1. Context
The aging of the population and the consequent increase in chronic diseases, such as stroke, have imposed a great socioeconomic burden on most countries around the world. Stroke is one of the main causes of premature death and disability, imposing significant costs on the healthcare systems, especially due to costly hospital care (1). Patients with stroke suffer from one or more health problems, such as physical, cognitive, behavioral, and emotional complications, which are expected to increase with aging and advances in treatment methods (2).
The economic burden of stroke is another important problem that imposes direct and indirect costs on households and governments. Besides the costs of hospitalization, nursing care, medications, and equipment, there are some indirect costs related to the loss of productivity in stroke patients (2). Until 2020, the lifetime cost was estimated to range between $ 59,800 and $ 230,000 per stroke (3). Therefore, policymakers, health system researchers, and healthcare providers need to seek solutions for developing cost-effective measures to treat patients with stroke and reduce their disability (1).
Rehabilitation services can help maximize the functional, emotional, mental, psychological, and social independence of individuals, which is of particular importance in both acute and chronic diseases. Rehabilitation programs can be established in various facilities (4). One of the interventions considered by policymakers in different countries in the last two decades is home care services. Factors, such as the increased number of the elderly, the subsequent increase in chronic diseases, lack of access to hospital services, advances in technology, and the subsequent provision of medical services at home, have resulted in the prioritization of these services in health care (5).
There have been several studies on the costs and consequences of home care for stroke patients, and comparisons have been made with other strategies; however, relatively different results have been reported. The results of some studies indicated that home care does not reduce the costs, but improves the health outcomes (2). The cost-effectiveness studies of home care have also provided conflicting results. While some studies have emphasized the high cost-effectiveness of home care (6-8), others have shown that home care for stroke patients is not only more expensive, but also less effective (9). Therefore, a comprehensive review of studies on the economic evaluation of home care and comparisons with other strategies are needed to select the best solution for providing care for patients with stroke. This study aimed to systematically review previous studies to compare home care and hospital care for stroke patients.
2. Methods
2.1. Inclusion and Exclusion Criteria
The eligibility criteria were defined based on the Population, Intervention, Comparison, Outcomes, and Study (PICOS) framework. The study population included patients with stroke in any age group. The intervention (comparison) group included home care for rehabilitation services (hospital care for rehabilitation services); the outcome was economic evaluation; and the study type was randomized clinical trial. Studies comparing home care with other types of care, including out-of-hospital outpatient services and care provided in long-term care facilities, were excluded, similar to web-based home care studies. The search identified studies published in English language between January 1, 1990 and January 31, 2021.
2.2. Data Sources
A systematic electronic search was performed in the following databases: PubMed, Scopus, Web of Science, and Embase. Besides, we searched the Google search engine and Google Scholar using the same keywords, scanned the references of relevant studies, and contacted the authors and experts to identify additional research and grey literature.
2.3. Literature Search
For a systematic search, a combination of keywords was used in this study. The search strategy for all databases is described in Table 1. Besides the electronic search, the reference lists of the included studies were also scanned for relevant articles.
| Databases | Search Strategy | Results |
|---|---|---|
