1. Background
Human immunodeficiency virus (HIV) infection, which results in acquired immunodeficiency syndrome (AIDS), is an important global public health problem. A large number of people are infected, and many die from the disease, resulting in a high social and economic impact on the affected countries (1). Despite advances in knowledge concerning the epidemic and public policies for its prevention and treatment, AIDS remains an incurable disease with a fatal outcome (2).
Mother-to-child transmission is the major route of HIV infection in children. Data show that this route of transmission has been responsible for 90% of cases in children aged under 13 years in Brazil (3).
The first case of HIV infection among children in Brazil occurred in 1987 (4). In 1994, the AIDS clinical trials group (ACTG) 076 protocol was found to be effective for prophylaxis related to vertical HIV transmission. The protocol consists of the administration to pregnant women of zidovudine (AZT), alone or in combination, starting from the 14th week of pregnancy; this is followed by a booster injection 4 hours before delivery and the oral administration of AZT to newborns during the first 6 weeks of life in association with artificial baby nutrition. These measures have reduced HIV transmission rates by 67.5% (5). Currently, the use of three antiretroviral drugs is recommended for preventing vertical transmission (4), the rate of which is around 1.2% (6). Table 1 lists some information on the stages of AIDS among children around the world in 2013, according to the report of the joint united nations programme on HIV/AIDS (UNAIDS).
| Regional | HIV Infected Children, 0 - 14 Years Old | Lethality, % | ||
|---|---|---|---|---|
| Living with HIV | Estimated Number of New Infections | Estimated Deaths From AIDS | ||
| Western and Central Europe and North America | 4,100 (3,600 - 4,700) | < 1,000 (< 500 ≤ 1,000) | < 500 (< 500 - 500) | 12.2 |
| East and Southern Africa | 1.2 million (1.1 - 1.3 million) | 96,000 (76,000 - 120,000) | 68,000 (57,000 - 81,000) | 5.7 |
| Latin America and Caribbean | 37,000 (31,000 - 44,000) | 2,500 (1,800 - 3,700) | 2,300 (1,700 - 3,100) | 6.2 |
| Middle East and North Africa | 10,000 (8,400 - 13,000) | 2,100 (1,600 - 3,000) | 1,100 (< 1,000 - 1,400) | 11.0 |
| West and Africa | 530,000 (430,000 - 60,000) | 76,000 (57,000 - 100,000) | 50,000 (38,000 - 64,000) | 9.4 |
| Eastern Europe and Central Asia | 5,700 (4,800 - 6,900) | < 1,000 (< 500 ≤ 1,000) | < 500 (< 200 ≤ 500) | 8.8 |
| Asia and Pacific | 190,000 (150,000 - 180,000) | 23,000 (18,000 - 26,000) | 14,000 (11,000 - 15,000) | 7.4 |
| Global | 2.0 million (1.7 - 2.2 million) | 200,000 (160,000 - 250,000) | 140,000 (110,000 - 160,000) | 7.0 |
Serological screening for HIV is recommended for all pregnant women in the first trimester of pregnancy. When the mother does not have adequate access to prenatal diagnosis, screening can occur later, and it often only takes place in the third trimester or at delivery; in these cases, a rapid screening for HIV infection should be performed (7). In Brazil, HIV testing has been provided to all parturient women in maternity units since 2001, which allows for diagnosis and preventive measures to reduce the perinatal transmission of HIV (8).
Early diagnosis of vertical HIV infection in infants is vital when it comes to initiating antiretroviral therapy, prophylaxis against opportunistic diseases, and management of infectious and nutritional disorders (9). However, serological diagnosis of HIV infection in children born to HIV-infected mothers should only be carried out 18 months after birth due to the presence of maternal immunoglobulin G (IgG) antibodies, which cross the placenta during pregnancy and remain in the child’s body during that period until complete elimination (10). Children are considered HIV infected when they test positive for proviral DNA or plasma RNA quantification in two different blood samples. In contrast, for a child to be considered noninfected, he or she should present negative test results in two different blood samples or be followed up until all maternal antibodies disappear (7).
