1. Background
COVID-19, also known as Coronavirus Disease 2019, was first discovered in December 2019 in Wuhan, China (1). The World Health Organization (WHO) designated this novel coronavirus as severe acute respiratory syndrome Coronavirus 2 (SARS-CoV-2) on February 12, 2020. On January 30, 2021, the WHO declared COVID-19 a global public health emergency (2, 3). The spread of SARS-CoV-2, a single-stranded RNA virus, has been rapid worldwide, with a high level of transmissibility (4). Currently, SARS-CoV-2 has affected more than 222 countries. World Health Organization reports indicate that as of March 10, 2024, there have been 774,889,074 confirmed cases of COVID-19 worldwide, resulting in 7,038,623 deaths (https://covid19.who.int/).
In Iran, as of November 26, 2023, a total of 155,460,000 vaccine doses have been administered. Despite vaccination efforts, from January 3, 2020, to April 28, 2024, the COVID-19 pandemic has led to over 7,627,186 confirmed cases and more than 146,811 deaths (https://covid19.who.int/region/emro/country/ir). The primary modes of transmission for SARS-CoV-2 are through respiratory droplets and contact (5).
COVID-19 infection affects all organ systems, including the gastrointestinal tract, neurological system, cardiovascular system, hepatocellular system, pulmonary system, urinary system, and immune system (6, 7). All age groups can be affected by SARS-CoV-2, with older adults (people over 50), immunocompromised individuals, and patients with chronic diseases being the most vulnerable to severe infections (8, 9).
World Health Organization classifies COVID-19 infections as mild, severe, or critical based on clinical symptoms (10, 11). Infants and children generally experience lower rates of COVID-19 infection, with up to 45% either being asymptomatic carriers or having a moderate clinical course of the disease. Children with underlying medical conditions may develop severe COVID-19 infections (12).
The inflammatory response significantly influences the progression of COVID-19, with disease severity and mortality often indicated by hematological and inflammatory parameters (13, 14). Neutrophil-to-monocyte ratio (NMR), lymphocyte count, neutrophil-to-lymphocyte ratio (NLR), C-reactive protein (CRP), platelet-to-lymphocyte ratio (PLR), D-dimer, white blood cell count (WBC), ferritin, fibrinogen, procalcitonin, and levels of various inflammatory cytokines are commonly considered prognostic indicators of COVID-19 severity (15, 16). According to Abdulla et al., patients with severe illness exhibit significant differences in serum levels of IL-6, CRP, and S-ferritin compared to those with mild or moderate illness (11). Yuan et al. demonstrated that severe and critically ill patients often present with lower lymphocyte counts, reduced red blood cells and hemoglobin, and decreased levels of immunoglobulin G antibodies specific to SARS-CoV-2. They also noted elevated levels of D-dimer, fibrinogen, WBC count, neutrophil count, IL-6, CRP, procalcitonin, ESR, ferritin, and LDH in patients with severe or critical illness (14). Alkan et al. found that hospitalized children with COVID-19 frequently have elevated WBC, lymphocyte, and platelet counts, as well as higher RDW, CRP, procalcitonin, D-dimer, and lymphocyte-to-monocyte ratio values (12).
Recognizing the risk factors for severe prognosis in COVID-19 patients is crucial, especially given the absence of standardized treatments and medications (17).
2. Objectives
In the present study, we conducted a retrospective cross-sectional study to investigate the role of hematological parameters in assessing the severity of COVID-19 infection among children admitted to Mofid Children's Hospital, Tehran, Iran.
3. Methods
3.1. Inclusion Criteria
Patients who met all the following criteria were included in the current study: (1) patients without any underlying disease; and (2) patients with a positive COVID-19 real-time PCR test.
3.2. Exclusion Criteria
Patients who met any of the following criteria were excluded from the current study: (1) patients who had underlying diseases; (2) patients who did not undergo hematologic tests; (3) patients with incomplete medical records; and (4) patients with negative real-time PCR tests.
3.3. Study Design
The hematological parameters of children with COVID-19 infection admitted to Mofid Children's Hospital were examined retrospectively from 2019 to December 2022. After reviewing the medical records, all patients' demographic data and clinical information were extracted at admission and discharge from the hospital. The demographic data and clinical information included: Age, gender, pulse rate, respiratory rate, blood pressure, fever, oxygen saturation (SpO2), duration of hospitalization, admission to Intensive Care Units (ICUs), use of a ventilator, mortality rate, WBC count, red blood cell (RBC) count, hemoglobin level (Hb), mean corpuscular volume (MCV), platelet count (PLT), percentages of neutrophils and lymphocytes, red cell distribution width (RDW), erythrocyte sedimentation rate (ESR), CRP, creatine phosphokinase (CPK), lactate dehydrogenase (LDH), ferritin, fibrinogen, aspartate aminotransferase (AST), alanine transaminase (ALT), alkaline phosphatase (ALP), and creatinine.
