1. Context
Health is a fundamental pillar of sustainable development (1, 2). Three of the millennium development goals specifically target health, while five additional goals are closely interconnected with health outcomes. The 2002 World Summit on Sustainable Development in Johannesburg recognized the critical role of health in achieving sustainable development (3, 4). Universal health coverage (UHC) is essential for promoting sustainable development and necessitates a robust financing system to ensure access to high-quality health services (3, 5). Sustainable financing in healthcare provides long-term funding to support the system effectively. This approach involves creating financial strategies that meet both current and future healthcare needs while minimizing instability and dependence on short-term solutions. Ultimately, this fosters a solid framework for the consistent delivery of quality healthcare (6, 7).
Sustainable health system financing refers to the ability of government to fund the healthcare system adequately while ensuring the timely allocation of resources and maintaining a surplus budget. This approach aims to achieve UHC without compromising the financial stability of other public sectors (8). The production of resources must prioritize several key factors: Ensuring sufficiency, promoting sustainability, allowing for growth potential, minimizing economic fluctuations, facilitating equitable distribution, simplifying collection processes, and gaining political acceptance (9). A sustainable health system effectively balances the obligations of providers, associated costs, and available financial resources. The World Health Organization (WHO) advocates for several strategies to achieve this balance, including improving resource collection, enhancing health services, increasing the share of the health budget relative to GDP, implementing taxes on harmful substances, and promoting partnerships within the healthcare sector (10).
Strategic purchasing is key to improving sustainable financing of health systems by maximizing the value of resources. By efficiently acquiring goods and services, health systems can reduce costs, increase efficiency, and improve the quality of care, leading to better allocation of financial resources and sustainability. Furthermore, it aligns purchasing decisions with health objectives, fosters long-term partnerships with providers, and facilitates better pricing strategies, thus contributing to a sustainable financing model (11). Purchasing health services is crucial for achieving sustainable financing in health systems. This can be accomplished through two primary approaches: Passive purchasing, where a fixed budget is allocated to cover the services provided, and strategic purchasing, which involves selecting service packages, providers, delivery methods, pricing structures, and eligible recipients to improve overall health system performance (12).
Appointing a health purchasing trustee can enhance the procurement of services, address individual health needs, improve health literacy, and strengthen governance. It is crucial to assess the effectiveness of all contracts to ensure the delivery of quality services and the appropriate selection of facilities. A 2010 report from the WHO emphasized that while adequate funding is important, maintaining high service quality is equally vital (13). Strategic procurement of health services is essential to achieving sustainable financing in a health system of country. This strategy allows financial resources to be managed more efficiently, improving service quality, reducing costs, empowering local communities, and encouraging social participation. By implementing it, countries can develop effective solutions for sustainable financing, improve public health, and reduce inequalities in access to health services (14).
Strategic purchasing makes it possible to evaluate results, adjust health programs, and move towards sustainable development by optimizing resources and improving the quality of life. It is essential for those responsible for the health system to understand these solutions, so the evidence on strategic purchasing and sustainable financing is reviewed.
2. Evidence Acquisition
This scoping review consisted of five key stages in 2024: Defining the research question, identifying relevant studies, selecting appropriate articles, organizing the collected information, and analyzing the data to present the findings. PRISMA guidelines were strictly followed. Scoping reviews provide an overview of essential concepts in a specific research domain and allow for synthesizing findings and identifying gaps in the literature. This methodology offers advantages such as a thorough assessment of the nature and scope of research activities and enhances the applicability and generalizability of findings in the relevant field (15).
2.1. Research Question
The questions guiding this study are: "What strategic purchasing solutions align with the sustainable financing of health systems?" and "Which of these strategic purchasing solutions has been most frequently cited in the literature related to sustainable health system financing?"
2.2. Search Strategy and Identifying Literature
The search strategy was developed and executed by a trained librarian with expertise in the relevant field. We conducted a comprehensive search for all related articles published in English over the past two decades, from December 21, 2002, to December 21, 2024. This search was carried out across several databases, including Google Scholar, Embase, ProQuest, Web of Science, Scopus, and PubMed, utilizing tailored search strategies and relevant keywords for each database. The specific keywords employed in this search included:
(1) Solution keywords: Solution, strategy, methods, mechanism, policy, plan, schedule, scheme, program, tactics, procedure.