| PubMed | (((((("Cost-benefit analysis" [Mesh]) OR "Cost-effectiveness" [Title/Abstract]) OR "cost effectiveness" [Title/Abstract]) OR "Economic evaluation*" [Title/Abstract])) AND ((((((("Stroke" [Mesh]) OR "Stroke*" [Title/Abstract]) OR "Cerebrovascular accident*" [Title/Abstract]) OR "Cerebrovascular apoplexy" [Title/Abstract]) OR "CVA" [Title/Abstract]) OR "Apoplexy" [Title/Abstract]) OR "Brain vascular accident" [Title/Abstract])) AND (((((("Home care services" [Mesh]) OR "Home nursing" [Mesh]) OR "Home nursing" [Title/Abstract]) OR "Domiciliary care" [Title/Abstract]) OR "Home health" [Title/Abstract]) OR "Home care*" [Title/Abstract]). | 53 |
| WOS | (TS= ("Cost effectiveness" OR "Cost-effectiveness" OR "Economic evaluation*")) AND (TS= ("Stroke*" OR "Cerebrovascular accident*" OR "Cerebrovascular apoplexy" OR "CVA" OR "Apoplexy" OR "Brain vascular accident")) AND (TS= ("Home nursing" OR "Domiciliary care" OR "Home health" OR "Home care*")) | 31 |
| Scopus | (TITLE-ABS-KEY: ("cost effectiveness" [Title/Abstract] OR "Cost-effectiveness" OR "Economic evaluation*") AND TITLE-ABS-KEY: ("Stroke*" OR "Cerebrovascular accident*" OR "Cerebrovascular apoplexy" OR "CVA" OR "Apoplexy" OR "Brain vascular accident") AND TITLE-ABS-KEY: ("Home nursing" OR "Domiciliary care" OR "Home health" OR "Home care*")). | 106 |
| Embase | ("Cost-effectiveness analysis"/exp. OR "cost-effectiveness" OR "Cost effectiveness" OR "economic evaluation") AND "Cerebrovascular accident"/exp. OR "CVA" OR "(accident AND Cerebrovascular) OR "Acute cerebrovascular lesion" OR "Acute focal cerebral vasculopathy" OR stroke OR "Apoplexy" OR ("Blood flow disturbance" AND Brain) OR "Brain accident" OR "Brain attack" OR "Brain insult" OR "Brain insultus" OR "Brain ischaemic attack" OR "Brain ischemic attack" OR "Brain vascular accident" OR "Cerebral apoplexy" OR "Cerebral insult" OR "Cerebral stroke" OR "Cerebral vascular accident" OR "Cerebral vascular insufficiency" OR "Cerebrovascular accident" OR "Cerebrovascular arrest" OR "Cerebrovascular failure" OR "Cerebrovascular injury" OR "Cerebrovascular insufficiency" OR "Cerebrovascular insult" OR "Cerebral vascular accident" OR "Cryptogenic stroke" OR "Ischemic cerebral attack" OR "Ischemic seizure" OR "Ischemic cerebral attack" OR "Ischemic seizure" OR "Stroke") AND ("Home care"/exp. OR "Domestic health care" OR "Domiciliary care" OR "Home care" OR "Home health care" OR "Home health nursing" OR "Home help" OR "Home nursing" OR "Home service" OR "Home treatment" OR "Homemaker services") | 129 |
2.4. Study Selection
The PRISMA guidelines were used to screen the studies. The search results were entered into EndNote reference management software, and duplicate references were identified and removed. After removing duplicates, two authors screened the titles and abstracts of the articles, and then, the full-text of relevant studies was read for eligibility, based on the inclusion and exclusion criteria. Eligible studies were included in our review.
2.5. Data Extraction
Data, including the study details (authors, year of publication, country, and type of study), study perspective, type of economic evaluation, time horizon, study population, sample size, outcomes, cost-effectiveness ratio, and main findings, were collected. Data extraction was carried out independently by two authors, and any disagreement was resolved through discussion; a third author was also available to resolve disagreements.
2.6. Risk of Bias in Individual Studies (Quality Assessment)
Drummond’s ten-item checklist (1996) was used for the quality assessment of studies (10); studies with a score of seven were identified as qualified and included in the study. The Drummond checklist is a tool for assessing the quality of economic evaluation studies and a useful guide for conducting these studies. This checklist contains ten questions and considers (1) the specific research question; (2) description of the alternatives; (3) assessment of the effectiveness of the program or service; (4) identification of the costs and consequences of all alternatives; (5) measurement of the costs and consequences based on appropriate physical units; (6) valid evaluation of costs and consequences; (7) adjustment of costs and consequences for differential timing; (8) incremental analysis of costs and consequences of alternatives; (9) analysis of uncertainty in estimating the costs and consequences; and (10) review of all issues in discussion (11).