3.4. Data Analyses
All data were included in SPSS 25 and analyzed using statistical tests. A Mann-Whitney U test was used to compare quantitative variables between patients admitted to the ICU and those hospitalized in general wards. The Fisher exact test was employed to compare qualitative variables between these two groups. Additionally, the relationship between variables and the duration of hospitalization was assessed using the Mann-Whitney U test and Fisher exact test. Multivariable regression modeling was conducted to identify factors predicting the probability and duration of hospitalization for children with COVID-19 in the ICUs.
3.5. Ethic Statements
This study was approved by the Ethics Committee of Shahid Beheshti University of Medical Sciences, Tehran, Iran (IR.SBMU.RICH.REC.1402.004).
4. Results
4.1. Basic Characteristics of the Patients at Admission
Table 1 displays the demographic data and clinical information of patients at admission. There were 408 patients with COVID-19 infection, comprising 219 (57.7%) males and 189 (46.3%) females. The median age of patients was 24 months (ranging from 20 days to 204 months), and 379 patients (92.9%) had fever. Blood pressure increase was observed in 74% (304/408) of patients, while respiratory rate increase was noted in 8.8% (36/408). Elevated levels of WBC and neutrophils were found in 17.7% (72/408) and 74.8% (305/408) of patients, respectively. Hematology tests indicated elevated levels of ESR, CRP, creatinine, and ferritin in 51.7% (185/358), 67.4% (190/282), 69.3% (266/384), and 53.6% (90/168) of patients, respectively. Additionally, high levels of ALP and AST were detected in 98.2% (277/283) and 38.3% (118/308) of patients, respectively.
| Hematological Parameters (Normal Range) | Range | Minimum | Maximum | Mean | Median | Standard Deviation |
|---|---|---|---|---|---|---|
| Age | 20 (day) | 204 (month) | 56.30 (month) | 24 | 57.03 | |
| < 1 month | 10 (2.5) | |||||
| 1 month to < 1 year | 104 (25.5) | |||||
| 1 to <3 years | 94 (23) | |||||
| 3 to < 6 years | 56 (13.7) | |||||
| 6 to <12 years | 85 (20.8) | |||||
| 12 to 18 years | 59 (14.5) | |||||
| Blood pressure (90/60 mmHg and 120/80 mmHg) | 60.30 | 130.88 | 97.22 | 95.65 | 11.45 | |
| Normal level | 104 (25.5) | |||||
| Elevated level | 304 (74.5) | |||||
| Pulse rate (60 to 100 beats per minute) | - | 20 | 190 | 112.38 | 110 | 21.14 |
| Respiratory rate (12 to 60 breaths per minute) | 15 | 85 | 27.97 | 25 | 10.31 | |
| Normal level | 372 (91.2) | |||||
| Elevated level | 36 (8.8) | |||||
| SPO2 (%) (95% to 100%) | - | 75 | 100 | 96.34 | 97 | 2.98 |
| WBC (4.5 to 11.0 × 109/L) | 1.50 | 51.70 | 7.88 | 6.70 | 5.35 | |
| Elevated level | 72 (17.7) | |||||
| Normal level | 267 (65.6) | |||||
| Decreased level | 68 (16.7) | |||||
| RBC male: 4.7 to 6.1 million cells per microliter (cells/mcL) female: 4.2 to 5.4 million cells/mcL | - | 1.91 | 6.54 | 4.28 | 4.30 | 0.62 |
| HB males:14 to 18 g/dL; females: 12 to 16 g/dL | 5.60 | 99 | 11.73 | 11.60 | 4.67 | |
