1. Background
Cerebral palsy (CP) is children's most common movement disorder, with a prevalence rate of 2.2 per 1000 live births. It refers to a group of non-progressive abnormalities in the developing brain that lead to neurological deficits, developmental delays, and postural and movement control disorders (1).
Children with CP also have difficulties with their daily function and participation, resulting in low physical activity levels, such as walking, running, and climbing stairs (2, 3). The movement limitations may vary in different environments, including both indoors and outdoors and at school (4). It may also be associated with impaired cognition, mental retardation, seizures, and sensory impairments (vision, hearing, etc.) (1). These problems result in the children's lack of independence and dependence upon caregivers; again, their participation, social relationships, and interaction with others are restricted. These consequences ultimately reduce their quality of life (3, 5).
Examining the extent of problems with functional activities such as mobility and locomotion requires accurate and sensitive tools. Several observational tools and also questionnaires are available to assess locomotion and mobility problems in children with CP (6). However, observational methods have their limitations, such as the need to spend a lot of time training assessors and the difficulty of using them (7). There are few useful tools in Iran to assess the baseline of locomotion and mobility problems in these children or to evaluate their improvement in the treatment process.
The Mobility Questionnaire (MobQ) specifically measures the problems and limitations of mobility and locomotion in children with CP. This questionnaire is developed to monitor mobility limitations that children with CP experience. According to the definitions of the International Classification of Function, Disability, and Health (ICF), mobility limitation is defined as the difficulty that children have in performing motor activities (mobility. The mobility questionnaire comprehensively examines the movement limitations that a child experiences during the day. The MobQ measures individual participation indoors and outdoors and is a suitable and accurate tool (8).
The MobQ focuses on 47 motor activities. For research purposes, a shorter version (Mobility Questionnaire 28) is suggested, while for clinical applications, a 47-item one is recommended (9). The Mobility Questionnaire differs in many ways from the existing mobility measurement tools. The Gross Motor Function Measure (GMFM) assesses the child in a standard setting (10), while the MobQ measures the care problems that children may have in their environment (indoors and outdoors) (8).
The Activities Scale for Kids and the Pediatric Evaluation of Disability Inventory measure broader measures daily, while the Gillette Functional Assessment Questionnaire Walking Scale and the Functional Mobility Scale are specific to gait assessment; however, both generally assess mobility limitations and measure mobility constraints according to the latest ICF definition (11, 12).
2. Objectives
The validity and reliability of mobility have been assessed in various categories of children with cerebral palsy. In this study, we prospectively studied the internal consistency, factor analysis, and convergent validity of the Persian version of mobility in children with cerebral palsy and the reliability of the 47-item Mobility Questionnaire.
3. Methods
3.1. Study Design
This was psychometric research. The University of Social Welfare and Rehabilitation Sciences approved the study proposal. Then, we obtained ethical approval from the related committee with code IR.USWR.REC.1398.079.
3.2. Participants
In this study, 202 participants (84 girls and 118 boys, with a mean age of 95.92 months ± 23.73), 15 parents, and nine occupational therapists participated. A multistage sampling method was used to determine the construct validity and internal reliability of MobQ. The participants in the present psychometric testing study were caregivers of children aged six to 12 years. Participants were enrolled in the six private pediatric rehabilitation centers in Tehran, Iran, in September 2019. The number of participants was 202 caregivers for measuring factor analysis, convergent validity, and internal consistency, and 30 participants for the reliability part. The inclusion criteria in this study were as follows:
- Respondents who were caregivers of children with CP aged six to 12 years spent more than 11 hours a day with a child for at least a year.
- Children suspected of cerebral palsy by their physicians are referred to rehabilitation centers with a diagnosis of CP.
- Children who have no other major neurological or primary orthopedic problem
The exclusion criteria were as follows:
- An unwillingness of caregivers to respond to the MobQ at any stage of research and
- An incomplete test
3.3. Measures
3.3.1. Demographic Questionnaire
This questionnaire was used to collect information including age, gender, educational level, and parent's education level.