3. Results
3.1. Study Selection
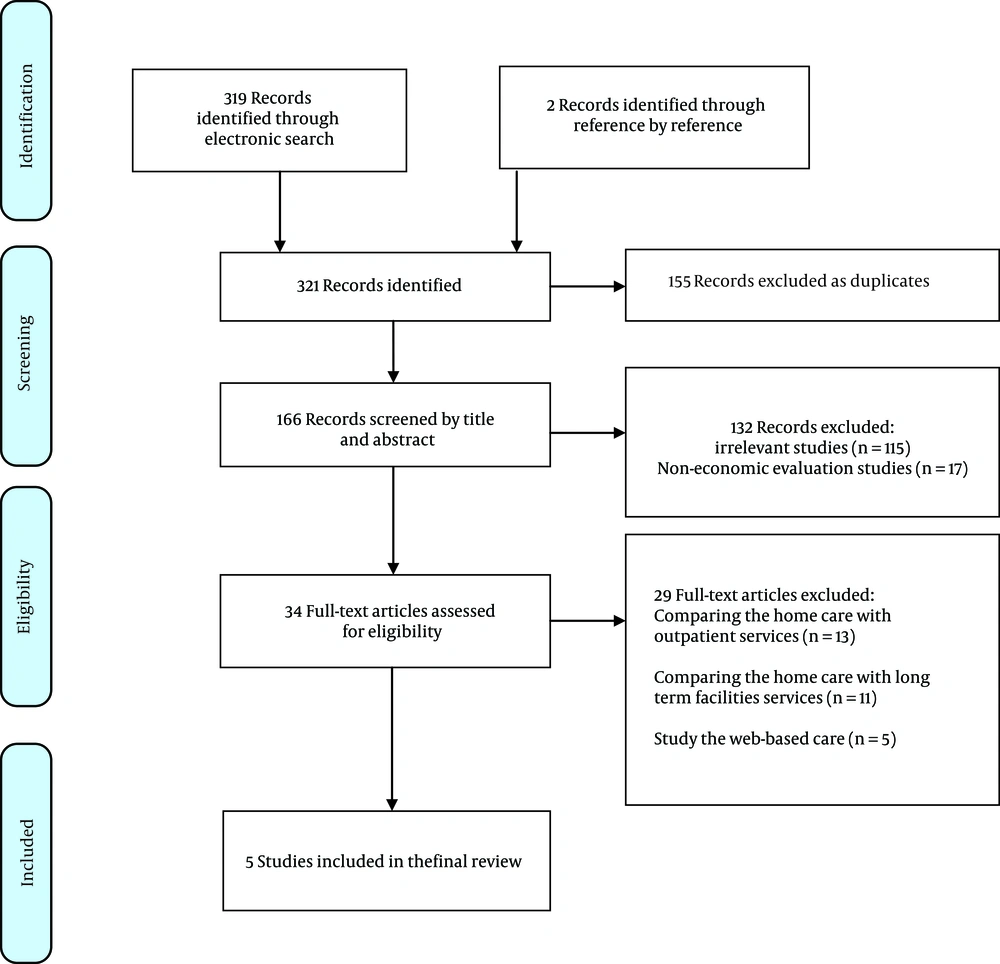
A total of 251 studies were identified through our systematic search and two studies through our review of the reference lists of the included studies. After removing duplicates, the titles and abstracts of 155 articles were screened, and the full-text of 14 studies was read based on the inclusion criteria. Finally, five economic evaluation studies were included in this review. The study screening process is shown in Figure 1.
3.2. Study Characteristics and Results of Individual Studies
All studies, with the exception of the study by Sritipsukh et al. (6), were conducted in the United Kingdom. In most studies, a cost-effectiveness analysis was conducted, and the costs were investigated from the provider’s perspective. The studied outcomes were quality of life and physical ability in most studies, and only in two studies, the incremental cost-effectiveness ratio (ICER) was reported. A summary of the study characteristics and results is presented in Tables 2 and 3.
| Authors, Year | Country | Study Design | Economic Evaluation | Perspective | Time Horizon | Population/Sample Size (Intervention/ Comparison) | Outcome Measure(S) |
|---|---|---|---|---|---|---|---|
| Patel et al., 2004 (12) | UK | RCT | Cost-effectiveness and cost-utility analysis | Societal | 12 months | Acute stroke patients; Stroke unit: 152; Domiciliary stroke care: 153. | Number of deaths, institutionalizations, and QALYs gained |
| Sritipsuk et al., 2010 (6) | Thailand | RCT | Cost-effectiveness analysis | Provider | 3 months | Ischemic stroke patients; Home rehabilitation: 30; Conventional hospital care: 28. | The Barthel index (for patients with mild disability and no disability) and mDS |
| Roderick et al., 2001 (13) | UK | RCT | Cost-effectiveness analysis | Provider/societal | 6 months | Stroke patients aged above 55 years; Domiciliary care: 54; Day hospital: 58. | Physical function (Barthel index), mobility index, mental state index, and social activity index |
| Young et al., 1993 (14) | UK | RCT | Cost-effectiveness | Provider/patient | 8 weeks | Patients with a new stroke; Home-based physiotherapy: 52; Hospital physiotherapy: 43. | Physical function (Barthel index) |
| Gladman et al., 1994 (15) | UK | RCT | Cost comparison | Provider | 6 months | Acute stroke patients; Domiciliary group: 162; Hospital care group: 165. | Extended Activities of Daily Living (ADL) scale (with three subscales of mobility, household ability, and leisure activity) and the Nottingham Health Profile |
Abbreviation: RCT, randomized controlled trial
| Authors, year | ICER | Main results |
|---|---|---|
| Patel et al., 2004 (12) | Total health and social care costs: Per additional 1% of deaths/institutionalizations avoided: 496. Per additional QALY gained: 64,097. | Home care was a more cost-effective option than the stroke team services in reducing mortality and institutionalization of stroke patients, but the costs and effectiveness of the stroke unit were higher than home care. At the implicit threshold per QALY in the United Kingdom (30,000 ₤), home care was considered as the most cost-effective option. |
| Total costs including informal care: Per additional 1% of deaths/institutionalizations avoided: 682. Per additional QALY gained: 89,132. | ||
| Sritipsuk et al., 2010 (6) | Barthel index (mild disability): 14,212 THBa, b | Compared to hospital care, providing a more expensive home rehabilitation program reduced the disability of a large number of patients, and the cost-effectiveness of home care was higher than hospital care based on the indicators studied. |
| Barthel index (no disability): 24,364 THB | ||
| Modified Rankin Scale (mRS): 13,644 THB. | ||
| Roderick et al., 2001 (13) | Not stated. | The costs of health services were the same in the two groups of home and hospital rehabilitation, but the cost of social services was higher in the home care group. The average cost of rehabilitation per patient was similar in both groups. |
| Home care was more effective in improving the physical function indicators than hospital care, while social function and mental health remained low. Differences in the physical function indicators were not statistically significant. | ||
