1. Background
The definition of aging is a reduction in the body's resistance to cellular stress (1, 2). Aging and inactivity are related with an increase in inflammatory factors and the formation of reactive oxygen species (ROS), as well as the development of atherogenesis and atherosclerotic plaques (2, 3). Several studies demonstrate that an increase in ROS production is associated with an increase in the lipid peroxidation index (MDA) and a decrease in antioxidant enzymes such as superoxide dismutase (SOD) and that when the oxidative and antioxidative balance in the body is disrupted, the levels of inflammatory cytokines such as tumor necrosis factor alpha (TNF-α) and C-reactive protein (CRP) increase (4, 5). There is a high correlation between inflammatory and oxidative indices and the frequency of cardiovascular illnesses, according to studies (5, 6).
Research has shown that inflammatory and oxidative markers decrease with lifestyle changes such as reducing energy intake and increasing physical activity (7). Recently, the prescription of combined training for the elderly has attracted the attention of researchers. Ruangthai and Phoemsapthawee (8) and Shimojo et al. (9) reported an improvement in oxidative status after a period of combined training. Also, Sadjapong et al.'s results indicated a decrease in high-sensitivity CRP (hs-CRP) after 24 weeks of combined training in overweight older adults (10). However, some studies have also reported conflicting results (11-14).
Alternatively, mental and social health issues are a complication of aging that affects the elderly (15). Previous research indicates that exercise enhances mental and social health and the elderly's quality of life (15, 16).
Iran's elderly population is increasing rapidly (12), and chronic inflammation caused by old age can be the main cause of many common diseases of this age. Physical activity is an effective and non-pharmacological way to improve the physical and mental health of the elderly. However, previous studies have examined the effect of aerobic and resistance training alone. The contradictory findings of earlier studies demonstrate the need for more research to discover the best effective technique of exercise for improving the physical condition of the elderly.
2. Objectives
This paper was conducted with the purpose of surveying the impact of eight weeks of combined training on inflammatory and oxidative factors and the general social health of overweight older men.
3. Methods
3.1. Participants
The present research is a quasi-experimental study using a pre-test and post-test design. The statistical population of the current research consisted of obese males aged 60 to 75 from Birjand. First, by calling the health centers of the city, 50 people were referred, and out of this number, 40 interested older men who met the entry criteria were selected in a purposeful and available manner. The sample size of the present study was determined by using the Medcalc-18.2.1 software and based on the results of previous research, at the significance level of 5% (first type error) and 95% statistical power (second type error). Then the participants were randomly divided into two equal training and control groups. The inclusion criteria were the absence of cardiovascular diseases, kidney diseases, diabetes, and body mass index (BMI) between 25 and 30 kg/m2, not having regular exercise activities during the past six months, the ability to do exercise activities, and injection of a COVID-19 vaccine. Exclusion criteria included irregular participation in training or any therapeutic intervention.
3.2. Training Protocol
The combined protocol was based on the exercise guide for the elderly and ACSM, including aerobic, resistance, and balance exercises with a gradual increase in intensity based on the ability of the participants with moderate to high intensity for eight weeks, three days per week (Table 1) (10). For the aerobic portion of the workouts, the maximum heart rate (HRmax = 220-age) and a Polar heart rate monitor were used to assess the intensity, and for the resistance portion, one maximum repetition was employed. Additionally, the exercise's intensity was regulated in accordance with the perceived RPE pressure in the 12 - 13 (moderately difficult) range in order to ensure the safety and appropriateness of the activity (10).
