1. Introduction
Rugby players are at high risk of sustaining shoulder injuries including instability and rotator cuff tears (1, 2), both isolated and combined (3). A mean of 241 player-days per club per season are lost in rugby union to shoulder injuries leading to an average of 81 days of absence with a high rate of recurrence (62%) (3). In Australian professional rugby league there were 252 games lost per club in the 2010 season due to 85 injuries of shoulder and arm, at 2.96 games per injury (or 20 player days), although differing definitions for injury apply (4).
Combined lesions of instability and rotator cuff failure are recognized in the community and in contact sports more commonly since the advent of MRI and arthroscopic assessment (5). However, published results of open instability repairs and reconstructions in younger patients have been good in previous years without MRI scans despite the lack of recognition or treatment of rotator cuff deficiency and open surgery that may have missed combined pathology.
If combined lesions are diagnosed in non-athletes, there can be seen good clinical and subjective outcomes in treating both arthroscopically in one surgery (6) or even only repairing the rotator cuff and treat the labral tear conservatively, as aging soft tissue favors stability (7).
Managing a combined rotator cuff tear and instability injury in professional contact athletes has been reported as requiring either sequential staged reconstruction and cuff repair (5) or combined open and arthroscopic surgery, but without consideration of career goals in management.
The ability of a player to compete at the elite level in contact sport depends on many factors surgery, but the finding of significant cuff pathology at retirement has prompted us to consider whether it is possible to manage emergency pathology with in season instability surgery whilst leaving significant rotator cuff deficiency present until career goals (such as participation in finals) are achieved, an issue largely ignored in scientific literature (8).
We consider it important to present an appropriate management program of treating in-season concurrent rotator cuff tear and instability injuries, as opposed to isolated instability (9) in an elite rugby player to fit in with his career goals (10), in this case consisting of immediate labral repair to allow return during the current season and delayed, off season rotator cuff repair after competing in a successful premiership campaign.
2. Case Presentation
