional status was estimated using the WHO weight for age, WHO chart for children under < 5 years old children, and the Centers for Disease Control and Prevention (CDC) chart for children > 5 years old.
Data from eligible children with confirmed COVID-19 and available medical record data, including demographics, clinical characteristics, and outcomes, were included in the analysis.
Statistical analysis was performed using the Statistical Package for the Social Sciences (SPSS) software, version 22.0 (IBM, Chicago, IL). The chi-square test was used for the comparison of categorical data. ANOVA and independent t-test were used to compare normally distributed numerical data. A P value < 0.05 was considered statistically significant.
Ethical approval for this study was obtained from the General Hospital of West Nusa Tenggara Province Ethics Committee (070.1/15/KEP/2020).
4. Results
During the study period, 146 COVID-19 confirmed subjects were included from one provincial hospital, 18 private and district hospitals, and three district central quarantine facilities. Cases came from all 10 districts in West Nusa Tenggara Province. There were 70 symptomatic subjects and 76 asymptomatic subjects (Table 1). Their ages ranged from 1 day to 18 years old with a median of seven years. Most cases belonged to the 10-18 years old age group (40.4%) and came from Mataram district (34.2%), the capital of our province. Of 146 subjects, 85 (58.2%) were males and 61 (41.8%) were females. Compared with symptomatic children, asymptomatic children had higher median age (138 vs. 24 months, P < 0.01), and most of them (58%) were 10-18 years of age (P < 0.01). The majority of asymptomatic subjects (40%) lived in Mataram District (P < 0.01), and 88% had a history of COVID-19 contact (P < 0.01). Compared to symptomatic subjects, they had a longer duration of PCR conversion (18 vs. 10 median days, P ≤ 0.01). However, by the end of the study period, most (82%) had complete isolation.
| Characteristics | Category | |||
|---|---|---|---|---|
| All cases N = 146 | Symptomatic N = 70 | Asymptomatic N = 76 | P Value | |
| Age | 0.000 | |||
| Median (min; max), months | 84 (0; 213)b | 24 (0;208)a | 138 (4; 213) | 0.000 |
| < 1 year, No. (%) | 27 (18.5) | 22 (31) | 5 (6.6) | |
| 1-< 5 years, No. (%) | 39 (26.7) | 27 (39) | 12 (16) | |
| 5-< 10 years, No. (%) | 21 (14.4) | 6 (8.6) | 15 (20) | |
| 10-18 years, No. (%) | 59 (40.4) | 15 (21) | 44 (5) | |
| Sex, No. (%) | 0.934 | |||
| Male | 85 (58.2) | 41 (59) | 44 (58) | |
| Female | 61 (41.8) | 29 (41) | 32 (42) | |
| District, No. (%) | 0.006 | |||
| Mataram | 50 (34.2) | 20 (29) | 30 (40) | |
| West Lombok | 38 (26.0) | 20 (29) | 18 (24 | |
| Central Lombok | 13 (8.9) | 9 (13) | 4 (5.3) | |
| East Lombok | 23 (15.8) | 13 (19) | 10 (13) | |
| North Lombok | 5 (3.4) | 5 (7.1) | 0 | |
| Othersc | 17 (11.6) | 3 (4.3) | 14 (18) | |
| History of COVID-19 contact, No. (%) | 0.000 | |||
| Yes | 80 (54.8) | 13 (19) | 67 (88) | |
| No | 66 (45.2) | 57 (81) | 9 (12) | |
| Degree of severity, No. (%) | ||||
| Asymptomatic | 76 (52.1) | 0 | 76 | |
| Mild | 17 (11.6) | 17 (24) | 0 | |
| Moderate | 4 (2.7) | 4 (5.7) | 0 | |
| Severe | 43 (29.5) | 43 (61) | 0 | |
| Critical | 6 (4.1) | 6 (8.6) | 0 | |
| Hospitalized, No. (%) | ||||
| Yes | 55 (37.7) | 55 (78.6) | 0 | |
| No | 91 (62.3) | 15 (21.4) | 76 (100) | |
| Duration of conversion, median (min; max), days | 13 (3; 57) | 10 (3; 31) | 18 (5; 57) | 0.000d |
| Completed isolation, No. (%) | 0.000d | |||
| Yes | 128 (87.7) | 66 (100) | 62 (81.6) | |
| No | 14 (9.6) | 0 | 14 (18.4) | |
| Death, No. (%) | 4 (2.7) | 4 (5.7) | 0 | - |
aP value was applied for comparison of symptomatic to asymptomatic groups.
