1. Background
Coronavirus disease 2019 (COVID-19) as an infection with a long incubation time was detected in Wuhan, China, in late December 2019. It has been considered by researchers worldwide and has threatened people’s mental health (1).
Recently, the World Health Organization projected the need for action on mental health and considered the front-line healthcare workers (HCWs) at greater risk of psychological problems. During such pandemics, HCWs on the front line have to deal with long working hours, greater risk of infection transmission, social isolation, and getting homesick, all of which can potentially give rise to severe psychiatric problems (1-3).
The COVID-19 pandemic is a rapidly evolving situation, and the psychological status of HCWs might be changed in this situation. A limited number of studies have been carried out on the probable strategies that could be used to address the psychological needs of front-line HCWs during this pandemic (4).
One of the interventions for reducing anxiety and increasing resilience in HCWs is Balint group work. Balint group is a group of trained and peer therapists and caregivers discussing the difficulties and issues in their relationship with patients in a thoughtful, insightful, and practical way (5). Balint group aims to change the uncertainty, confusion, and difficulty of perception, understanding, and meaning in the relationship between the caregiver and patient, leading to a more potent therapeutic alliance (6). It also empowers physicians to take the initiative in their profession when there is uncertainty or no clear answer (7). It helps them explore their interpersonal abilities and limitations and perceive and strengthen blind spots in dealing with patients (8). In one study, the effectiveness of the Balint group was evaluated in intensive care unit nurses. The results showed a significant effect of the Balint group on reducing burnout and improving the work quality of nurses (9).
The adjusted prevalence of COVID-19 in 2020 was estimated at 14.2%, accounting for 11,958,346 Iranian COVID-19 cases (10). The number of morbidities, including psychological complications, is higher, especially in vulnerable groups. However, a limited number of studies addressed anxiety and increasing resilience in the medical staff as one of the most at-risk groups. Various pharmacological and nonpharmacological interventions have effectively increased resilience and decreased anxiety caused by COVID-19 (11-14). Different studies on the effect of the treatments, as previously mentioned, have reported contradictory results. In addition, there is only one study about the Balint group in Iran (15).
2. Objectives
No study was found comparing the Balint group and pharmacotherapy in HCWs. Thus, we compared their effect on resilience and anxiety among HCWs.
3. Methods
3.1. Study Design
The present four-week quasi-randomized controlled research was done in Gorgan, Iran, between March 2021 and May 2021. Informed consent was obtained from the subjects who were quasi-randomly divided into parallel intervention groups, including the pharmacotherapy and Balint groups. The alternate allocation method was done following the enrollment order. In simple randomization, subjects were assigned to two groups considering the table of random numbers. The research protocol was registered at IRCT.IR (IRCT20200411047023N1, 26/01/2021).
3.2. Samples
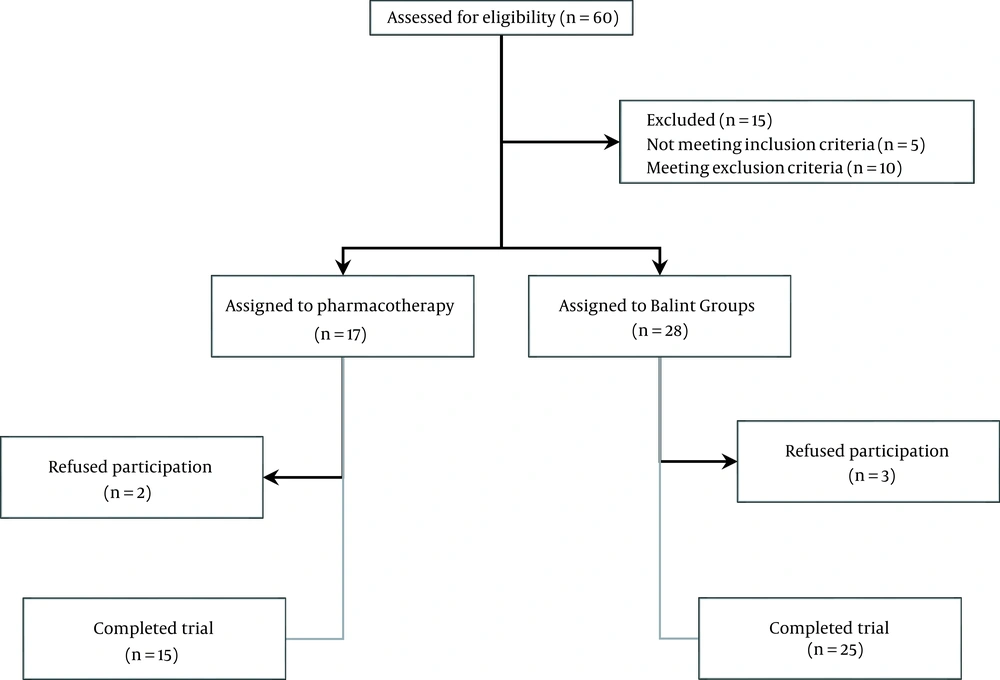
