1. Introduction
As successors to the millennium development goals (MDGs, 1990 - 2015) (1), the sustainable development goals (SDGs, 2016 - 2030) (2) present a new opportunity to promote health in the broad context of human development (3). However, there are significant challenges in adapting the global SDG framework to a wide variety of national circumstances, considering local health priorities and the options for organizing interventions. Like most countries of the world, the Islamic Republic of Iran is committed to achieving the SDGs. This paper describes Iran’s experience and lessons learnt in making the transition from MDGs to SDGs, under the auspices of the Supreme Council of Health and Food Security and the direct management of the Ministry of Health and Medical Education [MOHME]. We summarize the progress to date, and compile statistics for the period of 1990 - 2015, which serve as benchmarks against which to judge future progress.
Iran achieved most of the health-related MDGs reaching, for example, the targets for infant mortality rate and the maternal mortality ratio long before 2015. Iran’s commitment to meeting the MDGs contributed to strengthening the national health information system by identifying, for example, the need for better monitoring of health interventions such as immunization, and the treatment of tuberculosis and HIV/AIDS. This contributed to improvements in the coverage and quality of health care, especially in remote areas of the country and for disadvantaged populations. The objective of meeting MDGs had continuous political commitment between 1990 and 2015, despite changes in government and the imposition of international sanctions on Iran. Among the factors contributing to success were: inclusion of the MDGs in national development plans, which led explicitly to the provision of funding and other resources; improvements in communication and collaboration with international development agencies; and improvements in health governance through the integrated management of health services (4).
Iran is gradually shifting from its dominant medical approach to health to a social approach to health by paying greater attention to the underlying social, economic and environmental determinants of health- the three pillars of sustainable development. This transition began in the era of the MDGs, and the SDGs present a new opportunity to further that cause (5). In addition, the SDGs explicitly include targets and indicators for the control of non-communicable diseases and injuries (NCDS) -the dominant cause of illness and death in Iran today- which were missing from the MDGs.
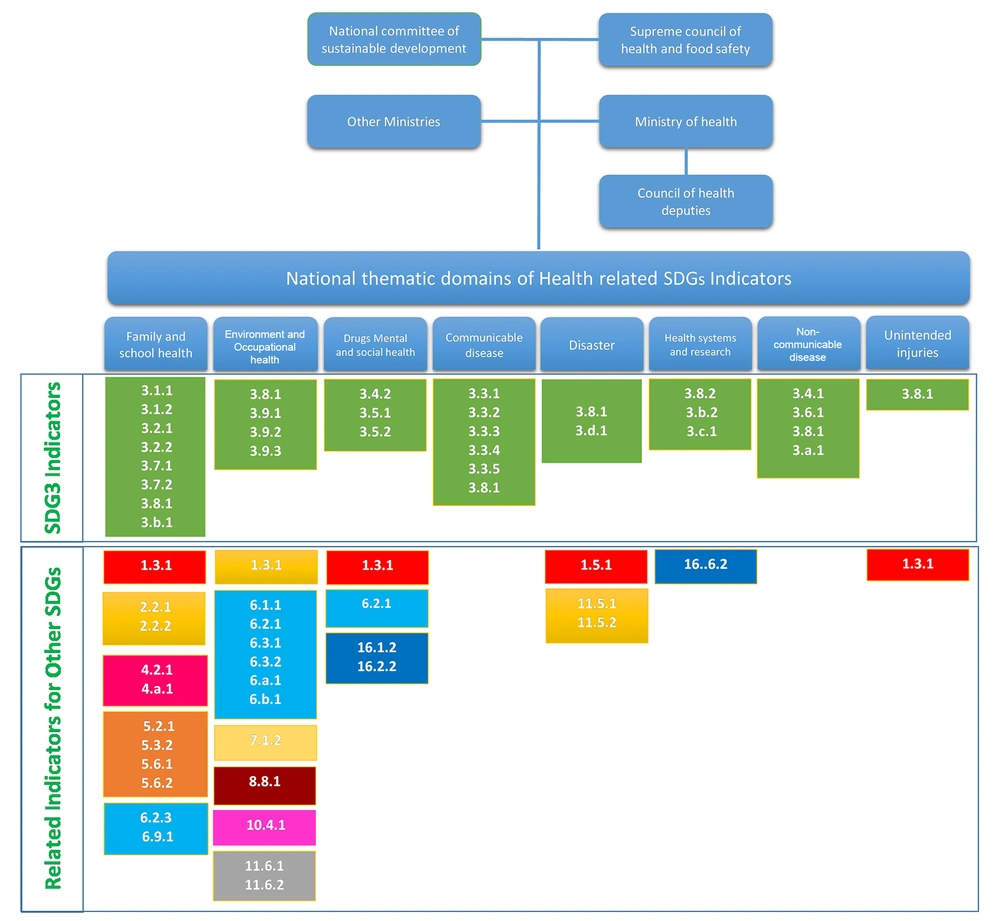
In Iran, multisectoral policy-making is led by the Supreme Council of Health and Food Security, chaired by the President of the country (Figure 1). Within the MOHME, the Department of Social Affairs is headed by a Deputy Minister, which among other multisectoral activities oversees the monitoring of progress, including health and equity. The Department also organizes a national festival of social responsibility and accountability for health with the participation of non-governmental organizations (NGOs) and civil society.
