1. Background
Diabetes mellitus (DM) is a metabolic disorder that occurs when the body cannot properly use glucose (1). This condition is caused by insulin deficiencies or resistance due to beta cell dysfunction. Diabetic nephropathy (2), cardiovascular disease (3), and diabetic retinopathy (4) are complications caused by beta-cell dysfunction.
In 2030, the number of patients with DM is expected to increase to 438 million of the adult global population, and it is expected to increase to 642 million in 2040 (5). The most common type of DM is type 2 diabetes mellitus (T2DM) which is occurring with increasing prevalence (3), accounting for 90% to 95% of all DM cases in the world (6). In 2030, it is estimated that T2DM will be the 7th leading cause of death in the world (7). In Indonesia, the number of deaths in 2014 due to DM was around 6% of the total number of non-communicable disease (NCD) deaths (8). The Indonesian Health Research reported that the Yogyakarta Province has the second largest prevalence of DM in Indonesia (9). Sleman Regency was ranked second after the city of Yogyakarta which had the highest number of patients with DM (10).
Diabetes self-management education (DSME) programs are of great importance in the treatment of these patients (11). The “Prolanis Program” is one of the programs promoted by the Indonesian government to control complications due to DM, but it has not been effective. One form of the program implementation is an education program that aims to improve the knowledge, attitudes and behavior (12), especially through DSME (3).
Education is an essential factor in a health promotion program (13) and is one of the techniques that plays an important role in preventing complications (12). Various educational methods are used to control T2DM, including theater performance art (TPA) based community empowerment. The main tools in this empowerment process are education and motivation (14). Education can be conducted in three to four hours with group discussions and counseling (15).
Education through traditional theater performances based-empowerment approach has been applied in Cambodia to increase public knowledge about health (16). Theater performance also can change physical activities and eating patterns behavior. This method provides a chance for everyone to interact and directly observe the ways to change behavior (17). The health belief model (HBM) explains that an individual will feel confident about the possibility of various results from the behavior they choose to do, also there is the perceived value of those results (18, 19).
Education through TPA is very effective because it is in accordance with the living conditions of the surrounding community and is one of the forms of traditional performances they are familiar with (16). The results of the preliminary study by interviews, indicated that one cause of the lack of knowledge is difficulty in understanding the languages provided by the educators. Foreign languages (other than Javanese) are one of the obstacles in conveying material, as well as ineffective communication which creates a tense atmosphere.
2. Objectives
This study aimed to measure the effectiveness of TPA-based community empowerment, as a form of education in improving the self-management behavior of patients with T2DM in Yogyakarta, Indonesia.
3. Methods
3.1. Study Area and Research Sample
This research was conducted at the two public primary care and two privates primary care settings in Sleman, Yogyakarta, Indonesia. The reason for choosing this primary care setting is because it has the most patients with T2DM and already has the “Prolanis program” implemented. The selection of respondents used a total sampling technique. From 138 patients, only 102 were eligible to become respondents. Sample size was calculated according to statistical calculation with statistical power (β) at 20%. According to the formula, a minimum of 32 subjects were needed for each group with a total sample size of 70 respondents. The sample size was already taking into account 10% drop-out probability. Respondents were selected based on inclusion criteria, which were: T2DM patients and enrolled as a “Prolanis” member in primary care, average age 30 until 69 years old, committed to attend TPA, took medication regularly according to the dosage for one full month and has a complete medical record status.
3.2. Research Design
The design of this study used a quantitative method with a quasi-experimental non-equivalent pre-posttest control group design. Knowledge, attitude and practice (KAP) data were collected by using questionnaires which were already validated. The questionnaires was validated and reliabilited with content validity, face validity and construct validity and all items was valid (probability (P < 0.05). All items’ questionnaires was reliable with Alpha Cronbach (Knowledge 0.6, attitude 0.78 and practice 0.82).
The questionnaire was designed based on the recommendations of endocrine experts’ associations and previous studies. All respondents were asked to complete an informed consent form before enrollment in this study and were randomly assigned into the intervention and control groups. The intervention group received TPA two times per month for three months while the control group only received health education from health care personnel. Measurements were done by using a questionnaire that contained three parts.
The instrument used is a closed question, meaning that the respondent chooses from the answers given. Each variable consists of fifteen questions and scores are calculated based on the mean, median, and standard deviation. Knowledge variable, each correct answer is given a score of “2”, “1” for doubtful answers, and “0” for incorrect answers. Attitude and practice variable, each question is assigned a score ranging from “5 to 1” for correct answers, and "0" for incorrect answers.
3.3. Intervention TPA
The preliminary study conducted by the investigator concluded that the most preferred educational media was performing arts. The majority of patients are ethnic Javanese. As a means to increase local credibility, the intervention used is the kind of performing arts that patients prefer. Each patient should learn or experience the basic of skills in drama, dance and vocals.