It is estimated that the survival of children with perinatally acquired AIDS in Brazil is around 60 months, with an upward trend emerging over recent years. The reduction in mortality rates in Brazilian children is attributed mainly to the effectiveness of antiretroviral therapy (ART), the free distribution and universal access to high-cost drugs, and the expansion of access to early diagnosis and treatment for AIDS and opportunistic infections (11).
2. Objectives
The aim of this study was to describe AIDS and the survival of children from birth to 13 years of age in the state of Santa Catarina, Brazil, between 1988 and 2013.
3. Methods
Santa Catarina is located in southern Brazil. In 2013, the estimated population was around 6.6 million. The state ranks fourth among all 27 Brazilian states in terms of economic development and gross domestic product (GDP) per capita. It has one of the highest levels of education and public health and one of the lowest rates of illiteracy in the country. Between 1980 and 2015, there were 40,307 reported cases of AIDS in Santa Catarina; between 2010 and 2014, the incidence rate was 32.3/100,000 population, which is higher than the national rate.
This was a retrospective cohort study of survival in children aged under than 13 years reported to have HIV infection in the state of Santa Catarina between 1988 and 2013. The cases were selected from the records of HIV infection cases reported by the Information system for notifiable diseases (Sistema de Informacao de Agravos de Notificacao, SINAN) and by the Mortality Information System (Sistema de Informacao sobre Mortalidade, SIM) of Santa Catarina, Brazil. HIV infection was confirmed by the detection of viral RNA in two different samples.
Records with available information regarding the variables of interest of less than 20% and redundant notifications were excluded. Notification records for children whose date of death was the same as the date of AIDS diagnosis, indicating a survival time of zero, were also excluded.
The data of interest registered in SINAN and the mortality database were exported to electronic files and delivered to the researchers. The IBM SPSS (SPSS for Windows v. 20, Chicago, IL, USA) was used for statistical analysis. The mean, median, and standard deviation were calculated for continuous variables, and proportions were determined for categorical variables. The Kaplan-Meier method was used to estimate survival rates. Survival time was estimated according to the time difference between the date in which the databases were received on December 31, 2013 and the date of HIV infection diagnosis. Among those who had died, the time difference between the date of death and date of diagnosis was taken into account to estimate survival rates. This study was submitted to and approved by the research ethics committee of Unisul under protocol number 12.034.4.01 III on May 2, 2012.
4. Results
Of 1,083 cases reported by SINAN, 38 were excluded due to duplication, and complete data were available for 990 patients (91.4%). The sociodemographic and epidemiological characteristics of children with HIV infection and maternal traits are presented in Table 2.
| Characteristics of Children | No. (%) | 95% CI |
|---|---|---|
| Gender | ||
| Male | 485 (49.0) | 45.8 - 54.2 |
| Female | 505 (51.0) | 47.9 - 54.2 |
| Age at diagnosis, mo | ||
| 0 - 27 | 505 (51.0) | 47.9 - 54.0 |
| 28 - 60 | 212 (21.4) | 19.1 - 23.8 |
| > 60 | 273 (27.6) | 24.8 - 30.4 |
| Skin color | ||
| Whites | 455 (46.0) | 42.7 - 49.0 |
| Nonwhites | 59 (6.0) | 4.4 - 7.5 |
| Unknown | 476 (48.1) | 44.9 - 51.3 |
| Exposure category | ||
| Perinatal | 947 (95.7) | 94.3 - 97.0 |
| Transfusion/hemophilia | 8 (0.5) | 0.1 - 0.9 |
| Drugs | 2 (0.2) | 0.0 - 0.5 |
| Heterosexual intercourse | 1 (0.1) | 0.0 - 0.3 |
| Unknown | 32 (3.2) | 2.2 - 4.3 |
| Maternal education, y | ||
| 0 - 8 | 134 (13.5) | 11.5 - 15.5 |
| > 8 | 636 (64.2) | 61.4 - 67.2 |
| Unknown | 220 (22.2) | 19.7 - 24.7 |
The mean elapsed time since diagnosis with HIV infection was 41.6 months (standard deviation [SD] = 40.7), with a median of 26 months, ranging from zero to 160 months from birth.
