1. Introduction
It has been demonstrated that urinary tract infections (UTIs) are common among hospitalized children, with Escherichia coli as their most frequent cause (1, 2). Among the Enterobacter genus, Enterobacter sakazakii, a ubiquitous bacterium, has been isolated from water, food, and other materials in various regions in hospitals and houses and is considered a new species. This species has been found capable of infecting the bloodstream and central nervous system with a 40 - 80% mortality rate (3, 4).
Premature infants are at a higher risk of acquiring E. sakazakii infections (5). This infection may have been isolated from the contaminated formula of powdered milk. In addition, some other environmental sources may be probably. Also, there is a strong relationship between some reasons for colonization with E. sakazakii and enterocolitis necrotizing (6). Infant formula and other sources of contamination with E. sakazakii may be linked to neonatal infections with this type of infection. Urinary tract infection caused by E. sakazakii is rare, and only one case report was published on a 63-year-old lady with chronic renal failure (7, 8). However, in the present study, we have reported a UTI with E. sakazakii in a 31-month-old boy with posterior urethral valve surgery. However, E.sakazakii can cause bacteremia, meningitis, and necrotizing enterocolitis, but E. sakazakii causes rare literature about UTI.
2. Case Presentation
A 31-month-old boy with a history of posterior urethral valves surgery presented to the emergency department. The surgery was done during the natal period. The first step in treatment was to relieve bladder outlet obstruction by placing a urethral catheter, and then cystoscopic valve ablation or vesicostomy was performed when the child was stable. The patient presented with a history of dysuria, dribbling, and a 24-hour history of fever, chills, and anorexia. At the time of admission, the patient was conscious and irritable. In addition, he had 28 per min of respiratory rate, 120 per min of pulse rate, 95/60 mmHg of blood pressure, and 38.2°C as the temperature. The examination was otherwise normal. The UTI detection was based on U/A and U/C, a colony count of more than 105, and positive nitrite and microscopic hematuria (9). For urine sampling, the patient urinates a small amount into the toilet bowl and then stops the flow of urine. Then, collect a urine sample in a clean or sterile cup until it is half full. Also, we did relieve bladder outlet obstruction by placing a urethral catheter, and then cystoscopic valve ablation or vesicostomy was performed when the child was stable. In the following, we took a urine sample (U/A) for more evaluation and patient investigation. We observed that the collected urine was revealed and turbid with many gram-negative bacilli in gram stain, positive leukocyte esterase, and 4 - 6 RBC/high-power field. A calibrated loop approach was used for urine culture (U/C) on blood agar and MacConkey agar. In addition, inoculated plates were incubated at 37°C for 24 hours and examined for bacterial growth. The organism was identified as E. sakazakii (> 105 cfu/mL), but there was no positive result in blood culture, so based on U/A and U/C, the diagnosis was done (9). The isolate was susceptible to ceftriaxone, gentamicin, and nitrofurantoin (Table 1).
| Variables | Results |
|---|---|
| Blood Test | |
