1. Background
Patients with acute anterior ST-segment elevation myocardial infarction (STEMI) usually develop more in-hospital mortality and complications than non-anterior myocardial infarction, mainly due to larger infarct size and more jeopardized myocardium (1, 2).
The left anterior descending artery (LAD) is the most common culprit vessel in anterior STEMI, and its acute occlusion leads to significant impairment of cardiac function and an unfavorable clinical outcome. This artery's two main branches are the diagonal and septal branches. The diagonal branches supply blood to the lateral parts of the left ventricle and maybe one or more. Previous studies have shown that the diagonal and septal branches may grow and increase in size and diameter in chronic LAD arterial occlusion.
On the other hand, previous studies have shown that the left ventricle wall motion score index (WMSI) is a reliable measure of reperfusion success in patients with acute STEMI (3-5) and could predict the short and long-term prognosis of these patients (6, 7). Also, as a surrogate of infarct size, WMSI could be used for myocardial remodeling assessment even better than left ventricular ejection fraction (LVEF) (4).
There are few studies about the impact of diagonal branch blood flow on these echocardiographic measures in patients with first acute anterior myocardial infarction undergoing primary angioplasty (8, 9).
2. Objectives
So, in the present study, we aimed to compare WMSI and LVEF in patients with first acute anterior STEMI treated with primary angioplasty based on diagonal branch blood flow after the procedure.
3. Methods
This prospective, single-center study enrolled patients with acute anterior STEMI treated with primary angioplasty on the LAD as a culprit vessel at Madani Heart Center in Tabriz in northwest Iran between October 2020 and March 2021.
Acute anterior STEMI was defined as persistent chest pain with ST-segment elevation in ≥ 2 precordial leads (≥ 0.2 mV in leads V2 and V3 and ≥ 0.1 mV in other leads).
We excluded patients with previous revascularization, unsuitable anatomy for coronary angioplasty, acute stent thrombosis, failed thrombolysis, cardiogenic shock, presentation after 12 hours, and poor echocardiographic image quality.
The ethics committee of the Tabriz University of Medical Sciences reviewed and approved the study protocol (ID: IR.TBZMED.REC.1400.592). The study was performed in compliance with the Declaration of Helsinki, and informed consent was obtained from all patients.
The largest branch of the diagonal branches was considered the main diagonal, and post-procedural thrombolysis in myocardial infarction (TIMI) flow in this branch was determined in all patients. Then, patients were divided into two groups: patients with final TIMI flow grade 3 in diagonal (sufficient diagonal flow) and patients with final TIMI flow less than grade 3 in diagonal (insufficient diagonal flow).
The study endpoints were the Wall-Motion Score Index (WMSI) and LVEF. We compared these two indexes in patients with versus without sufficient final diagonal coronary flow.
Patients underwent detailed echocardiography using a GE Vivid 7 Dimension Ultrasound System with the assessment of LVEF and WMSI on the third day after primary percutaneous coronary intervention (PPCI).
Left ventricular ejection fraction was calculated using Simpson's biplane disk methodic apical four- and four-chamber view. For calculation of Left Ventricular Wall Motion Score Index (LVWMSI), wall motion was assessed in 16 left ventricle myocardial segments as 1 - 4, where one is normal, and 2 - 4 represents hypokinetic, akinetic, and dyskinetic or aneurysmal. Left ventricular wall motion score index was then derived as the sum of all segment scores divided by the number of segments visualized.
The echocardiologists performing and interpreting the echocardiographic examination were blinded to the angiographic findings of the two groups.
All patients were given aspirin (100 mg) and clopidogrel (600 mg) on admission to the emergency room. A 100 IU/kg bolus of intravenous heparin was administered before the procedure. Primary PCI was performed using standard techniques via the femoral or radial artery. Thrombectomy devices and eptifibatide use were dependent on the operators.
3.1. Statistical Analysis
The data were expressed as mean ± standard deviation for quantitative variables and as frequency and percentage for qualitative variables. Continuous variables were compared using the student's t-test or Mann-Whitney U test. Categorical variables were compared using the chi-square test (or Fisher's exact test).
Statistical significance was set at a level of 0.05. All analyses were performed with SPSS version 25 software (IBM SPSS Statistics, USA).
4. Results
A total of 107 patients with first acute anterior STEMI were included in this study, of which 13 patients (12.1%) had insufficient diagonal flow after primary coronary angioplasty. The mean age of patients was 58.78 ± 12.28 years, and 84.1% were male.