Sixty individuals were evaluated for inclusion criteria, 15 of whom were excluded. A psychotherapy fellowship and a psychiatrist interviewed the participants and assessed them for entering the study. The cases were assigned to two groups, including 17 and 28, in the pharmacotherapy and Balint groups, respectively (Figure 1). The inclusion criteria included cases aged 18 - 59 years who had illness anxiety diagnosed by two psychiatrists considering the diagnostic and statistical manual of mental disorders (fifth edition), no history of psychiatric disease, being capable of using Skype and attending meetings, interaction with suspected COVID-19 patients, and experience of anxiety symptoms. The subjects were excluded in cases of psychiatric diseases other than COVID-19 anxiety, treatment with psychiatric medications, or pregnancy. In addition, those reluctant to continue attending the groups and cases absent from more than three sessions of the Balint group were excluded. Also, HCWs were screened by a blinded psychiatric coordinator for inclusion criteria through interviews by making phone calls.
3.3. Intervention
Those in the Balint group received eight sessions for four weeks. Those in the pharmacotherapy group were given oral sertraline tablets for four weeks (50 mg/day at first and increasing if required based on the tolerance and symptoms of patients). Because of COVID-19 transmission rates, the Balint group sessions were done online using video calls via Skype with nine members, an assistant leader, and a leader, for 60 minutes in each session, twice weekly. Another 15 minutes could be considered. Participants answered research and demographic questionnaires for data collection at baseline and after the study (fourth week). All subjects were assessed at baseline and after the study (pretest and posttest).
In the Balint group, the participants volunteered at the beginning of each session to discuss a problem. The group listened to the story with no interruption. Others could ask questions for more clarification after finishing the story by the presenter. The leader invited the participants to answer what they had heard in different forms. Other members took a reflective approach. Thus, more questions, emotional reactions, advice, and speculations were expected. The group leader discouraged the executor from over-interrogating, as the goal was to get the participants to work on the case. The leader was a psychotherapist trained as the leader of the Balint group (3).
3.4. Sample Size
G-power software 3.1.9.2 (16) was applied to obtain the appropriate number of research samples at a significance level of 0.05, with a beta of about 0.8 and an effect size of 0.5 based on other studies (17). Sixteen individuals were selected, but 20 cases were placed in each group based on the possible dropout rate.
3.5. Data Collection
The questionnaires included the Connor-Davidson Resilience Scale (CD-RISC) and Corona Disease Anxiety Scale (CDAS), which were provided online at https://forms.gle/QWmXdBEFKs2FXEy27 and offered on social media. A brief description regarding the research aim and the principal researcher was considered to explain the survey. Demographic information (e.g., age, gender, education level, and marital status) was gathered.
3.6. Ethical Considerations
The research was approved by the Golestan University of Medical Sciences (IR.GOUMS.REC.1399.023). Participation was voluntary, and the data remained confidential.
3.7. Research Tools
The corona disease anxiety scale has been designed and validated in Iran to assess COVID-19-related anxiety. It has 18 items with two subscales, namely psychological (items 1 - 9) and physical (items 10 - 18) symptoms rating on a four-point Likert scale from never: 0 to always: 3; thus, the total score can range between 0 and 54, and a higher score indicates higher anxiety levels. Its reliability was obtained for the first factor (α = 0.87), the second factor (α = 0.86), and the whole questionnaire (α = 0.91) (16).
