1. Background
Cardiovascular diseases (CVDs) are the primary cause of global mortality, resulting in approximately 17.9 million deaths annually (1). Heart attacks and strokes account for over 80% of CVD-related fatalities, particularly impacting individuals under 70 years of age (2). In Iran, CVDs lead to one million Disability-Adjusted Life Years (DALYs), representing 46% of all deaths and 20%-23% of the disease burden. The estimated increase in DALYs related to CVDs among Iranians aged ≥ 30 years by 2025 emphasizes the urgent need for effective interventions (3, 4).
Patients with prior CVDs have a significantly increased risk of experiencing recurrent CVD events or mortality (5). Myocardial infarction (MI) survivors have a four to five times higher risk of another MI compared to similar-age individuals without coronary artery disease (CAD) (6). The re-admission rate of CVD patients is notable, leading to increased in-hospital mortality and healthcare costs (7, 8). Furthermore, factors like age, smoking, hypertension, and diabetes are considered independent predictors of recurrent CVDs and mortality (5). Anxiety and depression are common after acute cardiac events, with about 20% of patients diagnosed with depression and up to 30% experiencing severe anxiety (9). Both conditions increase the risk of complications and adverse outcomes (10). Therefore, a comprehensive approach prioritizing both immediate recovery and long-term prevention is required (11).
Cardiac rehabilitation (CR) is a highly effective secondary prevention strategy for individuals who have experienced a CVD event (12). It includes exercise training, encouragement of physical activity, education on health, management of cardiovascular risk factors, and psychological support (13). Research shows that CR can decrease mortality by up to 26% and recurrent CVD events by 47%, while also enhancing functional status and quality of life (12). However, globally, only 20-30% of patients engage in CR annually. Factors such as gender, socioeconomic status, and patient characteristics — including comorbidities, depressive symptoms, and smoking — significantly affect participation in CR (14).
This study aims to identify and describe the factors affecting cardiac patients who participate in our CR center, the only one in Guilan Province.
2. Objectives
The objective of this study was to explore the demographic and social determinants that influence participation in CR programs.
3. Methods
3.1. Design and Settings
This cross-sectional study involved 250 cardiovascular patients who were referred to the same CR center in the private sector, the Noor Heart Clinic, located in Rasht, Iran, over the course of one year. Informed consent was obtained from all participants involved in the study. Participants were fully informed about the purpose of the research, their rights, and the voluntary nature of their participation. The consecutive sampling method was based on patients' gradual visits to our center, continuing until the required sample size was reached.
The inclusion criteria for participants consisted of cardiac patients who were referred to the CR center by a cardiologist for specific conditions such as stable angina, history of coronary angioplasty, history of coronary artery bypass surgery, heart valve surgery, heart failure, or heart transplant, and who were willing to participate in the study. The exclusion criterion was the incompleteness of the required information and refusal to participate.
3.2. Data Collection
Basic demographic information was collected for each participant, including age, gender (male or female), education level (undergraduate, diploma, or university), place of residence (urban or rural), smoking status (never smoked, currently smoking, quit for less than three months, or quit for more than three months), and whether they had supplementary insurance. The patient's weight and height were assessed using a digital scale and a height meter, individually. Measurements were taken without shoes and with the patient wearing light clothing.
Medications collected included those for diabetes and hypertension. Patients prescribed antidiabetic medications or informed by their doctor that they had diabetes were classified as diabetic. Hypertension was defined as having a systolic blood pressure (BP) of 140 mmHg or higher, a diastolic pressure of 90 mmHg or higher, or the use of any antihypertensive medication. The patient's BP was evaluated bilaterally using a mercury BP device following 10 minutes of rest. The higher value obtained from the measurements was recorded as the patient's BP. Blood pressure control in this study was guided by the European Society of Cardiology (ESC) guidelines, which recommend a target BP of less than 140/90 mmHg for all patients (15). Having a cardiac familial history was defined as heart-related conditions in first-degree relatives, before age 55 for men and 65 for women.