(2) Buying keywords: Buying, purchasing, commissioning, procurement. "Strategic purchasing" was also included.
(3) Healthcare financing keywords: Healthcare financing.
(4) Sustain keyword: Sustain.
The researchers conducted a comprehensive literature review using a combination of database searches, citation analysis, reference checks, and a review of grey literature (e.g., theses, technical reports) to identify relevant studies. This multi-faceted approach aimed to improve the quality and comprehensiveness of their selection process.
The search terms were as follows: ("financing"[Title/Abstract]) OR ("finances"[Title/Abstract]) OR ("financial"[Title/Abstract]) OR ("funding"[Title/Abstract]) AND ("Sustainability"[Title/Abstract]) OR ("Sustain"[Title/Abstract]) OR ("Sustained"[Title/Abstract]) OR ("Sustainable"[Title/Abstract]) AND ("Health Care"[Title/Abstract]) OR ("Health Care Systems"[Title/Abstract]) OR ("Healthcare"[Title/Abstract]) OR ("Healthcare System"[Title/Abstract]) AND ("buying"[Title/Abstract] OR "purchase"[Title/Abstract] OR "commission"[Title/Abstract] OR "procure"[Title/Abstract]) AND ("Solution"[Title/Abstract]) OR ("Strategy"[Title/Abstract]) OR ("Mechanism"[Title/Abstract]) OR ("Methods"[Title/Abstract]) OR "policy"[Title/Abstract] OR ("appointments"[Title/Abstract] OR "schedules"[Title/Abstract]) OR ("tactic"[Title/Abstract] OR ("program"[Title/Abstract] OR ("scheme"[Title/Abstract] OR "plan"[Title/Abstract] OR "procedure"[Title/Abstract] OR ("Technics"[Title/Abstract])) AND ("2002/12/21"[Date] : "2024/12/21"[Date])
2.3. Study Selection
A literature review of English-language studies on sustainable health system financing through strategic purchasing was conducted. After removing duplicates, two researchers independently screened articles based on titles and abstracts, resolving disagreements through discussion or consultation with a third researcher. EndNote X5 managed the process, and a PRISMA flowchart documented the selection steps.
This study also evaluates the quality of selected articles on strategic purchasing and sustainable financing using several criteria:
(1) Credibility of sources: Priority was given to articles published in reputable, globally recognized scientific journals.
(2) Research methodology: Studies employing rigorous scientific methods were considered higher quality.
(3) Innovation and novelty: Articles addressing new challenges in the field were valued for their contribution to advancing knowledge.
(4) Practicality of solutions: The applicability of proposed solutions for improving strategic purchasing processes was a key quality indicator.
(5) Social impact: The social implications of strategic purchasing decisions on sustainable financing were analyzed as an essential measure of quality.
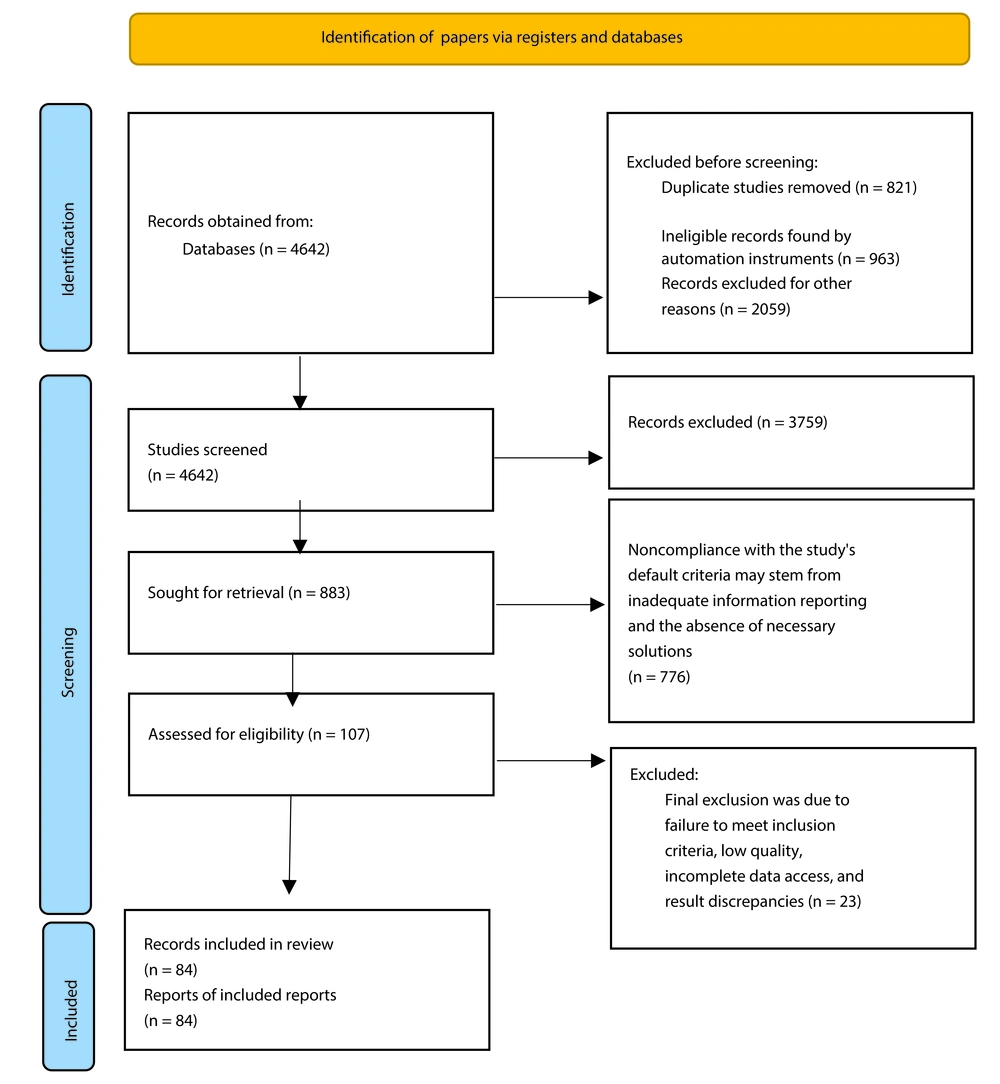