Connor and Davidson designed the Connor-Davidson resilience scale. It has 25 items on a five-point Likert scale from completely incorrect: 0 to always true: 4. The total score is between 0 and 100, with higher scores representing higher resilience and vice versa. The cutoff point was set at 50, indicating that scores > 50 show resilience (18). This test has some factors, including positive acceptance of change, personal competence perception, safe relationships, trust in individual instincts, tolerance, and spiritual effects, and tolerance of negative emotions (18). Cronbach’s alpha coefficient was 0.93 for its Iranian version (19).
3.8. Statistical Analysis
SPSS 16 analyzed the data, and the significance level was considered at < 0.05. The data are presented as mean ± standard deviation or frequency (%). The demographic variable homogeneity was assessed using the chi-square and Fisher’s exact tests, if possible, or a t-test. The continuous variables’ normality was assessed by the Shapiro-Wilk test. Because of no normal distribution of variables, the Wilcoxon signed-rank test compared the two groups.
The difference between quantitative variables after the intervention was studied using the analysis of covariance (ANCOVA) while considering baseline and those confounding variables as confounders. The correlations between the CDAS and its subscale differences (before-after) and the CD-RISC and its subscale differences (before-after) were evaluated using Spearman’s correlation coefficient.
4. Results
In this study, 45 eligible subjects were randomized into the Balint (n = 28) and pharmacotherapy (n = 17) groups (Figure 1). Five cases dropped due to non-adherence, and finally, 40 subjects could finish the study intervention after four weeks. No harm or unintended or critical side effects were observed during the intervention. The female-to-male ratios were 21/4 and 12/3 in the Balint and pharmacotherapy groups, respectively. The mean age was 34.0 ± 5.5 and 31.8 ± 3.9 years in the Balint and pharmacotherapy groups, respectively (P = 0.18).
Furthermore, most participants were married and had children. The percentage of individuals with Ph.D. was 68.0% in the Balint group; nevertheless, most subjects in the pharmacotherapy group had a bachelor’s or master’s degree. Moreover, all the participants in the pharmacotherapy group were in contact with suspicious COVID-19 patients. However, some cases in the Balint group had no history of close contact with COVID-19 patients in their workplace (Table 1).
| Balint (n = 25) | Pharmacotherapy (n = 15) | P-Value b | |
|---|---|---|---|
| Sex | > 0.99 | ||
| Male | 4 (16.0) | 3 (20.0) | |
| Female | 21 (84.0) | 12 (80.0) | |
| Age (y) | 34.0 ± 5.5 | 31.8 ± 3.9 | 0.184 |
| Marital status | 0.477 | ||
| Single | 9 (36.0) | 3 (20.0) | |
| Married | 16 (64.0) | 12 (80.0) | |
| Education level | < 0.001 | ||
| MD | 5 (20.0) | 6 (40.0) | |
| BSc or MSc | 3 (12.0) | 9 (60.0) | |
| PhD | 17 (68.0) | 0 | |
| Having children | 0.622 | ||
| Yes | 13 (52.0) | 9 (60.0) | |
| No | 12 (48.0) | 6 (40.0) | |
| Contact with COVID-19 patients in the workplace | < 0.001 | ||
| Close contact with COVID-19 patients | 11 (44.0) | 0 | |
| Contact with suspicious COVID-19 patients | 11 (44.0) | 15 (100.0) | |
| No contact with COVID-19 patients | 3 (12.0) | 0 |
a Data were presented as mean ± SD, frequency (%).
b Based on Fisher’s exact test, chi-square test, or t-test.