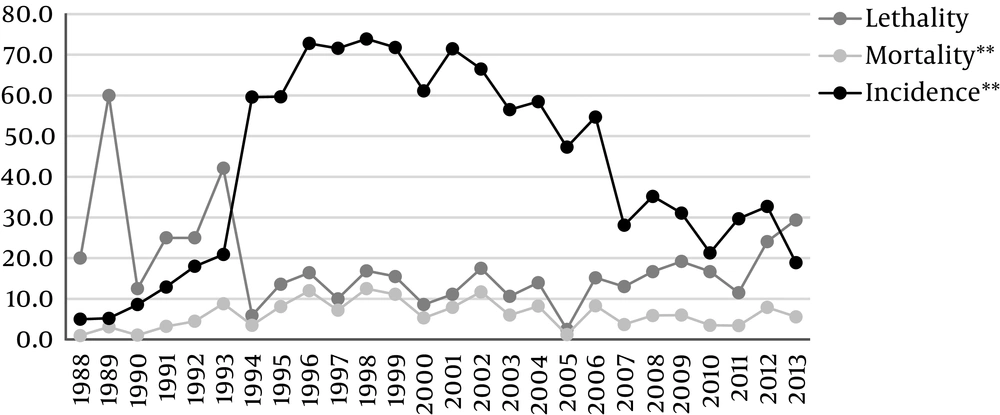
The incidence, lethality, and mortality rates in children were estimated based on the number of live births in the state of Santa Catarina. These data are presented in Figure 1.
The evolution of AIDS among children in the state of Santa Catarina suggests three well-defined periods. The first, between 1988 and 1993, involved relatively low incidence, from 5.0 to 20.9 cases per 100,000 live births (average 11.8 cases per 100,000 live births). This period also showed high lethality (average 30.8%) but low mortality rates (3.6 cases per 100,000 live births). The second period, which was characterized by high incidence (from 47.3 to 73.9 cases per 100,000 live births; average 63.5 cases) occurred between 1994 and 2006. The lethality rate was moderate (12.1%) during that period, as was the mortality rate (7.9 cases per 100,000 live births). The third period, from 2007 onwards, showed an incidence rate between 18.9 and 35.2 cases per 100,000 live births (average 28.1 cases per 100,000 live births), with an increased lethality rate (18.7%) and low mortality rate of 5.1 cases per 100,000 live births.
Regarding the evolution of HIV infection in children reported in the State of Santa Catarina, 844 (85.3% [95% confidence interval (CI): 82.9 to 87.4]) remained alive and 146 (14.7% [95% CI: 12.6 to 17.1]) died. The chance of survival at 60 months was estimated to be 88.1%.