A 27-year-old, elite professional National Rugby League (NRL) footballer (second rower) presented with a history of chronic full thickness rotator cuff tear over the past year, combined with acute on chronic anterior instability associated with a large Bankart lesion of his right shoulder. His first visit was after round 4 of a 29 week season following a severe subluxation. Suffering multiple minor subluxations within the last 2 seasons, the instability and soreness of his right shoulder was worsening, and he attempted to play on with conservative treatment through the season. He reported multiple falls on his shoulder with subluxation but no full dislocation of the shoulder. He represented after round 10 being unable to play on, and discussed mid-season surgery.
His clinical findings showed a near full ROM with positive anterior stress apprehension, positive load and shift and mildly positive O’Briens' sign, with no posterior instability and negative jerk test. Additionally the player presented with partial weakness in the rotator cuff, (mainly supraspinatus and subscapularis), with a positive Jobe test and a mildly positive lift off test.
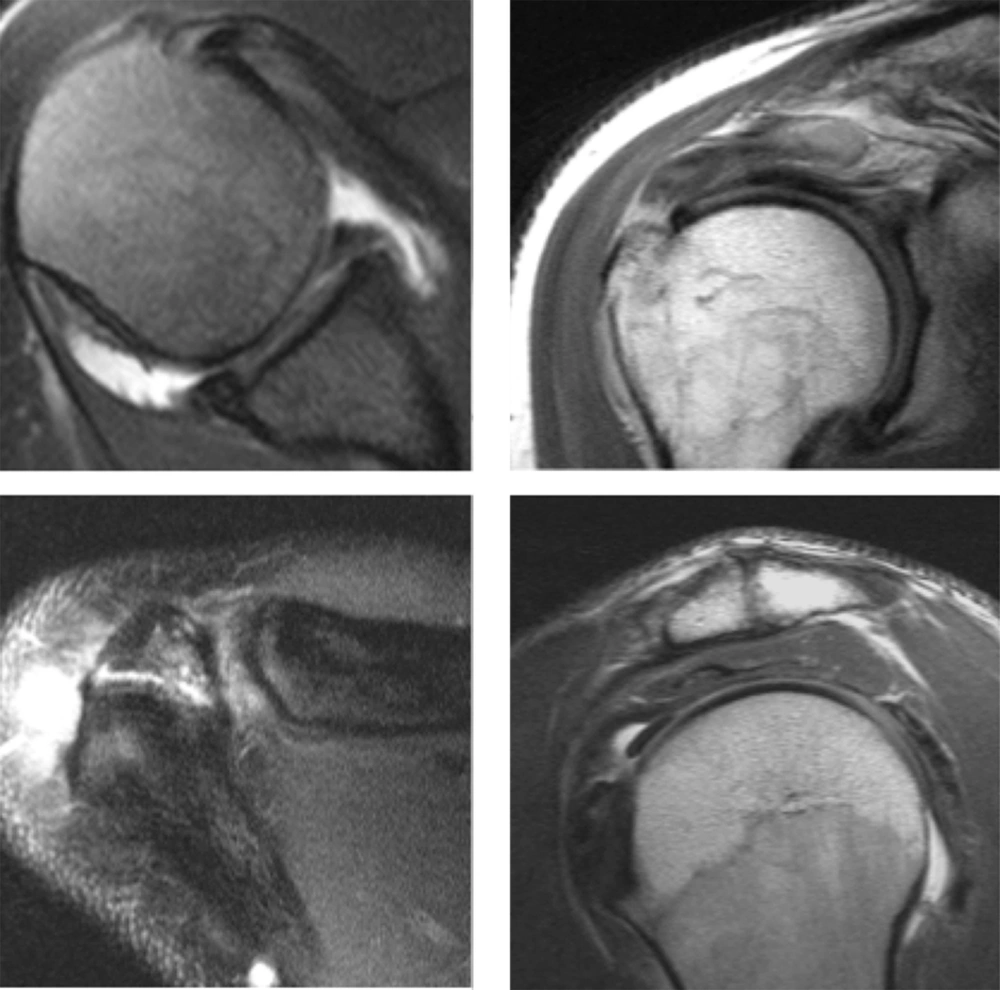
His MRI demonstrated a full thickness insertional tear 10 mm by 5 mm in the anterior supraspinatus tendon (Figure 1). The subscapularis tendon had a partial tear in the inferior third. The anterior inferior labrum showed a detached tear without bony involvement. A corresponding small Hill Sachs lesion was seen. There was moderate subacromial and subdeltoidal bursitis and hypertrophic ac-joint changes with inferior capsule thickening, and a pre-acromion type of Os acromiale.
After discussing treatment options in general and specific treatment options in his situation, the patient favored a procedure that gave him some chance of returning before the end of the season to play finals football. The chances of same season return after repair of a significant full thickness rotator cuff tear was considered remote, so after discussion with the player and the team physician, the player was offered an arthroscopic stabilization procedure without cuff repair. This was performed during the same week.
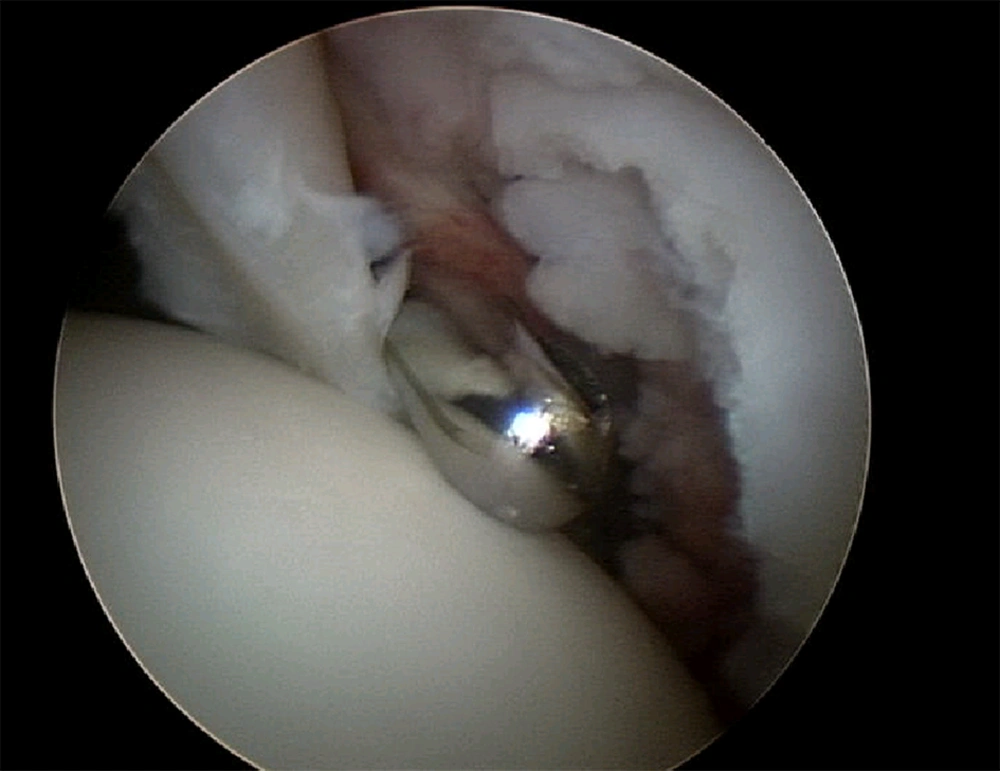
At surgery a locked buckle handle SLAP tear extending from 11 O’clock to 8 O’clock was recognized and the bucket handle excised. The large anterior Bankart lesion (2 O’clock to 6 O’clock) was repaired with Bioknotless anchors (Mitek) A 2.5 cm insertional tear in the supraspinatus was debrided but no repair performed (Figure 2). A bony decompression or resection of Os acromiale was not performed, but bursectomy and coraco-acromial ligament released. The player was immobilized in a sling for four weeks, followed by an aggressive rehabilitation program. He achieved full strength and range of motion.