| ≤ 10 | 73 (18) | |||||
| > 10 | 333 (82) | |||||
| MCV (80 – 100 femtoliters) | 7.40 | 108.80 | 81.58 | 80.90 | 8.03 | |
| Elevated level | 32 (7.9) | |||||
| Normal level | 320 (79.4) | |||||
| Decreased level | 51 (12.7) | |||||
| PLT (150,000 to 450,000 platelets per microliter) | 28 | 756 | 276.82 | 254 | 121.63 | |
| Elevated level | 36 (8.9) | |||||
| Normal level | 321 (79.3) | |||||
| Decreased level | 48 (11.9) | |||||
| Neutrophils (%) (40% to 60%) | 2 | 658 | 57.32 | 57 | 36.56 | |
| Elevated level | 305 (74.8) | |||||
| Normal level | 82 (20.1) | |||||
| Decreased level | 21 (5.1) | |||||
| Lymphocytes (%) (20% to 40%) | 3 | 300 | 38.22 | 35.55 | 23.92 | |
| Elevated level | 109 (26.8) | |||||
| Normal level | 196 (48.3) | |||||
| Decreased level | 101 (24.9) | |||||
| RDW (12% to 15%) | 11.30 | 20.40 | 13.62 | 13.20 | 1.54 | |
| ≤ 13 | 141 (38.6) | |||||
| > 13 | 224 (61.4) | |||||
| Reticulocytes (0.5% to 2.5%) | - | 0.20 | 2.30 | 0.68 | 0.55 | 0.53 |
| PT (11 to 13.5 seconds) | 12 | 23 | 12.45 | 12 | 1.19 | |
| Normal level | 111 (95.7) | |||||
| Elevated level | 5 (4.3) | |||||
| INR (0.9 to 1.1) | - | 1 | 2.50 | 1.05 | 1 | 0.16 |
| PTT (25 to 35 seconds) | - | 23 | 80 | 32.48 | 30 | 8.18 |
| ESR (≤ 20 mm/hr) | 2 | 99 | 27.04 | 21 | 20.98 | |
| Normal level | 173 (48.3) | |||||
| >20 | 185 (51.7) | |||||
| CRP (< 0.3 mg/dL) | 4 | 221 | 24.86 | 15 | 25.44 | |
| Normal level | 92 (32.6) | |||||
| Elevated level | 190 (67.4) | |||||
| LDH (160 to 370 units/L) | 3 | 2587 | 669.00 | 609 | 321.27 | |
| Elevated level | 180 (100) | |||||
| Normal level | 0 (0) | |||||
| Fibrinogen (200 to 400 mg/dL) (2.0 to 4.0 g/L) | - | 101 | 801 | 387.13 | 403 | 99.91 |
| Ferritin (7 to 140 ng/mL) | 14 | 800 | 201.66 | 102 | 230.53 | |
| Normal level | 78 (46.4) | |||||
| Elevated level | 90 (53.6) | |||||
| CPK (10 to 120 mcg/L) | 20 | 2058 | 219.09 | 120 | 293.21 | |
| Normal level | 56 (50.5) | |||||
| Elevated level | 55 (49.5) | |||||
| Creatinine (0.7 to 1.3 mg/dL) | 0.19 | 3.39 | 0.68 | 0.64 | 0.24 | |
| Normal level | 118 (30.7) | |||||
| Elevated level | 266 (69.3) | |||||
| AST(8 to 33 U/L) | 10 | 488 | 54.81 | 43.50 | 49.18 | |
| Elevated level | 118 (38.3) | |||||
| Normal level | 63 (20.5) | |||||
| Decreased level | 127 (41.2) | |||||
| ALT (7 to 56 U/L) | - | 8 | 392 | 37.02 | 24 | 44.53 |
| ALP (90 to 340 U/L) | 69 | 2310 | 472.30 | 429.69 | 226.11 | |
| Elevated level | 277 (98.2) | |||||
| Normal level | 5 (1.8) |
Abbreviations: N, number of patients; WBC, white blood cells; RBC, red blood cells; HB, hemoglobin; MCV, mean corpuscular volume; PLT, platelet; RDW, red cell distribution width; PT, prothrombin time; INR, international normalised ratio; PTT, partial thromboplastin time; ESR, erythrocyte sedimentation rate; CRP, C-reactive protein; LDH, lactate dehydrogenase; CPK, creatine phosphokinase; AST, aspartate aminotransferase; ALT, alanine transaminase; ALP, alkaline phosphatase.
a Values are expressed as No%.