| Exercise | Description | Intensity |
|---|---|---|
| Aerobic exercise | Seated marching, leg marching, arm swing, tap and clap, side bend, and arm raise | 10 - 15 min with intensity 50 - 60% of the HRmax for the first four weeks; 15 - 20 min with an intensity of 60 - 70% of the HRmax for the second four weeks |
| Resistance exercise | Arm curl, backward arm press, hip flexor, hip extensor, hip adductor, hip abductor, knee flexor, knee extensor, ankle plantar flexor, and ankle dorsiflexor | Reps: 8 - 10 × 2 set, intensity: 65 - 75% of the 1RM for the first four weeks; (Intensity was set by the color of the TheraBand.); Reps: 10 - 12 × 3 set, intensity: 85 - 90% of the 1RM for the second four weeks |
| Balance exercise | Sit to stand, knee bends, backward walking, walking and turning around, sideways walking, and heel-toe standing heel-toe walking one leg stand | Two hands support for the first four weeks; one or no hand support for the second four weeks |
3.3. Outcome Measures
The weight and body composition were also examined using a body composition analysis device (Inbody 720, Biospace, Seoul, Korea). The participants' diet was also controlled with a 24-hour food recall questionnaire. Serum levels of hs-CRP, TNF, MDA, and SOD, general-social health, and body composition were examined 48 hours before and after the training intervention. For sampling, each participant had 5 mL of fasting blood drawn from their brachial vein between 8 and 9 in the morning. The blood serum was separated after being centrifuged for 12 minutes at a speed of 3000 rpm, and it was then poured into special microtubes and kept at -80 degrees Celsius. Blood parameters were measured using the ELISA technique. The TNF-index was determined using a French-made Diaclone kit with a sensitivity of 8 pg/mL, and the hs-CRP index was determined using a Canadian-made Biochem diagnostic kit with a sensitivity of 10 ng/mL. The Human Elisa kit from ZellBio Germany, with a sensitivity of 0.1 umol, was also used to test MDA and SOD.
Keyes and Shapiro's social health scale was used to assess social health. The range of scores for 20 questions on this scale is between 20 and 100, and scoring was done using a 5-point Likert scale (very much = 5 to very little = 1). According to its designers (Keyes and Shapiro, 2004), the dependability of the scale was over 0.70 (17).
The overall health status was assessed using Goldberg's 1989 Mental Health Questionnaire (GQH-28). This self-report questionnaire has 28 items and four scores for physical health, anxiety, depressive illness, and social functioning disorder. This questionnaire's reliability has been assessed to be 0.87 (18).
3.4. Statistical Analysis
After confirming the normal distribution of the data using the Shapiro-Wilk statistical test, homogeneity of variances using the Leven test, two-way repeated measure analysis of variance, and Tukey's post hoc tests were used in SPSS statistical software version 22, and the level of significance was considered as P < 0.05.
4. Results
According to Table 2, the pre-test values of the anthropometric parameters did not significantly differ between the groups.
| Characteristics | Control Group (n = 20) | Training Group (n = 20) | P-Value (t-test) | t |
|---|---|---|---|---|
| Age (y) | 70.03 ± 2.02 | 69.73 ± 2.16 | 0.78 | 0.36 |
| Height (cm) | 156.26 ± 4.95 | 157.03 ± 4.21 | 0.51 | 0.60 |
| Weight (kg) | 62.24 ± 6.21 | 63.45 ± 5.07 | 0.58 | 0.49 |
| Body mass index (kg/m2) | 25.63 ± 1.42 | 25.79 ± 1.35 | 0.47 | 0.57 |
a Data are presented as mean ± standard deviation.
The two-way repeated measures ANOVA and Table 3 showed a significant association between the intervention time and groups in TNF-α (F = 4.44, P = 0.02), hs-CRP (F = 4.82, P = 0.03), MDA (F = 5.52, P = 0.01), SOD (F = 8.11, P = 0.001), fat mass (F = 9.39, P = 0.001) and fat percentage (F = 4.42, P = 0.02) levels.
