1. Background
Systemic lupus erythematosus (SLE) is a systemic autoimmune disease with clinical involvement that can affect human body organs or systems, especially skeletal muscles, kidney, heart, skin, and central nervous system (CNS) (1, 2). The prevalence of SLE in human population was reported about 20 to 150 cases per 100,000 people. Females affect10 times more than males by the SLE disease (3). SLE has a complex and strong genetic basis. Molecular genetic studies in humans and animals identified the important genes that contribute the pathogenesis of SLE. The most important genes predispose to disease are human leukocyte antigens (HLA) such as DR3, DR4, followed by non-HLA like protein tyrosine phosphatase non-receptor type 22 (PTPN22), signal transducer, activator of transcription 4 (STAT4), and interferon regulatory factor 5. Among non-HLA genes, PTPN22 is considered as the most effective gene in autoimmune diseases (4, 5).
SLE has various clinical appearances with a large number of autoantibodies. So far, more than 180 autoantibodies were identified in the blood of patients with SLE, although different people may show different antibody profiles (6). Currently, the clinical diagnosis of lupus relied on the presence of at least 4 out of 11 diagnostic criteria proposed by the American College of Rheumatology (ACR) for SLE (7). The presence of anti-nuclear antibodies (ANA) in patient’s serum is the most important laboratory criterion for the diagnosis of SLE. The most important characteristic of autoantibodies in SLE is targeting nuclear fusion, anti-nuclear antibodies (ANA), and antibodies against double-stranded DNA (ds-DNA), which is positive in more than 90% of the patients with SLE (2).
Various studies showed that PTPN22 gene contributes in predispose to autoimmune diseases (8, 9). The PTPN22 gene is located on chromosome 1p13 and encodes the lymph protein tyrosine phosphatase (LYP), which plays an important role in controlling signaling through T-cell receptor and negative control of T-cell activating in the later stages (8). B- and T-lymphocytes dysfunction is usually observed in patients with SLE and many studies recorded defects in B- and T-cell receptors signal transduction (10). The most common single-nucleotide polymorphism (SNP) in PTPN22 is (1858C > T) rs2476601. In this SNP, a missense mutation in nucleotide position 1858 in the coding area of gene converts cytosine into thymine, causing the single amino acid arginine to be converts into tryptophan in position 620 in exon 14 (11, 12). Another SNP in gene PTPN22 is rs2488457 (-1123G > C) in which a missense mutation in nucleotide position 1123 in promoter area converts guanine to cytosine (13). The PTPN22 mutations may cause T-cell activation and the induction of autoimmune diseases such as SLE, rheumatoid arthritis, autoimmune thyroid, and type 1 diabetes mellitus (T1DM) (14). Therefore, the probable association between +1858C > T and -1123G > C polymorphisms in PTPN22 promoter was studied in the current study among patients with SLE living the Southwest of Iran.
2. Methods
2.1. Study Population
The study was conducted on 120 patients with SLE confirmed by a rheumatologist and the positive profile of ANA and anti-dsDNA. Also, 120 healthy persons without a family history of autoimmune diseases, matched for age and gender, were selected as controls. In the study, all patients and controls were selected from Lorestan province in Southwest of Iran. The study was approved by the ethics committee of Khoramabad University of Medical Sciences, Khorramabad, Iran, and was conducted after obtaining the written informed consent from all participants.
2.2. Genotyping
Genomic DNA was extracted out of the subjects’ blood samples using the salting-out method and genotype was assessed using the PCR-restriction fragment length polymorphism (PCR-RFLP) method (15). Primers used to identify mutations of +1858C > T and -1123 G > C are given in Table 1. PCR was performed using 1 μL of template DNA (~ 100 ng μL-1), 1 μL of each primer (10 μL), 12.5 μL of master mix, and 7.5 μL of sterile distilled water in a total volume of 25 µL. To amplify the fragment containing +1858C > T mutation, the following procedure was conducted: the initial denaturation at 94°C for 4 minutes, 35 cycles including denaturation at 94°C for 30 seconds, the annealing at 60°C for 30 seconds, the extension at 72°C for 30 seconds, and the final extension at 72°C for 5 minutes. To amplify the fragment containing -1123G > C mutation, the following procedure was conducted: the initial denaturation at 94°C for 4 minutes, 35 cycles including denaturation at 94°C for 30 seconds, the annealing at 58°C for 30 seconds, the extension at 72°C for 30 seconds, and the final extension at 72°C for 5 minutes. Then, the PCR products were electrophoresed on 1.5% agarose gel; the fragment lengths for +1858C > T and -1123G > C were 392 and 171 bp, respectively.