4.2. Patients' Hematological Parameters at Discharge
The hematological parameters collected from patients before discharge from the hospital are displayed in Table 2. High levels of WBC, HB, PLT, and creatinine were found in 23.3% (38/163), 74.7% (121/162), 25.3% (41/162), and 50% (13/26) of patients, respectively. Moreover, MCV levels were normal in 85.7% of patients. Results showed that 37.7% (61/162) and 54.3% (88/162) of patients had high levels of neutrophils and lymphocytes, respectively.
| Hematological Parameters | At Discharge | |||||
|---|---|---|---|---|---|---|
| Range | Minimum | Maximum | Mean | Median | Standard Deviation | |
| WBC | 1 | 117 | 9.05 | 7.60 | 9.74 | |
| High | 38 (23.3) | |||||
| Normal | 103 (63.2) | |||||
| Low | 22 (13.5) | |||||
| RBC | - | 2.42 | 7.91 | 4.22 | 4.20 | 0.70 |
| HB | 7 | 17.50 | 11.23 | 11.1 | 1.83 | |
| ≤ 10 | 41 (25.3) | |||||
| > 10 | 121 (74.7) | |||||
| MCV | 62 | 106.05 | 82.08 | 81.70 | 6.15 | |
| High | 12 (7.5) | |||||
| Normal | 138 (85.7) | |||||
| Low | 11 (6.8) | |||||
| PLT | 6.20 | 965 | 341.40 | 306 | 171.78 | |
| High | 41 (25.3) | |||||
| Normal | 105 (64.8) | |||||
| Low | 16 (9.9) | |||||
| Neutrophils (%) | 9 | 94 | 52.45 | 58.35 | 22.13 | |
| High | 61 (37.7) | |||||
| Normal | 28 (17.3) | |||||
| Low | 73 (45.1) | |||||
| Lymphocytes (%) | 4 | 91 | 40.31 | 35 | 21.28 | |
| High | 88 (54.3) | |||||
| Normal | 34 (21) | |||||
| Low | 40 (24.7) | |||||
| Creatinine | ||||||
| Normal | 13 (50) | |||||
| High | 13 (50) | 0.43 | 1 | 0.67 | 0.64 | 0.16 |
Abbreviations: N, number of patients; WBC, white blood cells; RBC, red blood cells; HB, hemoglobin; MCV, mean corpuscular volume; PLT, platelet.
4.3. Changes in Hematological Parameters at Admission and Discharge
Table 3 displays the changes in hematological parameters of COVID-19 patients during admission and discharge from the hospital. Platelet and neutrophil levels were significantly higher at discharge than at admission (P < 0.001), while creatinine levels were significantly lower at discharge (P < 0.001).
| Hematological Parameters | Patients (N) | At Admission | At Discharge | t | df | P-Value |
|---|---|---|---|---|---|---|
| WBC | 163 | 8.55 ± 7.21 | 8.37 ± 4.74 | 0.38 | 162 | 0.70 |
| RBC | 159 | 4.19 ± 0.63 | 4.22 ± 0.70 | -0.79 | 158 | 0.42 |
| HB | 162 | 11.78 ± 7.14 | 11.23 ± 1.83 | 1.00 | 161 | 0.31 |
| MCV | 158 | 81.86 ± 7.03 | 82.09 ± 6.21 | -1.01 | 157 | 0.31 |
| PLT | 161 | 265.36 ± 139.00 | 342.04 ± 172.12 | -5.64 | 160 | < 0.001 |
| Neutrophils (%) | 162 | 59.24 ±19.77 | 52.45 ± 22.13 | 4.46 | 161 | < 0.001 |
| Lymphocytes (%) | 162 | 36.09 ± 27.84 | 40.31 ± 21.28 | -1.93 | 161 | 0.05 |
| Creatinine | 26 | 1.15 ± 0.56 | 0.67 ± 0.16 | 4.49 | 25 | < 0.001 |
Abbreviations: N, number of patients; WBC, white blood cells; RBC, red blood cells; HB, hemoglobin; MCV, mean corpuscular volume; PLT, platelet.
4.4. Hematological Parameters and Severity of COVID-19 Infection
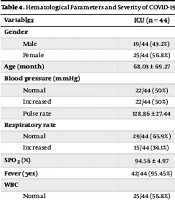
The study parameters were compared between patients admitted to ICUs and those admitted to general hospital wards. See Table 4 for details. Patients admitted to ICUs exhibited elevated levels of pulse rate (P < 0.001), respiratory rate (P < 0.001), MCV (P = 0.01), RDW (P = 0.002), PT (P = 0.006), and ESR (P = 0.04). Additionally, SPO2 levels were lower in patients admitted to ICUs (P < 0.001).
