1. Background
Hypertension (HTN) is a major cause of premature death is an important global health issue. World Health Organization estimates that 1.13 billion (20 - 25%) of people have HTN, and nearly two-thirds of them are living in low- and middle-income countries. Only one in five patients with HTN have adequately controlled blood pressure (1). In 2016, 17.9 million (44%) of noncommunicable disease-related deaths were due to cardiovascular disease with HTN as the leading risk factor (2). A systematic review study in Asia revealed that 27% of the population (ranging from 13.6 to 47.9%) had HTN, and a higher prevalence was found in urban people compared to the rural population (3).
In Iran, the overall pooled prevalence of HTN was reported 25% (22 - 28%) (4); and nearly one in four females and males were found to have HTN (4, 5). Organization and implementation of an integrated national plan for prevention and control of HTN in the rural regions of Iran has a long history, and some studies have reported the initiation of the pilot program since 1992 (6), and consequently, this program was extended to rural and urban areas covered by the health centers or family physicians. The Ministry of Health and Medical Education of the Islamic Republic of Iran has organized this national program to increase the identification and control of HTN in the adult population. In this program, a free screening of blood pressure (BP) at designated intervals can facilitate identifying hypertensive patients and conducting follow-up approaches to prevent HTN-related complications and mortality (7). Besides, a mass campaign -named as National Mobilization for the Prevention and Control of HTN (NMPCH; 2019)- for the screening of BP in adults aged 30 years and over was planned in 2019 (from May 17 to July 6), as an additional national program for all provinces of Iran.
Based on the mentioned national program, health centers affiliated to Babol University of Medical Sciences, similar to other Iranian medical universities providing healthcare services to the rural and urban population, initiated an operational plan to examine the BP of adults at scheduled intervals, and the individuals identified as hypertensive or prehypertensive cases should receive regular care or treatment plans.
2. Objectives
This study was done to describe this BP screening campaign (NMPCH; 2019) and to identify the strengths and weaknesses of the program in comparison with routine BP screening data collected over the past 15 years.
3. Methods
This historical cohort was conducted in 2019 - 2020 at Babol University of Medical Sciences, north of Iran. Data related to the 2019 BP screening mass campaign in adult people (NMPCH; 2019) were collected. All people aged 30 and over in different areas were invited to participate in the campaign. BP screening was performed free of charge in defined stations and health centers. In order to inform the study population about this program, information was provided through national and regional mass media, governmental organizations, health centers, mosques and other public places, and family physicians. No sampling was carried out, and all individuals aged ≥ 30 years who had been referred for this screening program were included in the study by the census.
Age, gender, marital status (defined as married versus never married, widowed, or divorced), where the adults have been screened (including rural health homes, urban and rural health centers, family physicians' offices, and screening stations located in different regions of the city), the amount of systolic and diastolic BP and the final diagnosis (normal BP, prehypertensive or hypertensive) were analyzed.
BP was measured in a sitting position, after 15 minutes of rest, with calibrated digital sphygmomanometers. In pregnant women, BP was measured while sitting or lying on the left side. Before a person was ready to be evaluated, the conditions, such as no smoking or drinking tea and coffee, were considered. The BP would be measured for the second time, five minutes after the first time, if the systolic BP (SP) was 140 mm Hg or more, or the diastolic BP (DP) was 90 mm Hg or higher; and mean systolic and diastolic BP was recorded. BP less than 120 / 80 mm Hg was considered as normal BP, and when the SP was 120 - 139 or the DP was 80 - 90 mm Hg, the person was classified as a prehypertensive case. Mean BP ≥ 140 / 90 mm Hg or taking antihypertensive medication was defined as HTN (7). Pulse pressure (PP) was calculated as the difference between the SP and DP, and mean arterial pressure (MAP) was calculated using the following formula (8):
or
Since the free-of-charge screening of the population aged 30 and over in rural and urban areas by the governmental health centers and family physicians has a long history in Babol, north of Iran (in the rural area longer than 15 years and in the urban area nearly for 7 years), the data collected in 2019 NMPCH program were compared with the health system information that has been recorded during the years 2004 - 2019.
Data analysis was conducted by SPSS 17 software using t-test, Chi-square test, logistic regression model, and one-way ANOVA. A P-value of less than 0.05 was considered significant.