3.3.2. Mobility Questionnaire
This questionnaire was developed to evaluate the limitations that children with CP experience, especially in mobility. The mobility questionnaire comprehensively examines the movement limitations children experience in their daily lives, covering a range of severity levels of movement limitations. Leo D Roorda developed this questionnaire in 2010. Interrater reliability and high intraclass correlation coefficients (ICCs) for MobQues47 (ICC 0.92) and MobQues28 (ICC 0.87) were obtained (8, 9).
3.3.3. Gross Motor Functions Classification Scale
Gross Motor Functions Classification Scale (GMFCS) is a standard observational classification system that categorizes children with CP into five main groups. This classification depends on the children's gross motor abilities and limitations. The need to use assistive technologies and devices also determines the child's score. Children with maximum independence are considered at level 1, and those with minimum independence are assigned to level 5. The validity and reliability of this tool were addressed by Dehghan et al. in 2011 studied the validity and reliability of GMFCS in Persian according to what they obtained. The Persian version of GMFCS could be a reliable classification system for classifying patients with cerebral palsy by medical and rehabilitation professionals (13).
3.4. Procedure
This study was performed in three main steps: (1) Translation and cross-cultural adaptation, (2) validity (construct, face, content, and convergent validity). And (3) reliability (test-retest).
3.4.1. Translation Process and Cross-cultural Adaptation Phase
The translation and cultural adaptation of the Persian version of the mobility questionnaire were performed by the IQOLA method (14). According to the IQOLA method, two people independently translated the original English version of the mobility questionnaire into Persian. These two were bilingual and native in Persian. After preparing two different Persian versions from these two translators, a discussion was held to agree on some different phrases to make one main version. After the agreement for the built version, two other back-translation to English were done by two bilingual translators who had no information about the study.
The developer made a comparison of the English version with the original questionnaire. A pretest was conducted on the Persian version of the mobility questionnaire for face and content validity through a sample including thirty parents of children with CP. The participants reported no difficulties understanding items; consequently, the Persian version of the mobility questionnaire was finalized for further evaluation of validity and reliability.
The parents signed written informed consent. An experienced occupational therapist interviewed the parents of eligible children with CP; they were informed about the purpose and procedures of the study. The demographic data were first obtained, and then the gross motor abilities of the participants were estimated by the Gross Motor Function Classification System (GMFCS). The Persian version of the mobility questionnaire was applied to all participants in two ways: Parents could be given a questionnaire for 24 hours to answer, or the assessor could read questions during one or two face-to-face sessions and then answer the questions. All 47 questions were answered within 20 - 25 minutes. After four weeks, the Persian version of the mobility questionnaire was completed again by the parents of all 200 children. The questionnaire was in paper format, and both rounds of assessment. The questionnaires were given to the parents in the clinic, as they were routine clients in the six clinics that the samples emerged from. The results of both evaluations were recorded. The data obtained from the study were analyzed with SPSS software, version 21.
3.4.2. Validity
The Lawshe method was used for content validity evaluation. The content validity index (CVI) and the content validity ratio (CVR) were used in this part. Nine experts (6 with a Ph.D. and 3 with a master's in occupational therapy and at least ten years of experience) participated and answered some questions about the necessity of each item in the questionnaire. The minimum acceptable value was based on the opinions of 9 experts, with a score of 0.78. In order to ascertain the CVI, experts' opinions on relevance, simplicity, and clarity were obtained; the numerical value of 0.79 was considered acceptable to evaluate the face validity. Accordingly, nine occupational therapists and 15 patients were surveyed regarding the comprehensibility and unambiguity of the questionnaire.
Also, to assess the convergent validity of the Persian version of the "Mobility Questionnaire," the Mobility Questionnaire and GMFCS were used. Convergent reliability is a way to examine the extent to which the evaluation results were correlated with the results of other tools. Two hundred two people completed both questionnaires in this study.
In order to assess construct validity, confirmative factor analysis (CFA) was used using the AMOS23 software. Goodness-of-fit index (GFI) for the CFA model was checked using the following criteria: Chi-2 (χ2) with a ratio < 5 as an acceptable ratio (1), as well as GFI, incremental fit index (IFI), and comparative fit index (CFI) with a cut-off ≥ 0.95 as acceptable (15). parsimonious comparative fit index (PCFI) and parsimonious normed fit index (PNFI) with a cut-off ≥ 0.5 as acceptable (15). Root mean square error of approximation (RMSEA) with a value < 0.08 was considered acceptable (15). Internal consistency was evaluated using Cronbach's alpha. Test-retest reliability and convergent validity were evaluated by the intraclass and Pearson correlation coefficients, respectively. All data analyses were conducted using SPSS version 22 software, except for CFA, which was conducted using AMOS version 22.