We also evaluated all variables between patients hospitalized for less than one week and those hospitalized for more than one week. Patients hospitalized for more than a week showed increased pulse rate (P = 0.002), respiratory rate (P < 0.001), ESR (P = 0.008), neutrophil percentage (P = 0.02), and lymphocyte percentage (P = 0.01) (see Table 4).
| Variables | ICU (n = 44) | NO-ICU (n = 364) | P-Value | ≤ 1 Week (n = 363) | > 1 Week (n = 45) | P-Value |
|---|---|---|---|---|---|---|
| Gender | 0.15 | 0.11 | ||||
| Male | 19/44 (43.2%) | 199/363 (54.8%) | 200 (55.1%) | 19 (42.2%) | ||
| Female | 25/44 (56.8%) | 164/363 (45.2%) | 163 (44.9%) | 26 (57.8%) | ||
| Age (mo) | 68.03 ± 69.27 | 55.03 ± 55.32 | 0.98 | 55.35 ± 56.06 | 64.03 ± 64.49 | 0.87 |
| Blood pressure (mmHg) | 0.12 | 0.06 | ||||
| Normal | 22/44 (50%) | 82/363 (22.6%) | 87/363 (24%) | 17/45 (37.8%) | ||
| Increased | 22/44 (50%) | 281/363 (77.4 %) | 276/363 (76%) | 28/45 (62.2%) | ||
| Pulse rate | 128.86 ± 27.44 | 110.39 ± 19.37 | < 0.001 | 111.08 ± 20.27 | 122.88 ± 25.03 | 0.002 |
| Respiratory rate | < 0.001 | <0.001 | ||||
| Normal | 29/44 (65.9%) | 342/363 (94.2%) | 342/363 (94.2%) | 30/45 (66.7%) | ||
| Increased | 15/44 (34.1%) | 21/363 (5.8%) | 21/363 (5.8%) | 15/45 (33.3%) | ||
| SPO2 (%) | 94.56 ± 4.97 | 96.56 ± 2.57 | < 0.001 | 96.46 ± 2.82 | 95.42 ± 3.96 | 0.03 |
| Fever (yes) | 42/44 (95.45%) | 336/363 (92.60%) | 0.75 | 55.35 ± 56.06 | 64.03 ± 64.49 | 0.54 |
| WBC | 0.43 | 0.07 | ||||
| Normal | 25/44 (56.8%) | 241/362 (66.6%) | 244/362 (67.4%) | 23/45 (51.1%) | ||
| Increased | 10/44 (22.7%) | 62/362 (17.1%) | 59/362 (16.3%) | 13/45 (28.9%) | ||
| Decreased | 9/44 (20.5%) | 59/362 (16.3%) | 59/362 (16.3%) | 9/45 (20%) | ||
| HB | 0.67 | 0.003 | ||||
| < 10 | 9/44 (20.5%) | 63/361 (17.5%) | 57/361 (15.8%) | 16/45 (35.6%) | ||
| > 10 | 35/44 (79.5%) | 298/361 (82.5%) | 304/361 (84.2%) | 29/45 (64.4%) | ||
| MCV | 0.01 | 0.41 | ||||
| Normal | 29/44 (65.9%) | 290/358 (81%) | 286/358 (79.9%) | 34/45 (75.6%) | ||
| Increased | 9/44 (20.5%) | 23/358 (6.4%) | 26/358 (7.3%) | 6/45 (13.3%) | ||
| Decreased | 6/44 (13.6%) | 45/358 (12.6%) | 46/358 (12.8%) | 5/45 (11.1%) | ||
| PLT | 0.14 | 0.01 | ||||
| Normal | 33/44 (75%) | 288/360 (80%) | 290/360 (80.6%) | 31/45 (68.9%) | ||
| Increased | 2/44 (4.5%) | 33/360 (9.2%) | 34/360 (9.4%) | 2/45 (4.4%) | ||
| Decreased | 9/44 (20.5%) | 39/360 (10.8%) | 36/360 (10%) | 12/45 (26.7%) | ||
| Neutrophils (%) | 0.06 | 0.02 | ||||
| Normal | 5/44 (11.4%) | 77/364 (21.2%) | 79/363 (21.8%) | 3/45 (6.7%) | ||
| Increased | 34/44 (77.3%) | 271/364 (74.5%) | 265/363 (73%) | 40/45 (88.9%) | ||
| Decreased | 5/44 (11.4%) | 16/364 (4.4%) | 19/363 (5.2%) | 2/45 (4.4%) | ||