bMinimum age of subjects was one day old.
cOthers: Sumbawa, West Sumbawa, Bima, Dompu;
dsubjects who died in the symptomatic group were not included.
Clinical manifestations in the symptomatic group are shown in Table 2. The most common symptom was cough (81%), followed by fever (69%), fatigue/malaise (63%), and difficulty in breathing (60%). Most symptomatic COVID-19 patients were hospitalized with severe disease, mainly pneumonia (70%). Comorbidities were found in 16 (out of 49) pneumonia subjects, and complications only occurred in six of them.
| Clinical Manifestations | N= 70 |
|---|---|
| Symptoms at admission, No. (%) | |
| Fever | 48 (69) |
| Cough | 57 (82) |
| Fatigue/malaise | 44 (63) |
| Sore throat | 3 (4.3) |
| Rhinorrhoea/nasal blockage | 29 (41) |
| Difficulty breathing | 42 (60) |
| Gastrointestinal symptomsa | 14 (20) |
| Degree of severity, No. (%) | |
| Mild | 17 (24) |
| Moderate | 4 (5.7) |
| Severe | 43 (61) |
| Critical | 6 (8.6) |
| Hospitalized, No. (%) | |
| Yes | 55 (79) |
| No | 15 (21) |
| Diagnosis, No. (%) | |
| Upper ARI | 18 (26) |
| Lower ARI (pneumonia) | 49 (70) |
| Othersb | 3 (4.3) |
| Pneumonia, Comorbiditiesc (N = 49) | |
| Yes | 16/49 |
| No | 33/49 |
| Pneumonia, Complicationdd (N = 49) | |
| Yes | 6/49 |
| No | 43/49 |
| Nutritional status, No. (%)e | |
| Normal | 54 (77) |
| Malnourished | 13 (19) |
| Severely malnourished | 3 (4) |
Abbreviations: ARI, acute respiratory infection.
aNausea/vomiting only (5), nausea vomiting with diarrhea (3), nausea/vomiting with abdominal pain (1), diarrhoea only (4), abdominal pain only (1).
bHead trauma (2), neonatal asphyxia (1).
cAnemia, asthma, malignancy, congenital heart disease, epilepsy.
dAcute respiratory distress syndrome (5), pleural effusion (1).
eBased on body weight for age WHO chart for < 5 years old children, and CDC for > 5 years old children.
Hospitalized COVID-19 confirmed subjects were younger than non-hospitalized subjects (P < 0.01), most of them (40%) were less than five years of age, with a median age of 15 months (Table 3). Most of them (60%) lived in Mataram and West Lombok District. Only four hospitalized patients had a history of COVID-19 contact (P < 0.01). They had a higher respiratory rate and temperature (P < 0.01), and lower oxygen saturation (P < 0.01) than non-hospitalized, symptomatic COVID-19 patients. The laboratory results showed a lower hemoglobin level (P = 0.015) and higher WBC count (P = 0.01) at admission. There was no difference concerning sex, nutritional status, chest X-ray, and duration of conversion between hospitalized and non-hospitalized symptomatic subjects (Table 3).
