1. Background
Integrons are known to be associated with the capture and dissemination of resistance determinants in gram negative pathogens. These genetic elements harbor a gene (intI) encoding a site-specific recombinase (integrase), which is a recombination site, attI, where the gene cassettes are located, and a promoter located inside intI, which causes gene cassettes to be transcribed. Based on the homology of intI sequence, at least three distinct classes of integrons have been described. Class 1 integrons are the most ubiquitous type within clinical isolates of gram negative bacteria, whereas class 2 and 3 integrons are less frequently detected (1).
Over the last decade, there has been a dramatic increase in the prevalence of extended spectrum β-lactamases (ESBLs). These enzymes are capable of conferring resistance to third-generation cephalosporins (e.g. ceftazidime and cefotaxime) and aztreonam but not cephamycins (e.g. cefoxitin) and carbapenems (2). In addition, ESBL genes are usually found within integrons, which may facilitate the spread of such genetic elements. In fact, the acquisition of ESBL genes by strains containing integrons may increase the emergence of multidrug-resistant pathogens under antibiotic selective pressure (3-5).
Although Escherichia coli are considered to be a part of the intestinal flora of humans, pathogenic E. coli strains can cause diverse gastrointestinal and extraintestinal diseases. Diarrheagenic strains of E. coli can be divided into five main pathotypes based on their virulence markers: enteropathogenic E. coli (EPEC), enteroinvasive E. coli (EIEC), enterotoxigeuic E. coli. (ETEC), enterohaemorrhagic E. coli (EHEC), and enteroaggregative E. coli (EAEC). Among these pathotypes, EPEC remains the major cause of infantile diarrhea in developing countries (6). The pathogen is classified into two subgroups according to the presence of bundle-forming pili (BFP), an adhesin which is a virulence factor of typical EPEC (tEPEC), but it is absent from atypical EPEC (aEPEC). Unlike tEPEC, aEPEC is more widespread in industrialized countries. However, recent researches emphasize their growing prevalence in developing regions (7). In Iran, EPEC is considered to be one of the main causes of diarrhea among children. However, recent studies have revealed a gradual decline in the prevalence of EPEC due to improved hygiene standards and sanitation. Some of these studies have reported prevalence rates of EPEC which varies between 3.7% and 9% in Tehran (8, 9).
2. Objectives
Information regarding the occurrence of antimicrobial resistance in pathogens should be considered in clinical management, when optimal treatment is needed. Numerous studies have examined the distribution of integrons in ESBL-producing E. coli strains (10-13). Despite this, there is a paucity of epidemiological data on the occurrence of integrons as well as ESBLs among EPEC isolates. Therefore, the aim of this study was to investigate the prevalence of integrons and ESBLs in EPEC strains isolated from children with diarrhea in Tehran, Iran.
3. Patients and Methods
3.1. Bacterial Isolates and Identification
A total of 413 E. coli isolates were obtained from 363 stool samples (one stool per patient) from children less than 10 years-of-age. These patients had already been admitted to three pediatric hospitals in Tehran, from September 2011 to January 2013. The children suffered from acute diarrhea and had evidence of more than three episodes of watery, loose, or bloody stools per day. Briefly, after gross and microscopic examinations, the stool specimens were cultured on MacConkey agar and xylose-lysine desoxycholate agar (Merck, Germany). The cultured plates were incubated at 37°C for 24 h till growth occurred. Up to five lactose-fermenting colonies were selected separately and subjected to routine biochemical tests. Genomic DNA was prepared by boiling each E. coli isolate. PCR for the eae gene was performed to confirm the identification of EPEC isolates using an Eppendorf thermal cycler (Eppendorf AG, Germany) (14). The PCR amplification was performed in a reaction mixture with a total volume of 25 μL, containing 20 μL distilled water, 50 ng of template DNA, 2.5 μL of 10X Taq polymerase buffer, 0.4 μL dNTPs (10 mmol/L), 1 unit of Taq DNA polymerase 1.5 mmol/L MgCl2, and 0.4 mmol/L of each primer. The PCR program consisted of an initial denaturation at 94°C for 4 min, followed by 35 cycles of denaturation at 93°C for 30 s, annealing at 55°C for 30 s, and extension at 72°C for 30 s, followed by a final extension at 72°C for 4 min. In addition, all of the EPEC isolates were studied for the presence of stx and bfp genes (15, 16). E. coli strains ATCC 2348/9 (eae and bfp) and EDL933 (stx1 and stx2) were used as a positive control. Reactions were performed under the same conditions as described above, except for annealing temperatures (Table 1). PCR products were analyzed by electrophoresis through 1.5% agarose gel and visualized under ultraviolet light after staining with ethidium bromide.