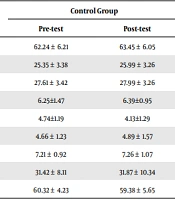
| Variables | Control Group | Training Group | Time × Group Interaction P-Value | ||
|---|---|---|---|---|---|
| Pre-test | Post-test | Pre-test | Post-test | ||
| Weight (kg) | 62.24 ± 6.21 | 63.45 ± 6.05 | 63.45 ± 5.07 | 62.27 ± 6.01 | 0.07 |
| Fat mass (kg) | 25.35 ± 3.38 | 25.99 ± 3.26 | 26.36 ± 4.21 | 25.15 ± 3.52b | 0.001 c |
| Fat percentage (%) | 27.61 ± 3.42 | 27.99 ± 3.26 | 28.42 ± 3.27 | 26.31 ± 3.38b | 0.02 c |
| TNF-α (pg/mL) | 6.25±1.47 | 6.39±0.95 | 6.32 ± 1.29 | 4.27 ± 1.27b | 0.02 c |
| hs-CRP (ng/mL) | 4.74±1.19 | 4.13±1.29 | 4.96 ± 0.99 | 3.83 ± 0.73b | 0.03 c |
| MDA (nmol/mL) | 4.66 ± 1.23 | 4.89 ± 1.57 | 5.03 ±1.01 | 3.48 ± 1.27b | 0.01 c |
| SOD (nmol/mL) | 7.21 ± 0.92 | 7.26 ± 1.07 | 6.57 ± 1.28 | 8.82 ± 1.23b | 0.001 c |
| General health | 31.42 ± 8.11 | 31.87 ± 10.34 | 34.02 ± 9.32 | 25.36 ± 9.02 | 0.001 c |
| Social health | 60.32 ± 4.23 | 59.38 ± 5.65 | 57.38 ± 7.21 | 69.87 ± 4.14 | 0.02 c |
a Values are expressed as mean ± SD.
b P ≤ 0.05 significant difference compared to pre-test; P ≤ 0.05 significant difference Time × Group Interaction with two-way repeated measurement analysis of variance.
c P ≤ 0.05 significant difference Time _ Group Interaction with two-way repeated measurement analysis of variance.
Tukey’s test showed that the training group had significantly decreased TNF-α (F = 6.05, P = 0.01), hs-CRP (F = 4.98, P = 0.03), MDA (F = 5.52, P = 0.01) and fat mass (F = 4.40, P = 0.04) after the intervention. However, the training group showed significantly increased SOD after the intervention (F = 6.05, P = 0.01).
Furthermore, there was a significant difference in the mean changes of TNF-α (F = 7.32, P = 0.01), hs-CRP (F = 4.86, P = 0.03), MDA (F = 5.03, P = 0.01), fat mass (F = 4.41, P = 0.04) and SOD (F = 4.69, P = 0.04) in the training group compared to the control group.
Also, significant associations between intervention time and groups were observed for general health (F = 11.12, P = 0.001) and social health (F = 5.11, P = 0.02) scores (Table 3). Tukey's test indicated a significant decrease in general health in the training group (F = 9.56, P = 0.001) and increased social health (F = 4.97, P = 0.01) after the intervention. After eight weeks of combined training, the mean changes in general health (F = 9.56, P = 0.001) were higher in the training group compared to the control group.
5. Discussion
The findings of this research demonstrated that eight weeks of combined training decreased MDA levels and increased SOD activity in older people which is in line with the results of Ruangthai and Phoemsapthawee (8) and Shimojo et al. (9).
In contrast to the above findings, the results of the study by Attarzadeh Hosseini et al. indicated no significant change in MDA and SOD after 12 weeks of high-intensity interval and moderate-intensity continuous training in obese older women (12). Probably the reason for the contradiction is the difference in the intensity and duration of the exercise protocol.
It appears that the oxygen species generated during exercise activate a crucial signaling pathway like mitogen-stimulating protein kinase, which causes the transcription of various factors. Additionally, the activation of cellular signaling pathways increases the expression of enzymatic antioxidants like SOD, which reduces levels of fat peroxidation and MDA (19, 20).