| Lymphocytes (%) | 0.58 | 0.01 | ||||
| Normal | 23/44 (52.3%) | 173/362 (47.8%) | 79/363 (21.8%) | 3/45 (6.7%) | ||
| Increased | 9/44 (20.5%) | 100/362 (27.6%) | 265/363 (73%) | 40/45 (88.9%) | ||
| Decreased | 12/44 (27.3%) | 89/362 (24.6%) | 19/363 (5.2%) | 2/45 (4.4%) | ||
| RDW | 0.002 | 0.02 | ||||
| < 13 | 7/41 (17.1%) | 134/324 (41.4%) | 133/327 (40.7%) | 8/38 (21.1%) | ||
| > 13 | 34/41 (82.9%) | 190/324 (58.6%) | 194/327 (59.3%) | 30/38 (78.9%) | ||
| PT | 0.006 | 0.08 | ||||
| Normal | 19/23 (82.6%) | 91/92 (98.9%) | 87/89 (97.8%) | 24/27 (88.9%) | ||
| Increased | 4/23 (17.4%) | 1/92 (1.1%) | 2/89 (2.2%) | 3/27 (11.1%) | ||
| ESR | 0.04 | 0.008 | ||||
| Normal | 10/32 (31.3%) | 162/325 (49.8%) | 163/321 (50.8%) | 10/37 (27%) | ||
| Increased | 22/32 (68.8%) | 163/325 (50.2%) | 158/321 (49.2%) | 27/37 (73%) | ||
| CRP | 0.10 | 0.83 | ||||
| Normal | 10/30 (33.3%) | 82/252 (32.6%) | 83/252 (32.9%) | 9/30 (30%) | ||
| Increased | 20/30 (66.7%) | 170/252 (67.5%) | 169/252 (67.1%) | 21/30 (70%) | ||
| Ferritin | 0.22 | 0.06 | ||||
| Normal | 10/28 (35.7%) | 68/139 (48.9%) | 69/138 (50%) | 9/30 (30%) | ||
| Increased | 18/28 (64.3%) | 71/139 (51.1%) | 69/138 (50%) | 21/30 (70%) | ||
| CPK | 0.44 | 1.00 | ||||
| Normal | 7/17 (41.2%) | 49/94 (52.1%) | 46/92 (50%) | 10/19 (52.6%) | ||
| Increased | 10/17 (58.8%) | 45/94 (47.9%) | 46/92 (50%) | 9/19 (47.4%) | ||
| Creatinine | 0.02 | 0.03 | ||||
| Normal | 20/43 (46.5%) | 98/341 (28.7%) | 98/340 (28.8%) | 20/44 (45.5%) | ||
| Increased | 23/43 (53.5%) | 243/341 (71.3%) | 242/340 (71.2%) | 24/44 (54.5%) | ||
| Blood culture | 0.24 | 0.05 | ||||
| Positive | 4/36 (11.1%) | 14/265 (5.3%) | 13/264 (4.9%) | 5/37 (13.5%) | ||
| Negative | 32/36 (88.9%) | 251/265 (94.7%) | 251/264 (95.1%) | 32/37 (86.5%) | ||
| AST | 0.16 | 0.21 | ||||
| Normal | 9/34 (26.5%) | 54/274 (19.7%) | 52/271 (19.2%) | 11/37 (29.7%) | ||
| Increased | 16/34 (47.1%) | 102/274 (37.2%) | 103/271 (38%) | 15/37 (40.5%) | ||
| Decreased | 9/34 (26.5%) | 118/274 (43.1%) | 116/271 (42.8%) | 11/37 (29.7%) | ||
| ALK | 0.08 | 0.08 | ||||
| Normal | 2/30 (6.7%) | 3/252 (1.2%) | 3/252 (1.2%) | 2/30 (6.7%) | ||
| Increased | 28/30 (93.3%) | 249/252 (98.8%) | 249/252 (98.8%) | 28/30 (93.3%) |
a Values are expressed as mean ± SD.
4.5. Risk Factors (Predictor Factors) for the ICU Admission
Pulse rate (odds ratio: 0.95) and respiratory rate (odds ratio: 5.42) were associated with a higher risk of ICU admission due to COVID-19 (Table 5). Additionally, we observed that respiratory rate (odds ratio: 0.16) and hemoglobin level below 10 (odds ratio: 4.23) were associated with a higher risk of ICU admission lasting more than a week (Table 6).