| Gene | Primer Sequence (5' to 3') | Product (bp) | Ta°C |
|---|---|---|---|
| eae | 229 | 55°C | |
| 5'-CTGAACCAGATCGTAACGGC-3' | |||
| 5'-TGATAAGCTGCAGTCGAATCC-3' | |||
| bfp | 324 | 58°C | |
| 5'-AATGGTGCTTGCGCTTGCTGC-3' | |||
| 5'-GCCGCTTTATCCAACCTGGTA-3' | |||
| stx1 | 302 | 55°C | |
| 5'-CGCTGAATGTCATTCGCTCTGC-3' | |||
| 5'-CGTGGTATAGCTACTGTCACC-3' | |||
| stx2 | 516 | 56°C | |
| 5'-CCTCGGTATCCTATTCCCGG-3' | |||
| 5'-CTGCTGTGACAGTGACAAAACGC-3' | |||
| intI1 | 160 | 54°C | |
| 5'-CAGTGGACATAAGCCTGTTC-3' | |||
| 5'-CCCGAGGCATAGACTGTA-3' | |||
| intI2 | 789 | 54°C | |
| 5'-CACGGATATGCGACAAAAAGGT-3' | |||
| 5'-GTAGCAAACGAGTGACGAAATG-3' |
3.2. Identification of Integrons
For detection of the different classes of integrons, PCR was performed for all of the EPEC isolates using specific primers (17) (Table 1). Clinical isolates of E. coli containing integrons were used as positive controls.
3.3. Serogrouping
The confirmed EPEC isolates were further serogrouped by the slide agglutination test using EPEC O-specific polyvalent antisera (Baharafshan Institute of Research and Development, Tehran, Iran). The polyvalent antisera consisted of four separated pools, which were able to react with the following serogroups: polyvalent 1 (O26, O55, and O111), polyvalent 2 (O86 and O127), polyvalent 3 (O44, O125, and O128), and polyvalent 4 (O20 and O114).
3.4. Antibiotic Susceptibility Testing
Antimicrobial susceptibility was determined by the Kirby-Bauer disk diffusion method as per Clinical Laboratory Standards Institute (CLSI) recommendations. The antimicrobial disks (Mast, United Kingdom) used were; ampicillin (10 µg), augmentin (30 µg), cefotaxime (30 µg), ceftazidime (30 µg), cefoxitin (30 µg), tetracycline (30 µg), ciprofloxacin (5 µg), co-trimoxazole (25 µg), and imipenem (10 µg). E. coli ATCC 25922 was used as the quality control.
3.5. Phenotypic Detection of ESBL Producers
The CLSI guidelines for the detection of ESBL producers consist of an initial screening test and a phenotypic confirmatory test. The isolates which showed resistance to at least one of the third-generation cephalosporins (i.e. ceftazidime and cefotaxime) were analysed further using a combined disk. An enhancement in inhibition zone diameter (≥ 5 mm) for either ceftazidime (30 μg) or cefotaxime (30 μg) tested in combination with clavulanic acid, versus its inhibition zone diameter when tested alone, confirmed an ESBL producing organism (2).
3.6. Statistical Analysis
Chi-square or Fisher's exact tests were used for comparison of the categorical data. P-value less than 0.05 was considered to be statistically significant.