In this way, regular exercise can improve the oxidative stress caused by old age and being overweight.
Another finding of this research was the reduction of TNF-α and hs-CRP after eight weeks of combined training. In line with this research, El-Kader reported that after six months of aerobic and resistance training in the elderly, TNF-α and IL-6 were considerably decreased in both training groups (21). Also, the results of Sadjapong et al.'s research showed a significant reduction in hs-CRP after 24 weeks of moderate-intensity combined training in overweight older adults (10).
In contrast to the results of this research, Colato et al. reported an increase in TNF-α and hs-CRP levels after 12 weeks of concurrent training with moderate intensity (13).
Additionally, Ryrso et al. showed an increase in TNF-α and no change in CRP after eight weeks of low-intensity aerobic and resistance training in obese COPD seniors (14). These researchers stated the low intensity of exercise (30 - 40% of maximum heart rate and one maximum repetition) and no change in body composition as the reason for their results. The inconsistency between the results of the studies may be due to differences in baseline levels of inflammatory factors, sampling time, and exercise protocols. A further factor that may contribute to the discrepancy in the results of research is the variation in fat mass reduction as a consequence of training.
Previous research has reported that the concentration of TNF-α increases with more abdominal fat or with increasing age (22), and the decrease of fat mass is the most significant factor in enhancing the inflammatory markers. Since adipose tissue is one of the main sources of IL-6 and TNFα production, with the decrease of adipose tissue caused by regular exercise, especially aerobic exercise, the serum level of these cytokines also reduces (13, 14). Also, resistance training, by increasing muscle mass, has anti-inflammatory benefits. In the present study, in the training group, fat mass and fat percentage decreased after eight weeks of training, and probably this improvement in body composition was effective in reducing inflammatory cytokines. In general, combined training seems to be more beneficial than resistance and aerobic training alone in reducing fat mass and inflammatory markers.
Besides, one of the possible mechanisms of the decrease of inflammatory cytokines is probably due to the decrease in ROS production. Regarding the relationship between ROS and TNF-α, it can be concluded that exercise could moderate the process of TNF-α production by reducing the production of ROS (14). During this process, low-density lipoprotein (LDL) is altered to its oxidized form (oxLDL). Moreover, the nuclear factor NF-κB is activated, and at last, this transcription factor could activate proinflammatory genes such as TNF- α (10, 14).
Additionally, a significant association between circulating levels of TNF- α, and MDA was also noted in the research by Soundravally et al. (23). Probably one of the reasons for the decrease in TNF-α and hs-CRP in the present study is the decrease in MDA and increase in SOD.
Another finding of the current research was the improvement in the general social health of the elderly after eight weeks of training. Studies have shown that engaging in physical activity can have beneficial effects on other aspects of the elderly's life, especially their spiritual and psychological aspects, and lead to in life satisfaction (16, 24, 25).
One of the theoretical models about the psychosocial changes related to exercise (sedation or relaxation) is probably the activation of the central nervous system and the release of endorphins. Exercise increases self-confidence and self-sufficiency by reducing anxiety. According to some reports, the increase in self-confidence may be related to the regulation of endocrine, catecholamine, and endogenous opioid peptides (including endorphins) that occur in the body after exercise (24, 26).
Lack of control over psychological conditions and individual differences of the subjects was one of the limitations of the present research. However, the appropriate and applicable exercise protocol for the elderly and high precision in the implementation of different stages of the research are the strengths of the research. Therefore, according to the results of the present study, this exercise protocol can be used as a preventive method to improve the inflammatory, oxidative, and psychosocial health of the elderly.
5.1. Conclusions
Based on the results of this study, eight weeks of combined training significantly decreases MDA, TNF-α, and hs-CRP and increases SOD, and enhances general and social health in overweight elderly. In this regard, it can be stated that regular combined training has a significant effect in preventing the effects of oxidative stress and inflammation in the elderly.