The intervention was designed based on the HBM and social cognitive theory (SCT). Health belief model (HBM) constructs explain and predict a patient’s healthy behavior, which emphasize the patient’s beliefs about health and health behavior. Meanwhile, the SCT constructs emphasize reinforcements of the patient’s internal and external responses by means of observation. The important constructs of both theories are contained in the TPA. When patients participate in TPA, they will experience firsthand the healthy and unhealthy behaviors of their peers. By sharing these experiences, patients can predict their own health so they can feel motivated to select the healthy behavior.
Theater performing arts (TPA) interventions were done over three months with as many as four-step meetings which were adapted from “The California arts standards for theatre (20). Schedule (nine meetings) and duration (30 minutes) of the intervention were determined based on the agreement of all respondents to avoid boredom (Table 1). The determination of ideas was done by means of discussion groups with the assistance of a performing arts expert and general practitioner. The chosen language was a combination of Indonesian and Javanese (according to the local culture). The intervention given to the control group was conventional health education from the Ministry of Health. The intervention of TPA will be implemented later in the control group after the study is complete.
| Agenda | Schedule | Outcome |
|---|---|---|
| Determining and developing ideas | Meeting I | Performing arts themes, scenario and script |
| Role-play training | Meeting II | Understand the role of the character |
| Designation of characters | Meeting III | Confirm the role of the figures performed |
| Early pre-performance | Meeting IV - VII | Preparation for performing arts |
| Advanced pre-performance | VIII | Final preparation for performing arts |
| Theater performance | Meeting IX | Creates relaxed and fun atmosphere |
aMeeting I - III: Every two weeks; meeting IV - IX: every weeks.
3.4. Data Analysis
Univariate analysis was done to see the characteristics of respondents and pre-post test scores. Normality tests were done before the comparison of difference test. The intervention group was analyzed using Kolmogorov-Smirnov test (n > 50) while the control group was assessed using Shapiro-Wilk test (n < 50). For attitude and practice variables, independent t-test was used, meanwhile knowledge variables were assessed by Mann-Whitney test. The researchers obtained ethics approval before beginning the research from the Medical and Health Research Ethics Committee, on August 12, 2019 (number KE/FK/0938/EC/2019).
4. Results
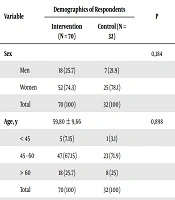
The amount of the initial and final samples of the study did not change, which was 102, consisting of 70 samples in the intervention group and 32 samples in control group. The difference in the number of samples was because in the intervention group all samples were very interested and wanted to watch the performing art show. In addition, they are Javanese ethnicity and enjoy performances of Javanese art. Most of them also have the experience of performing theater, although it happened a few years ago. The majority of samples in the intervention and control groups who were women aged 45 - 60 years old with senior high education. From the results of the statistical analysis, all characteristics were homogeneous (P > 0.05). Homogeneity test of numerical data characteristics was done by using the independent sample t-test (Table 2).
| Variable | Demographics of Respondents | P | |
|---|---|---|---|
| Intervention (N = 70) | Control (N = 32) | ||
| Sex | 0.184 | ||
| Men | 18 (25.7) | 7 (21.9) | |
| Women | 52 (74.3) | 25 (78.1) | |
| Total | 70 (100) | 32 (100) | |
| Age, y | 59.80 ± 9.66 | 0.898 | |
| < 45 | 5 (7.15) | 1 (3.1) | |
| 45 - 60 | 47 (67.15) | 23 (71.9) | |
| > 60 | 18 (25.7) | 8 (25) | |
| Total | 70 (100) | 32 (100) | |
| Education | 0.604 | ||
| No education | 2 (2.9) | 3 (9.4) | |
| Elementary | 18 (25.7) | 6 (18.8) | |
| Junior high | 16 (22.9) | 7 (21.9) | |
| Senior high | 19 (27.1) | 8 (25) | |
| College | 15 (21.4) | 8 (25) | |
| Total | 70 (100) | 32 (100) | |
| Job | 0.103 | ||
| Wage earner | 22 (31.45) | 8 (25) | |
| Not a wage earner | 15 (21.45) | 5 (15.6) | |
| Jobless | 33 (47.1) | 19 (59.4) | |
| Total | 70 (100) | 32 (100) | |
aValues are expressed as No. (%) or mean ± SD.
Pretesting was done by visiting selected samples at Prolanis meetings which are held routinely every two weeks at the research location. The investigators explained the procedure for filling out each item of the questionnaire. The intervention group pretest was done before the PST, while the control group was done before the conventional education in the “Prolanis program”.