Information about psychological factors was collected from patients using the Hospital Anxiety and Depression Scale (HADS) Questionnaire, administered during the first rehabilitation session for all clients. To ensure accuracy, patients and their companions received detailed instructions on completing the questionnaire. Patients were advised to answer in a relaxed state and submit the completed forms to the rehabilitation nurse at the next session. The HADS was initially developed by Zigmond and Snaith (16) as a screening tool for identifying psychiatric disorders in outpatient clinics and general hospitals. This self-report instrument consists of 14 items and is designed to assess the presence and severity of depression and anxiety symptoms experienced by patients over the past week. Scores on the depression and anxiety subscales of the HADS questionnaire range from 0 to 21. Within both subscales, scores ranging from 0 to 7 are considered normal, scores between 8 and 10 indicate mild symptoms, scores between 11 and 14 suggest moderate symptoms, and scores between 15 and 21 indicate severe symptoms.
To understand why some patients are not participating in the CR program, follow-up phone calls were conducted, and patients were spoken to during their visits to inquire about their reasons for non-participation. The data were then analyzed using descriptive statistics to calculate the frequencies and percentages for each reason, both overall and by gender.
3.3. Ethical Consideration
This study was approved by the Ethics Committee of Guilan University of Medical Sciences in Iran (approval number: IR.GUMS.REC.1400.193).
3.4. Statically Analysis
Descriptive findings were presented using means and standard deviations for quantitative data, and frequencies and percentages for qualitative data. The Shapiro-Wilk test was utilized to assess the normality of the data distribution. When normal distribution conditions were satisfied, the chi-square test was employed to evaluate the association between two qualitative variables, while the t-test was used to analyze the relationship between a quantitative variable and a binary qualitative variable. All statistical analyses were performed using SPSS version 21, with a significance level set at P < 0.05.
4. Results
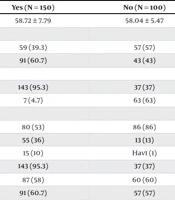
The study involved 250 participants, with 60% participating in a CR program. As shown in Table 1, the results indicate that the average age of participants and non-participants did not show a statistically significant difference (P = 0.5). Among the participants, 60% were men, while 57% of the non-participants were women. Furthermore, over 95% of the CR program participants resided in urban areas, while more than 63% of non-participants lived in rural areas.
| Participation in CR Program | Yes (N = 150) | No (N = 100) | P-Value |
|---|---|---|---|
| Age | 58.72 ± 7.79 | 58.04 ± 5.47 | 0.5 |
| Gender | 0.004 | ||
| Women | 59 (39.3) | 57 (57) | |
| Men | 91 (60.7) | 43 (43) | |
| Location | 0.001 | ||
| Urban areas | 143 (95.3) | 37 (37) | |
| Rural areas | 7 (4.7) | 63 (63) | |
| Education | 0.001 | ||
| High school | 80 (53) | 86 (86) | |
| High school diploma | 55 (36) | 13 (13) | |
| University | 15 (10) | Hav1 (1) | |
| Using additional insurance | 143 (95.3) | 37 (37) | 0.001 |
| Diabetes | 87 (58) | 60 (60) | 0.7 |
| BP | 91 (60.7) | 57 (57) | 0.5 |
| Cigarettes | 0.1 | ||
| No | 99 (66) | 79 (79) | |
| Yes | 33 (22) | 7 (7) | |
| Quitting less than three months | 8 (5.3) | 4 (4) | |
| Quitting more than three months | 10 (6.7) | 10 (10) | |
| Having a family history | 83 (55.3) | 61 (61) | 0.3 c |
| BMI | 0.1 | ||
| < 18.5 | 10 (6.6) | 11 (11) | |
| 18.5 - 24.99 | 20 (13.3) | 10 (10) | |
| 25 - 30 | 62 (41.3) | 49 (49) | |
| > 30 | 58 (38.6) | 30 (30) |
Abbreviation: CR, cardiac rehabilitation; BP, blood pressure.
a Values are expressed as mean ± SD or No. (%).
b This table summarizes demographic and health-related factors comparing between participants and non-participants.
c P-values indicate statistical significance for differences between groups.
There was a statistically significant difference in the frequency of participants and non-participants in the CR program in terms of education, with over 86% of the non-participants not having a high school degree, while nearly 53% of the participants had a diploma. Additionally, the data revealed that over 95% of CR program participants had supplementary insurance, whereas over 67% of non-participants did not have supplementary insurance, with this disparity proving to be statistically significant (P = 0.001).