| Independent Variables | Wald | df | Sig | Exp (B) | 95% CI for Exp (B) | |
|---|---|---|---|---|---|---|
| Upper | Lower | |||||
| Pulse rate | 6.22 | 1 | 0.01 | 0.95 | 0.99 | 0.92 |
| Respiratory rate | 4.64 | 1 | 0.03 | 5.42 | 25.27 | 1.16 |
| SPO2 (%) | 1.25 | 1 | 0.26 | 1.11 | 1.33 | 0.92 |
| MCV | 0.54 | 1 | 0.46 | 0.49 | 3.20 | 0.07 |
| RDW | 1.02 | 1 | 0.31 | 2.10 | 8.86 | 0.49 |
| PT | 0.87 | 1 | 0.35 | 4.43 | 101.49 | 0.19 |
| ESR | 0.004 | 1 | 0.44 | 0.95 | 3.86 | 0.23 |
| Creatinine | 0.58 | 1 | 0.47 | 0.58 | 2.27 | 0.15 |
| Independent Variables | Wald | Df | Sig | Exp (B) | 95% CI for Exp (B) | |
|---|---|---|---|---|---|---|
| Lower | Upper | |||||
| Pulse rate | 1.04 | 1 | 0.30 | 1.01 | 0.99 | 1.03 |
| SPO2 (%) | 0.08 | 1 | 0.77 | 1.01 | 0.90 | 1.15 |
| Respiratory rate | 14.75 | 1 | < 0.001 | 0.09 | 0.02 | 0.31 |
| RDW | 1.03 | 1 | 0.30 | 0.59 | 0.21 | 1.62 |
| ESR | 0.26 | 1 | 0.60 | 0.77 | 0.29 | 2.04 |
| Creatinine | 0.75 | 1 | 0.38 | 1.54 | 0.57 | 4.15 |
| Neutrophils | 1.19 | 1 | 0.27 | 0.23 | 0.01 | 3.71 |
| Lymphocytes | 0.35 | 0.55 | 1.39 | 0.46 | 4.17 | |
| PLT | 6.81 | 1 | 0.59 | 0.22 | 0.07 | 0.69 |
| HB | 4.91 | 1 | 0.02 | 3.23 | 1.14 | 9.15 |
5. Discussion
The present study focused on analyzing and summarizing the clinical parameters in children diagnosed with COVID-19 infection at admission and discharge. Our analysis of the patients' basic characteristics at admission revealed that 92.9% of patients had a fever. Additionally, 74% of patients showed an increase in both blood pressure and respiratory rate, and 74.8% of patients had elevated levels of neutrophils. According to previously published studies, typical symptoms of COVID-19 infection include fever, cough, dyspnea, malaise, fatigue, and sputum production (1, 18-20). Results from hematology tests showed that 51.7%, 67.4%, 69.3%, and 53.6% of patients had elevated levels of ESR, CRP, creatinine, and ferritin, respectively. Among the liver function tests, 98.2% of patients were found to have high levels of ALP enzyme.
Our analysis of hematological parameters before discharge from the hospital revealed that 23.3%, 74.7%, 25.3%, and 50% of patients had high levels of WBC, HB, PLT, and creatinine, respectively. Moreover, 85.7% of patients had a normal level of MCV, and 54.3% of patients had a high percentage of lymphocytes.
Several studies have examined the clinical and laboratory parameters of COVID-19 since December 2019. Alkan et al. analyzed hematological parameters and inflammatory markers in children with COVID-19 infection, finding lymphocytosis as the main hematological abnormality. Their study also noted elevated levels of WBC, lymphocytes, PLT, RDW, CRP, procalcitonin, D-dimer, and lymphocyte-to-monocyte ratio in hospitalized patients (12). Akbeyaz et al. identified cough, fever, and vomiting as common clinical symptoms in children with COVID-19, reporting that patients infected with the Omicron variant had lower hemoglobin and lymphocyte levels but higher D-dimer, INR, prothrombin time, and activated partial thromboplastin time (21). Saleh et al. from Saudi Arabia reported fever as the most frequent clinical symptom among COVID-19 patients (22).
Comparison of hematological parameters during admission and discharge from the hospital revealed significantly higher PLT and neutrophil levels at discharge compared to admission, while creatinine levels were significantly lower upon discharge.