| Name | Primer Sequence | Tm |
|---|---|---|
| rs2476601-F | 5′-TTAGCGCTAGCCTCAATGACGACC-3′ | 67.9 |
| rs2476601-R | 5′-TGAGCCTCAGACATCTCCAGTCC-3′ | 68.3 |
| rs2488457-F | 5′-AGCCAACSTCCWCTAAGTGGGCTG-3′ | 51.4 |
| rs2488457-R | 5′-GAGTTTCCTCTGACTCCATCGCAG-3′ | 59.21 |
2.3. Digestion
Genotyping PCR products for PTPN22 mutation was performed using the RFLP method. PCR products containing +1858C > T mutation were digested with the restriction enzyme Rsa1 (Promega GmbH, Germany) in an overnight incubation at 37°C. The reaction included 10 μL of PCR products, 0.5 μL (20,000 IU/µL) of Rsa1, and 2 μL of buffer in 7.5 μL of sterile distilled water. PCR products with -1123G > C mutation were digested with the restriction enzyme Sac1 (Promega GmbH, Germany). Especially, the reaction included 10 μL of PCR products, 0.5 μL (20,000 IU/µL) of enzyme Sac1, and 2 μL of buffer in 7.5 μL of sterile distilled water. PCR products containing -1123G > C mutation were also digested in an overnight incubation at 37°C. Then, the digested products were electrophoresed on 2.5% agarose gel.
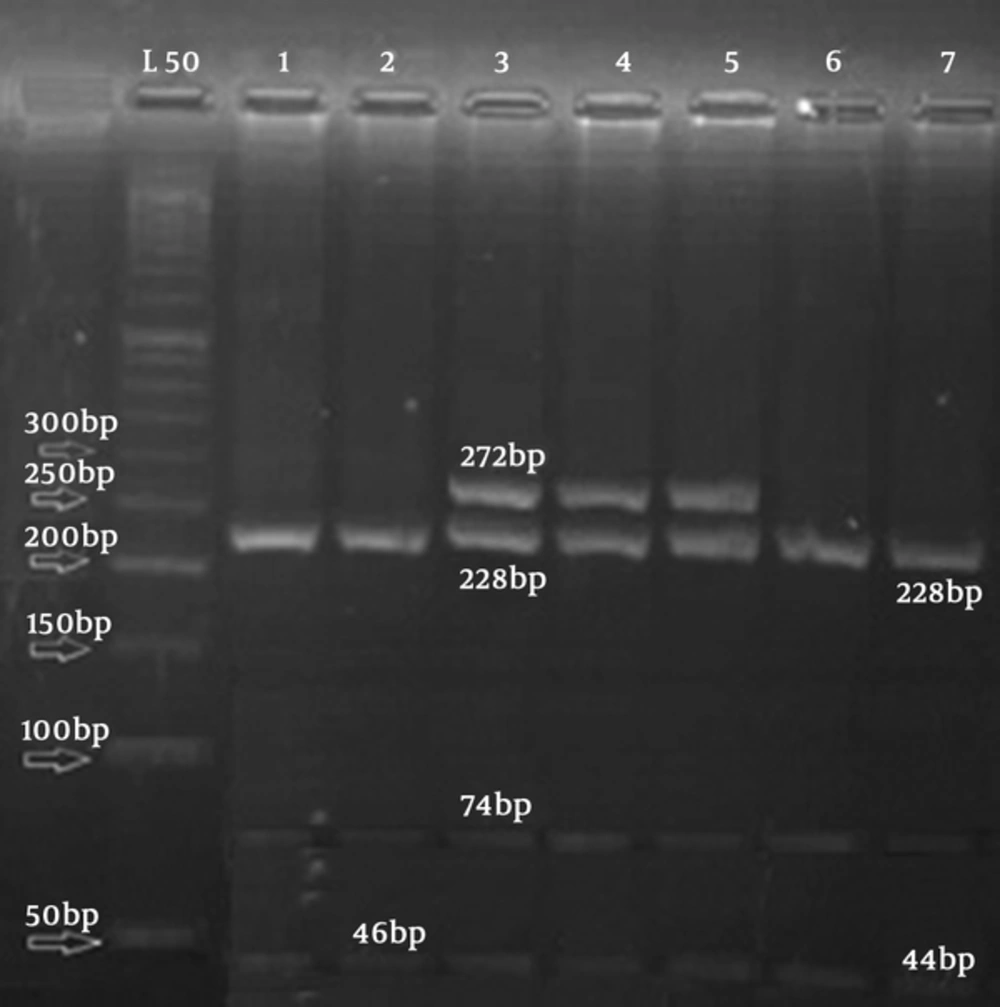
In relation to rs2476601 polymorphism, as shown in Figure 1, the 392-bp PCR products were digested with Rsa1 for each genotype as follows: the homozygous wildtype allele CC had 4 bands of 228, 74, 46, and 44 bp, and heterozygote CT had 5 bands of 272, 228, 74, 46, and 44 bp.