| Characteristics, N =70 | Hospitalized, N=55 | Non-hospitalized, N=15 | P Value |
|---|---|---|---|
| Age | 0.000 | ||
| Median (min; max), months | 15(0; 204)b | 160 (36; 208) | 0.000 |
| <1 year, No. (%) | 22 (40) | 0 | |
| 1-<5 years, No. (%) | 26 (47) | 1 (6.7) | |
| 5-<10 years, No. (%) | 4 (7.3) | 2 (13) | |
| 10-18 years, No. (%) | 3 (5.4) | 12 (80) | |
| Sex, No. (%) | 0.642 | ||
| Male | 33 (60) | 8 (53) | |
| Female | 22 (40) | 7 (47) | |
| District, No. (%) | 0.038 | ||
| Mataram | 16 (29) | 4 (27) | |
| West Lombok | 17 (31) | 3 (20) | |
| Central Lombok | 8 (15) | 1 (6.7) | |
| East Lombok | 11 (20) | 2 (13) | |
| North Lombok | 1 (1.8) | 4 (27) | |
| Othersc | 2 (3.6) | 1 (6.7) | |
| History of COVID-19 contact, No. (%) | 0.000 | ||
| Yes | 4 (7.3) | 9 (60) | |
| No | 51 (93) | 6 (40) | |
| Nutritional status, No. (%)d | 0.947 | ||
| Normal | 39 (71) | 11 (73) | |
| Malnourished | 13 (24) | 3 (20) | |
| Severely malnourished | 3 (5.5) | 1 (6.7) | |
| Presentation at admission | |||
| Respiratory rate; median (min; max), TPM | 43 (18;75) | 20 (16;25) | 0.000 |
| SpO2; median (min; max), No. (%) | 97 (78;100) | 99 (95;100) | 0.009 |
| Axillary temperature; mean ± SD, °C | 37.5 ± 0.9 | 36.5 ± 0.4 | 0.000 |
| Decreased consciousness, No. (%) | 4 (7.3) | 0 | |
| Laboratory examinatione | |||
| Haemoglobin; mean ± SD, g/dL | 11.2 ± 2.2 | 12.8 ± 0.6 | 0.015 |
| WBC counts; median (min; max), 103/µL) | 12.1 (4.0; 66.5) | 8.9 (5.0; 11.4) | 0.01 |
| Neutrophil; median (min; max), % | 51.4 (21.5; 86.5) | 54.4 (45.0; 75.0) | 0.66 |
| Lymphocyte: median (min; max), % | 32.5 (4.1; 69.4) | 35.6 (18.0; 47.0) | 0.624 |
| Platelets count; median (min; max), 103/µL | 349 (70; 1,130) | 336 (221; 452) | 0.447 |
| ESR; median (min; max), mm/hourf | 11.5 (2.0; 109.0) | 12.5 (7.0; 20.0) | 0.983 |
| Chest X-rayg; No. (%) | |||
| Normal chest X-ray | 5 (9.1) | 12 (92.3) | |
| Unilateral infiltration | 20 (36) | - | |
| Bilateral infiltration | 28 (51) | - | |
| Unilateral consolidation | 3 (5.6) | 1 (7.6) | |
| Pleural effusion | 1 (1.9) | - | |
| Duration of PCR conversion, median (min; max), daysh | 10 (3; 30) | 13 (4; 31) | 0.425 |
Abbreviations: ESR, erythrocyte sedimentation rate; PCR, polymerase chain reaction; TPM, times per minute; WBC, white blood cells.
aAll data were presented as median (min; max) when the distribution was not normal.
bMinimum age of subjects was one day old.
cOthers: Sumbawa, West Sumbawa, Bima, Dompu.
dBased on body weight for age WHO chart for < 5 years old children, and CDC for >5 years old children.
eThere were two missing data in the hospitalized group, and three missing data in the non-hospitalized group.
fn = 24 in the hospitalized group, and n=8 in the non-hospitalized group.
gThere was one missing data in the hospitalized group but three subjects had combination, and two missing data in the non-hospitalized group.
hSubjects who died were not included.