This research was approved by the Ethics Committee of Babol University of Medical Sciences (ID: IR.MUBABOL.HRI.REC.1398.248).
4. Results
Totally, 220,241 adult people, with a mean age of 49.82 ± 14.26 (range: 30 - 105) years, including 134,638 (61.1%) female and 85,603 (38.9%) male have been screened in Babol for 2019 -NMPCH. Of these, 110,132 cases (50.0%) were living in urban area and 110,109 (50.0%) in rural regions; 191,700 cases (87.0%) were married and 28,541 cases (13.0%) were unmarried. Age distribution of the participants showed that 66,279 cases (30.1%) were in the age group of 30 - 39; 53,621 cases (24.3%) in 40 - 49; 46,352 cases (21.0%) in 50 - 59; 30,186 cases (13.7%) in 60 - 69; 15,211 cases (6.9%) in 70 - 79; and 8,592 cases (3.9%) were in the age group of 80 years and over. The mean age was 50.56 ± 14.41 years for men and 49.35 ± 14.15 years for women (P < 0.0001).
Data represented that in 109,250 (49.6%) of the examined individuals, BP had been measured by the health care providers working in rural health homes; 41,861 (19.0%) by the family physicians working in the urban area, 7,496 (3.4%) by the family physicians working in the rural area, 19419 cases (8.8%) had referred to the screening stations located in the crowded parts of the city, and 42,215 (19.2%) by other healthcare providers working in the health centers affiliated to Babol University of Medical Sciences.
In this mass campaign, 42,107 (19.1%; 95% CI: 18.95 - 19.28%) of the individuals had HTN, either new cases of HTN or previously diagnosed patients, 112,406 cases (51.0%) had normal BP, and 65,728 cases (29.8%) had been diagnosed as prehypertensive cases. Mean, standard deviation, minimum, and maximum of SP, DP, MAP, and PP were 114.74 ± 13.05 mm Hg (60 -270), 71.60 ± 8.99 mm Hg (40 - 148), 85.98 ± 9.53 mm Hg (46.67 - 183.33), and 43.14 ± 9.44 mm Hg (10.00 - 145.00), respectively. The older the age, the higher frequency of HTN; as in people aged 50 years or older, at least 1 in 4, and in ≥ 70 years old more than 1 out of 2 cases had HTN.
After controlling for demographic covariates, the logistic regression models showed significantly higher odds of HTN for married individuals (adjusted OR = 1.23; 95% CI: 1.19 - 1.27; P < 0.0001) and living in urban regions (adjusted OR = 1.84; 95% CI: 1.79-1.88; P < 0.0001). The prevalence of HTN showed no significant difference between men and women (P = 0.476).
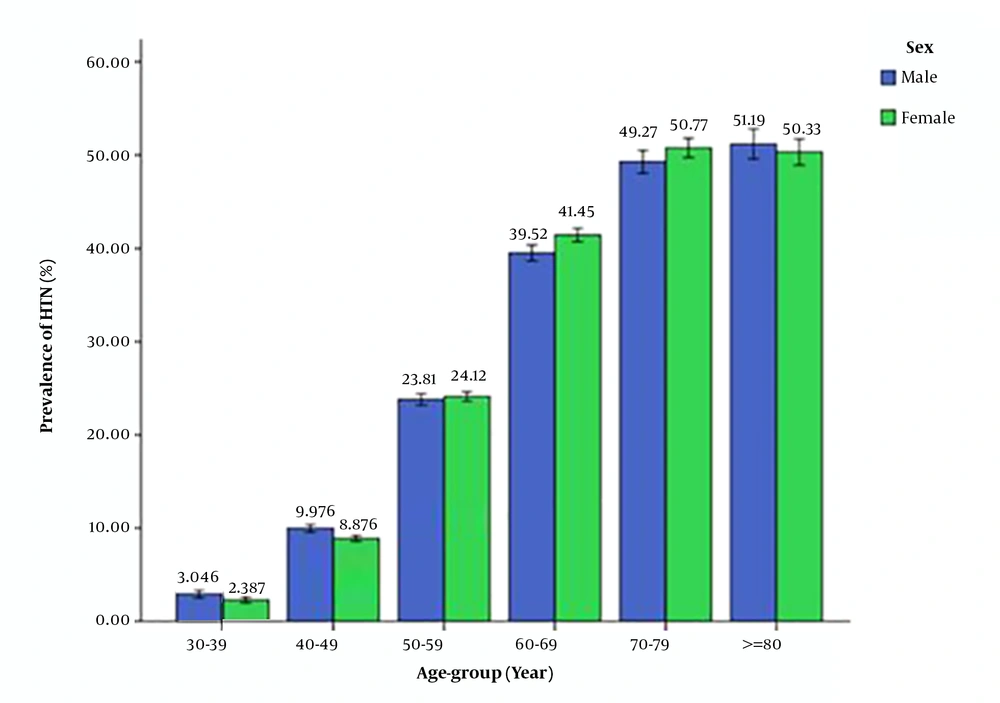
Mean SP, DP, MAP, and PP based on the participants' gender, living area, and marital status are presented in Table 1, and the prevalence of HTN among men and women and in different age groups is displayed in Figure 1.