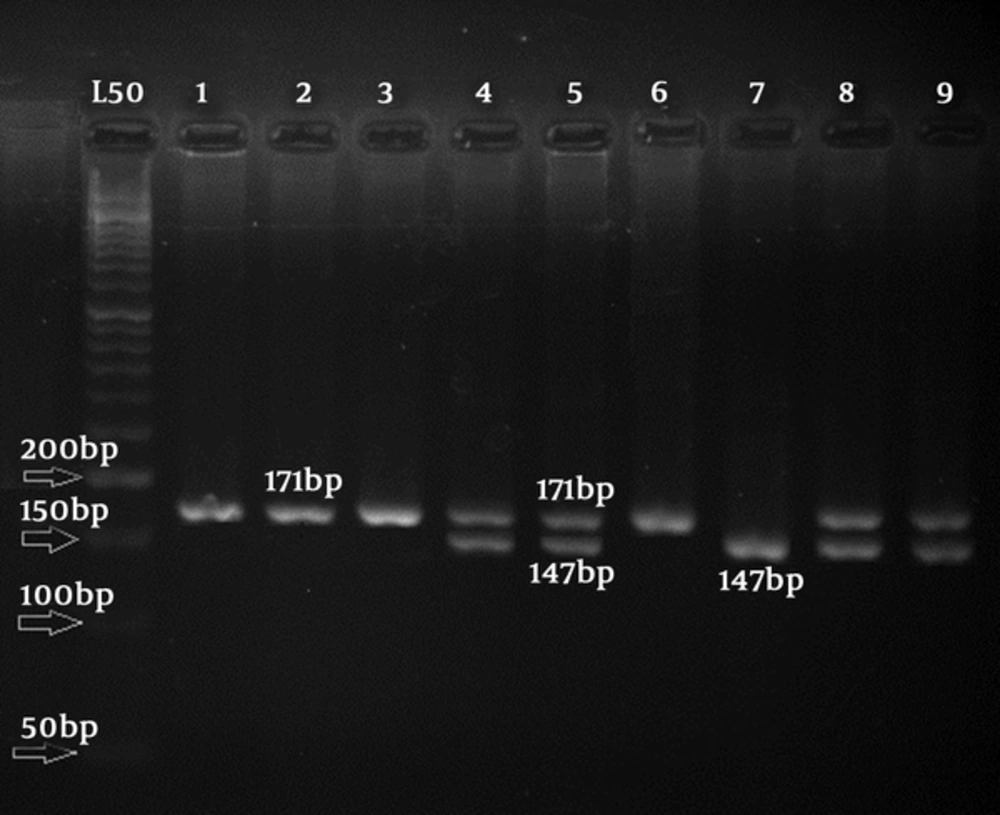
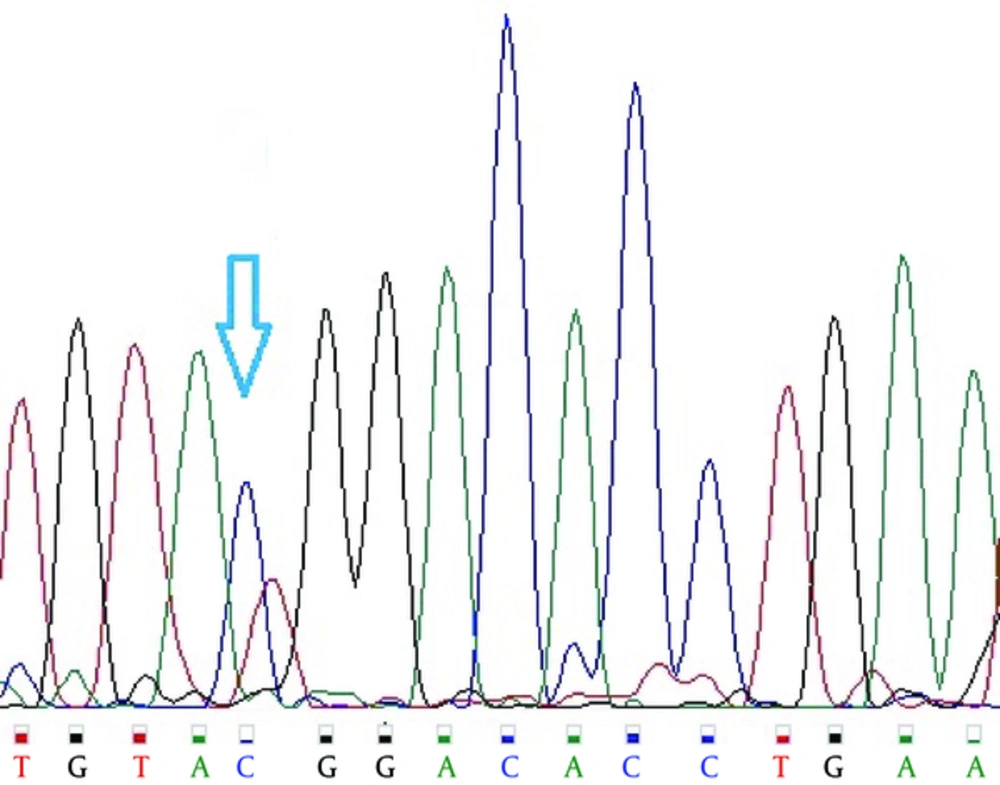
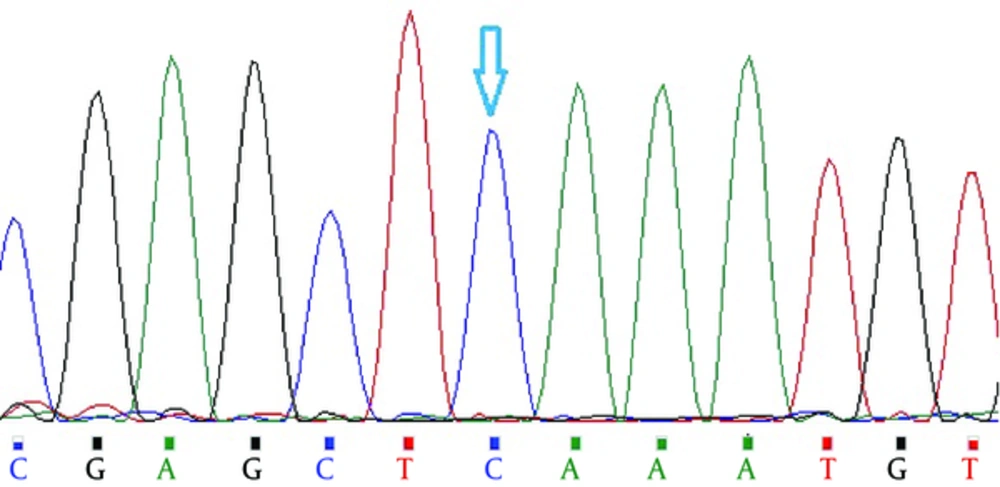
In the case of rs2488457 polymorphism, as shown in Figure 2, after digesting the PCR products with Sac1, the allele -1123G showed a 171-bp band on the gel, while the allele -1123C showed two 147- and 24-bp bands and heterozygote GC had three 171-, 147-, and 24-bp bands; the 24-bp band not observed on agarose gel due to the small size. To verify the results of PCR-RFLP for each polymorphism, 10% of the PCR products were sequenced (Figures 3 and 4).
2.4. Statistical Analysis
Data were analyzed with SPSS version 24.0 (IBM SPSS Statistics 24) and the Hardy-Weinberg equilibrium was tested. The continuous data were expressed as mean ± standard deviation (SD) and the frequencies of the alleles and genotypes in patients and controls were compared using chi-square test. Odds ratio (OR) and 95% confidence interval (CI) were calculated. P value of less than 0.05 was considered significant.