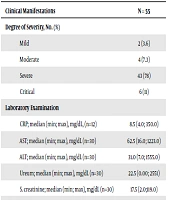
Of 55 hospitalized subjects with confirmed COVID-19, pneumonia was the most frequent diagnosis (89%) (Table 4), and bilateral infiltrate (51%) was the most frequent radiological finding (Table 3). Also, 29% of hospitalized patients had comorbidities. The shortest mean duration length of stay was found in critical subjects, and death occurred in 4 (7%) of hospitalized patients (Table 4). The rate of hospitalization for subjects with confirmed COVID-19 aged < 1 year, 1-< 5 years, 5-< 10 years, and 10-18 years were 81.5%, 66.7%, 19.0%, and 5.1%, respectively.
| Clinical Manifestations | N = 55 |
|---|---|
| Degree of Severity, No. (%) | |
| Mild | 2 (3.6) |
| Moderate | 4 (7.3) |
| Severe | 43 (78) |
| Critical | 6 (11) |
| Laboratory Examination | |
| CRP; median (min; max), mg/dL, (n=12) | 8.5 (4.0; 350.0) |
| AST; median (min; max), mg/dL (n=30) | 62.5 (16.0; 1223.0) |
| ALT; median (min; max), mg/dL (n=30) | 31.0 (7.0; 1555.0) |
| Ureum; median (min; max), mg/dL (n=30) | 22.5 (0.00; 2551) |
| S. creatinine; median (min; max), mg/dL (n=30) | 17.5 (2.0;119.0) |
| Diagnosis, No. (%) | |
| Upper ARI | 3 (5.5) |
| Lower ARI (pneumonia) | 49 (89.0) |
| Othersb | 3 (5.5) |
| Comorbiditiesc, No. (%) | |
| Yes | 16 (29.1) |
| No | 39 (70.9) |
| Complicationsd, No. (%) | |
| Yes | 6 (10.9) |
| No | 49 (89.1) |
| Length of hospital stay, mean ± SD, dayse | |
| Mild | 15.5 ± 3.5 |
| Moderate | 18.8 ± 10.3 |
| Severe | 16.6 ± 5.1 |
| Critical | 8.7 ± 9.0 |
| Death, No. (%) | 4 (7.2) |
Abbreviations: ALT, alanine transferase; ARI, acute respiratory infection; AST, aspartate transferase; CRP, C-reactive protein.
aData were presented as median (min; max) when the distribution was not normal.
bHead trauma, neonatal asphyxia.
canaemia, asthma, malignancy, congenital heart disease, epilepsy.
dacute respiratory distress syndrome, pleural effusion.
elength of hospital stay of one day or less were noted as one day.
Six (11%) of all hospitalized subjects presented with a critical illness at admission. Unfortunately, in our setting, only two critical cases could be transferred to a Pediatric Intensive Care Unit (PICU). Of the four subjects who died, one death occurred while hospitalized at a district hospital without a PICU, and three patients died in the emergency room of a district hospital before referral to a PICU in tertiary hospital; COVID-19 was confirmed using the post mortem nasopharyngeal swab collection. Case information on the children who died is shown in Table 5. All children who died were less than two years of age and with no history of COVID-19 contact. All were diagnosed as severe pneumonia with acute respiratory distress syndrome (ARDS). Three had associated encephalitis (1 subject), acute diarrhea with severe dehydration (1 subject), or pleural effusion (1 subject).