The study did not find any significant differences in the frequency of cardiac risk factors such as diabetes, BP, smoking, overweight, and obesity between the two groups (P > 0.05).
As indicated in Table 2, over 34% of the participants reported experiencing moderate to severe anxiety, while more than 37% reported experiencing moderate to severe depression. The study found no statistically significant difference in the prevalence of various degrees of depression and anxiety between men and women (P > 0.05).
| Psychological Factors | Men (n = 91) | Women (n = 59) | Total (n = 150) | P-Value |
|---|---|---|---|---|
| Anxiety | 0.6 | |||
| Normal | 34 (37.4) | 19 (32.2) | 53 (35.3) | |
| Mild | 44 (31.9) | 21 (27.1) | 45 (30) | |
| Moderate | 6 (23.1) | 10 (25.4) | 36 (24) | |
| Severe | 7 (7.7) | 9 (15.3) | 16 (10.7) | |
| Depression | 0.1 | |||
| Normal | 31 (34.1) | 19 (32.2) | 50 (33.3) | |
| Mild | 34 (37.4) | 15 (25.4) | 49 (32.7) | |
| Moderate | 20 (22) | 15 (25.4) | 35 (27) | |
| Severe | 6 (6.6) | 10 (16.9) | 16 (10.7) |
a Values are expressed as No. (%).
Table 3 details the reasons for non-participation in the CR program, highlighting that the primary reason was the inability to afford rehabilitation, with distance being the second most common factor. Chi-square analysis revealed no statistically significant differences in these reasons between men and women (P = 0.4). Table 3 shows the total number of non-participants (n = 100) and highlights the primary reasons for non-participation by gender.
| Reasons for Non-participation | Total (n = 100) | Female (n = 57) | Male (n = 43) | P-Value |
|---|---|---|---|---|
| Distance | 20 (20) | 12 (21.1) | 8 (18.6) | 0.4 |
| Not having a companion | 11 (11) | 5 (8.8) | 6 (13.9) | 0.4 |
| Cost | 69 (69) | 40 (70.1) | 29 (67.4) | 0.4 |
a Values are expressed as No. (%).
5. Discussion
Our research findings reveal significantly lower participation rates among women in CR programs compared to men (Table 1). This aligns with the study by Firoozabadi et al. (17), which involved 1,053 participants, of whom only 357 were female. The primary barriers identified included cost, transportation, distance, and comorbidities. Similarly, Ritchey et al. (18) conducted a study monitoring participation and completion rates among Medicare beneficiaries, finding that only 18.9% of women participated in CR compared to 28.6% of men among 366,103 eligible patients. The adjusted prevalence ratio of 0.91 (95% CI: 0.90 - 0.93) indicates that, after controlling for other factors, women were approximately 9% less likely to participate in the program than men. Participation rates were particularly low for non-Hispanic Black, Hispanic, and Asian women, averaging between 10% and 12%. In a meta-analysis of 297,719 individuals with diagnoses eligible for CR, women exhibited a 36% lower enrollment rate compared to men (19). Despite lower participation rates, research suggests that women can achieve comparable or even greater mortality benefits from CR than men. However, while participation rates among men have improved, those among women have stagnated (14, 20).
Studies have shown several factors significantly impact women's utilization of CR. Women are often older and carry a higher burden of comorbidities, which can lead healthcare providers to perceive them as more complex, resulting in fewer referrals. Common reasons for not enrolling in CR include transportation issues, family responsibilities, and the belief that exercise is tiring or painful (14, 20, 21).
In our study, a notable difference in educational attainment was observed between participants and non-participants. A significant portion of participants held a diploma or university degree, while the majority of non-participating patients had education levels below a diploma (Table 1). Similarly, Svendsen et al. (22) revealed that lower educational attainment was significantly associated with higher odds of not participating in CR and dropping out. Kjesbu et al. (23) found results similar to ours. Their study classified educational levels into three categories: Basic, intermediate, and high, revealing that individuals with lower educational attainment were significantly less likely to engage in CR. In the study by Gaalema et al. (24), involving 1,407 patients, educational attainment was indicated as a key predictor of the number of CR sessions completed. Additionally, they revealed that lower educational levels were associated with less improvement in cardiorespiratory fitness, even after controlling for other factors.