4. Results
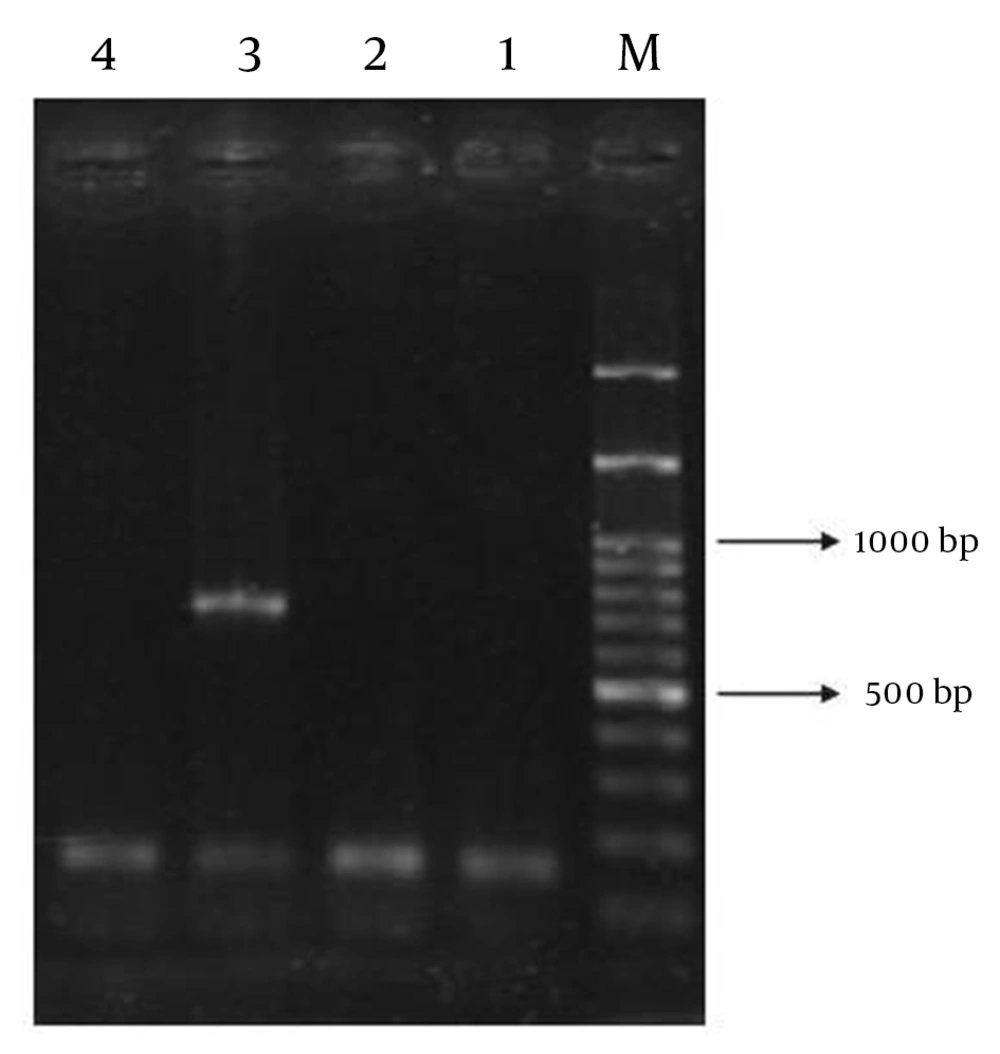
Amongst the 413 isolates of E. coli, 42 were EPEC. The patients comprised 18 (42.9%) males and 24 (57.1%) females, with a female-to-male ratio of 1.3:1. Of the 42 EPEC isolates, 16 (38.1%) were classified as typical EPEC and 26 (61.9%) were classified as atypical EPEC. In addition, integron class 1 was detected in 24 (57.1%) isolates. However, integron class 2 was found to coexist with class 1 in 2 (4.8%) isolates (Figure 1). The most common serogroups among the EPEC strains were found to be members of poly group II (14.3%, n = 6), and poly group III (9.5%, n = 4), whereas the majority of the strains (76.2%, n = 32) were nontypeable (NT) with the polyvalent antisera used. Furthermore, a phenotypic confirmatory test showed that 9 (21.4%) isolates were ESBL producers. Resistance to ampicillin was observed in 26 isolates (61.9%), followed by co-trimoxazole (n = 23, 54.8%), augmentin (n = 18, 42.9%), tetracycline (n = 16, 38.1%), cefotaxime (n = 9, 21.4%), ceftazidime (n = 8, 19%), and ciprofloxacin (n = 7, 16.7%). All of the isolates (100%) were susceptible to imipenem and cefoxitin. No statistically significant associations were observed between integrons and other mentioned categories (Table 2). However, integrons were significantly associated with resistance to certain antibiotics, including co-trimoxazole (P = 0.016), and tetracycline (P = 0.006) (Table 3).