| Characteristics | Case 1 | Case 2 | Case 3 | Case 4 |
|---|---|---|---|---|
| Date of death | 28/4/2020 | 19/05/2020 | 23/05/2020 | 27/06/2020 |
| Place of death | Emergency room | Emergency room | Emergency room | Isolation roomb |
| Length of stay (days) | Less than 1 | Less than 1 | Less than 1 | 4 |
| Age (months) | 6 | 6 | 9 | 15 |
| Sex | Female | Male | Male | Male |
| District | East Lombok | East Lombok | Mataram | Central Lombok |
| History of COVID-19 Contact | None | None | None | None |
| PCR test positive results | Post mortem | Post mortem | Post mortem | On second swab collected |
| Symptoms at admission | Fever, cough, fatigue, dyspnea | Fever, cough, nasal discharge, dyspnea, seizure | Fever, dyspnea, vomiting, diarrhea, fatigue | Fever, cough, fatigue, dyspnea |
| Axillary temperature, °C | 38.8 | 36.8 | 40.2 | 36.6 |
| Respiratory rate, TPM | 50 | 42 | 58 | 62 |
| SpO2 at admission | 90 % (without oxygen) | 99 % (3 lpm, nasal cannula) | 78 % (2 lpm nasal cannula) | 96 % (5 lpm oxygen mask) |
| Degree of severity | Critical | Critical | Critical | Severe |
| Diagnosis | Severe pneumonia | Severe pneumonia, suspicion of encephalitis | Severe pneumonia, acute diarrhea with severe dehydration | Severe pneumonia, pleural effusion |
| Comorbidities | None | None | None | None |
| Complication | ARDS | ARDS | ARDS | ARDS, pleural effusion |
| Nutritional statusc | Normal | Normal | Normal | Normal |
| Laboratory | ||||
| Haemoglobin, g/dL | No data | 10 | 10.5 | 12.7 |
| WBC counts, 103/µL | No data | 12.1 | 7.5 | 47.1 |
| Neutrophil, % | No data | 86.0 | 46.4 | 49.0 |
| Lymphocyte, % | No data | 10.9 | 34.9 | 29.7 |
| Platelets count, 103/µL | No data | 573 | 332 | 1,062 |
| Chest X-ray | Unilateral infiltrate | No data | Bilateral infiltrate | Bilateral infiltrate, pleural effusion |
Abbreviations: ARDS, acute respiratory distress syndrome; PCR, polymerase chain reaction; WBC, white blood cell; TPM, times per minute; lpm, liter per minute.
aNo data: the subjects were so critical and had already died before the blood sample could have been taken (case 1), and before chest X-ray had been performed (case 2).
bThe hospital did not have a pediatric intensive care unit for COVID-19. The subject died in the isolation room before being transferred to referral hospital.
cBased on body weight for age WHO chart.
5. Discussion
To the best of our knowledge, this is the first retrospective study on the characteristics and outcomes of children with COVID-19 from Indonesia that included symptomatic and asymptomatic cases. According to the published data, published on July 12, 2020, 6,094 (8.05%) of 75,699 reported COVID-19 cases were children. Updated data on December 31, 2020 showed increased proportions to 84,539 (11.5%) of 735,124 cases (3, 10). In the West Nusa Tenggara Province, of 1,571 COVID-19 cases detected up to July 2020, 146 (9.29%) were children. During the same period, there were 539 children hospitalized for suspected COVID-19 according to the national guidelines; 55 (10.2%) of them were eventually COVID-19 confirmed by RT-PCR. As of December 31, 2020, 485 of 5,725 COVID-19 cases in the West Nusa Tenggara were children (11).
The proportion of COVID-19-confirmed cases in children in West Nusa Tenggara is higher than reports from other countries. A systematic review of 45 relevant scientific papers (mostly studies from China and a few reports from Italy, Iran, or South Korea) revealed that children have accounted for 1-5% of all COVID-19 cases (1). Overall, children have represented 2% in China, 1.2% in Italy, 5% in the United States, and 4% of confirmed COVID-19 cases in Australia (1, 12-14). However, the proportion of COVID-19 cases in children in West Nusa Tenggara is lower than reported by a retrospective study by Dong et al. from the first two months of the COVID-19 pandemic in China. Of 2135 pediatric cases, they found 728 (34.1%) laboratory-confirmed cases and 1407 (65.9%) suspected cases (15). This might happen because China is the source of pandemic, and they performed massive screening of all children that were exposed or lived in an epidemic area (i.e., Hubei province) and also included some non-epidemic areas.