The mean differences (before-after) in the total CDAS scores in the Balint and pharmacotherapy groups were 12.3 ± 12.7 and 12.7 ± 8.4, respectively, which were not significantly different (P ≥ 0.52). Since the workplace, education level, and CDAS total score were significantly different between the two groups, ANCOVA was carried out. As shown in Table 2, after adjustment for confounders, there was no significant difference in CDAS scores between the two groups (P = 0.53). The mean decline of psychological and physical symptoms was more in the pharmacotherapy group than in the Balint group. Nonetheless, none of the mentioned differences were statistically significant (P > 0.05). Additionally, a significant improvement was observed in CDAS scores and its subscales in both groups after the intervention (P < 0.01; Table 2).
| Variables and Time Point | Group | Adjusted P-Value | Effect Size (Partial Eta Square) | |
|---|---|---|---|---|
| Balint (n = 25) | Pharmacotherapy (n = 15) | |||
| Score on the psychological symptoms subscale of CDAS | 0.888 b | 0.001 | ||
| Before | 13.7 ± 5.9 | 19.7 ± 4.7 | ||
| After | 7.2 ± 3.6 | 12.3 ± 5.7 | ||
| Difference | -6.5 ± 6.0 | -7.4 ± 5.5 | ||
| P-value | < 0.001 c | 0.002 c | ||
| Effect size d | -0.79 | -0.79 | ||
| Score on the physical symptoms subscale of CDAS | 0.164 b | 0.058 | ||
| Before | 9.0 ± 7.5 | 15.8 ± 5.3 | ||
| After | 3.2 ± 2.6 | 10.5 ± 6.1 | ||
| Difference | -5.8 ± 7.2 | -5.3 ± 4.1 | ||
| P-value | 0.001 c | 0.002 c | ||
| Effect size d | -0.66 | -0.80 | ||
| Total CDAS score | 0.527 b | 0.012 | ||
| Before | 22.7 ± 12.6 | 35.5 ± 9.5 | ||
| After | 10.4 ± 5.3 | 22.9 ± 11.3 | ||
| Difference | -12.3 ± 12.7 | -12.7 ± 8.4 | ||
| P-value | < 0.001 c | 0.001 c | ||
| Effect size d | -0.76 | -0.83 | ||
a Data presented as mean ± SD.
b Based on ANCOVA, adjusted for measurements before the intervention, education level, and workplace.
c Based on Wilcoxon signed-rank test.
d Effect size for Wilcoxon signed-rank test is calculated as Z/√N.
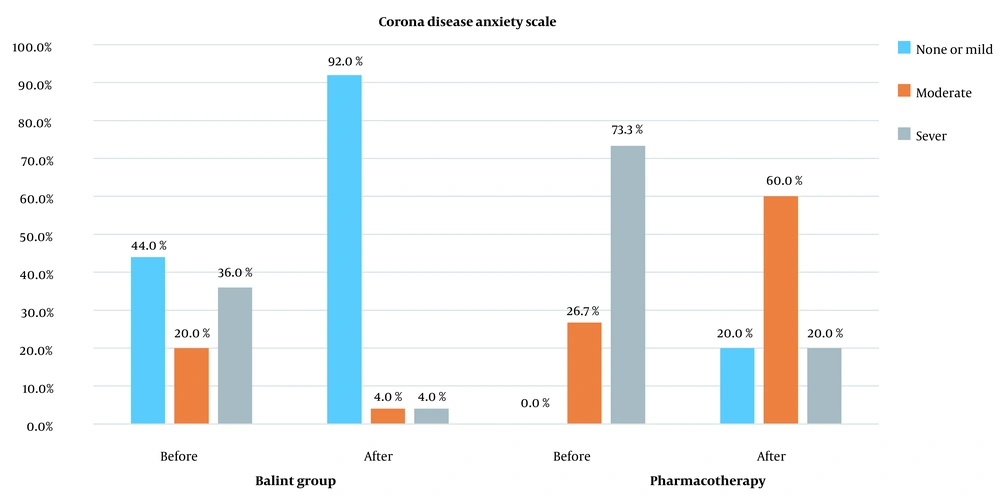
Based on CDAS scores, before the intervention, 20.0% and 36.0% of the individuals in the Balint group had moderate and severe COVID-19 anxiety, respectively, both of which reduced to 4.0% after the intervention. Furthermore, in the pharmacotherapy group, the frequency of mild anxiety increased from 0.0% to 20.0%, and severe COVID-19-related anxiety decreased from 73.3% to 20.0% after the intervention (Figure 2).