Several studies have examined changes in hematologic parameters during COVID-19. A systematic review conducted by Waleed et al. in Pakistan revealed that patients with COVID-19 infection exhibited increased levels of neutrophils, lactate dehydrogenase, serum ferritin, interleukins (IL-6, IL-2, IL-7), CRP, procalcitonin, TNF-α, D-dimer, and fibrinogen degradation products. Additionally, their study reported decreased levels of thrombocytes and lymphocytes in these patients (13). In another study, Abdulla et al. investigated the relationship between changes in hematological parameters and disease severity in COVID-19 patients. They found that lymphocyte counts decreased in severely ill patients compared to those with mild and moderate symptoms. Moreover, severely ill patients exhibited significantly increased serum levels of IL-6, CRP, and ferritin (11). Bozkurt et al. identified higher body mass index and lower albumin levels as factors associated with postpartum progression of COVID-19 (23). Yuan et al. conducted a study to assess changes in hematological and immunological parameters in COVID-19 patients, revealing that severe and critically ill patients had significantly elevated levels of D-dimer, fibrinogen, WBC count, neutrophil count, IL-6, CRP, procalcitonin, ESR, ferritin, and lactate dehydrogenase (14). A study by Mermutluoğlu et al. in Turkey indicated that COVID-19 patients had elevated levels of mean platelet volume (MPV), neutrophil-to-lymphocyte ratio (NLR), and PLR (15). Matin et al. found that patients with severe COVID-19 infection had lower lymphocyte counts and increased NLR levels compared to non-severe patients (24). Qin et al., in a systematic review and meta-analysis, investigated immune dysfunction parameters in COVID-19 patients, noting significantly increased levels of cytokines such as IL-1β, IL-1Ra, IL-2R, IL-4, IL-6, IL-8, IL-10, IL-18, TNF-α, IFN-γ, IgA, IgG, CD4+ T/CD8+ T cell ratio, WBC, neutrophils, PLT, ESR, CRP, ferritin, serum amyloid A, D-dimer, and LDH in severely ill patients or non-survivors (25). In contrast, Uzel et al. found no statistically significant differences in blood parameters between COVID-19 patients with mild or severe clinical symptoms (26).
In this study, we investigated the correlation between hematological parameters, ICU hospitalization, and duration of hospital stay. Our findings revealed that increased pulse rate, respiratory rate, MCV, RDW, PT, and ESR were associated with ICU admission. Additionally, patients admitted to ICUs had lower SPO2 percentages compared to those not admitted. In Iran, Sadeghi et al. demonstrated that initial admission SPO2, hematocrit (HCT), CRP levels, and myalgia predict ICU admission (27). Moradinia et al., also from Iran, identified age, cough, blood oxygen levels, and diastolic blood pressure as factors associated with ICU hospitalization in COVID-19 patients (28). Candelli et al. reported from Italy that blood type A, PaO2/FiO2 ratio, LDH, lactate levels, dyspnea, and SpO2 were significantly linked to ICU admission in COVID-19 patients (29). A study by Hergens et al. in Sweden found that hypertension, obesity, and type II diabetes were all risk factors for ICU admission with COVID-19 (30). Kurniyanto et al. in Indonesia highlighted age ≥ 60 years, obesity, shortness of breath, leukocyte count > 10,000/L, SPO2 < 95%, and moderate-severe COVID-19 as strongly associated with ICU referral (20).
We also found that patients hospitalized for more than a week showed increased pulse rate, respiratory rate, ESR, neutrophil percentage, and lymphocyte percentage. Furthermore, these patients had hemoglobin levels above 10 and RDW levels above 13. Mermutluoğlu et al. from Turkey identified a positive correlation between hospitalization duration and fifth-day D-dimer and ferritin levels. They also noted a negative relationship between hospitalization duration and lymphocyte counts on admission day and the fifth day, suggesting that elevated ferritin and D-dimer levels and decreased lymphocyte counts may prolong hospital stays for COVID-19 patients (15). Alkan et al. reported a positive correlation between elevated WBC and procalcitonin levels and hospitalization in children with COVID-19 infections (12). Saleh et al.'s study in Saudi Arabia found that blood group A, hypertension, age < 14 years, and respiratory symptoms were significantly associated with admission to the pediatric intensive care unit (PICU). Their results also indicated that higher levels of factor VIII and fibrinogen were linked to longer hospital stays (22).
However, our study has several limitations: (1) A significant number of patients' clinical information at discharge was inaccessible, preventing a comprehensive analysis of all parameters; (2) Patients were not categorized based on the severity of their illness, limiting our ability to analyze differences between mild and severe COVID-19 cases; and (3) We lacked access to data on treatment outcomes and mortality rates related to COVID-19.
5.1. Conclusions
The present study identified a statistically significant correlation between pulse rate, respiratory rate, MCV, RDW, PT, ESR, and SPO2 percentage with ICU admission. Hence, these clinical parameters may influence ICU hospitalization. Moreover, these factors could prove valuable in identifying patients at high risk for ICU admission. We observed that increases in pulse rate, respiratory rate, ESR, RDW, neutrophil percentage, and lymphocyte percentage were associated with prolonged hospital stays. However, further studies with larger sample sizes are necessary to ascertain the prognosis and severity of COVID-19 infection in children.