During our study period, the number of asymptomatic subjects was slightly higher (76, 52%) than symptomatic subjects. This finding differs from other studies that found a lower proportion of asymptomatic cases, such as Ding et al. (17.4%), de Souza et al. (14.2%), Hoang et al. (19.3%), Guo et al. (5.9%), and Dong et al. with 4.4% (5, 15-18). The higher proportion of asymptomatic cases in our study can be attributed to the relatively older age of asymptomatic subjects or testing practices, as most had a history of COVID-19 contact, detected via contact tracing of family clusters from a confirmed case, and were tested as part of contact tracing. Transmission among family members was similar to that reported in a systematic review of pediatric patients with COVID-19, which found that 66% were diagnosed after their family members were confirmed to be infected with SARS-CoV-2 (18). Another study found that the most common source of transmission was the parent, considered as the index case for 324 (56%) infections in children (12). Wu et al. found that 65 (out of 68) (96%) pediatric patients with COVID-19 were household contacts of adults (19).
In our study, COVID-19-confirmed subjects were predominantly male, and their age ranged from 1 day to 213 months old, with a median age of 84 months. There were also three COVID-19 cases in neonates (3, 4, and 5 days of age, respectively) born to COVID-19 confirmed mothers. This finding suggests that children of all ages were susceptible to SARS-CoV-2, although the evidence of vertical intrauterine transmission was scarce (1). The subjects' median age of seven years was similar to Dong et al. and Guo et al.'s studies, while Gotzinger et al. and Kim et al.'s studies found the median age of five and eight years, respectively. Slightly higher male proportions were also seen in other studies (12, 15, 18, 20).
Fever, cough, and fatigue/malaise were the most frequent clinical manifestations at admission in symptomatic subjects in our study. Ding et al., Guo et al., Hoang et al., Kim et al., de Souza et al., Wu et al., and Zhang et al. also mentioned fever and cough as predominant symptoms (5, 16-21). Similar to other previous studies, we also reported gastrointestinal symptoms, such as nausea/vomiting, diarrhea, and abdominal pain (2, 6, 16-18, 20, 21).
Most symptomatic hospitalized COVID-19 subjects were in severe (n = 43 or 78%) or critical (n = 6 or 11%) condition, and all of them were diagnosed with pneumonia. Oxygenation, fluid support, and empirical antibiotics are recommended by the WHO guidelines for pneumonia in children (22). Hospitalized subjects were significantly younger than non-hospitalized subjects. Most of them were less than five years of age, with a median age of 15 months, and had no history of COVID-19 contact. This finding is different from the study by de Souza et al. that found 145 (36.9%) children with COVID-19 were diagnosed with pneumonia and 43 (10.9%) with upper airway infections (16). We had quite a high proportion of COVID-19 subjects with pneumonia because, from the beginning of the pandemic in Indonesia, all patients hospitalized with lower respiratory tract infection in our province were suspected of having COVID-19 infections, even without a history of COVID-19 contact. In our province, many adults were not disciplined in implementing the COVID-19 restrictions and continued to bring out their children to public places. A study by Zhang et al. also found that about 48% of cases had no history of exposure to an identified COVID-19 source (21).
In the present study, 55 (37.7%) of all COVID-19 subjects were hospitalized, and only 16 of them (29%) had comorbidities. This finding is similar to studies by Gotzinger et al., Kim et al., and Zhang et al., which found 145 (25%), 6 (18%), and 222 (38.5%) subjects had pre-existing medical conditions respectively (12, 20, 21). The hospitalized group showed significantly higher respiratory rates and temperatures and lower oxygen saturation on admission. Laboratory results showed lower hemoglobin levels and higher WBC counts at admission, but there was no difference in WBC differential counts or inflammatory markers. These results were similar to other studies showing that elevated inflammatory markers were less common in children, and lymphocytopenia seemed rare (1, 2, 17). There was no chest CT scan performed in this study. Our national guidelines do not recommend to perform chest CT scan routinely, except for certain indication. Echocardiography was performed only for subjects suspected to have congenital or acquired heart disease. However, we performed chest X-rays for hospitalized subjects and some non-hospitalized subjects. We found that 51% of chest X-rays showed bilateral infiltrate. Various categories have been used in different studies to describe radiographic findings. Kim et al. found 65.7% infiltrate/consolidation, while Hoang et al. found 21% patchy lesion in chest X-rays of COVID-19 pediatric cases (17, 20). Another study revealed 21% local bilateral patchy shadowing by chest CT-scanning (2).