This comprehensive evaluation approach provides a deeper understanding of strategic purchasing solutions and their impact on sustainable health system financing (Figure 1).
2.4. Inclusion/Exclusion Criteria
Inclusion and exclusion criteria guided the article selection for the review, ensuring a thorough literature search by screening reference lists. We included original research, reviews, and English publications focusing on strategic purchasing models or criteria (search date: December 21, 2024). Excluded were abstracts of non-English studies, conference presentations, and newsletters.
2.5. Data Charting
A standardized form was developed to organize the information. Data collection was performed using a form designed by the researchers in Excel 2016. Two independent researchers, experienced in data extraction, carried out the process separately, resolving discrepancies with a third researcher. Influencing factors were extracted and documented in a table that included the author, year of publication, country, data collection methods, journal, purpose of the study, and key findings.
2.6. Collating and Reporting the Results
Data were summarized in a table with key characteristics of the studies and a content analysis of the main findings and themes. Two researchers independently coded the data, familiarizing themselves with the articles and extracting solutions for sustainable health system financing. Data collection followed Ritchie and Spencer’s framework analysis, which includes several stages: Familiarization with the data, identification of the thematic framework, indexing, creation of tables, data collection, and interpretation of results (16).
3. Results
We identified 4,642 articles in our search. We first removed 3,759 duplicates and eight articles without full text, leaving 107 for review. After examining these, we excluded 23 studies that did not discuss strategic purchasing for sustainable health financing (Figure 1). A comprehensive review of the remaining studies was conducted, and essential information was extracted into a standardized form.
3.1. Descriptive Characteristics of Studies
The results of this review are summarized in Appendix 1 in Supplementary File. A total of 84 articles identified strategic purchasing solutions aligned with the sustainable financing of health systems. Among these, 23 studies employed qualitative methods (26%), 16 used quantitative methods (20%), 24 utilized review methods (28%), 8 adopted mixed methods (9%), and 7 employed other methodologies (9%) for data collection. The studies conducted in 2024 were primarily qualitative and originated from various countries, including Iran in Asia, the Netherlands in Europe, Nigeria in Africa, and the United States. Appendix 1 in Supplementary File provides an overview of the general characteristics of these studies.