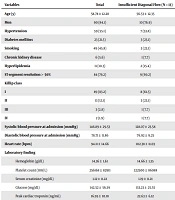
The clinical characteristics of the patients are shown in Table 1. Patients with insufficient diagonal flow had lower systolic blood pressure (128.07 ± 23.58 mm Hg vs. 149.5 ± 29.43 mmHg, P value = 0.014) and higher heart rate (102.38 ± 11.03 BPM vs. 92.94 ± 14.78 BPM, P = 0.029) than patients with the sufficient diagonal flow.
| Variables | Total | Insufficient Diagonal Flow (N = 13) | Sufficient Diagonal Flow (N = 94) | P-Value |
|---|---|---|---|---|
| Age (y) | 58.78 ± 12.28 | 56.53 ± 12.35 | 59.09 ± 12.31 | 0.48 |
| Men | 90 (84.1) | 10 (76.9) | 80 (85.1) | 0.43 |
| Hypertension | 59 (55.1) | 7 (53.8) | 52 (55.3) | 0.92 |
| Diabetes mellitus | 23 (21.5) | 3 (23.1) | 20 (21.3) | 0.56 |
| Smoking | 49 (45.8) | 3 (23.1) | 46 (48.9) | 0.07 |
| Chronic kidney disease | 6 (5.6) | 1 (7.7) | 5 (5.3) | 0.54 |
| Hyperlipidemia | 11 (10.3) | 2 (15.4) | 9 (9.6) | 0.39 |
| ST-segment resolution > 50% | 84 (79.2) | 9 (69.2) | 75 (80.6) | 0.34 |
| Killip class | 0.10 | |||
| I | 89 (83.2) | 8 (61.5) | 81 (86.2) | |
| II | 13 (12.1) | 3 (23.1) | 10 (10.6) | |
| III | 3 (2.8) | 1 (7.7) | 2 (2.1) | |
| IV | 2 (1.9) | 1 (7.7) | 1 (1.1) | |
| Systolic blood pressure at admission (mmHg) | 146.89 ± 29.53 | 128.07 ± 23.58 | 149.5 ± 29.43 | 0.01 b |
| Diastolic blood pressure at admission (mmHg) | 78.71 ± 11.86 | 76.92 ± 9.25 | 78.94 ± 12.21 | 0.56 |
| Heart rate (bpm) | 94.11 ± 14.66 | 102.38 ± 11.03 | 92.94 ± 14.78 | 0.02 b |
| Laboratory finding | ||||
| Hemoglobin (g/dL) | 14.36 ± 1.61 | 14.66 ± 1.35 | 14.31 ± 1.65 | 0.47 |
| Platelet count (109/ L) | 256168 ± 82911 | 322500 ± 86988 | 246896 ± 78422 | 0.002 b |
| Serum creatinine (mg/dL) | 1.12 ± 0.22 | 1.19 ± 0.21 | 1.11 ± 0.22 | 0.20 |
| Glucose (mg/dL) | 142.52 ± 56.39 | 133.23 ± 25.55 | 143.81 ± 59.38 | 0.52 |
| Peak cardiac troponin (ng/mL) | 16.95 ± 10.18 | 22.63 ± 6.12 | 16.16 ± 10.41 | 0.03 b |
| Medications post-procedure | ||||
| ASA | 107 (100) | 13 (100) | 94 (100) | - |
| Clopidogrel | 107 (100) | 13 (100) | 94 (100) | - |
| Beta blocker | 64 (40.2) | 5 (38.5) | 59 (62.8) | 0.094 |
| Statin | 107 (100) | 13 (100) | 94 (100) | - |
| ACE or ARB | 107 (100) | 13 (100) | 94 (100) | - |
| Diuretic | 50 (46.27) | 9 (69.2) | 41 (43.6) | 0.083 |
Abbreviations: ACEI, angiotensin-converting enzyme inhibitor; ARB, angiotensin receptor blocker; bpm, beat per minute.
a Values are expressed as mean ± SD or No. (%).
b Statistical significance was set at a level of 0.05.
The patients with insufficient diagonal flow after the procedure had higher peak troponin levels than the other group. (22.63 ± 6.12 ng/mL vs. 16.16 ± 10.41 ng/mL, P = 0.031). All patients received aspirin, clopidogrel, statin, and ACE or ARB. Beta-blockers were prescribed to 40.2% of patients, and diuretics to 46.27%.
