1. Introduction
Erdheim-Chester disease (ECD) is a very rare, non-familial, xanthogranulomatous non-Langerhans cell histiocytosis of an unknown origin. William Chester and his tutor, Jakob Erdheim (a Viennese pathologist), first characterized this disease in 1930 (1). However, the exact etiology of ECD has not been established. ECD is known to affect multiple organs, with various manifestations of highly variable severity. The classic presenting symptom of ECD is bone pain, followed by bilateral, symmetric metaphyseal, and diaphyseal sclerosis of the long bones. However, gastrointestinal involvement is extremely rare. Herein, we present the case of a 35-year-old man with ECD, who frequently presented to our gastroenterology department with non-specific abdominal symptoms, nausea, and weight loss.
2. Case Presentation
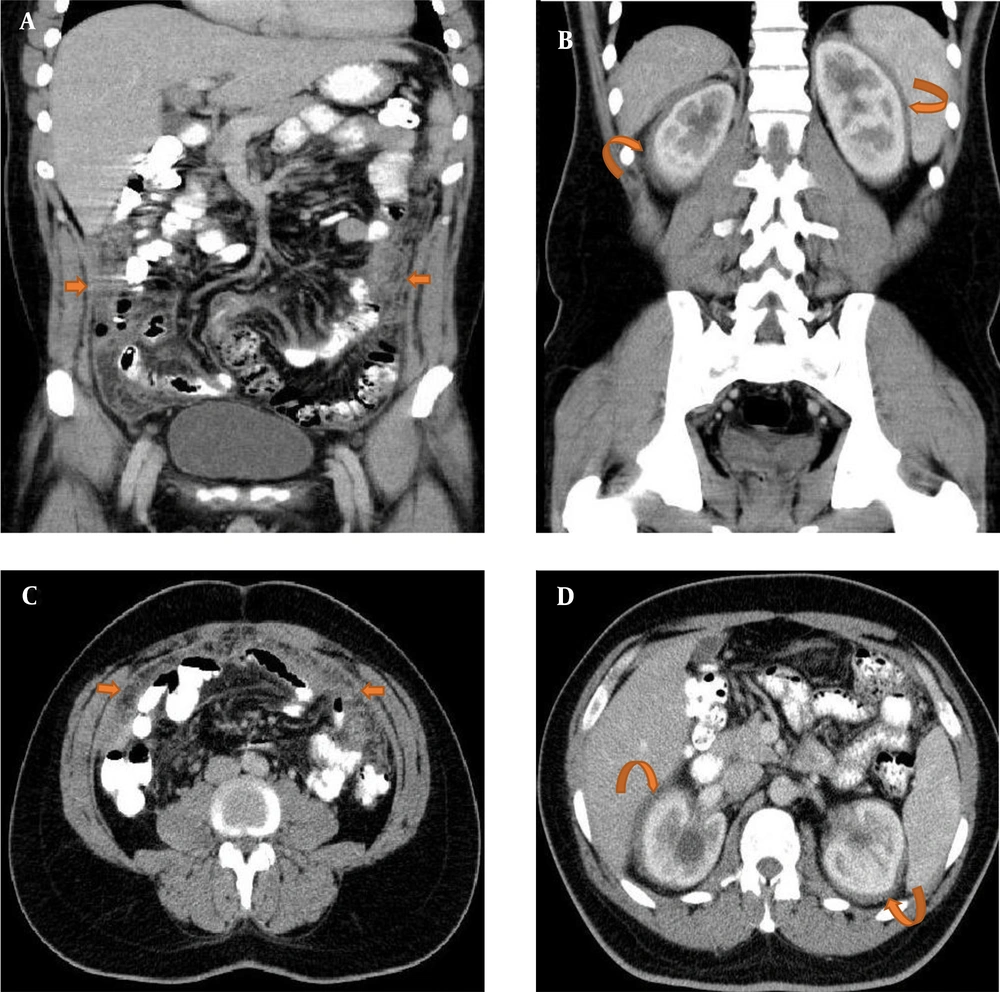
In this case report, we describe the case of a 35-year-old man, presenting to our medical clinic and imaging center. He complained of non-specific abdominal pain, nausea, and weight loss (> 10 kg) for two years. Physical examination and biochemical screening, except for CRP (235 mg/dL) and erythrocyte sedimentation rate (ESR: 65 mm/h), indicated no abnormalities. On the following day, an abdominopelvic computed tomography (CT) scan was performed. It revealed an aggressive peritoneal infiltration surrounding bowel loops, especially the terminal ileum, cecum, and ascending colon, which also affected retroperitoneal structures, including the kidneys, creating a “hairy kidney” appearance (Figure 1). Due to omental caking, peritoneal nodularity, and mesenteric infiltration observed in the patient’s abdominopelvic CT scan, besides unexplained significant weight loss, peritoneal carcinomatosis and lymphoma were included in the differential diagnosis.
A 35-year-old man with non-specific abdominal pain, nausea, and weight loss (> 10 kg) for two years; A, C, Coronal and axial contrast-enhanced computed tomography (CECT) show an infiltrating, heterogeneously enhancing peritoneal soft tissue density, surrounding the bowel loops and significant omental caking (arrows); B, D, Coronal and axial CECT scans show that perirenal fat infiltrates symmetrically, and the perirenal fascia has a “hairy kidney” appearance (curved arrows). The renal calyceal system is also dilated on both sides.