Several factors contribute to the link between educational attainment and CR participation. Individuals with lower education levels often face increased barriers to accessing CR services, such as transportation challenges and limited access to personal vehicles, which are particularly difficult for those with fewer financial resources. Additionally, securing non-emergency medical transportation may be harder for those with less education. The costs associated with CR, including co-pays, also significantly affect attendance; reducing these costs can enhance engagement in preventive health behaviors, especially among individuals with lower educational backgrounds.
Our study found a significant difference in residency patterns, with most CR participants living in urban areas, while many non-participants were from rural regions (Table 1). Similarly, in the study by Guduguntla et al. (25), those living within the same zip code as the rehabilitation facility had a significantly higher participation rate of 46.0%, compared to 34.3% for those outside the zip code. Additionally, they revealed that distance played a crucial role in participation; individuals residing within 10 miles had a use rate of 38.6%, while those living 20 miles or more away saw a marked decrease to 19.5%. In the study by Leung et al. (26), which aimed to explore the relationship between geographic factors and the utilization of CR among patients with coronary artery disease, out of the nine studies that assessed rurality, five (55.6%) found a significant negative correlation between rural residency and participation in CR programs.
Geographic barriers play a significant role, as longer distances to CR facilities can deter participation, compounded by limited transportation options that make access difficult. Infrastructure challenges, such as inadequate public transport and poor road conditions, further complicate the situation. Many rural patients perceive transportation issues as a major barrier, often prioritizing these concerns over the actual distance to facilities, along with anxiety about travel logistics. Additionally, the availability of CR programs in rural areas is often limited, leading to reduced referral rates and lower enrollment. Socioeconomic factors also contribute, as patients in rural regions may have lower financial resources, affecting their ability to travel for CR. Lastly, there may be less awareness of the benefits and availability of CR in these populations. Addressing these barriers through targeted interventions, such as home-based CR programs and improved community outreach, could enhance participation among rural patients.
Conversely, in the study by Van Iterson et al. (27), although residents of large urban areas had the greatest number of CR centers available, their eligibility, participation, and completion rates were significantly lower. In contrast, individuals in noncore rural areas, despite having access to fewer centers, demonstrated higher levels of engagement and success in CR programs. However, in their study, Southern rural residents had participation rates that ranked among the lowest in the nation. The limitation of their study was the inability to explain why noncore rural residents, despite fewer CR centers, showed participation patterns that contradict the assumption that availability affects usage.
Lower participation rates among rural residents in rehabilitation programs can be attributed to two main factors: Distance to services and lower socioeconomic status. Residents in rural areas often face significant travel distances to access these programs, which can discourage them from participating. The challenges of long-distance travel are worsened by limited public transportation options and the necessity of having a personal vehicle, making it particularly difficult for those with fewer resources. Additionally, socioeconomic status plays a crucial role in this context. Rural populations often experience lower income levels and reduced financial resources, which can limit their ability to afford co-pays, travel expenses, and the time away from work needed for rehabilitation sessions. Consequently, rural patients may prioritize transportation challenges over the actual distance to facilities and may be less informed about available resources. This situation can lead to lower referral rates and decreased engagement in rehabilitation programs.
In our study, the use of additional insurance was significantly associated with higher participation rates (Table 1). Similarly, Park et al. (28) in their study, which included 2,988 patients with acute coronary syndrome who underwent percutaneous coronary intervention, revealed that having supplementary insurance or coverage for CR can significantly impact patients' decisions to participate in rehabilitation programs. In the meta-analysis by Sun et al. (29), lacking insurance or relying on self-payment for outpatient cardiac rehabilitation (OCR) services was significantly linked to lower participation rates compared to individuals with any form of health insurance. Farah et al. (30) also reported that cost-sharing was linked to reduced attendance in CR and demonstrated a dose-response relationship, where increased cost-sharing correlated with decreased participation. In our study, more than 95% of participants in the CR program had supplementary insurance, while over 67% of non-participants lacked such coverage.
