1. Background
Owing to the importance of natural childbirth and lowering the risk of cesarean section, one of the midwifery priorities is the preparation of a pregnant woman’s cervix. In circumstances where the cervix is closed, and there is no effacement, preparation of the cervix is typically the first step in inducing labor (1). Inducing labor is the right thing to do if the benefits of inducing labor are greater than the benefits of staying pregnant for both the mother and the baby (2). It is crucial to discover a low-cost, and safe method for inducing labor before spontaneous labor begins, in late pregnancies, and in cases when underlying pregnancy concerns exist (3).
The score described by Bishop in 1964 is one quantitative measure used to predict the result of labor induction. A bishop score of four or less is regarded as an unfavorable indicator of the cervix and suggests the need for cervical preparation (4). Induction of labor using safer techniques can reduce economic expenditures and prevent complications from cesarean section (5, 6). Hydroscopic dilation, intra-cervical Foley catheter, artificial membrane rupture, and infusion of extra-amniotic saline are examples of non-pharmacological (mechanical) approaches (7). In the past, labor induction has been aided by the use of drugs, including prostaglandin E2, prostaglandin E1, oxytocin, nitric oxide donors, and dexamethasone (8). Oxytocin may cause uterine hyperstimulation, amniotic fluid embolism, fetal heart rate reduction, and neonatal hyperbilirubinemia as well as misoprostol increases the risk of fetal meconium, diarrhea, headache, and gastrointestinal bleeding (9).
Inducing labor pains can be aided by using evening promise oil (Oenothera) (10, 11). Because evening primrose composition is a prostaglandin precursor, it may induce labor alone and, in combination with misoprostol, may lessen the need to re-dose. Due to fewer side effects compared with other labor-inducing medicines, patients may be more favorable to its use, leading to more vaginal deliveries and fewer cesarean sections and problems. Information and clinical data on the use of evening primrose oil for cervix preparation and labor induction are lacking. There are a variety of procedures and amounts of drugs employed in the studies that are now accessible, and the findings are biased, of poor quality, and often conflicting (12, 13).
2. Objectives
In this study, we aimed to demonstrate the impact of the evening primrose capsule on inducing labor, as well as to compare its effect to that of misoprostol.
3. Methods
This study is a prospective clinical trial that was performed on 200 low-risk pregnant women with obstetric indications in the delivery unit of Yas Hospital in Tehran from 2018 to 2020 (24 months) after obtaining an ethics license from the ethics committee of Tehran University of Medical Sciences. One hundred patients were randomly assigned to received primrose or placebo in a 1:1 allocation by a computer-generated simple randomization list. The allocation sequence was kept blinded to the recruiters and local staff. The stratification factors to be balanced across treatment groups were age and BMI. The patient, the prescribing nurse, the data collector, and the statistical analyst were unaware of the intervention. Before starting the trial, all participants were explained the purpose of the study and obtained informed consent, as well as received a vaginal examination (done by a resident in gynecological surgery), calculation of the bishop score, and NST for 30 minutes. The fetal heart rate (FHR) and lack of uterine contractions were verified.
Term or post-term pregnancy, live fetus, single fetus with cephalic presentation, intact embryonic membranes, amniotic fluid index greater than five, normal NST, cervical Bishop score of two or less, absence of uterine contractions and labor pains, and first or second pregnancy were the inclusion criteria. Exclusion criteria included a history of prostaglandin allergy, previous cesarean section or hysterectomy, third trimester bleeding, placenta Previa and need for preterm labor induction, PROM, non-cephalic fetal presentation, multiple pregnancies, suspected fetal malformation, Bishop score above three, presence of uterine contractions, uncertain NST, suspected chorioamnionitis, and high-risk pregnancies, including preeclampsia, intrauterine growth restriction, oligohydramnios, and polyhydramnios.
Misoprostol 25 micrograms (a quarter of a 100-microgram tablet) manufactured by Searl (Cytotec) and 500 mg evening primrose capsules manufactured by Webber naturals (the second group) were inserted in the posterior fornix, and up to 60 minutes after insertion, the groups were compared. The patient was positioned in the left lateral position. Patients were constantly watched for FHR and uterine contractions, and the mother’s vital signs were checked every hour. In the case of ineffective contractions, the next dose of the medicine was administered every three hours until the bishop score reached > 4, up to a maximum of three doses, with a vaginal examination conducted before each dose to ascertain the bishop score. In the latent period of labor, examinations were conducted every three to four hours and every 1 - 2 hours in the active phase.