3. Results
The results of clinical and statistical data of patients with SLE are shown in Table 2. Out of 120 patients with SLE tested for anti-dsDNA, 47.5% were positive and 52.5% were negative. Also, among the patients with SLE tested for ANA, 49.2% were positive and 50.8% were negative. The statistical results showed no significant difference in genotype distribution for both +1858C > T (P = 0.551, OR = 1.249, 95% CI = 0.601 to 2.598 and P = 0.502, OR = 1.286, 95% CI = 0.617 to 2.678) and -1123 G > C (P = 0.884, OR = 0.811, 95% CI = 0.049 to 13.512 and P = 0.917, OR = 0.861, 95% CI = 0.052 to 14.347) polymorphisms for the positive patients, compared with the negative ones for ANA and anti-dsDNA factors.
| Genotype | ANAa | P Value | OR (95% CI) | Anti-dsDNAa | P Value | OR (95% CI) | ||
|---|---|---|---|---|---|---|---|---|
| + | - | + | - | |||||
| +1858C > T | ||||||||
| CC | 35(29.2) | 37 (30.8) | - | - | 36 (30) | 36 (30) | - | - |
| CT | 22 (18.3) | 26 (21.7) | 0.551 | 1.249 (0.601 - 2.598) | 21 (17.5) | 27 (22.5) | 0.502 | 2.286 (0.617 - 2.678) |
| TT | 0 | 0 | - | - | 0 | 0 | - | - |
| -1123G > C | ||||||||
| GG | 29 (24.2) | 22 (18.4) | 0.848 | 1.318 (0.07 - 22.263) | 25 (20.9) | 26 (21.7) | 0.978 | 0.962 (0.057 - 16.223) |
| GC | 25 (30) | 37 (30.8) | 0.884 | 0.811 (0.049 - 13.512) | 31 (25.8) | 36 (30) | 0.917 | 0.861 (0.052 - 14.347) |
| CC | 1 (0.8) | 1 (0.8) | - | - | 1 (0.8) | 1 (0.8) | - | - |
aThe variables were only assessed the patients and are presented as No. (%).
3.1. Genotype and Allele Frequencies of the +1858C > T Polymorphism of PTPN22 Gene
The genotype and allele frequencies of +1858C > T in patients with SLE and the controls are shown in Table 3. Genotype frequencies for the PTPN22 1858T SNP were in Hardy-Weinberg equilibrium in the controls. The results showed no significant difference between the allele (P < 0.001) and genotype frequencies (P < 0.001). TT and CT genotypes in patients and controls were 40% and 87%, respectively; in addition, the CC genotype significantly increased in patients (72% vs. 33% in controls, P < 0.001, OR = 3.955, 95% CI = 2.300 to 6.801).
| Variable | Patient, No. (%) | Control, No. (%) | df | P Value | OR | 95% CI | Adjusted ORa (95% CI) |
|---|---|---|---|---|---|---|---|
| Genotype | |||||||
| CC | 72 (60) | 33 (27.5) | 1 | < 0.001 | 0.253 | 0.147 - .0435 | 0.144 - 0.440 |
| CT | 48 (40) | 87 (72.5) | - | - | - | - | - |
| TT | 0 | 0 | - | - | - | - | - |
| Allele | |||||||
| C | 192 (80) | 153 (63.75) | 1 | < 0.001 | 0.44 | 0.291 - 0.663 | - |
| T | 48 (20) | 87 (36.25) | - | - | - | - | - |
aThe adjusted OR for age and gender.