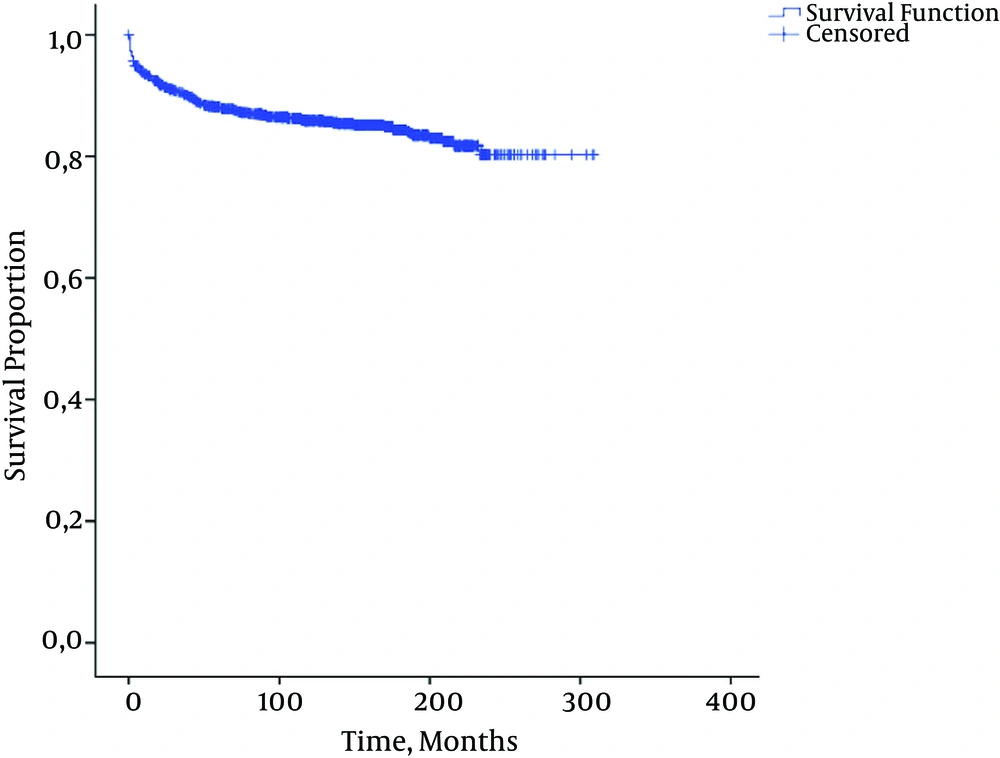
Among those who died, the time between diagnosis and death ranged from 1 to 234 months, with a mean of 39.7 months (SP = 54.0) and a median of 16 months (SE = 4.5). At death, children’s ages ranged from 2 to 319 months, with a mean of 73.8 months (SD = 70.8) and a median of 55 months. Survival was estimated at a mean of 263 months (SE = 3.6; 95% CI: 256.0 to 270.1). Figure 2 shows the survival curve for children who died during the study period.
5. Discussion
The study included the records of 990 children infected with HIV from the beginning of the epidemic in 1988 to 2013 in the state of Santa Catarina. The children were diagnosed at a median of 26 months of age, and 51% of them were female. Vertical transmission was the main route of infection.
Matida et al. (2011) reported that 51.7% of girls were affected with pediatric AIDS (12). However, a study conducted by Soeiro et al. (2011) in Amazon, Brazil found a higher percentage of boys (58%) than girls among children with AIDS (13). Therefore, vertical transmission of HIV infection does not seem to be related to gender. In this study, there was a gender balance in the number of AIDS cases.
A median of 26 months was the time elapsed between birth and HIV diagnosis in most cases (51%), which is consistent with the minimum of 18 months necessary to provide a definitive diagnosis of HIV infection in children. However, the other cases from the sample had late diagnosis, which can be attributed to infections that occurred after birth. It could also be that no screening was performed during prenatal care, and the diagnosis may have been made via the late identification of clinical manifestations of AIDS in the child. In a study conducted by Marques (2002), among 116 HIV-positive pregnant women, 109 (94%) had prenatal care; out of these, 49 (45%) were aware of their HIV-positive condition, 41 (38%) had a diagnosis of HIV infection during the prenatal period, and 19 (17%) were informed of the infection only after their child's birth (14).
The time elapsed between the diagnosis of HIV infection and case notification presented a median of 3 months, and the most plausible hypothesis to explain this was an inadequate use of SINAN data by healthcare personnel. Some deficiencies may have occurred due to misdiagnosis or delayed confirmation tests, carelessness with the mandatory notification, and errors in data collection and data entry, resulting in delays in the registration of AIDS cases. Perinatal transmission was the predominant mode of HIV acquisition (95.7%), consistent with the national profile in which AIDS in children aged less than 13 years old occurs through vertical transmission (92.8%).