The player returned in round 23/26 to elite level rugby league (12 weeks after reconstruction surgery), and played out the season, being involved in the grand final winning side. In the grand final, he was able to compete at intense level, being involved in heavy direct contact collisions to the affected shoulder.
The patient then underwent routine rotator cuff repair and arthroscopic resection of an Os acromiale two weeks after grand final festivities. At surgery the rotator cuff tear did not appear to have enlarged from the time of arthroscopic reconstruction. The anterior labrum was solidly repaired and required no extra procedure. The Player returned to play at 5 months (after summer break) at elite level once again, again recovering full range of motion. The player has continued at elite level for seven years since then, including a change of clubs, and has returned for stabilization surgery of the contralateral side some 3 years later, with good results and return to ongoing elite level, high demand contact sport.
3. Discussion
Rugby union and rugby league players are exposed to a high risk of sustaining anterior instability and rotator cuff injuries, but the presentation of full thickness rotator cuff tears concurrent with instability are unusual.
The current literature available suggests either concurrent repair with an extended time out of sport, or staged repairs with even longer rehabilitation. The possibility of surgically repairing one of the pathologies present and returning to sport before treating the other has not been considered in published studies.
Rotator cuff tears are often diagnosed as concommitant injuries with SLAP and/or Bankart Lesions (11). The history then often consists of a long period of subjective subluxation and soreness, as described in our patient, followed by an acute trauma which leads to medical assessment.
Goldberg et al. (5) report on a series of six elite rugby union players, who were treated with a two stage procedure: open rotator cuff repair followed by an open shoulder stabilisation some 10 weeks later. They justify the decision for a 2-stage procedure on the different rehabilitation programs following rotator cuff repair and instability repair. They chose open procedures, considering those to be more reliable for elite athletes.
Goldberg et al. (5) was able to present successful outcomes quoting “rapidly returning the patients to their professional highly demanding sports” but requiring 9 months after the first surgery, which means missing most if not all of one season. Considering the average career of a rugby league player, which is on average 6 years according to NRL statistics, and dropping to 4 years in athletes with a shoulder stabilization (12), this is a loss of almost 20% of his professional career.
Recently a case report was published by Wilk et al. (13) presenting a Surgical Repair of a combined 330° capsulolabral lesion and partial-thickness rotator cuff tear in a professional American Football quaterback. The Patient underwent an arthroscopic 330° capsulolabral repair; with concomitant rotator cuff repair and subacromial decompression five days post injury. After completing 28 weeks of a multiphased rehabilitation program he was able to return to play 8 months later, for the start of the next season. Although the repair was successful and the player continued playing NFL football at high level he lost one year of season, which for NFL Players this would be 15% of his total career (NFL Management Council stats 2002).
According to Voos et al. (6), who presented 29 patients with concomitantly repaired rotator cuff and labral lesions, report satisfactory clinical outcome as well as full ROM at an average follow-up of 2.7 years. However, the results of this cohort study do not include any elite-level athletes, with average age 47 years old (and therefore more representative of the general population).
Open shoulder stabilizations such as the Latarjet procedure are also widely reported for rugby players with instability. Concerns about length of rehabilitation and invasiveness in this specific group are unnecessary, according to Neyton et al. (14). They retrospectively assessed 34 rugby players with a mean follow-up of 12 years. No recurrence of either dislocation or subluxation occurred. However, only sixty-five percent of this group returned to playing rugby.
Our patient achieved life long career goals by staging the surgical treatment of his shoulder pathology, in a manner not considered typical for patient care in undertaking repair of all damaged tissues on presentation. Our patient considers the decision making as shared with the clinician, and was delighted with the outcome long term.
As seen in the literature, patients who have undergone an acute, soon-after-injury capsulo-labral repair, especially with concomitant rotator cuff repair, require intensive and protracted post-operative rehabilitation with a balance of protective healing in conjunction with a more rapid progression of ROM for an elite athlete.
We believe that a 2-stage procedure with urgent “in-season” labral reconstruction and delayed rotator cuff repair is a reliable method to get the athlete back to sport as soon as possible with confident and reliable shoulder function in the short term but undergoing definitive cuff repair later (after achieving career goals) without significant risk of additional damage or early onset arthrosis.