Iran’s commitment in 2012 to the Rio+ 20 declaration and its “21 agenda” (6), a precursor to the SDGs, led to the establishment of a National Committee for Sustainable Development (NCSD) that was chaired by a Deputy President and comprised high-level managers from more than 10 ministries and two national bodies, the National Organization of Environment and the National Organization of Planning and Budget (7). Following the launch of the SDGs, the NSCD was designated as the body responsible for preparing the United Nations Voluntary National Reports [VNR] to document progress on SDGs. In addition, the MOHME was given responsibility for overseeing progress towards SDG3, and also was appointed as a partner for SDG1 (poverty), SDG2 (hunger), and SDG6 (water and sanitation).
Between 2015 and 2018 the MOHME has ensured that health was placed in the 6th National Development Plan, established a department of SDGs and health along with a national steering committee for health, raised awareness about health-related SDGs within government and across the country, and carried out a benchmarking and trend analysis of health-related SDGs (8).
2. Methods
To benchmark health in the SDGs, a mapping exercise was conducted to identify all health-related targets and indicators of SDG3 and other SDGs, guided by WHO reports (1, 9, 10) and extensive consultation, for example with all concerned departments of the MOHME and with the Council of Health Deputy Directors of the ministry. The final list included 34 targets and 56 indicators running across 12 of the 17 SDGs. Of these, 21 targets and 29 indicators were derived from goals other than SDG3 (Table 1)
| Goal/Health Related SDG Indicators | 1990 | 1995 | 2000 | 2005 | 2010 | 2015 | Source |
|---|---|---|---|---|---|---|---|
| SDG 3 | |||||||
| 3.1.1: Maternal mortality ratio (maternal deaths among women aged 15 - 49 years per 100,000 live births) | 123 | 80 | 51 | 34 | 27 | 25 | UN-2017 (6) |
| 3.1.2: Proportion of births attended by skilled health personnel (doctors, nurses, midwives, or country-specific medical staff [e.g., clinical officers]) | 89/6 | 97/3 | 98/1 | 99 | Iran MDG report, 2014 (4) | ||
| 3.2.1: Under-5 mortality rate (probability of dying before the age of 5 years per 1,000 live births) | 57.5 | 45.3 | 34/7 | 25/7 | 19/2 | 15/5 | WHO, 2019 (9) for years 1990, 1995 and UN, 2017 (6) for years 2000 and later |
| 3.2.2: Neonatal mortality rate | 26/5 | 22/6 | 19/2 | 15/3 | 11/7 | 9/5 | UNSDSN, 2017 (11) |
| 3.6.1: Death rate due to road traffic injuries | 33/5 | 40/8 | 33/9 | UNSDSN, 2017 (11) | |||
| 3.7.1: Proportion of women of reproductive age (aged15 - 49 years) who have their need for family planning satisfied with modern methods | 92/50 | 94/10 | 94/30 | 92.1 (EMRO 2016) | Iran MDG Report, 2014 (4) | ||
| 3.7.2: Adolescent birth rate (aged 10 - 14 years; aged15 - 19 years) per 1,000 women in that age group | 34/70 | 32/60 | 33.7 (2011) | 33.68 (2013) | UNSDSN, 2017 (11) | ||
| 3.a.1 Age-standardized prevalence of current tobacco use among persons aged 15 years and older | |||||||
| • Prevalence of smoking any tobacco product among persons aged > 18 male | 30/2 | 26/8 | 23/8 | 21/5 | WHO, 2016 (11, 12) | ||
| • Prevalence of smoking any tobacco product among persons aged > 18 female | 5/8 | 2/9 | 1/5 | 0/7 | WHO, 2016 (12) | ||
| Health-related indicators for other SDGs | |||||||
| 2.2.1: Prevalence of stunting (height for age < -2 standard deviation from the median of the World Health Organization (WHO) Child Growth Standards) among children under 5 years of age | 27/5 | 22/9 | 14/1 | 7/9 | 6/9 | 6/8 | WHO/EMRO, 2015 (11, 13) |
| 2.2.2: Prevalence of malnutrition (weight for height > +2 or < -2 standard deviation from the median of the WHO Child Growth Standards) among children under 5 years of age, by type (wasting and overweight) Maternal mortality ratio | |||||||
| Proportion of wasted children (weight for height below minus two standard deviations from the median) under the age of 5 years | 8/9 | 7/8 | 5/4 | 4/4 | 4/4 | 4/4 | UNICEF-WHO-The World Bank-2016 (11, 14) |
| 6.1.1: Proportion of population using safely managed drinking water services | |||||||
| Proportion of population using improved drinking water sources (Total) | 89/60 | 97/88 | 98.13 (2014) | Iran MDG Report, 2014 (4) | |||
| 6.2.1: Proportion of population using safely managed sanitation services, including a hand-washing facility with soap and water | |||||||