Cesarean section was performed in patients with obstetric indications, including concentrated meconium, long distance from labor and no effective uterine contractions, fetal distress (lack of fetal heart rate variability with recurrent late or variable deceleration, prolonged deceleration, or fetal bradycardia that did not respond to initial treatments), cord presentation, placental abruption, and no change in dilatation progression with a dilatation rate of six cm or higher and ruptured membranes despite four hours of appropriate uterine activity (uterine contraction pattern of 200 units or more per 10 minutes).
Successful induction of labor is characterized by three contractions every 10 minutes and a dilated cervix of at least four centimeters. All observations in both groups were recorded on the observation sheet, including the interval between vaginal administration of misoprostol and evening primrose capsules and the onset of defined uterine contractions, the mean change in Bishop cervical score, the length of the active phase of labor, time elapsed to dilatation of six cm (active phase of labor delivery), from six cm dilatation to full dilatation and from full dilatation to labor, number of repeated doses of misoprostol and evening primrose in each group, total dose used, need for induction of labor with oxytocin, prevalence of tachysystole uterus (Five or more contractions in 10 minutes), type of delivery (normal vaginal delivery, cesarean section), fifth minute Apgar score of the baby, meconium excretion, umbilical cord pH, NICU hospitalization rate, and maternal complications, including headache and gastrointestinal problems, including nausea, vomiting, and diarrhea). The information entered was statistically evaluated.
3.1. Ethical Consideration
The study was approved by the Tehran University of Medical Sciences and the Medical Ethics Committee with reference number IR.TUMS.MEDICINE.REC.1398.763.
3.2. Statistical Analysis
Data were reported as mean ± standard deviation (SD). Pearson correlation analysis was used to test for univariate linear relationships between the variables. A P-value less than 0.05 was statistically significant. The information was analyzed using SPSS version 25.
4. Results
A non-probability random selection approach was used to select 200 patients, a method chosen based on the sample size of people with comparable conditions in the research population. Statistical calculations with a confidence level of 95% were used to figure out how many samples to take. The experimental group consisted of two distinct groups of 99 and 101 participants. In the first test group, misoprostol 25 micrograms were given vaginally to start labor. In the second test group, 500 mg of vaginal evening primrose capsules were used to start labor. In terms of mother age, BMI, gravidity, history of abortion, the bishop score, and gestational age, there was no statistically significant difference between the two groups.
Eleven and seventeen hours passed between the administration of the first dose of misoprostol and evening primrose and the dilatation of six cm, respectively. The independent t-test revealed that this difference was statistically significant with a P-value of 0.001. With misoprostol and evening primrose, the average time between a six-cm dilation and full dilation was three hours, which was not statistically significant (P = 0.061), according to an independent t-test. In the misoprostol and evening primrose groups, the average time between full dilation and birth was 45 minutes and 35 minutes, respectively. This difference was not statistically significant (P = 0.108, independent t-test) (Table 1).
| Name of Group | Mean ± SD | P-Value |
|---|---|---|
| Inactive phase (h) | < 0.001 | |
| Misoprostol (n = 99) | 10.75 ± 3.15 | |
| Evening primrose oil (n = 101) | 14.38 ± 5.83 | |
| Time elapsed from dilatation of 6 cm to full dilatation (h) | 0.061 | |
| Misoprostol (n = 99) | 2.88 ± 1.09 | |
| Evening primrose oil (n = 101) | 2.6 ± 0.97 | |
| Time elapsed between full dilatation and delivery (h) | 0.108 | |
| Misoprostol (n = 99) | 43.84 ± 27.92 | |
| Evening primrose oil (n = 101) | 37.57 ± 27.02 |
In this study, 141 individuals experienced NVD, with 67 in the first group and 74 in the second group; 59 individuals had cesarean birth, with 32 in the first group and 27 in the second. In this aspect, the difference between the two groups was not statistically significant (P = 0.386). Moreover, 155 cases required augmentation with oxytocin; 60 cases in the first group (misoprostol) and 95 cases in the second group (evening primrose). Compared to the two groups, 31 cases got a dose and did not require a repeat dose; 23 cases were in the first group (misoprostol), and 8 cases were in the second group (evening primrose). Furthermore, 68 women required two doses, with 59 in the first group (misoprostol) and 9 in the second group (evening primrose). Seventeen and 84 patients in the first and second groups required the third dose of the treatment, respectively. In the two characteristics listed above, the difference between the two groups was statistically significant (P < 0.001) (Table 2).