3.2. Extracted Solutions of Studies
The database search results were imported into EndNote X7. Two authors independently screened the titles and abstracts to identify relevant papers, which were then downloaded. During the second screening, selected articles were marked with five stars for high relevance. Solutions were manually extracted and analyzed through several steps: Reviewing studies, coding data, and using MAXQDA20 software. This involved identifying, refining, naming, and presenting themes. The strategic purchasing solutions were categorized into five themes with 39 solutions: Five for service providers, six for purchasers, fourteen for payment methods, five for packaging, and nine stewardship solutions (Table 1).
| Themes | Sub-theme (Solation) |
|---|---|
| Providers | Boosting private sector involvement in healthcare |
| Establish systems for managing public complaints, balancing ethics and profit | |
| Monitor provider performance and act | |
| Provision of services based on leveling and referral system | |
| Competition among providers based on quality | |
| Purchasers | Major insurers making strategic purchases |
| Independence, self-rule, and enhancing the power of insurance companies | |
| Service providers and suppliers must be distinct from trustees. | |
| Insurance companies should use their bargaining power when setting prices. | |
| Insurance companies should invest in the market | |
| Transparency and accountability of providers and purchasers | |
| Payment method | Revise payment methods (future and evolving payments) |
| Priority interventions categorization (high and low priorities purchase) | |
| Designing and establishing case-based (“DRG”) | |
| Performance-based payment | |
| Payment to encourage better quality | |
| Developing tariffs based on the final price | |
| Payment based on guidelines | |
| Service grading | |
| Electronic health record | |
| Protect against fraud and corruption | |
| Inductive demand control | |
| Reduced out-of-pocket payments (financial protection) | |
| Mixed payment system | |
| Pay providers regularly | |
| Package | Compilation and design of the same basic insurance package for all people |
| Focus on prevention services | |
| Designing basic package interventions based on cost-effectiveness | |
| Designing basic package interventions based on HTA | |
| Prioritizing vulnerable groups in designing services. | |
| Stewardship (government) | Developing a system to track proper use of medical guidelines and protocols |
| Creating a policy-making and legislation system for strategic purchasing | |
| Creating a unified system for managing information across all care levels | |
| Creating a transparent information system | |
| Creating a system for healthcare buyers and providers licenses and accreditation | |
| Institutionalizing customer orientation | |
| Institutionalizing evidence-based/evidence-informed decision | |
| Allocate resources equitably across areas | |
| Regulation clear minimum standards and monitoring mechanisms |
Thirty Nine Solutions Across Five Categories to Attain Strategic Procurement of Health Services Aligned with Sustainable Financing of the Healthcare System
4. Discussion
The research sought to identify strategic procurement solutions to finance sustainability in health systems. One prominent solution is collaboration between private sector entities, which can increase investment in health markets in low-income countries and improve public services. The public sector is often less efficient than the private sector, and by encouraging competition between private providers, higher-quality health services can be obtained (17). Clinical guidelines play a crucial role by providing criteria, standards, and indicators for performance evaluation and payment based on outcomes. They assist in making informed decisions and monitoring service performance and process management. Clinical audits are essential for the continuous improvement of health service delivery, with clinical guidelines being integral to this audit process (18, 19).
Informing health service recipients about providers’ skills and expertise fosters trust and acceptance, which are vital for patient recovery and overall health outcomes. This trust influences patients' adherence to medical advice, emphasizing treatment ethics over financial motives within the health system (20, 21). Health service providers are committed to maintaining, restoring, and improving community health. Accreditation and ranking processes enhance credibility and formalize standards, focusing on continuous quality improvement and safety. These evaluations encompass facilities, human resources, organizational practices, and data collection (22-24). Furthermore, effective grading of health services and a robust referral system are critical components of a successful health system. Identifying community needs, designing appropriate care pathways, and executing referrals accurately are essential for achieving strategic purchasing objectives. Without these systems in place, delivering cost-effective care becomes challenging; thus, precise service grading and an effective referral system are vital for fulfilling purchasing requirements (25, 26).