| Proportion of population using improved sanitation facilities | 64/30 | 92/51 | Iran MDG Report, 2014 (4) |
The ensuing task was to map these indicators on to Iran’s existing monitoring and evaluation framework in the national health information system, so as to ensure efficient planning and implementation (15). The MOHME categorized the indicators into 8 “thematic domains”, and each domain was assigned to one department within MOHME (Figure 1). This arrangement for monitoring and evaluation has clarified responsibility and ownership by each department allowing better integration into the current structure and function of MOHME and has reduced the burden of data collection.
3. Results and Discussions
The benchmarking exercise presented a series of lessons for tracking progress towards the SDGs. First, some governmental departments were concerned about possible unforeseen consequences of providing access to official data through international publications. Given the sensitivity around certain kinds of data such as suicide, HIV/AIDS, alcohol use, some indicators may in future be monitored but with results reported only within government departments. Second, the expanded set of SDG indicators requires some data from outside the ministry of health, for example those related to drug abuse or water quality, which has meant establishing new collaborations among ministries and with NGOs. Third, some SDG indicators are new to Iran’s health information system, such as those related to early child development, and therefore require new sources of data. Where data are not yet available, we used existing national indicators that were closest to those required by the SDG framework (Table 1). Fourth, some SDG indicators were imprecisely defined (with little clarification given by metadata) such as the indicator related to social protection (1.3.1). Finally, some national data were inconsistent with international estimates. In general, we have preferred to use national data, and only when these were unavailable or inaccessible did we use information from secondary sources such as the WHO and other UN agencies. All in all, some data were not yet available at all for the benchmarking exercise: 3 indicators from SDG3 and 13 indicators from other SDGs (Table 1).
Taking these limitations into account, the data so far assembled for the period of 1990 - 2015, show that significant improvements have been made in health status in terms of decreased MMR, IMR, U5MR as shown in Table 1. Iran has made progress towards the achievement of universal health coverage as reflected for example in increase of reproductive health services, and reduction of stunning. Iran is also on course to achieve several targets within SDG3 well before 2030, and for some has already achieved the target for 2030 such as MMR which is below 70 per 100000 live births, NMR which is below 12 per 1000 live births, and U5MR which is also less than 25 per 1000 live births, safe delivery at birth, and tuberculosis. The main exceptions to progress, seen in national averages, are for unmet family planning needs, HIV incidence and road traffic accidents. Behind the national averages, some indicators reveal a lack of progress within socially and economically disadvantaged provinces as in Sistan-Balochestan (16). There are likely to be more such examples, but not all data are presently in a (disaggregated) form that allows the measurement of inequalities that have consequences for health.
In conclusion, the graduation from MDGs to SDGs has helped Iran to focus on the top priorities for health (especially non-communicable diseases and injuries), and to implement programs that have adopted a socio-economic and environmental approach to health. There are clearly challenges in organization, implementation and evaluation, some of which are made evident by the benchmarking exercise described here. There is, however, strong political and social commitment to achieving the SDGs in Iran, from the Supreme Council of Health and Food Security to civil society. This study recommends following the key recommended framework of actions for policy makers in this filed in Iran: (1) Equity, shared responsibility and evidence-informed and oriented approach; (2) Strengthening, integrating and linking information systems across sectors; (3) Aligning, adjusting and integration of SDGs; (4) Strengthening stakeholder partnership and participation and effective multisectoral collaboration; (5) Awareness raising, advocacy and capacity building.