| Misoprostol (n = 99) | Evening Primrose Oil (n = 101) | P-Value | |
|---|---|---|---|
| Total received dose | < 0.001 | ||
| 1 | 23 | 8 | |
| 2 | 59 | 9 | |
| 3 | 17 | 84 | |
| Need for oxytocin augmentation | < 0.001 | ||
| No | 39 | 6 | |
| Yes | 60 | 95 | |
| Delivery type | 0.386 | ||
| Vaginal | 67 | 74 | |
| Cesarean section | 32 | 27 |
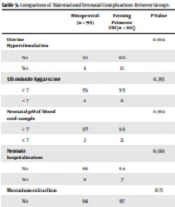
Compared to the two groups, there were a total of eight hyperstimulated cases in the first group only (misoprostol). In this regard, there was a considerable difference between the two groups. Four out of the six patients in the first group and two in the second group had an Apgar score of less than seven. In comparison, four cases had a pH of less than seven, two in the first group and two in the second. Also, 18 patients were admitted to the NICU, including 11 infants in the first group and seven infants in the second. There were nine incidences of disposal of meconium, five in the first group and four in the second. Using an independent t-test, the above items did not differ substantially (P > 0.05). Compared to the other two groups, a total number of maternal problems, such as headaches or gastrointestinal disturbances, were observed. All 15 patients in the first group experienced headaches after taking medicine, while only three patients in the second group experienced headaches. There were also five incidences of gastrointestinal problems, including diarrhea and nausea, all of which occurred only in the first group. In terms of maternal complications, the difference between the two groups was statistically significant (Table 3).
| Misoprostol (n = 99) | Evening Primrose Oil (n = 101) | P-Value | |
|---|---|---|---|
| Uterine hyperstimulation | 0.004 | ||
| No | 91 | 101 | |
| Yes | 8 | 0 | |
| 5th minute Apgar score | 0.393 | ||
| > 7 | 95 | 99 | |
| < 7 | 4 | 2 | |
| Neonatal pH of blood cord sample | 0.992 | ||
| > 7 | 97 | 99 | |
| < 7 | 2 | 2 | |
| Neonate hospitalization | 0.302 | ||
| No | 88 | 94 | |
| Yes | 11 | 7 | |
| Meconium extraction | 0.71 | ||
| No | 94 | 97 | |
| Yes | 5 | 4 | |
| Maternal headache | 0.003 | ||
| No | 84 | 98 | |
| Yes | 15 | 3 | |
| Maternal gastrointestinal complication | 0.022 | ||
| No | 94 | 101 | |
| Yes | 5 | 0 |
5. Discussion
This study examined the effects of 25 micrograms of vaginal misoprostol and 500 milligrams of vaginal evening primrose capsules for cervical preparation and labor induction. The number of prior pregnancies, abortions, gestational age, and Bishop score were identical, and there was no statistically significant difference between the groups. The average age of the mothers in our investigation was 30 years old, and their average BMI was 31. Considering that the purpose of this study was to analyze Bishop scores ≤ 2, there was no significant difference between the two groups in this respect.