There was a significant improvement in CD-RISC subscale scores, including personal competence and trust in one’s instincts, tolerance, and spiritual influences, after the intervention in both groups. However, the positive acceptance of change subscale scores significantly decreased (P < 0.05). The comparison of total scores of the CD-RISC and its domains after the intervention while adjusting for the aforementioned covariates indicated no significant difference between the two groups, except for the spiritual influences domain, which significantly increased in the sertraline group (P = 0.03; Table 3).
| Variables and Time Point | Group | Adjusted P-Value | Effect Size (Partial Eta Square) | |
|---|---|---|---|---|
| Balint (n = 25) | Pharmacotherapy (n = 15) | |||
| Personal competence | 0.696 b | 0.005 | ||
| Before | 19.4 ± 11.1 | 16.3 ± 2.5 | ||
| After | 26.9 ± 4.4 | 25.9 ± 5.5 | ||
| Difference | 7.6 ± 9.7 | 9.7 ± 5.0 | ||
| P-value | 0.003 c | 0.001 c | ||
| Effect size d | -0.59 | -0.88 | ||
| Trust in one’s instincts | 0.364 b | 0.025 | ||
| Before | 16.1 ± 8.7 | 13.9 ± 2.5 | ||
| After | 22.5 ± 3.5 | 22.2 ± 5.1 | ||
| Difference | 6.4 ± 8.4 | 8.3 ± 4.5 | ||
| P-value | 0.001 c | 0.001 c | ||
| Effect size d | -0.65 | -0.85 | ||
| Positive acceptance of change | 0.111 b | 0.075 | ||
| Before | 13.6 ± 7.4 | 10.0 ± 1.8 | ||
| After | 3.7 ± 2.0 | 7.1 ± 4.3 | ||
| Difference | -9.9 ± 7.1 | -2.9 ± 4.4 | ||
| P-value | < 0.001 c | 0.018 c | ||
| Effect size d | -0.82 | -0.61 | ||
| Control | 0.790 b | 0.002 | ||
| Before | 7.9 ± 4.1 | 6.2 ± 0.9 | ||
| After | 10.0 ± 1.9 | 9.5 ± 2.1 | ||
| Difference | 2.2 ± 3.5 | 3.3 ± 1.9 | ||
| P-value | 0.007 c | 0.001 c | ||
| Effect size d | -0.53 | -0.83 | ||
| Spiritual influences | 0.031 b | 0.134 | ||
| Before | 4.2 ± 2.9 | 3.9 ± 0.9 | ||
| After | 5.4 ± 1.7 | 6.3 ± 1.3 | ||
| Difference | 1.2 ± 2.8 | 2.4 ± 1.3 | ||
| P-value | 0.059 c | 0.001 c | ||
| Effect size d | -0.38 | -0.86 | ||
| Total CD-RISC score | 0.527 b | 0.012 | ||
| Before | 61.2 ± 33.3 | 50.3 ± 7.7 | ||
| After | 82.6 ± 11.9 | 80.0 ± 16.4 | ||
| Difference | 21.4 ± 29.0 | 29.7 ± 14.5 | ||
| P-value | 0.004 c | 0.001 c | ||
| Effect size d | -0.57 | -0.88 | ||
a Data presented as mean ± SD.
b Based on ANCOVA, adjusted for measurements before the intervention, education level, and workplace.
c Based on Wilcoxon signed-rank test.
d Effect size for Wilcoxon signed-rank test is calculated as Z/√N.
There was a significant negative correlation between the CDAS and CD-RISC scores (before-after) in the Balint group. This study also investigated the correlation between the subscales of the two studied questionnaires. As shown in Table 4, there was a significant correlation in all the subscales of the CDAS and CD-RISC in the Balint group. In contrast to the Balint group, the correlation between the positive acceptance of change and CDAS psychological symptoms scores was positive and significant (Table 4).