3.4.3. Reliability
For the test-retest reliability, 30 parents answered the MobQ after one week, again (16). The gained scores in the first and second assessments were then computed with intra-class coefficients (ICC). Scores were interpreted as fair (0.40 - 0.59), good (0.60 - 0.75), and excellent (≥ 0.75) (17). Anchoring the items was done to calibrate measures in both assessments (18). The standard error of measurement (SEM) was also obtained for agreement measures.
ICC equal to or higher than 0.85 was considered an acceptable minimum of reliability. Also, Cronbach's alpha coefficient was used to evaluate internal consistency. Cronbach's alpha coefficient equal to or higher than 0.70 was considered the optimal level of internal consistency.
Statistical Analysis: Descriptive statistics were used for the measurements. To specify the content validity, CVI and CVR were considered. Absolute and relative reliability was then measured using the standard measurement error index (SEM) and ICC, respectively. Internal consistency was also described by calculating Cronbach's alpha. The test-retest reliability was obtained by calculating the ICC and evaluating the convergent validity according to the GMFCS.
4. Results
Two hundred children (84 girls and 118 boys), with a mean age of 95.92 months and a standard deviation of 23.73 (Table 1), participated in this study. For the content validity evaluation, the CVI and CVR were checked for all questions based on the opinions of 9 occupational therapists (Table 2). The obtained values were above the minimum acceptable value for all questions (content validity index: 0.78).
| Variables | Values |
|---|---|
| Gender | |
| Girl | 118 (58.4) |
| Boy | 84 (41.6) |
| Type of CP | |
| Hemiplegia | 56 (27.7) |
| Diplegia | 52 (25.7) |
| Quadriplegia | 49 (24.3) |
| Other | 45 (22.3) |
| Educational level | |
| school | 93 (46.1) |
| preschool | 16 (7.9) |
| No education | 93 (46) |
| GMFCS | |
| I | 32 (15.8) |
| II | 44 (21.8) |
| III | 23 (11.4) |
| IV | 51 (25.2) |
| V | 52 (25.7) |
| Actin | |
| Splint | 107 (53) |
| Walker | 20 (9.9) |
| Wc | 3 (1.5) |
| PWC | 1 (.5) |
| Other | 10 (5) |
| No | 61 (30.2) |
| Age, mo; maen ± SD | 95.92 ± 23.73 |
aValues are expressed as No. (%) unless otherwise indicated.
| CFA | χ2 | df | P-value | CMIN/Df | RMSEA | PCFI | PNFI | GFI | IFI | CFI |
|---|---|---|---|---|---|---|---|---|---|---|
| Model | 3007.75 | 1034 | < 0.001 | 2.90 | 0.077 | 0.699 | 0.667 | 0.929 | 0.931 | 0.931 |
Abbreviations: CFA, confirmatory factor analysis; CMIN/DF, chi-square/degree-of-freedom ratio; RMSEA, root mean square error of approximation; PCFI, parsimonious comparative fit index; PNFI, parsimonious normed fit index; GFI, goodness-of-fit index; IFI, incremental fit index; CFI, comparative fit index.
Based on the opinion of 9 experts (occupational therapists) and 15 people (parents of children with cerebral palsy) who completed the questionnaire, the Persian version of the mobility questionnaire was shown to be understandable and unambiguous. The ICC in this study was 0.998, with a 95% confidence interval, thus indicating the questionnaire's appropriate reliability. Also, Cronbach's alpha coefficient in this study was 0.996, thus showing that the questionnaire had high internal consistency. In order to assess the convergence validity of the Persian version of the "Mobility Questionnaire," this questionnaire and the GMFCS were completed by 202 people. A high negative correlation coefficient (0.937) was found between the two questionnaires.