Evening primrose extract contains linoleic (70 - 74%), γ-linolenic (8 - 10%) acids, Omega-6 essential fatty acid with anti-inflammatory properties, palmitic acid, oleic acid, and stearic acid as well as small quantities of Myristic, Oleopalmitic, Vaccenic, Eicosanoic, and Eicosenoic acid (14). Essential fatty acids (EFAS) are precursors of prostaglandin synthesis and have a pivotal role in regulating the metabolism of the body (15). In the human diet, linoleic acid is the most common n-6 PUFA. The longer chain PUFAs such as GLA, DGLA, and AA are formed in the body as a result of the metabolism of linoleic acid (16). PGE2 and PGF2 production in vitro by explants from the mother’s endometrium was dramatically elevated in the presence of a high LA diet. Women’s COX-2 expression level and activity are both increased in the last stages of pregnancy, which leads to increased production of the prostaglandin PGF2. Increasing PGF2 is usually regarded as an important phase in the labor procedure (17). Previous research has revealed that dietary polyunsaturated fatty acids (PUFAs) may also affect steroid hormone levels (18, 19).
In our research, we also focused on maternal problems, including gastrointestinal issues and headaches, which were more prevalent in the first group (misoprostol). It is in line with what the FDA has indicated (20).
One dosage of 1,000 mg of EPO, administered vaginally at 41 weeks of pregnancy, increased the Bishop score and decreased the amount of time needed to deliver a baby in post-term pregnancies in Azad et al.’s randomized controlled study (21). It is consistent with our findings, which showed that the average time between dilation to six cm and full dilatation and the time between full dilatation and delivery was not significantly different in the misoprostol and evening primrose groups, despite the significant difference in duration between the first dose of misoprostol and the beginning of active labor. Some investigations have come to the same conclusion. In 2006, Ty-Torredes Clinical Trial, which included 71 participants, there was no difference between evening primrose oil (EPO) and the placebo in terms of Bishop score or cervical length with TVS. There was also no difference between evening primrose oil and the modified BPP or NST fetal profile (13). Also, EPO injection before hysteroscopy improved the cervix of 36 non-menopausal women studied by Vahdat et al. It is easy to use, readily available, reasonably priced, and does not have any significant side effects (22). Nouri et al.’s Clinical Trial showed that women in their fertile years who did not have a history of normal NVD and women who had already gone through menopause preferred EPO capsules to misoprostol before gynecological surgeries (23).
Controversial outcomes have also been found in another research. Evening primrose oil was administered orally to 54 first-time mothers from 37 weeks of gestation in research by Dove and colleagues. When it came to lowering labor time, evening primrose oil had no impact, but it did increase oxytocin use for augmentation; it also increased cessation of descent and the requirement for a vacuum; and it raised risk for rupture of fetal membranes (10). Hashemnejad et al.’s study, which was a triple-blind case-evidence clinical investigation, found that vaginal primrose capsules did not help prepare the cervix (24). Moradi et al.’s meta-analysis showed the same thing (25): Oral ingestion of evening primrose oil did not seem to be beneficial for cervical ripening. Although in our study, the second group (evening primrose) significantly showed some weakness in line with these investigations. Possibly, the contradictory findings in numerous studies are due to the fact that different interventions, research methods, and sample strategies were used in each study. When compared to misoprostol, we discovered that evening primrose use had no effect on uterine tachysystole. Meconium excretion did not differ significantly between the two groups. According to the authors, these findings are analogous to those of Mitri et al.’s study (26). Meconium in the amniotic fluid increased in the subject receiving misoprostol, and the higher doses of misoprostol required less oxytocin, but they also raised the chance of uterine tachysystole and/or fetal heart rate alterations in this study. There were no significant differences between the two groups in terms of the overall number of cesarean sections, Apgar score, pH, hospitalization in the NICU, or meconium excretion in our research. Lack of dilatation during active labor was the most prevalent reason for cesarean section in both groups. The above findings are comparable to a 2014 study by Ayati et al. on 140 women who had a medical or midwifery indication for induction of labor. Every six hours for a period of 24 hours, women in the first group received 25 g of intravaginal misoprostol, whereas women in the second received 25 g of sublingual misoprostol. Between the two groups, there was no significant difference in maternal and neonatal outcomes. Fetal discomfort and inability to progress in the active delivery process were the most common reasons for cesarean sections in both groups (27).
5.1. Conclusions
Evening primrose capsules can be used to induce labor because of the lower risk of hyperstimulation of the uterus and the higher tolerance. There should be more research done to see if this medicine can be used alone or in conjunction with misoprostol or mechanical dilators or if it can be administered at home rather than in the hospital.