| CDAS | Psychological Symptoms | Physical Symptoms | ||||
|---|---|---|---|---|---|---|
| r | P-Value* | r | P-Value* | r | P-Value* | |
| Balint group | < 0.001 | < 0.001 | < 0.001 | |||
| CD-RISC | -0.742 | -0.791 | -0.728 | |||
| Personal competence | -0.772 | -0.841 | -0.731 | |||
| Trust in one’s instincts | -0.737 | -0.798 | -0.747 | |||
| Positive acceptance of change | -0.751 | -0.825 | -0.694 | |||
| Control | -0.781 | -0.782 | -0.790 | |||
| Spiritual influences | -0.787 | -0.726 | -0.806 | |||
| Pharmacotherapy group | ||||||
| CD-RISC | -0.336 | 0.221 | -0.448 | 0.094 | -0.087 | 0.757 |
| Personal competence | -0.334 | 0.223 | -0.456 | 0.088 | -0.105 | 0.711 |
| Trust in one’s instincts | -0.459 | 0.085 | -0.477 | 0.072 | -0.258 | 0.353 |
| Positive acceptance of change | 0.649 | 0.009 | 0.654 | 0.008 | 0.395 | 0.146 |
| Control | -0.435 | 0.105 | -0.502 | 0.056 | -0.269 | 0.333 |
| Spiritual influences | -0.011 | 0.968 | -0.246 | 0.376 | 0.255 | 0.358 |
a r = Spearman correlation coefficient.
5. Discussion
Anxiety is a common psychological complication among HCWs during the COVID-19 pandemic (20-22). However, a limited number of studies have considered the treatments and coping strategies to reduce this complication. We assessed the effectiveness of pharmacotherapy and the Balint group for increasing resilience and reducing anxiety in HCWs during the COVID-19 outbreak.
It was observed that the Balint group and pharmacotherapy with sertraline significantly reduced anxiety symptoms and increased the resilience of HCWs, consistent with the findings of other studies (23, 24). Limited data are available on the impact of the Balint group on resilience and anxiety symptoms in HCWs, and our research could add data in this regard.
In the current study, there was a considerable increase in resilience and a reduction in anxiety in HCWs, which is in line with the results of other investigations that showed that one of the most influential factors that could make HCWs more resilient is reducing stress and anxiety. Increasing stress awareness also allowed HCWs to be better prepared for the problematic aspects of their work. Another factor is Balint and stress-busting group participation that might facilitate resilience (5, 25). Also, the ability to have an appropriate relationship with the patient can improve clinical outcomes (26). Balint groups can assist medical students and healthcare professionals in increasing their empathy skills and decreasing interpersonal problems (27), thus reducing anxiety in HCWs.
A review of previous studies, consistent with the present study, showed that the Balint group improved the empathy and well-being of HCWs via narrative interactions and respectful inquiry-oriented dialogues, increased resilience, and helped them use more appropriate methods to fight against stress (28). Self-monitoring and self-awareness could also increase resilience in HCWs (29). Thus, the aforementioned findings confirm that the Balint group can increase resilience in HCWs through sharing feelings, stressful experiences, and anxious inner reflections with others and raising their awareness. Accordingly, sharing such experiences can vent negative emotions. Experiencing the commonality of such feelings can decrease anxiety symptoms (30).
Therefore, the reinforcement of emotional and mental conditions of HCWs improves their resilience in facing patients in emotional and stressful situations, which is in line with the results of the present study. Lin et al. declared an association between mental-related variables and the resilience rate of HCWs dealing with COVID-19 (31). Lin et al. reported a negative correlation between resilience and anxiety symptoms and depression and also a positive correlation between active coping style and anxiety and depression symptoms, which is consistent with our result (31).
We also used pharmacotherapy, with a significant effect on increasing resilience and reducing anxiety. The aforementioned result is consistent with the results of other studies (32, 33). The serotonin system is involved in neural anxiety processing. Moreover, sertraline and other selective serotonin reuptake inhibitors increase stress resistance and help individuals be more flexible in tense situations, thus increasing resilience (34). This study showed that pharmacotherapy was more effective than the Balint group but had numerous side effects. Nevertheless, psychological interventions have no side effects and are highly time-consuming (35).
5.1. Conclusions
The Balint group and pharmacotherapy can improve COVID-19-related anxiety and boost resilience in HCWs. Therefore, they are recommended for various groups of HCWs exposed to long-time anxiety and stress.