| Leukocyte × 109/L | 11.86 |
| Neutrophils, % | 71 |
| Lymphocytes, % | 20 |
| Hemoglobin, g/dL | 10.5 |
| RBC × 1012/L | 3.82 |
| HCT, % | 30.8 |
| PLT × 109/L | 157 |
| M.C.V f lit | 80.63 |
| M.C.H, pg | 27.49 |
| ESR, mm/h | 51 |
| CRP | 3+ |
| Urea, mg/dL | 40 |
| Cr, mg/dL | 0.8 |
| Na, meq/L | 134 |
| K, meq/L | 4.4 |
| U/A | |
| S.G | 1025 |
| Appearance | Turbid |
| PH | 5.8 |
| Glu | Negative |
| Ketones | Negative |
| Bilirubin | Negative |
| Protein | Negative |
| Nitrite | Positive |
| Leukocyte esterase | Positive |
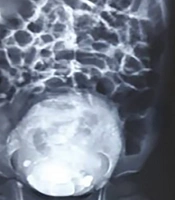
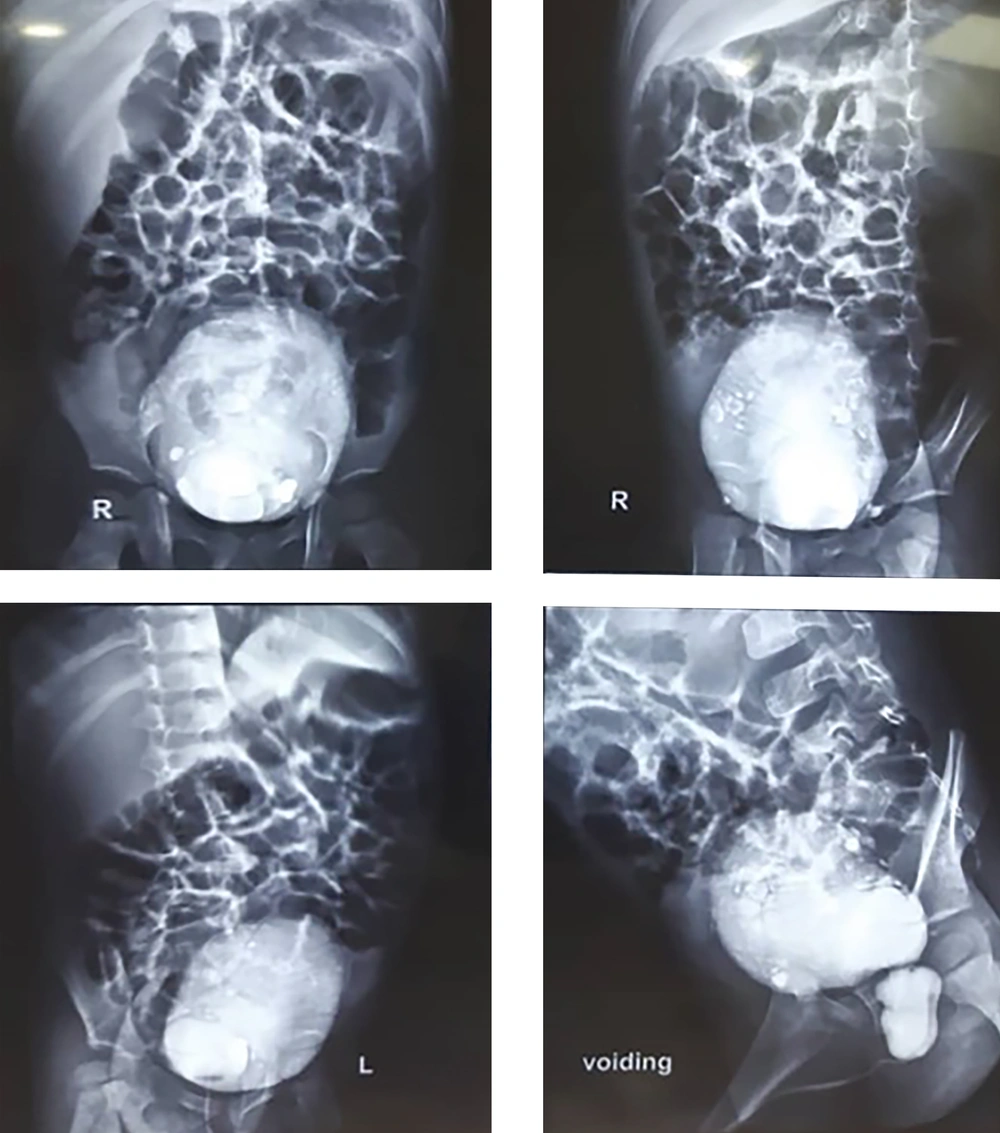
Renal ultrasonography indicated bilateral severe hydronephrosis, bilateral multiple kidney scars, left kidney pyonephrosis, bilateral dilated ureter, the thickness of the bladder, and 70 cc residual urine volume after voiding. In a renal scan with 99mTc-DMSA, we found impairment of global cortical function in both kidneys and bilateral urinary obstruction. In the VCUG report, it is said that the bladder wall has several diverticula, and when urinating, the upper part of the urethra has a v-shaped appearance, and inside it, a lucent fat is seen, which looks like a valve and represents PUV. The PUV have undergone surgery and were follow-up and were normal in our follow-up (Figure 1).
3. Discussion
E. sakazakii has been reported as an invasive infection in infants (10). It has also been isolated from contaminated powdered infant formula. Premature infants are more susceptible to E. sakazakii infection (11). This infection is a bacterial agent capable of surviving in very dry environments. This opportunistic, gram-negative, rod-shaped bacteria can cause bacteremia, meningitis, and necrotizing enterocolitis in children and has also been reported in invasive infantile infections (12). It has also been extracted from contaminated powdered infant formula. Evidence shows that prematurity can increase infants' susceptibility to E. sakazakii infection (10). In another case report, Hayashi et al. mentioned that Enterobacter sakazakii is a rare but important cause of necrotizing enterocolitis, bloodstream infection, and central nervous system infections in humans, with 40 - 80% mortality rates. It has not been reported to cause urinary tract infections (13). However, in a pediatric case, we reported a urinary tract infection due to E. sakazakii.
The presented case did not use a powdered formula and was not premature. Post-urethral valve surgery may increase this patient's susceptibility to infection with E. sakazakii. However, the evaluated cases probably have acquired this infection from an environmental source because many environmental sources have been reported for E. sakazakii. Chronic renal failure (CRF) and impaired immune systems can increase the susceptibility of patients to E. sakazakii infection. While the sources of E. sakazakii are unknown, many environmental places have been reported as sources of infection (3).
3.1. Conclusions
E. sakazakii can cause bacteremia, meningitis, and necrotizing enterocolitis, but there is rare literature about urinary tract infections with E. sakazakii. However, the present study reported a case of urinary tract infection with E. sakazakii in a 31-month-old baby with post-urethral valve surgery. Based on this, we can diagnose, manage, and treat this condition based on the data mentioned in the discussion section.