In this study, 202 children with CP with an age range of 23.73 ± 95.92 participated. The boys were 58.4%, and the girls were 41.6% of this population. The GMFCS scores showed 25.7% in level 5, 27.7% hemiplegia, and 53% using splints outdoors.
4.1. Confirmatory Factor Analysis
Fitting indices showed that the one-factor structure of the mobility scale has a good and acceptable fit in the community of children aged 6-12 years with cerebral palsy. (RMSEA = 0.077, PCFI = 0.699, PNFI = 0.667, GFI = 0.929, IFI = 0.931 and CFI = 0.931) (Table 2). Therefore, the mobility scale is one-dimensional and was confirmed based on confirmatory factor analysis. All factor loads of the mobility items were greater than 0.7 and significant (all PS < 0.001) (Table 3).
| Item Number | Mean ± SD | Factor Loading | Item Number | Mean ± SD | Factor Loading |
|---|---|---|---|---|---|
| Mobility 1 | 3.14 ± 1.24 | 0.744 | Mobility 25 | 2.12 ± 1.60 | 0.953 |
| Mobility 2 | 3.12 ± 1.19 | 0.729 | Mobility 26 | 2.14 ± 1.62 | 0.945 |
| Mobility 3 | 2.81 ± 1.38 | 0.843 | Mobility 27 | 2.10 ± 1.61 | 0.954 |
| Mobility 4 | 2.63 ± 1.50 | 0.856 | Mobility 28 | 2.14 ± 1.59 | 0.948 |
| Mobility 5 | 2.55 ± 1.51 | 0.902 | Mobility 29 | 2.11 ± 1.59 | 0.947 |
| Mobility 6 | 2.55 ± 1.51 | 0.914 | Mobility 30 | 2.08 ± 1.59 | 0.945 |
| Mobility 7 | 2.66 ± 1.40 | 0.840 | Mobility 31 | 1.91 ± 1.56 | 0.936 |
| Mobility 8 | 2.51 ± 1.44 | 0.885 | Mobility 32 | 1.90 ± 1.57 | 0.925 |
| Mobility 9 | 2.33 ± 1.54 | 0.926 | Mobility 33 | 1.76 ± 1.53 | 0.918 |
| Mobility 10 | 2.23 ± 1.50 | 0.865 | Mobility 34 | 1.66 ± 1.49 | 0.903 |
| Mobility 11 | 2.20 ± 1.56 | 0.897 | Mobility 35 | 1.80 ± 1.55 | 0.929 |
| Mobility 12 | 2.29 ± 1.56 | 0.925 | Mobility 36 | 1.91 ± 1.25 | 0.663 |
| Mobility 13 | 2.25 ± 1.54 | 0.923 | Mobility 37 | 1.71 ± 1.51 | 0.937 |
| Mobility 14 | 2.26 ± 1.54 | 0.913 | Mobility 38 | 1.60 ± 1.50 | 0.926 |
| Mobility 15 | 2.36 ± 1.52 | 0.851 | Mobility 39 | 1.60 ± 1.51 | 0.914 |
| Mobility 16 | 2.17 ± 1.59 | 0.903 | Mobility 40 | 1.57 ± 1.02 | 0.911 |
| Mobility 17 | 2.18 ± 1.55 | 0.914 | Mobility 41 | 1.57 ± 1.54 | 0.926 |
| Mobility 18 | 2.01 ± 1.57 | 0.920 | Mobility 42 | 1.53 ± 1.46 | 0.918 |
| Mobility 19 | 2.05 ± 1.58 | 0.926 | Mobility 43 | 1.46 ± 1.42 | 0.909 |
| Mobility 20 | 2.05 ± 1.56 | 0.915 | Mobility 4 4 | 1.38 ± 1.31 | 0.900 |
| Mobility 21 | 2.04 ± 1.59 | 0.925 | Mobility 45 | 1.39 ± 1.27 | 0.888 |
| Mobility 2 2 | 2.08 ± 1.59 | 0.917 | Mobility 46 | 1.34 ± 1.22 | 0.873 |
| Mobility 23 | 2.01 ± 1.60 | 0.925 | Mobility 47 | 1.32 ± 1.18 | 0.874 |
| Mobility 24 | 2.07 ± 1.62 | 0.935 |
As it is mentioned in Table 4, the ICC in this study was 0.998, with a 95% confidence interval, thus indicating the questionnaire's appropriate reliability. Scores were interpreted as fair (0.40 - 0.59), good (0.60 - 0.75), and excellent (> 0.75) (17). Also, Cronbach's alpha coefficient in this study was 0.996, thus showing that the questionnaire had high internal consistency. Cronbach's alpha coefficient equal to or higher than 0.70 was considered the optimal level of internal consistency. In order to assess the convergent validity of the Persian version of the "Mobility Questionnaire," this questionnaire and the GMFCS were completed by 202 people. A high negative correlation coefficient (0.937) was found between the two questionnaires.