| Characteristics | Systolic Blood Pressure (mm Hg) | P-Value | Diastolic blood pressure (mm Hg) | P-Value | Mean Arterial Pressure (mm Hg) | P-Value | Pulse Pressure (mm Hg) | P-Value |
|---|---|---|---|---|---|---|---|---|
| Gender | < 0.001 | < 0.001 | < 0.001 | < 0.001 | ||||
| Male (n = 85,603) | 116.12 ± 12.81 | 72.79 ± 8.56 | 87.23 ± 9.17 | 43.32 ± 9.36 | ||||
| Female (n = 134,638) | 113.87 ± 13.13 | 70.84 ± 9.17 | 85.18 ± 9.67 | 43.03 ± 9.49 | ||||
| Age (y) | < 0.001 | < 0.001 | < 0.001 | < 0.001 | ||||
| 30 - 39 (n = 66,279) | 109.57 ± 10.31 | 68.83 ± 8.27 | 82.41 ± 8.13 | 40.75 ± 8.19 | ||||
| 40 - 49 (n = 53,621) | 112.76 ± 11.78 | 70.92 ± 8.86 | 84.87 ± 9.05 | 41.84 ± 8.66 | ||||
| 50 - 59 (n = 46,352) | 116.96 ± 13.19 | 73.04 ± 8.98 | 87.68 ± 9.58 | 43.92 ± 9.47 | ||||
| 60 - 69 (n = 30,186) | 120.35 ± 13.69 | 74.25 ± 8.81 | 89.61 ± 9.57 | 46.10 ± 10.07 | ||||
| 70 - 79 (n =15,211) | 122.11 ± 14.36 | 74.61 ± 8.90 | 90.44 ± 9.78 | 47.50 ± 10.79 | ||||
| ≥ 80 (n = 8,592) | 122.30 ± 14.13 | 74.79 ± 8.94 | 90.63 ± 9.73 | 47.51 ± 10.63 | ||||
| Living area | < 0.001 | < 0.001 | < 0.001 | < 0.001 | ||||
| Urban (n = 110,132) | 115.68 ± 12.98 | 72.46 ± 8.77 | 86.87 ± 9.38 | 43.23 ± 9.34 | ||||
| Rural (n = 110,109) | 113.80 ± 13.06 | 70.74 ± 9.12 | 85.09 ± 9.59 | 43.06 ± 9.54 | ||||
| Marital status | < 0.001 | < 0.001 | < 0.001 | < 0.001 | ||||
| Married (n = 191,700) | 114.72 ± 13.00 | 71.62 ± 8.99 | 85.99 ± 9.52 | 43.09 ± 9.39 | ||||
| Not being married (n = 28,541) | 114.92 ± 13.41 | 71.43 ± 8.95 | 85.93 ± 9.59 | 43.49 ± 9.81 |
The association between the examined characteristics and the occurrence of HTN is presented in Table 2.