We chose to analyze the data in three time periods based on the evolution of the AIDS epidemic in Brazil. The first period is related to the beginning of the AIDS epidemic, which occurred before the epidemiological mother-to-child HIV transmission scenario was determined; at this time, effective pharmacological therapy for the prevention and treatment of AIDS cases was not available. The low incidence should be attributed to the lack of full AIDS diagnosis in children, which reflects great lethality, because AIDS cases were discovered at an advanced stage of the disease, resulting in death. In the second period, there was broad access to diagnostic testing among pregnant women, which reflected an increased incidence with moderate lethality and mortality rates, where the reduction is attributable to the adoption of the ACTG protocol. In the third period, there was a high incidence of AIDS, despite the knowledge about ways to prevent it and national and global measures to combat mother-to-child transmission of HIV. This fact may indicate a lack of adherence to drug therapy, which is free and widely accessible, leading to an increase in mortality rates. In this study, if we analyze only the figures for 2013, the mortality rate was 18.9%, which is much higher than the rates of other regions in the world, as the overall global mortality rate was 7% for that year.
Regarding the group of children who died during the study period, the survival rate was 39.7 months, which is a lower result than that found throughout the literature. In a study comparing different Brazilian regions, the median survival time was 20 months for cases diagnosed up to 1988; this increased to 24 months for cases diagnosed in 1988–1992 and to 50 months for cases diagnosed in 1993 - 1994 (15).
The first national study, conducted in 1983 - 1998, revealed that the probability of 60-month survival among HIV-infected children was 52.8%. The second national study showed a considerable increase, with a survival probability of 86.3% at 60 months (16). Therefore, the 88.1% survival probability at 60 months shown in this study is consistent with the national data. Evidence for the progressive survival time increase includes the success of antiretroviral therapy, free and universal access to treatment, and the improvement of patient attention and monitoring (17).
As mentioned in the methodology section, this study excluded cases in which the date of AIDS-related death was the same of AIDS diagnosis (55 cases); this resulted is in a 5.3% decrease in the percentage of deaths in the sample. However, since these cases were distributed randomly, such exclusion did not interfere with the final results. According to the State of Santa Catarina health surveillance department (DIVE-SC), there are two hypotheses to explain this finding in the database, as follows: Either the AIDS cases were only identified when the cause of death was determined or there was an error in the information system (SINAN), which replicated the date of death and randomly changed the date of diagnosis. According to DIVE-SC, the second hypothesis has already been verified for AIDS cases in adults, and was not associated with the possibility of occurrence among AIDS cases in children as well. When we consider at the survival curve (Figure 2), however, it is clear there is a large number of censored cases, because many children had a short survival time (median survival, 16 months) from diagnosis to death.
There was a reduction in child mortality worldwide between 2000 and 2010. However, 64% of the total deaths among children were related to infectious diseases and only 2% to AIDS. Despite advances in the early detection of maternal and child infection and specific drug therapy, the number of deaths in this population is still considerable (18).
Proper HIV screening during prenatal care combined with pharmacological treatment during pregnancy and seroconversion monitoring will allow the appropriate management of AIDS cases. These measures can be implemented with the aim of reducing child mortality (7, 9).
The limitations of this study include the high rate of unfilled variables in the databases reviewed, since the information ignored by the system hampers a thorough characterization of the AIDS epidemic in this age group. It was impossible to determine whether the partial completion of the notification form could be attributed to human error or if, in fact, these data were not known or not reported by the patients’ relatives.
Based on the findings from this study, it can be concluded that out of the 990 surveyed children, 51% were female, 46% were white, and 13.5% had low socioeconomic status based on the mother’s education. Perinatal infection was the main route of transmission (95.7%).
Regarding the evolution of the AIDS cases within the study group, 146 (14.7%) children died because of AIDS. Among those who died, the survival time after AIDS diagnosis ranged from 1 to 234 months, with a mean of 39.7 months and a median of 16 months. The median age of children who died of AIDS-related causes was 55 months.
The studied indicators suggest that the AIDS epidemic in children showed a decreasing tendency in the incidence and mortality rates. However, there was also an unexpected growth trend in the lethality rate in the last period.