| Features | Number of Isolates | Integron-Positive Isolates, No. (%) | P value |
|---|---|---|---|
| Age group, y | 0.91 | ||
| < 2 | 22 | 12 (54.5) | |
| 2-5 | 13 | 8 (61.5) | |
| > 5 | 17 | 4 (57.1) | |
| Gender | |||
| Female | 24 | 13 (54.2) | 0.65 |
| Male | 18 | 11 (61.1) | |
| EPEC group | 0.46 | ||
| Atypic | 26 | 16 (61.5) | |
| Typic | 16 | 8 (50) | |
| ESBL production | 0.26 | ||
| No | 33 | 17 (51.5) | |
| Yes | 9 | 7 (77.8) |
a Abbreviations: ESBL, extended spectrum β-lactamase; EPEC, enteropathogenic Escherichia coli
| Antibiotic Susceptibility | Integron-Positive Isolates No. (%) | P value |
|---|---|---|
| Ampicillin | 0.93 | |
| Resistant (n = 26) | 15 (57.7) | |
| Sensitive (n = 16) | 9 (56.3) | |
| Augmentin | 0.86 | |
| Resistant (n = 18) | 10 (55.6) | |
| Sensitive (n = 24) | 14 (58.3) | |
| Ceftazidime | 1.0 | |
| Resistant (n = 8) | 5 (62.5) | |
| Sensitive (n = 34) | 19 (55.9) | |
| Cefotaxime | 0.71 | |
| Resistant (n = 9) | 6 (66.7) | |
| Sensitive (n = 33) | 18 (54.5) | |
| Cefoxitin | - | |
| Resistant (n = 0) | 0 (0) | |
| Sensitive (n = 42) | 24 (57.1) | |
| Ciprofloxacin | 0.68 | |
| Resistant (n = 7) | 5 (71.4) | |
| Sensitive (n = 35) | 19 (54.3) | |
| Co-trimoxazole | 0.016 | |
| Resistant (n = 23) | 17 (73.9) | |
| Sensitive (n = 19) | 7 (36.8) | |
| Imipenem | - | |
| Resistant (n = 0) | 0 (0) | |
| Sensitive (n = 42) | 24 (57.1) | |
| Tetracycline | 0.006 | |
| Resistant (n = 17) | 14 (82.4) | |
| Sensitive (n = 25) | 10 (40) |
5. Discussion
The problem of resistance to antimicrobial agents is not unique in Iran, where easy and unrestricted access to antibiotics diminishes the value of such agents for those patients who actually need them. The growing prevalence of resistance genes in enteric pathogens is common in developing countries (18, 19). In our research, high levels of resistance to commonly used antibiotics such as ampicillin and co-trimoxazole were observed in EPEC isolates. This result is in accordance with previous findings from other countries, such as; Vietnam (18), Mexico (20), Argentina (21), Tanzania (22), and Peru (19). Since these antibiotics are widely used to treat diarrhea, it is therefore not surprising that we found higher resistance rates against those antimicrobial agents among our isolates. Compared with other investigations (18, 19, 23), our study showed a higher prevalence of resistance to ciprofloxacin in EPEC isolates. However, in a study conducted by Bakhshi et al., almost all of the isolates were found to be resistant to ciprofloxacin, trimethoprim, and tetracycline (8).