Almost 90% of all subjects in this study had complete isolation at the end of the study. However, a longer duration of PCR conversion may be caused by placement in district central quarantine facilities or self-isolation at home, where PCR testing as part of the COVID-19 health protocol could not be applied on time.
Most pediatric COVID-19 cases presented mild to moderate clinical features, and only a few develop severe or critical diseases (0.6% and 0.3%, respectively) (18). There were six (4.1%) critical subjects in our study, three of them died in this study period. One patient who was admitted with severe COVID-19 and pleural effusion died. This represents four (4.9%) (out of 81) deaths that occurred in COVID-19-confirmed cases in the West Nusa Tenggara Province, and 2.7% of total children with COVID-19 in the study period. This case fatality rate was higher than that reported by de Souza et al. (1.2% critical cases and only one death) and Ding et al. (almost 0% critically ill) (5, 16). One of the fatalities had severe pneumonia with pleural effusion. However, the cause of the pleural effusion might be related to other comorbidities such as TB, as clinical work up in this subject was not completed because the subject died before pleural fluid analysis and other laboratory examinations could be done.
In the present study, all deaths occurred in children diagnosed with severe pneumonia with ARDS. This is similar to a study on 48 children with COVID-19 in North America PICUs, which found 35 (73%) patients presented with respiratory symptoms, and two of them died (6). In our province, the only General Hospital of West-Nusa-Tenggara Province, the tertiary hospital, has a PICU with limited capacity. We believe that only one tertiary hospital PICU is not sufficient for referrals of severe COVID-19 cases from 10 districts. The findings might help the local government to formulate strategies and to improve facilities for further treatment of pediatric COVID-19.
This study has several strengths. First, this is the first retrospective study of COVID-19 from Indonesia, an Asian country outside of China, that included all confirmed COVID-19 cases in children and adolescents from the beginning of the pandemic. Second, it is important to highlight that this study has captured data from children and adolescents who were managed both within the hospital and outside hospital settings, including district central quarantine and self-isolation, respectively.
Our study has some potential limitations. First, this study only covered a brief 4-month period at the beginning of the COVID-19 pandemic in Indonesia. Second, we were unable to assess more details about clinical characteristics of asymptomatic and non-hospitalized children with COVID-19 because these data were unavailable at the time of analysis. Third, there was substantial variation in the duration of time to repeat the nasopharyngeal swabs for evaluation and discontinuation of isolation. This variation is due to several reasons, such as limitations in RT-PCR capacities and facilities, local protocols used in different district hospitals, and that some subjects were isolated outside the hospital. Fourth, inter-observer bias may occur because nasopharyngeal samples were taken by different persons, and RT-PCR was performed in five different laboratories. However, all staff involved in nasopharyngeal swab collection and testing had been trained by West Nusa Tenggara Province Health Office, with external quality control performed by the Agency of Health Research and Development, Ministry of Health. Fifth, some children were still in isolation at the end of our study. To gain a better understanding of COVID-19 in children, a multicenter study conducted over a longer study period should be conducted, with detailed patient information, particularly on clinical manifestations and outcomes.
5.1. Consclusions
This study describes COVID-19 cases in children in West Nusa Tenggara Province, Indonesia, early in the pandemic. Most symptomatic COVID-19 children were less than five years of age, presented with severe pneumonia, and had no history of COVID-19 contact. Although most children recovered, four subjects died, all of whom were diagnosed with pneumonia with acute respiratory distress syndrome. This preliminary study also provides important data for performing larger and more extensive studies on children with COVID-19 infection. The findings from this study might be useful for formulating strategies and guidelines for the prevention and treatment of pediatric COVID-19 in the future. Continued tracking of SARS-CoV-2 infections among children by contact tracing from affected family members and suspected COVID-19 cases based on national guideline are important to characterize the morbidity and mortality.