| Characteristics | Those with Hypertension, No. (%) | Crude Odds Ratio (95% CI for Crude Odds Ratio) | P-Value | Adjusted Odds Ratio (95% CI for Adjusted Odds Ratio)a | P-Value |
|---|---|---|---|---|---|
| Gender | < 0.0001 | 0.476 | |||
| Male (n = 85,603) | 17,100 (19.98) | ||||
| Female (n = 134,638) | 25,007 (18.57) | M / F = 1.09 (1.07-1.12) | 0.99 (0.97 -1.02) | ||
| Age (y) | < 0.0001 | < 0.0001 | |||
| 30-39 (n = 66,279) | 1,740 (2.63) | Reference | Reference | ||
| 40 - 49 (n=53,621) | 4,986 (9.39) | 3.80 (3.60 - 4.02) | 4.02 (3.80 - 4.25) | ||
| 50-59 (n = 46,352) | 11,123 (24.00) | 11.71 (11.12 - 12.34) | 12.51 (11.87 -13.18) | ||
| 60-69 (n = 30,186) | 12,274 (40.67) | 25.42 (24.11 -26.80) | 27.75 (26.31 -29.26) | ||
| 70-79 (n = 15,211) | 7,628 (50.15) | 37.31 (35.24 - 39.51) | 42.25 (39.87 -44.77) | ||
| ≥ 80 (n = 8,592) | 4,356 (50.70) | 38.14 (35.79 - 40.65) | 42.92 (40.21 -45.80) | ||
| Living area | Urban / Rural=1.36 (1.33 - 1.39) | < 0.0001 | 1.84 (1.79 -1.88) | < 0.0001 | |
| Urban (n =110,132) | 23,634 (21.5) | ||||
| Rural (n=110,109) | 18,473 (16.8) | ||||
| Marital status | Married / Not married = 0.70 (0.68 - 0.72) | < 0.0001 | 1.23 (1.19 -1.27) | < 0.0001 | |
| Married (n = 191,700) | 35,177 (18.4) | ||||
| Not being married (n = 28,541) | 6,930 (24.3) |
aAll the four mentioned characteristics, including age, gender, living area, and marital status were entered in logistic regression analysis.
Table 3 shows the examined people in the integrated health system program for screening of BP in Babol, from 2004 to 2018. This table can be representative of the advantage of the 2019 mass campaign to cover the target population.
| Year | Total adult population aged 30 years and over | Hypertension (+), No. (%) | Hypertension (-), No. (%) | Considerations |
|---|---|---|---|---|
| 2004 | 98,130 | 4,677 (4.8) | 93,453 (95.2) | Only the rural population had been considered as the target group. |
| 2005 | 100,097 | 5,109 (5.1) | 94,988 (94.9) | Only the rural population had been considered as the target group. |
| 2006 | 103,607 | 6,006 (5.8) | 97,601 (94.2) | Only the rural population had been considered as the target group. |
| 2007 | 103,607 | 6,062 (5.9) | 97,545 (94.1) | Only the rural population had been considered as the target group. |
| 2008 | 107,562 | 6,721 (6.2) | 100,841 (93.8) | Only the rural population had been considered as the target group. |
| 2009 | 110,509 | 6,985 (6.3) | 103,524 (93.7) | Only the rural population had been considered as the target group. |
| 2010 | 106,497 | 7,550 (7.1) | 98,947 (92.9) | Only the rural population had been considered as the target group. |
| 2011 | 108,252 | 7,771 (7.2) | 100,481 (92.8) | Only the rural population had been considered as target group. |
| 2012 | 111,277 | No information was found | Only the rural population had been considered as the target group. | |
| 2013 | 112,809 | 2,023 (1.8) | 110,786 (98.2) | Family physician program was started in urban areas besides to rural area; however, a comprehensive information system was not available. |
| 2014 | 115,804 | No information was found | ||
| 2015 | 115,804 | No information was found | ||
| 2016 | 115,804 | No information was found | ||
| 2017 | 129,428 | 10,789 (8.3) | 118,639 (91.7) | |
| 2018 | 129,428 | No information was found | ||
5. Discussion
More than 220,000 adult people aged 30 years and older were recruited in this mass campaign, and their BP was examined. Women showed more participation in this program than men; the rate of referral of women was 1.6 times higher than that of men. A volunteer-based campaign named May Measurement Month (MMM) was implemented in 2017 in some European countries, such as the United Kingdom and the Republic of Ireland, in which 77,014 adults aged 18 years and over were screened. The results showed that 23.4% of the examined people had raised BP, and 40.5% of the previously recognized patients taking antihypertensive drugs had uncontrolled BP. Also, women participated more than men (F / M = 61/39) (9). In 2018 MMM, in which 89 countries participated, 1,504,963 individuals were examined, and 33.4% of them had raised BP. More women than men were screened in different regions except for the Middle East, South Asia, and North Africa (10). Another similar mass campaign in Jamaica in 2017, in which 566 adults were recruited, 47.3% of the participants had HTN, and no gender difference was observed in the screened population (11). Sociodemographic characteristics, lifestyle behaviors, race, and ethnicity can cause such differences in the prevalence of HTN in different regions. Also, the literature review represents more healthcare-seeking behaviors in women than men (12, 13).