| Home care and hospital care for rehabilitation of elderly patients showed the same cost-effectiveness. | ||
| Young et al., 1993 (14) | Not stated. | The cost of rehabilitation services at hospitals was 61% higher than home care, and its effectiveness in improving the indicators was low. Therefore, rehabilitation at home was more effective than hospitalization. |
| Gladman et al., 1994 (15, 16) | Not stated. | There was no significant difference in the effectiveness of the two strategies, but hospital care was 27% less costly than home care. |
| For patients discharged from the geriatric wards, daily hospital services were 2.4 times more effective in reducing mortality and institutionalization than home care. However, the cost of hospital care was higher than home care. | ||
| For stroke unit patients, the effectiveness of home care in terms of patients' household and leisure activities was higher than that of outpatient services. However, the cost of outpatient services was 2.6 times higher than home care | ||
| For patients from general medicine wards, the outcomes were the same for the two strategies. However, the cost of outpatient services was 56% of home care costs. Therefore, outpatient services were a more cost-effective option. |
aThai Baht
bThe exchange rate in 2008 was 33.36 THB for US$1.
The included studies reported different results regarding the effects of home care on improving different indicators and the cost-effectiveness ratio of home care and hospital care. The results of most studies revealed that providing rehabilitation services at home was a more cost-effective option than rehabilitation at hospital for improving many indicators, such as the patient’s physical function and quality-adjusted life year (QALY), and for reducing mortality and institutionalization.
3.3. Risk of Bias in Studies
The quality of studies was evaluated based on the Drummond checklist, and all studies were scored above seven. The results of the quality assessment of studies are presented separately in the checklist questions in Appendix 1.
3.4. Synthesis of Results
Since the included studies were highly heterogeneous, it was not possible to combine the results and analyze them quantitatively.
4. Discussion
So far, few studies have been published on the economic evaluation of home care as an alternative for hospital services in stroke patients. This study aimed to compare home care and hospital services for stroke patients. The results of two out of these five studies showed that home care was a more cost-effective option for reducing disability among stroke patients compared to hospital care. We identified 5 relevant studies that generally had good quality. In these studies, improvement in the Barthel index was a common outcome. In the Sritipsukho et al.'s study (6), in addition to the Barthel index, the Modified Rankin Scale (mRS) was also used to assess the improvement of patients’ physical performance. The results of this study showed that home care imposed more direct costs than conventional hospital care; meanwhile, it could be more effective in reducing the patients' disabilities.
The amount of ICER required for improvement from major to minor stroke based on the MRS index, achieving mild disability, and achieving no disability based on the Barthel index was 13,644, 14,212, and 24,364 Thai Baht, respectively. The cost of avoiding disability in one additional patient was one-fourth of the recommended cost of adding one QALY, based on the Thai national guidelines; therefore, home care was considered as a cost-effective option for reducing disability among stroke patients in Thailand (6). According to the results of Young et al.'s study, there was no significant difference between home care and hospital care in terms of improving the Barthel index (17). They examined the costs of two interventions, and their findings showed that home care had less direct costs than hospital care. Similar results were obtained even when indirect costs, including the emotional distress of the patient and main caregiver, were added to the analysis (14).