| Analysis | Results |
|---|---|
| Intragroup correlation coefficient (ICC) | 0.998 |
| Cronbach's alpha | 0.996 |
| Spearman correlation coefficient (SCC) | 0.937 |
| Standard error of measurement (SEM) | 75.14% |
| Minimal detectable change (MDC) | 21% |
| Construct reliability (CR) | 0.995 |
| The average variance extracted (AVE) | 0.810 |
Also, the values of AVE > 0.5, CR > 0.7, and CR > AVE indicate the convergent validity of the mobility questionnaire. Acceptable indicators for convergent validity are AVE > 0.5, CR > 0.7, and CR > AVE (19).
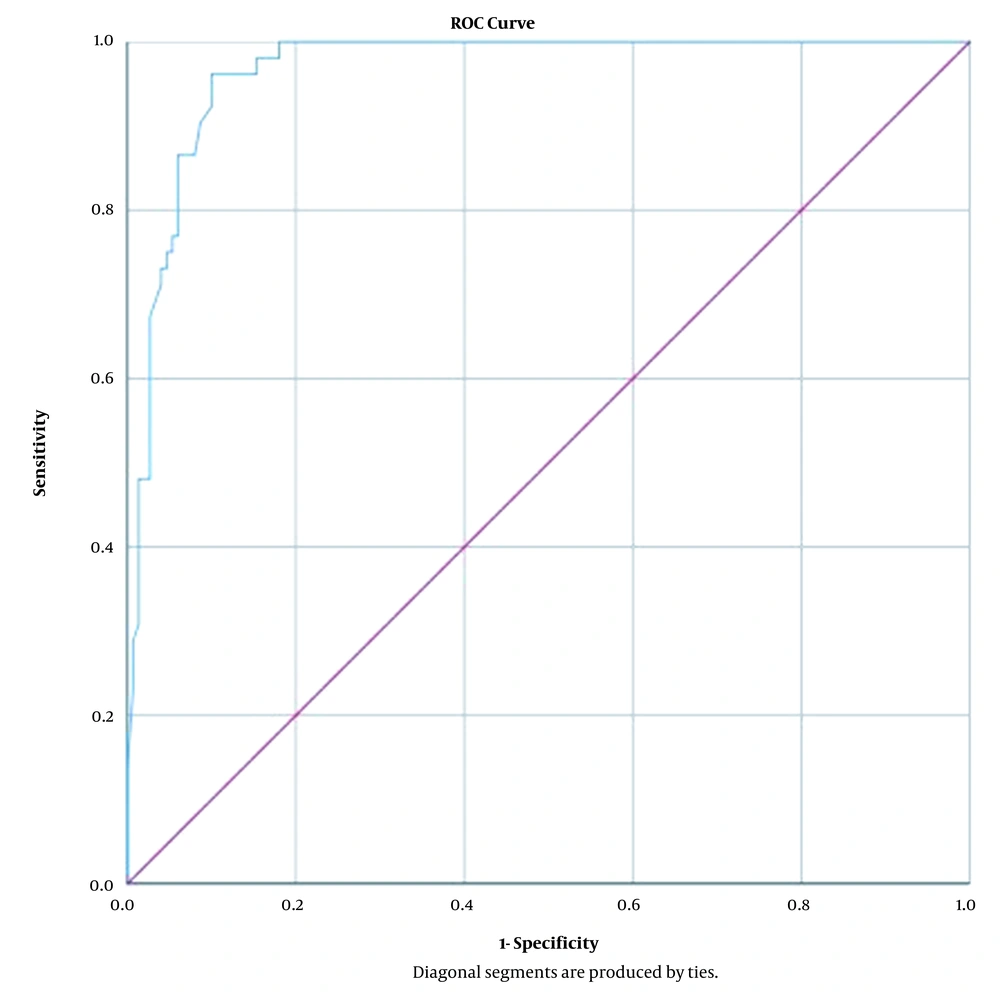
The mobility cut-off point was determined using the GMFCS scale based on characteristic functional curve (ROC) analysis. The area below the ROC curve of 0.967 was obtained with a standard error of .011 (CI: 0.945 - 0.988) (Figure 1). According to the ROC curve, the most appropriate cut-off point for measuring the mobility of children aged 6 - 12 years with cerebral palsy was 137.5; The numerical value of the sensitivity is 0.981, and the specificity is 0.180.