3.2. Genotype and Allele Frequencies of the -1123G > C Polymorphism of PTPN22 Gene
The genotype and allele frequencies of -1123G > C in patients with SLE and the controls are shown in Table 4. Genotype frequencies for the PTPN22 1123G SNP were in the Hardy-Weinberg equilibrium in the controls. Genotype containing allele 1123C (CC and GC) increased in patients with SLE, compared with the controls (57.5% vs. 45.8%); there was no association between the -1123 G > C polymorphism and SLE disease (P = 0.0902, OR = 4.102, 95% CI = 0.794 to 21.193).
| Variable | Patient, No. (%) | Control, No. (%) | df | P Value | OR | 95% CI | Adjusted ORa (95% CI) |
|---|---|---|---|---|---|---|---|
| Genotype | |||||||
| GG | 51 (42.5) | 65 (54.2) | 1 | 0.307 | 2.354 | 0.456 - 12.156 | 0.412 - 11.716 |
| GC | 67 (55.8) | 49 (40.8) | 1 | 0.092 | 4.102 | 0.794 - 21.193 | 0.732 - 20.814 |
| CC | 2 (1.7) | 6 (5) | - | - | - | - | - |
| Allele | |||||||
| C | 169 (70.4) | 179 (74.6) | 1 | 0.307 | 0.811 | 0.543 - 1.212 | - |
| G | 71 (29.6) | 61 (25.4) | - | - | - | - | - |
aThe adjusted OR for age and gender.
4. Discussion
The PTPN22 is recently known as the negative regulator of B- and T-cell receptors in cell signaling pathway. The existence of an allele of PTPN22 (+1858C > T), participating in the R620W mutation, and the existence of a single nucleotide variant (-1123G > C) of this gene, located on its promoter, were demonstrated in SLE and other autoimmune diseases (16). The PTPN22 C1858T allele corresponding to R620W amino acid substitution (arginine to tryptophan) was associated with several autoimmune diseases including SLE.
The frequency of PTPN22 R620W polymorphism is usually very low in general population, but in some regions such as Scandinavia it reaches 15% (17). Various studies showed a heterogeneous allelic distribution in a North-East gradient of the 1858T allele frequency in different populations associated or not associated with PTPN22 C1858T single nucleotide polymorphism for the autoimmune diseases (18-20). The association between PTPN22 1858T and SLE was first reported in white people of North America by Kyogoku et al. (20).
In the present study, the probable association between rs2476601 and rs2488457 polymorphisms of PTPN22 gene and the risk of SLE were studied in a sample of Iranian population. According to the results, there was relationship in rs2476601 polymorphism (P < 0.001, OR = 0.253,95% CI = 0.147 to 0.435) and no relationship in rs2488457 polymorphism (P = 0.0902, OR = 4.102, 95% CI =0.794 to 21.193) and the increased risk of SLE in the studied population. Besides, the comparison of both positive and negative ANA and positive and negative anti-dsDNA genotype frequency in both polymorphisms showed no significant differences. Table 3 shows no relationship between the studied factors and the disease.
Similarly to the results of the current study, Orozco et al., in Span (21), Reddy et al., in Sweden (22) and a study in Egypt (1) confirmed the association between the 1858C > T polymorphism of PTPN22 gene and the development of SLE in patients. Few studies reported no association between PTPN22 polymorphism and SLE. Wu et al., reported no association in this regard among patients with SLE living in North America, Finland, and Great Britain (23). Viken et al., reported the results similar to those of Hui on patients with SLE in Norway and Caucasia (24). Also, Aksoy et al., reported no association between PTPN22 polymorphism and SLE in a study conducted in Turkey (25).
The -1123G > C (rs2488457) is a SNP in the promoter site of a PTPN22; the DNA sequence around this SNP binds to transcription factor AP4, which can affect mRNA expression, and accordingly, the performance of LYP. In this SNP, missense mutation in -1123 position converts G to C; therefore, the -1123 allele can affect the expression of mRNA of PTPN22 and cause dysregulation in B- and T-cells of patients with SLE (13). In the white Europeans, PTPN22 -1123G > C is often expressed with PTPN22 1858C > T (20). A study performed by Feng et al., on patients with rheumatoid arthritis in China (26) and another study by Kawasaki et al., in Asian populations such as Japan and Korea showed the association between rs2488457 (-1123G > C) polymorphism and susceptibility to T1DM (27). In a study in Mexico, there was no association between the -1123G > C and + 1858C > T and D polymorphisms of PTPN22 and the development of SLE (13).
The current study was only conducted on a population of Lorestan province, Iran; hence, more studies including global and regional data are necessary to verify the results. In conclusion, the study showed association between the +1858T allele and no association between-1123C allele of PTPN22, and SLE in the population of the Southwest of Iran, which in second one (-1123 allele) can be attributed to the small sample size in the present study. Therefore, further studies on a greater sample sizes are needed to evaluate the association between the patients with SLE and PTPN22 mutation.