1. Background
The pandemic of severe pneumonia caused by severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) has emerged since December 2019 (1). The first corresponding cases originated in Wuhan, China, and rapidly spread to other countries (2). Symptoms in adults with severe COVID-19 typically present during the second week of illness, when viral loads have decreased, and laboratory evidence of inflammation has increased (3). These observations show that dysregulated innate and adaptive immune responses have a crucial role in the severity of the condition (4). However, most children and adolescents with SARS-CoV-2 infection have mild COVID-19 (5).
The National Health Service (NHS) issued a warning in April 2020 that a multisystem inflammatory syndrome in children (MIS-C) could be linked to COVID-19, presenting with cardiovascular shock, fever, and hyper inflammation (6). MIS-C case definitions vary but generally include the age younger than 21 years, persistent fever, multi-organ dysfunction, laboratory evidence of inflammation, lack of an alternative diagnosis, and prior SARS-CoV-2 infection (7). Many factors, including being overweight, asthma, and ethnic origin, black or Asian, may be risk factors for MIS-C (8).
In the published case series, many patients with MIS-C have had some clinical and paraclinical presentations similar to those of Kawasaki disease (6, 9). Some patients also presented with the characteristics of toxic shock syndrome or macrophage activation syndrome (10). MIS-C is a syndrome presenting with fever and organ involvement but without pathognomonic findings or diagnostic tests (11). Unlike Kawasaki disease, MIS-C reportedly mainly occurs in adolescents and children older than five years of age (6, 12).
2. Objectives
Knowledge of demography, clinical course, para clinical data, treatment, and prognosis of MIS-C can contribute to the better management of the patients and, as a result, reduced mortality and morbidity rates. This study summarized the demographical and clinical characteristics of 75 children with MIS-C in Shiraz, southern Iran.
3. Methods
In the present observational and retrospective study, we included people under 18 years of age, from September 22, 2020, to March 10, 2021, in Namazi hospital, Shiraz, Iran, with a diagnosis that met the MIS-C definition criteria. The case definition included seven criteria: Age < 21 years, severe diseases leading to hospitalization, fever lasting for at least 24 hours, laboratory markers of significant inflammation, one or more organ involvement, proof of infection with SARS-CoV-2 based on RT-PCR, antibody testing, exposure to a person with COVID-19 in the past month, and lack of an alternative diagnosis. Inclusion criteria in our study were the same as diagnostic criteria for MIS-C, and the exclusion criteria were age >18 and no consent to participate.
4. Results
We included 75 children who met the criteria for confirmed MIS-C in the study. The median age was 6.2 years (interquartile range, 1 to 16), with 44 (58.6%) males. Thirty-five patients (46%) had positive tests for SARS-CoV-2 RT-PCR, antibody testing, or both, and 30% had a history of contact with COVID-19 cases. Three patients had a personal account of COVID-19, with an average time of four weeks between COVID-19 infection and the onset of MIS-C symptoms (Table 1).
| Characteristics | Values |
|---|---|
| Age (y), median | 6.2 (1 - 16) |
| Male sex | 44 (58.6) |
| Positive SARS-Cov-2 PCR test | 1 (1.3) |
| Positive SARS-Cov-2 antibody test | 32 (42.6) |
| Positive SARS-Cov-2 PCR or antibody test | 33 (44) |
| Positive SARS-Cov-2 PCR and antibody test | 2 (2.6) |
| Contact a person with COVID-19 | 23 (30.6) |
| A history of COVID-19 | 3 (4) |
a Values are expressed as No. (%) unless otherwise indicated.