Angiographic findings of patients are shown in Table 2. The proximal LAD involvement was more seen in patients with the insufficient diagonal flow (69.2% vs. 35.1%, P = 0.018). The mean final diagonal TIMI flow was 2.49 ± 0.49 in the insufficient group and 3 ± 0 in the sufficient group (P < 0.001).
| Variables | Total | Insufficient Diagonal Flow (N = 13) | Sufficient Diagonal Flow (N = 94) | P-Value |
|---|---|---|---|---|
| Vessel number | 0.252 | |||
| 1VD | 56 (52.3) | 9 (69.2) | 47 (50) | |
| 2VD | 28 (26.2) | 1 (7.7) | 27 (28.7) | |
| 3VD | 23 (21.5) | 3 (23.1) | 20 (21.3) | |
| Proximal LAD occlusion | 42 (39.3) | 9 (69.2) | 33 (35.1) | 0.018 b |
| Mid LAD occlusion | 65 (60.7) | 4 (30.8) | 61 (64.9) | |
| Door-to-balloon time, minutes | 43.87 ± 17.94 | 41.38 ± 19.13 | 44.22 ± 17.84 | 0.595 |
| Total ischemic time, minutes | 177.03 ± 105.61 | 164.53 ± 59.71 | 178.76 ± 110.58 | 0.651 |
| Contrast volume, milliliter | 210.61 ± 75.76 | 226.92 ± 91.77 | 208.3 ± 73.54 | 0.410 |
| Thrombosuction | 2 (1.9) | 0 | 2 (2.1) | 0.771 |
| Eptifibatide | 89 (83.2) | 13 (100) | 76 (80.9) | 0.078 |
| Low thrombus burden | 18 (16.9) | 1 (7.7) | 17 (18.1) | 0.69 |
| High thrombus burden | 89 (83.1) | 12 (92.3) | 77 (81.9) | |
| Stent length (millimeter) | 22.52 ± 6.61 | 21.92 ± 6.57 | 22.61 ± 6.64 | 0.728 |
| Stent diameter (millimeter) | 3.21 ± 0.39 | 3.42 ± 0.53 | 3.17 ± 1.36 | 0.029 b |
| Initial LAD TIMI 0, 1 | 85 (79.4) | 13 (100) | 72 (76.5) | 0.06 |
| Final LAD TIMI < 3 | 22 (20.5) | 13 (100) | 8 (8.5) | < 0.0001 b |
| Initial diagonal TIMI 0, 1 | 48 (44.8) | 13 (100) | 35 (37.2) | < 0.0001 b |
Abbreviations: LAD, left anterior descending artery; TIMI, thrombolysis in myocardial infarction.
aValues are expressed as mean ± SD or No. (%).
b Statistical significance was set at a level of 0.05.
Regarding echocardiographic findings, LVEF was lower in patients with the insufficient diagonal flow (32.92 ± 7.29% vs. 39 ± 8.68%, P = 0.018). Also, this group had larger left ventricular end-systolic volume (LVESV) (57.84 ± 16.65 mL vs. 49.12 ± 19.83 mL, P = 0.042) and higher LVWMSI (1.68 ± 0.28 vs. 1.49 ± 0.26, P = 0.029) (Table 3).
No patients died during the in-hospital course. Heart failure was the most common adverse event, which occurred in 35.5% of patients. In-hospital outcomes were not different between patients with or without sufficient diagonal flow.
| Variables | Total | Insufficient Diagonal Flow (N = 13) | Sufficient Diagonal Flow (N = 94) | P-Value |
|---|---|---|---|---|
| BSA (m2) | 1.85 ± 0.18 | 1.82 ± 0.12 | 1.86 ± 0.19 | 0.488 |
| LVEDD (mm) | 4.68 ± 0.49 | 4.72 ± 0.51 | 4.67 ± 0.49 | 0.754 |
| LVESV(mL) | 79.88 ± 20.75 | 85.53 ± 17.58 | 79.10 ± 21.11 | 0.155 |
| LVEF (%) | 38.26 ± 8.73 | 32.92 ± 7.29 | 39 ± 8.68 | 0.018 a |
| LAV (mL) | 51.53 ± 15.41 | 57.34 ± 22.98 | 50.73 ± 14.02 | 0.310 |
| LVESD, (mm) | 3.25 ± 0.62 | 3.42 ± 0.67 | 3.23 ± 0.61 | 0.448 |
| LVEDV,(mL) | 50.18 ± 19.61 | 57.84 ± 16.65 | 49.12 ± 19.83 | 0.042 a |
| FS (%) | 30.18 ± 8.53 | 27.61 ± 7.45 | 30.54 ± 8.65 | 0.249 |
| LAVI (mL/m2) | 27.99 ± 8.67 | 31.91 ± 13.83 | 27.45 ± 7.65 | 0.254 |
| LVWMSI | 1.51 ± 0.27 | 1.68 ± 0.28 | 1.49 ± 0.26 | 0.029 a |
Abbreviations: BSA, body surface area; FS, fractional shortening; LAV, left atrial volume; LAVI, left atrial volume index; LVEDD, left ventricular end-diastolic dimension; LVEDV, left ventricular end-diastolic volume; LVEF, left ventricular ejection fraction; LVESD, left ventricular end-systolic dimension; LVESV, left ventricular end-systolic volume; LVWMSI, Left Ventricular Wall-Motion Score Index.
a Statistical significance was set at a level of 0.05.