Besides disability and QALY, mortality and hospitalization have been also studied as important outcomes in comparing the cost-effectiveness of home care versus hospital care for stroke patients. Patel et al. (12) showed that home care was a more cost-effective option for reducing mortality and institutionalization in stroke patients, compared to medical services provided by the stroke team; however, the cost and effectiveness of the stroke unit were higher than home care. In this study, the costs of health services and providers, other formal care agencies, and informal caregivers were included in calculating the total societal costs.
Informal costs were considered to account for a large percentage of the total cost, which was higher in patients admitted to the stroke unit compared to other patients. According to the results of the sensitivity analysis, if the patient was not willing to pay for the QALYs gained, home care was more likely to be the cost-effective option. As the patient’s willingness to pay up to ₤ 60,000 increased, the probability of cost-effectiveness for the stroke team and the stroke unit increased, as well. However, at the implicit threshold per QALY in the United Kingdom (₤ 30,000), home care was considered as the most cost-effective option (12).
In another study by Gladman et al., the Extended Activities of Daily Living (ADL) scale and the Nottingham Health Profile were used to measure the stroke patients’ outcomes. According to the results of this study, there was no significant difference in the effectiveness of home care and hospital care. However, the cost of hospital services was lower than that of home care. Patients in this study were divided into three groups based on the severity of their disease. The first group included patients, who were discharged from the geriatric wards and were more likely to die or be institutionalized, including patients who were older, disabled, and had a severe stroke or cognitive impairment. Patients who received daily hospital services were less likely to die or be institutionalized compared to their counterparts who received home care. However, the costs of hospital care were higher than home care. For this subgroup, the ICERs were not calculated, and no sensitivity analysis was performed to determine the cost-effectiveness of the two interventions (15, 16). In another study by Roderick et al., the cost-effectiveness of home care versus geriatric day-hospital care was assessed for older adults (> 55 years). In this study, the participants in the two groups were well-balanced in terms of age, sex, social class, and the initial Barthel index. The physical function (Barthel index), Rivermead Mobility Index, mental status, social activity, and health status were the outcomes of this study. According to their results, the costs and effectiveness of the two services were not significantly different; therefore, no significant difference was found in the cost-effectiveness of the two strategies. While the cost of health services was lower in home care, the cost of social services was higher than hospital care (13).
It seems that home care for high-risk stroke patients, including older adults, is not a more cost-effective option than hospital care. While there was no significant difference in the cost-effectiveness of home care and hospital care in improving the physical and mental performance of elderly patients, hospital care was a more effective strategy for reducing the mortality and hospitalization of high-risk patients. If these patients were willing to pay for the additional costs of hospital care, hospital care might be a cost-effective strategy.
The second and third groups of patients in the study by Gladman et al. included patients discharged from the stroke unit and general medical wards, respectively. In patients discharged from the stroke unit, the effectiveness of home care in improving the patients' household and leisure activities and also the cost of home care services was higher than that of outpatient services. For this subgroup, the ICERs were not calculated, and no sensitivity analysis was performed to determine the cost-effectiveness of the two interventions. For patients from the general medicine wards, while the outcomes were the same for the two strategies, the cost of outpatient services was lower than home care; therefore, outpatient services were a more cost-effective option (15, 16).
The results of the current systematic review showed that home care was a more cost-effective option for stroke patients based on some indicators, such as the Barthel index, MRS index, quality of life, mortality, and hospitalization as compared to hospital care. However, there were some exemptions to this conclusion. For older patients, home care and hospital care showed the same cost-effectiveness in improving the Barthel index. When the patients' outcomes were measured by the ADL scale and the Nottingham Health Profile, hospital care was generally more cost-effective for stroke patients than home care. However, the cost-effectiveness pattern was heterogeneous in the subgroups of patients with different levels of disease severity and dependence. Also, in some cases, because of not calculating the ICERs and not performing a sensitivity analysis, we could not determine whether home care or hospital care was a more cost-effective strategy.
This systematic review investigated an interesting topic among stroke patients and provided useful information about the economic evaluation of home care. However, due to the scarcity of relevant studies, the generalization of our results requires caution. Another limitation of this study is that the outcomes examined in the literature were very limited, and only some of the effects of the interventions were addressed in this review.
4.1. Conclusions
Home care is a more cost-effective option than hospital care for stroke patients, based on some indicators, such as the Barthel index, mRS index, quality of life, mortality, and hospitalization. However, there are some exemptions to this conclusion. Due to some limitations, such as heterogeneity of interventions in the existing studies, differences in patients’ disabilities, different perspectives toward economic evaluation, and differences in the health systems of different countries, further research is needed according to the context of each country and based on clinical trials.