Imaging and echocardiographic results (Table 2)
| Variables | No. (%) |
|---|---|
| Abdominal free fluid | 17 (22) |
| Hepatitis | 1 (1.3) |
| Stasis in kidneys | 1 (1.3) |
| First-day echocardiography | |
| Tricuspid regurgitation | 58 (77.3) |
| Mitral regurgitation | 36 (48) |
| Abnormal LV function | 15 (21) |
| Myocarditis | 1 (1.3) |
| Second echocardiography | |
| Tricuspid regurgitation | 33 (44) |
| Mitral regurgitation | 23 (30) |
| Abnormal LV function | 5 (6) |
None of the patients had organomegaly in abdominopelvic sonography. Abdominal free fluid was present in 17 patients (22%). One patient had hepatitis, and one had stasis in both kidneys. On the first day of echocardiography, 77% of patients had tricuspid regurgitation, of which 44% was trivial, 21% were mild, and 12% were moderate. In addition, 48% had mitral regurgitation, of which 10.7% was trivial, 26.7% was mild, and 10.7% was moderate. Also, 21% had abnormal LV function, of which 4% was poor, and one patient had myocarditis. After 5 - 7 days, repeated echocardiography revealed 44% of patients with tricuspid regurgitation, of which 30.7% were trivial, 12% were mild, and 1.3% were moderate. Moreover, 30% had mitral regurgitation, of which 24% was trivial, and 6% was mild. Finally, 6% had abnormal LV function, of which 2.6% were poor.
Moreover, 18% of the patients received inotropes (digoxin, dopamine, and dobutamine), 60% ASA, 32% IVIG, 84% glucocorticoid (methylprednisolone 2 mg/kg/day IV), and 25.3% received furosemide. Antibiotics were used for all the patients, whereas remdesivir and tocilizumab were not used. Eighteen patients (24%) cared for in an intensive care unit, and five cases (7.4%) required invasive mechanical ventilation. Seventy-three patients (97.4%) recovered, and two patients (2.6%) died (Table 3).
| Parameters | No. (%) |
|---|---|
| Antibiotics | 75 (100) |
| Glucocorticoid | 63 (84) |
| Aspirin | 45 (60) |
| Intravenous immunoglobulin (IVIG) | 24 (32) |
| Furosemide | 19 (25.3) |
| Inotropes | 14 (18) |
| ICU admission | 18 (24) |
| Mechanical ventilation | 5 (7.4) |
| Mortality | 2 (2.6) |
| Discharged from hospital | 73 (97.4) |
5. Discussion
This survey reported one of the first series of patients from Iran with MIS-C, of whom 3% died and 24% required admission to PICU. The median age of 6.2 years in our population is similar to other reports (13-15). Unlike a previous report (16), none of the patients in our study was under one year old. Clinical guidelines recommend assessing antibodies and PCR to diagnose MIS-C due to the high quantity of patients with MIS-C and negative COVID-19 PCR results (12). Also, 41% of the patients had negative PCR results and positive SARS-CoV-2 antibody tests, emphasizing the role of measuring SARS-CoV-2 antibody in MIS-C diagnosis. Furthermore, in patients with atypical manifestations of MIS-C, positive antibody results should be considered to enhance clinical recognition of this condition (17). It should be noted that the percentage of the patients with positive SARS-CoV-2 antibody tests in our study was lower than that in other studies, which may be due to the reasons, such as poor quality of kits or very early checking of SARS-CoV-2 antibodies. Also, the use of a set of inflammatory markers, hypercoagulability tests, and organ damage indicators (e.g., CRP, ferritin, D-dimer, cardiac enzymes, liver enzymes, and creatinine) would be helpful in the early identification of this COVID-19-associated condition (17).
In the present study, the mean level of inflammatory markers (CRP, ESR, procalcitonin, and ferritin) was significantly higher than usual (Table 4). It should be noted that in the studied population, unlike other provocative tests, WBC counts were variable from 2700 to 31200.