In this study, there were significant differences between pre- and post-test mean scores of the attitude and practice variables but not the knowledge variable, in both control and intervention groups (P < 0.05). Substantively, it is said to have a small effect size (d) if d: 0.2, medium effect if d: 0.5 and large effect if d: 0.8 and very large effect if d: 1.3 (21). Hence, PST had a very large power to change practice (d = 1.32) and large effect on attitude (d = 1.11), but had small effect on the knowledge variable (d = 0.3) (Table 3).
| Variable | ΔMean | Std. Dev | P | d (M1-M2) |
|---|---|---|---|---|
| Knowledge | 0.145 | 0.301 | ||
| Intervention | 2.64 | 4.68 | ||
| Control | 1.13 | 5.61 | ||
| Attitude | < 0.001 | 1.109 | ||
| Intervention | 7.49 | 7.04 | ||
| Control | -1.47 | 6.76 | ||
| Practice | < 0.000a | 1.324 | ||
| Intervention | 12.07 | 8.13 | ||
| Control | -1.22 | 7.47 |
aM1, Δ mean intervention; M2, Δ mean control
5. Discussion
Health education is a very important part in controlling DM (22). In this study, education through the performing arts was effective in improving the attitude and practice in controlling blood glucose levels. This education is done based on the community by involving the patient’s active role in exchanging opinions. Education through traditional arts has proven to be effective in increasing knowledge and practice. Patients can exchange experiences in controlling blood glucose based on their daily experiences. Based on this experience patients can increase motivation in participation to control blood glucose practice (23, 24). The TPA approach is an excellent media to deliver health message since can create a relaxed and entertaining environment. The language used was mostly Javanese/Indonesian, so most patients could better understand the material presented. This intervention can be applied in other areas according to local cultural conditions. The determination of preferred cultural arts can be decided by group discussions.
TPADM program was effective in increasing behavior to control their blood glucose, although didn’t show cause and effect relation between knowledge, attitude and practice. The investigator didn’t conduct a methodological investigation, but the possible cause for not increasing knowledge was the routine examination of patients at local health services. Most of the patients received education during routine treatment from the doctor and easy access to health services (25). However, it was difficult for them to understand and implement the material in daily life. The results of this study are similar to previous studies, which explain that most patients with T2DM only knew about the importance but did not understand how to control their blood glucose levels. They received the information from doctors and nurses, but it was difficult to apply it in their daily lives, for example, they still consumed a diet prohibited for patients with T2DM (26).
Theater performing arts still had a very good effect on the patients with T2DM by increasing their attitudes and practice in controlling their blood glucose, although those variables will be interrelated after receiving education (7). The results of this study are different from previous research which stated that education can improve the KAP of patients with T2DM in controlling blood glucose levels (27-29). Obstacles in changing behavior of patients with DM were influenced by knowledge, attitude and beliefs (13).
This program is an educational with a peer group discussion was effectively changed the behavior of patients with T2DM in physical activity and eating control (30). This condition was influenced by the patients’ motivation and perceptions about the importance of introducing DM interventions. It was influenced by the interaction between patients or patients with nurses (professionals) when giving material (31-33). Peers share experiences in controlling blood glucose (34) and improve the self-management of patients with DM (30, 35).
Study results in some countries, education has been developed through art performances. This method has effectively changed the behavior. The success of the program was influenced by the roles of each character in the play (17, 23, 24). In Addition, traditional music and prayer as a good medium for health promotion to increase public awareness about the importance of using the right medicine (23).
This study results provide further support to drive a paradigm shift about the health care system from a doctor-centered approach to a patient-centered approach. In implementing these programs, patients are encouraged to create a relaxed and pleasant atmosphere through effective communication. Such communication can be created through a warm atmosphere, mutual trust, empathy, and mutual respect. Each patient also has the confidence of the facilitator (peers) that they care about, understand, and are mutually concerned with the problem perceived illness (36).
Effective communication between patients is the primary keys to creating a pleasant atmosphere. Also, the selection of an exciting scenario according to the patients’ choice is a success factor in creating this atmosphere. Story scripts and character role plays are essential so that each player has a task according to the agreement. The role of the facilitator is essential, especially in effective communication (37). Duration of education is effective if conducted weekly at a maximum and at least every month (34, 35). Patients’ participation in self-care can be increased through therapeutic communication (38). Also, health workers’ therapeutic communication can enhance the self-awareness and healing of patients (39, 40).
The community empowerment model is characterized by the dominance of the patient’s’ active role. Professionals assist in clarifying the inappropriate patients’ opinions during group discussions (41). Each patient must identify the strengths and obstacles in achieving the goal by actively participating in the assistance of trained health workers (14). The TPADM program can be implemented consistently and continuously through Prolanis activities. Obstacles cause community empowerment to not be achieved, namely, the low quality of human resources and limited support from local institutions (42). Implementing the PSTDM program is necessary to build trust, increase awareness, and develop the program (41, 43).
5.1. Conclusions
The results of the current study indicate that Education through community empowerment-based TPA can be effective in improving the self-management behavior of patients with T2DM in Yogyakarta. If more comprehensive and generalizable studies conducted on the Javanis population support this hypothesis, assessment and correction are executed in non-Javanis patients with T2DM. Education through TPA can create a relaxed, pleasant, and humorous atmosphere so that patients more easily accept and appreciate the health recommendations of the material delivered by their peers.