In terms of solutions related to purchasers, healthcare insurers leverage their financial resources to negotiate advantageous terms with providers. This approach enhances service quality and sustainability while simultaneously reducing costs (27). Insurers can foster a healthier and more sustainable healthcare ecosystem by prioritizing patient care and environmental responsibility. To ensure unbiased decision-making, they should separate service providers from trustee roles, eliminating conflicts of interest. Leveraging their negotiating power, insurers can secure fair pricing and promote responsible practices throughout the healthcare sector. Strategic investments in sustainable technologies will further advance these goals (28, 29).
Systematic tariff setting is vital for managing health system costs. Legal authorities set these tariffs, determining what buyers pay providers for services. Tariffs affect costs, patient satisfaction, access, and efficiency. Low tariffs may cause unnecessary services and decline in quality, while high tariffs can boost provider demand (30). Tariff setting uses either value-based or cost-based pricing. Value-based pricing prioritizes service quality. Providers are paid via budgets, salaries, incentives, performance-based payments, or bonuses (or combinations). Fixed payments (e.g., per capita rates) are consistent regardless of service volume, unlike variable payments. Trustees should utilize fixed payments (budgets, per capita rates), supplementing them with performance-based payments or bonuses (31, 32).
A universal basic insurance package ensures essential health services for all, promoting equity. It must be comprehensive, sustainable, and adaptable to health needs and financial conditions, supported by robust governance (3, 33). Focusing on preventive services can reduce long-term healthcare costs and improve health outcomes, as vaccinations decrease chronic disease rates. Cost-effective interventions maximize health benefits relative to spending (34). Implementing health technology assessment (HTA) facilitates informed decision-making and enhances funding transparency. Additionally, prioritizing vulnerable groups is crucial for addressing their specific health needs, ultimately improving community health and reducing disparities (35, 36).
Stewardship solutions create a system to ensure proper adherence to clinical guidelines. There is a global conversation about evidence-based practice in health systems. Clinical guidelines use scientific evidence to guide decisions in fields like physiotherapy, medicine, and nursing (37). These guidelines are based on research to enhance service quality, lower costs, improve community health, and meet international standards, offering criteria and indicators for performance assessment and purchasing decisions (38, 39). This framework allows for the evaluation of decisions and the monitoring of service performance and process management (40). The absence of effective stewardship undermines strategic purchasing, resulting in a less cost-effective health system. According to the WHO, there are three key components to managing health systems: (1) Establishing guidelines and protocols, (2) influencing policies and strategies, and (3) regulating behaviors. Identifying the primary individual responsible for strategic purchasing is essential. Developing health policies requires careful, long-term planning (25, 41).
Electronic health records (EHR) provide healthcare providers with access to patient histories, improving coordination, reducing errors, and enhancing care quality. Healthcare organizations need to evaluate adherence to policies to boost quality, safety, and effectiveness, which guides resource allocation and service procurement (42, 43). Customer focus is essential in strategic healthcare purchasing; understanding and addressing the needs of target groups is key to success. Customer satisfaction highlights the importance of clear communication about purchasing objectives and ensuring quality in service (44, 45).
To achieve strategic purchasing objectives that align with sustainable financing, it is necessary to establish an institutional authority that makes decisions on purchases, selects and designs payment systems for health service providers, and signs contracts with them. It is also important to maintain flexibility in the allocation of funds to cover costs associated with results, as well as to implement an adequate system to design, execute, and monitor strategic purchasing mechanisms.
4.1. Conclusions
Strategic purchasing is crucial for achieving sustainable financing in healthcare due to rising costs and needs. Policymakers and health system managers can enhance strategic purchasing by defining health service packages at various levels and ensuring free health services for vulnerable groups, such as refugees or those with rare diseases. Creating payment systems and information collection systems is essential for managing service procurement. To improve resource allocation, strategic purchasing should focus on cost-effective care, directing funds toward priority populations and creating incentives for fair and efficient use of resources. Governments need to support strategic purchasing by updating legal frameworks and assessing healthcare systems before designing purchasing schemes. Educating providers and citizens about their roles is also vital. Strategic purchasing involves deciding which services to buy, whom to buy from, how to buy, and for whom. Ministries of health can drive reforms through gradual changes and offer support.
4.2. Limitations
Our study had limitations, such as a restricted search strategy and specialized keywords. Although efforts were made to use various databases and keywords, some relevant articles may have been missed.