Among the enrolled patients, many came to the hospital late; the median time from the onset of MIS-C symptoms was 7.7 days, which shows delayed referral of patients compared to previous studies (18-20). These findings also reinforce the need to educate parents and physicians regarding the early diagnosis of the disease.
| Tests | Values |
|---|---|
| Mean white blood cell count (cell/mL) | 9600 |
| Mean hemoglobin level (g/dL) | 12.8 |
| Platelet under 100000 µL | 13 (17%) |
| Abnormal troponin (> 0.005 ng/mL) | 31 (41%) |
| Abnormal aspartate aminotransferase (AST) level (>33 U/L) | 7 (9.3%) |
| Abnormal alanine aminotransferase (ALT) level (> 40 U/L) | 9 (12%) |
| Hypoalbuminemia (< 3.4 g/dL) | 10 (13.3%) |
| Mean C-reactive protein serum level (mg/L) | 45.55 (IQR, 1 - 202) |
| Erythrocyte sedimentation rate, mm/h | 48 (IQR, 1 - 131) |
| Procalcitonin | 10.1 (IQR, 0.05 - 80) |
| Ferritin | 792.1 (IQR, 1 - 2543) |
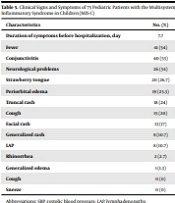
Unlike other studies (19-21), in which gastrointestinal symptoms were the predominant presenting symptoms of MIS-C patients (on average 80% compared to 26% in our study), fever and Kawasaki-like features, like conjunctivitis (53%) and strawberry tongue (26.7%) appeared predominantly as the presenting features of patients in our study. In addition to fever and features of Kawasaki, like conjunctivitis (53%) and strawberry tongue (26.7%), the patients in our study exhibited cough (20%) and neurological problems (34%) (Table 5).
| Characteristics | No. (%) |
|---|---|
| Duration of symptoms before hospitalization, day | 7.7 |
| Fever | 41 (54) |
| Conjunctivitis | 40 (53) |
| Neurological problems | 26 (34) |
| Strawberry tongue | 20 (26.7) |
| Periorbital edema | 19 (25.3) |
| Truncal rash | 18 (24) |
| Cough | 15 (20) |
| Facial rash | 13 (17) |
| Generalized rash | 8 (10.7) |
| LAP | 8 (10.7) |
| Rhinorrhea | 2 (2.7) |
| Generalized edema | 1 (1.3) |
| Cough | 0 (0) |
| Sneeze | 0 (0) |
Abbreviations: SBP, systolic blood pressure, LAP, lymphadenopathy.
MIS-C is significantly associated with cardiac manifestations, including ventricular dysfunction and valvular regurgitation (22). In the present study, the echocardiography performed on the first day of admission of patients demonstrated that 21% had LV dysfunction upon arrival at the hospital, though only 6% of them had LV dysfunction at the time of discharge. These findings may indicate the importance of early hospital care and cardiac consultations during MIS-C to prevent short-term and long-term complications.
Currently, there are some controversies regarding the treatment of MIS-C. In our center, most patients (84%) received glucocorticoids, with IVIG administered to 32% of them. The use of corticosteroids and IVIG could improve the clinical status and reduce the inflammatory process in patients. Antibiotics were used in all cases. Also, 18% of the patients received inotropes, similar to 20% in the Italian cohort (23), and 24% of the patients transferred to the ICU. In contrast with European studies (Riphagen et al. 2020 (6) and Belhadjer et al. 2021 (12)) and an American study conducted by Kaushik et al. 2020 (17), fewer patients in our study required mechanical ventilation (7.4%). Clinical improvement was seen in 97% of cases, and similar to another study (17), 3% died. A noteworthy point in the clinical findings of the two patients who died is that one of them had LV dysfunction and moderate mitral regurgitation at the time of admission, and his heart condition did not improve despite medical treatment, but the other one had normal LV function and trivial mitral regurgitation at the time of admission, and during hospitalization, he developed LV dysfunction. It should be noted that our patient’s mortality rate was relatively higher than that in some other studies, which may be due to our center as a referral center and accepting critically ill patients.
The present study has some limitations: First, misdiagnosis of MIS-C due to the similarity of respective clinical manifestations to those of other viral diseases, and second, the small sample size.