We also found that 34.7% of participants experienced varying levels of anxiety, ranging from moderate to severe, while 37.7% exhibited similar levels of depression. Additionally, the analysis indicated no significant differences in psychological factors between male and female patients (Table 2). Similarly, in the study by Rao et al. (31), moderate symptoms of depression, anxiety, and stress were found in 18%, 28%, and 13% of adults entering CR, respectively. Those with moderate symptoms showed significantly lower adherence to rehabilitation (P < 0.001). Bruyninx et al. (32) examined data from charts over six years (2012 - 2017) involving 1,178 patients. Among these, a significant percentage (29.3%) reported symptoms of psychological distress, indicating signs of anxiety and depression. Given the significant prevalence of depression and anxiety among cardiac patients referred to our rehabilitation center, along with the emphasis of international CR guidelines on screening all patients for these conditions, it is essential to recognize the impact of treating these disorders on the overall well-being of cardiac patients. Consequently, a more targeted and comprehensive approach to reducing the incidence of anxiety and depression in this population is crucial.
Our study did not find significant differences in the frequency of cardiac risk factors such as diabetes, BP, smoking, overweight, and obesity between the patients who participated in the CR program and those who did not (P > 0.05). However, among participants, 60.7% had high BP, 58% had diabetes, and 55.3% were smokers (Table 1). Additionally, over 80% of patients from both groups were classified as overweight or obese based on Body Mass Index. Gabulova et al. (33) also reported significantly high rates of uncontrolled risk factors among CR patients, including 54.6% with elevated systolic BP, 86.8% with high LDL cholesterol, 60.6% with diabetes, and 66.6% overweight, with 25% obese. In the study conducted by Knapik et al. (34), which involved 731 diabetic patients eligible for heart vessel revascularization, it was found that 38.4% of these patients had poorly controlled blood sugar levels. The lack of distinction in risk factor burden between the two groups reveals a concerning reality: Despite having multiple modifiable risk factors, a significant number of patients were unable to benefit from the comprehensive care provided by the CR program. This indicates the existence of substantial barriers that prevented these high-risk individuals from accessing and engaging with essential secondary prevention services.
The findings of the study emphasize the urgent need for health policymakers to focus on addressing the non-clinical obstacles that hinder participation in CR programs. Factors such as lack of insurance coverage, limited transportation options, and socioeconomic challenges play a crucial role in determining an individual’s ability to consistently attend and complete the recommended CR sessions. Regarding the findings on non-participation among patients referred to our CR program, 59% cited a lack of supplementary insurance as a barrier, 20% identified distance as an issue, 11% mentioned the absence of a companion, and 69% reported cost as a significant problem (Table 3). In a similar study conducted in Europe in 2021 (35), the most common reasons cited by patients for not participating in CR programs were a lack of belief in the benefits of such programs (43%) and distance from transportation (28%). The differences in the primary reasons reported by patients in our study compared to those in previous studies can be attributed to variations in economic conditions between our population and European societies, as well as differences in insurance coverage for these services.
5.1. Limitations
This study has several limitations. First, there may be selection bias, as the study population might not fully represent all cardiac patients, which limits the generalizability of the findings. Additionally, relying on self-reported barriers introduces the possibility of recall and social desirability biases, which may affect the accuracy of the reported reasons for non-participation. The absence of longitudinal data prevents an assessment of long-term adherence and health outcomes among participants. While key demographic, socioeconomic, and geographic factors were considered, unmeasured confounding variables, such as cultural perceptions, provider referral biases, and healthcare literacy, may have influenced participation rates. Although anxiety and depression were assessed, the study did not investigate their direct impact on motivation, engagement, or completion rates of CR programs. Lastly, although the study identifies significant barriers to CR participation, it does not evaluate the effectiveness of potential interventions, such as telehealth options, financial assistance programs, or home-based CR models, which could help address some of the identified challenges. Addressing these limitations in future research could provide a more comprehensive understanding of the barriers to CR participation and inform strategies to enhance accessibility and engagement.
5.2. Conclusions
Regarding the distribution of risk factors in both groups, nearly half of the individuals are still not participating. Therefore, strategies to increase participation are crucial. Gender disparities in CR need to be reduced to ensure equitable access. Appropriate interventions are necessary to address the barriers women face, such as age, comorbidities, transportation issues, and family responsibilities. Strategies should focus on improving referral and participation rates for both genders, with special attention given to social determinants of health (SDOH), including education levels and insurance coverage. Enhancing affordability and access to care is essential for promoting health equity and encouraging program engagement. Additionally, understanding psychosocial factors and encouraging behavioral adjustments are vital for achieving optimal outcomes in managing CVDs within CR settings.