5. Discussion
This study examined the validity and reliability of a 47-item mobility questionnaire. The results indicated the appropriate validity and reliability of the mobility questionnaire in Iranian children with CP.
Reviewing the literature on the mobility questionnaire's validity and reliability showed that only two studies examined the validity and reliability of the mobility questionnaire. The present study results were consistent with both studies' results (8, 20). In another study, van Ravesteyn et al. (8) also examined the interrater and intra-rater reliability, content validity, and structure of the mobility questionnaire. The results on reliability showed that in regard to inter-rater reliability, high intraclass correlation coefficients were obtained for the 47-item mobility questionnaire (92%) and the 28-item mobility one (87%). Regarding content validity, the results showed that 46 of the 47 items of the mobility questionnaire were related to the ICF mobility category. The results related to constructing validity also showed that the decrease in scores in the mobility questionnaire was accompanied by an increase in the level of scores in the Gross Motor Functions Classification Scale. Also, there was a positive correlation between the overall scores of the mobility questionnaire and the Gross Motor Functions Measure (75% with the 47-item mobility questionnaire and 67% with the 28-item questionnaire). Based on the results, the validity and reliability of the 47-item mobility questionnaire in Iranian children with CP were also high (8, 9).
Nine occupational therapists confirmed the content validity analysis for all questions (CVR = 0.78 and CVI = 0.79). In order to evaluate the convergent validity, our hypothesis about the negative correlation between the mobility questionnaire and the GMFCS scores was confirmed, obtaining a high negative correlation between them. We did not expect a strong correlation due to the differences between GMFCS and MobQ. GMFCS can be completed based on parents' opinions, evaluating the gross skill level and classifying children into only five levels; however, the mobility questionnaire pays special attention to the details and skill level, indoors and outdoors.
One advantage of this questionnaire is its feasibility. Completing the mobility questionnaire takes relatively little time, with no problems for the child; it can be used by mail too. In addition, a significant benefit of MobQ is that it shows the potential problems during the activities that mobility is one of their demands. This feature covers the definition of mobility restrictions according to the ICF (8).
Regarding the reliability results, the 47-item mobility questionnaire had good test-retest reliability and internal consistency. So, it can measure changes in children's mobility problems during treatment. According to the factor analysis, a cut-off score of 137.5 was gained, which shows higher numbers than this amount shows a more serious problem in children with CP.
In future studies, the mobility questionnaire's responsiveness should be assessed to ensure that it can be useful for monitoring clinical changes in children's mobility limitations through time.
The present study faced some limitations that should be considered. One of the limitations that can be mentioned is that the inter-rater and intra-rater reliability study was not done. Doing these studies is suggested as well as a constructive validity study. The other limitation was the lack of similar studies of the MobQ psychometric properties in children with CP, which restricted the discussion.
At last, it can be concluded that the Persian version of the MobQ in Iranian children with CP has good validity and reliability, so therapists can use it to determine and pursue treatment goals to improve mobility in children with CP.
5.1. Conclusions
This study showed that the Persian version of the 47-item Mob-Q had good validity and reliability for Iranian children with CP. Therefore, this questionnaire can serve as a practical test to assess mobility in children with CP; it can also be used for clinical and research purposes to measure mobility in children with CP.