Although imipenem and cefoxitin are not indicated to treat diarrhea, we tested the susceptibilities of EPEC isolates to these antibiotics, since they could be empirically or incidentally used. Fortunately, none of the isolates were resistant to those antimicrobial agents, indicating that these antibiotics are the most effective agents against EPEC isolates.
As previously noted, integrons are frequently reported in clinical isolates of Enterobacteriaceae. It is well known that integrons are able to capture and express gene cassettes encoding certain beta-lactamases. Hence, these genetic elements facilitate the spread of such resistance genes not only within the same species, but also to other genera (3). In Iran, previous studies reported that prevalence rates of integrons in E. coli range from 27.1% to 44.8% (24-26). However, these studies have mainly focused on E. coli strains other than diarrheagenic pathotypes. In our study, the existence of class 1 integrons was confirmed in 57.1% of the EPEC isolates. By contrast, Najibi et al. reported a higher rate of class 1 integrons (82%) among EPEC isolates (27). Like other investigations, we found that the class 1 integron was more prevalent than those of class 2 (24-26). We also showed that the presence of integrons was independently associated with resistance to co-trimoxazole and tetracycline. Resistance to co-trimoxazole could be directly related to the presence of sul and/or dfr genes within the integrons, while the association of tetracycline with the presence of an integron is likely to be due to tet genes which have been found on R-plasmids or transposons and cotransferred along with their respective integrons (28). Nevertheless, for better elucidation of these associations, sequencing of gene cassettes within integrons should be performed.
As for ESBL detection and resistance to third-generation cephalosporins, our result showed a low incidence of ESBL production among EPEC isolates, which contrasts
with that of other studies (18, 20). However, Alikhani et al. reported a much higher rate of resistance to cefotaxime (73.6%) among EPEC strains (23). Although previous studies have shown the association of ESBL genes with class 1 integrons (3, 29, 30), no significant association was observed between these two categories in this study (P = 0.26) using a Fisher's exact test. This result may indicate that the selection and spread of ESBL genes does not play a major role in integron dispersion, except when ESBL genes are within an integron platform. However, with a small sample size, the data should be interpreted with caution and should not be extrapolated to a larger population, or be used to make broad conclusions. Given the fact that the incidence of ESBLs was low among EPEC isolates, future studies with a larger sample size will yield more accurate results.
In the present study, most of EPEC isolates were not typeable with diagnostic antisera and belonged mainly to the atypical group. Therefore, serogrouping for identification should not be used in laboratories, except as part of outbreak investigations. Because of this, PCR is highly recommended for the proper identification of EPEC (6).
In recent years, the significance of EPEC as the causative agent of diarrhea has declined in the literature. Similarly, our finding is in agreement with other results which showed a decline in the number of diarrheal cases in several regions in Iran, probably due to improvements in hygiene standards (8, 9). It is worth noting that breastfeeding promotion could reduce gastrointestinal infections as milk contains antibodies (e.g. SIgA) which protect the intestinal epithelium against diarrheagenic pathogens. Indeed, the WHO guidelines on diarrhea management recommend continued breastfeeding during episodes of diarrhea. EPEC diarrhea does not usually need antibiotic therapy except for severe cases. On the other hand, asymptomatic carriage of enteric pathogens is very common in developing countries. Multiple factors influence colonization rather than illness, including; host susceptibility (children ages, breastfeeding, nutrition, etc.), bacterial factors (virulence gene content), and environmental factors (poor hygiene) (6). One of the major drawbacks of the current study was that healthy carriers were not involved. Therefore, the prevalence of EPEC among asymptomatic carriers could not be assessed.
In conclusion, our results revealed that class 1 integrons are prevalent among EPEC isolates, regardless of whether or not they produce ESBLs. Without doubt, these isolates will be capable of capturing and expressing new drug resistance determinants. Finally, the emergence of resistant gut pathogens can hinder the appropriate management and treatment of gastrointestinal diseases.