No significant difference was observed in the percentage of rural and urban people who had participated in this mass campaign. Individuals who were living in rural areas were mostly visited by healthcare providers working in rural health homes; however, the urban population had been screened by their family physicians or other healthcare providers working in the governmental health centers. In the 2018 MMM program, lower-middle-income countries showed a higher percentage of participants (54.4%) than other countries (10). A similar percentage of rural and urban participants in Babol in the 2019 Iranianian campaign can be due to public health program coverage in this city. The rural health homes, even in the furthest rural areas, the family physicians and healthcare providers in rural and urban health centers facilitated free BP screening of people. Furthermore, during the mentioned campaign, awareness of the target population via mass media, such as national and local radio, television, and social networks, might trigger them to refer to be examined.
Nearly 19% of adult people aged ≥ 30 years were recognized as hypertensive patients; also, more than 66,000 individuals had referred to their related healthcare teams to care as a prehypertensive group. The prevalence of HTN was 13.6 - 47.9% in Asia (3) and 22 - 28% in Iran (4). The National Action Plan for the prevention and control of noncommunicable diseases and their related risk factors in Iran has involved all Medical Sciences Universities with their health services to cover all regions of the country. A reduction in the prevalence of raised BP or the current prevalence of HTN has been emphasized in this strategic plan (14). Individuals identified as prehypertensive cases should be examined regularly by related health centers and family physicians based on a defined national protocol.
In this research, older age, being married, and living in urban areas were found as factors to increase the risk of HTN. Recent evidence showed that macroscopic and microscopic changes that occur in the heart, vascular system, and autonomic nervous system with increasing age make a person prone to have raised BP at older ages (15). Previous studies reported different results about the association of marital status and raised BP (16). For example, a longitudinal study in Iran revealed that being never married was correlated with a higher risk of HTN in men (17). A study in Ghana represented higher odds of HTN for married, cohabiting, or previously married women; however, no significant association was observed between marital status and HTN for men (18). It seems that marriage may have both positive and negative impacts on BP; socioeconomic status of the couple, quality of marriage, and supportive behaviors in marital relationships are effective in the association between marriage and BP (16).
Some previous studies reported low physical activity, lower consumption of fruit and vegetables, and more fast food intake correlated with a higher prevalence of HTN in urban regions of Iran (19).
Although HTN was more common in men at the beginning of the data analysis process, no significant statistical difference was found between men and women after controlling the covariates. Various mechanisms have been listed to describe gender differences in HTN, such as hormonal differences, pregnancy-associated factors, where the BP was being examined (might cause white coat HTN), sympathetic nervous activity, renin-angiotensin system, immunoregulatory mediators, and endothelin activity (20).
Data related to the current health care services during the last 15 years showed that the prevalence of registered patients with raised BP was a maximum of 8.3% of the population aged 30 years and over. The national 2019 mass campaign provided an opportunity for adults to be screened for BP during a short time -less than two months- and to be referred to the relevant health units for further care if they have been identified as hypertensive or prehypertensive cases. Higher coverage of the screened population in 2019 NMPCH resulted in a higher percentage of patients with HTN being identified and registered compared with the routine health system program.
Considering HTN as the most common preventable risk factor for cardiovascular diseases, chronic kidney disease, and cognitive impairment, and the leading single contributor to all-cause mortality and morbidity worldwide (21), inexpensive, structured, time-bounded, and population-based programs for the promotion of BP screening in adults and high-risk populations are recommended.
The most important strength of this study is the large size of the study population. It was the first mass campaign of BP screening in Iran, including all provinces of the country. Drug regimen, lifestyle behaviors, and anthropometric indices had not been assessed in this campaign. Lack of evaluation of these factors can be mentioned as the limitations of this study.
5.1. Conclusions
As nearly one in five out of the 220,241 people aged ≥ 30 years who were studied in this research had HTN, and nearly 30% had been diagnosed as prehypertensive individuals. A continuous BP screening program is recommended in this region. Raised BP was increased when individuals had older age, were married, or living in urban regions.