5. Discussion
The main findings of the present study were:
- Insufficient diagonal branch flow was not uncommon after primary angioplasty of the LAD and was found in more than 10% of cases.
- This finding was associated with poor clinical and hemodynamic status during the presentation, as evidenced by lower BP and more tachycardia.
- These patients had higher troponin levels than patients with sufficient diagonal flow.
- These patients had worse left ventricular systolic function, as evidenced by larger LVESV, lower LVEF, and higher Regional Wall Motion Score Index (RWMSI).
- These patients often had proximal occlusion of the LAD.
The prognostic impact of the diagonal branch flow in patients undergoing PPCI of LAD for acute anterior STEMI has been investigated in a few studies in recent years. Most of these studies have considered clinical events as the study endpoint, and only a few studies have evaluated the impact of the diagonal branch flow after primary angioplasty on echocardiographic findings in patients with acute anterior STEMI. In 2018, Yamamoto et al. investigated the prognostic impact of insufficient diagonal flow after primary angioplasty for acute anterior STEMI in 229 patients, more than 25% of whom had insufficient diagonal flow (8).
Their study found no statistically significant differences between patients with or without sufficient diagonal flow regarding in-hospital mortality and mechanical complications. However, in the group with insufficient diagonal flow, in-hospital mortality was higher. In the Yamamoto et al.'s study (8), as in our study, left ventricular systolic function was lower in the group with insufficient diagonal flow, and they had worse RWMSI. In the present study, in-hospital adverse events were similar between patients with or without sufficient diagonal flow. There was no in-hospital death in the present study, probably because of the small sample size. On the other hand, in the present study, LVESV after primary angioplasty was larger in the group with the inadequate diagonal flow, which may indicate greater left ventricular remodeling in this group. Numerous studies in patients with acute myocardial infarction and chronic coronary artery disease have shown that LVESV is one of the most important prognostic echocardiographic factors for short-term as well as long-term survival and adverse events (10-12).
Another study by Zhang et al. revealed that in patients with acute anterior STEMI, the absence of flow in the diagonal branch before primary angioplasty was associated with increased mortality at 18 months and worsening left ventricular systolic function (9). Indeed, all studies by Yamamoto et al. (8), Zhang et al. (9), and the present study demonstrate that the establishment of diagonal flow during primary angioplasty of the LAD plays an important role in improving left ventricular systolic function, although all three studies differ in methodology and sample size.
However, the present study may be one of the first to address increased LVESV (as a predictor of LV remodeling) in patients with insufficient diagonal branch flow after primary angioplasty in patients with LAD occlusion. This factor could potentially affect the prognosis of patients with acute anterior STEMI undergoing mechanical reperfusion, which may require longer follow-up with more cases.
In the present study, troponin levels, which roughly correlate with infarct size, were significantly higher in the group with the insufficient diagonal flow. This could explain the lower left ventricular function, higher RWMSI, and higher end-systolic volume. In other words, based on the results of the present study and previous studies, the absence of adequate diagonal flow after primary angioplasty may be considered a sign of failure of revascularization in acute anterior wall myocardial infarction. It seems that these patients should receive aggressive anti-ischemic and anti-remodeling treatments and more secondary preventive measures.
This study has several limitations: The first and most important limitation is that most patients with insufficient diagonal flow had proximal LAD occlusion, and worth echocardiographic findings like larger LVESV, lower LVEF, and higher RWMSI might be due to the site of myocardial infarction rather than diagonal branch flow which needs further powered studies.
The others were the small sample size and the lack of long-term follow-up. Also, this study was single-center and non-randomized, and clinical adverse events were relatively infrequent, so the impact of post-PPCI diagonal flow on these events could not be accurately addressed.
Large prospective multicenter randomized clinical trials are required to confirm or preclude our findings in the present study.
5.1. Conclusions
The present study showed that in patients with acute anterior STEMI undergoing primary angioplasty, insufficient diagonal branch flow after the procedure was associated with greater enzymatic infarct size, worse left ventricular systolic function, and larger left ventricular end-systolic volume.