Following the patient’s inconclusive initial evaluations, the medical team decided to perform an additional image-guided core biopsy of the omentum and peritoneum. The microscopic examination of the lesion indicated the infiltration of peritoneal fat by fibrohistiocytic cells and a small population of lymphocytes. Histiocytic cells were composed of sheets of foamy cells with abundant cytoplasm, mixed occasionally with Touton giant cells. These cells displayed features of ordinary histiocytes. Besides, several regular mitoses were found. Immunophenotypically, the cells were positive for the histiocyte marker, CD68, and negative for S100, Langerin, and cytokeratin (Figure 2).
A, Infiltration of peritoneal fat by fibrosis and histiocytic cells (Haemotoxylin and Eosin [H&E] staining, × 200 magnification); B, Infiltration by fibrohistiocytic cells, lymphocytes, and several Touton giant cells (H&E staining, × 400 magnification); C, Sheets of foam cells with abundant cytoplasm (H&E staining, × 400 magnification); and D, CD68-stained macrophages (immunohistochemistry, × 200 magnification).
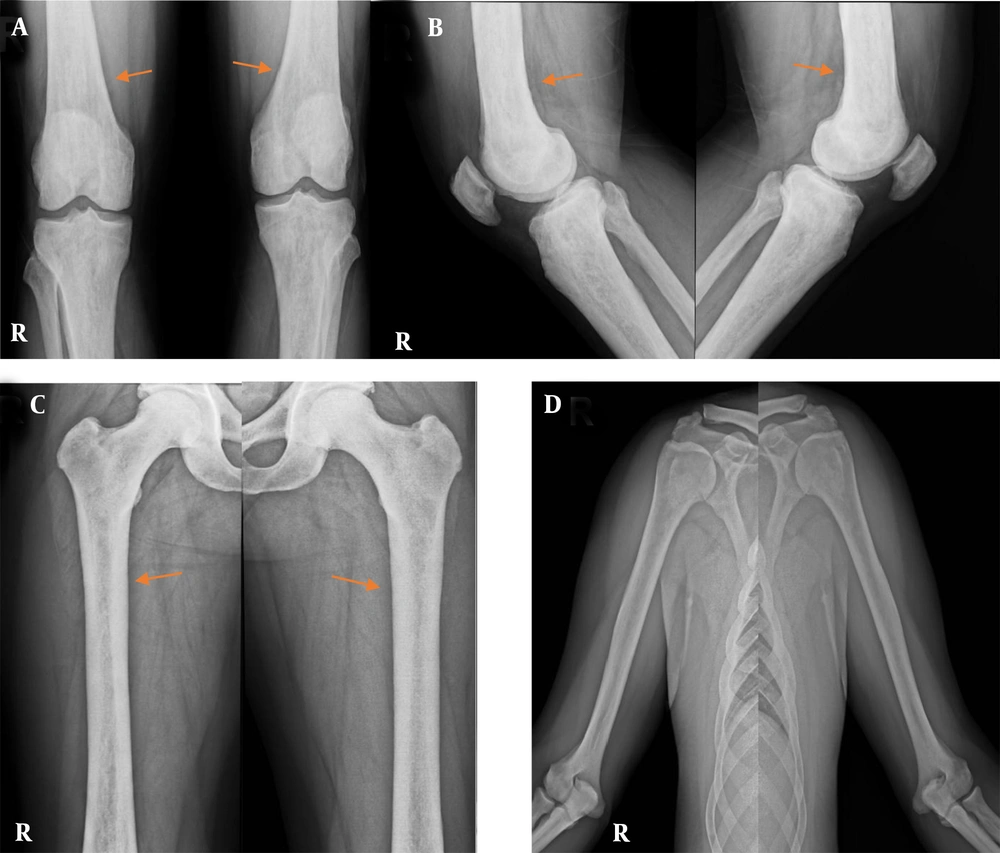
Further radiographic skeletal survey, based on the histopathological results of ECD, as a multiorgan systemic disease, was carried out, which indicated diffuse sclerosis in the long bones of the lower limbs (Figure 3).
3. Discussion
ECD is an uncommon, non-inherited, multiorgan non-Langerhans cell histiocytosis, with an unknown pathogenesis. It is commonly diagnosed in middle-aged people, with a marginal male predilection. Pathologically, this disease is characterized by the infiltration of lipid-laden histiocytes, Touton giant cells, and a variable extent of background fibrosis. In the immunohistochemical tissue study, the histiocytes stained positive for CD68, whereas S-100 and CD1 were negative, unlike Langerhans cell histiocytosis (LCH). Moreover, it is associated with BRAF V600E mutations (2). The concurrence of ECD with LCH with double infiltration of various cells has been also reported (3-5).
ECD usually presents with a range of non-specific manifestations; however, the most common presenting symptom is bone pain, followed by bilateral, symmetric metaphyseal, and diaphyseal sclerosis of the long bones in the majority of patients (6). Rarely, patients show clinical symptoms, such as gastrointestinal involvement, and misdiagnosis can contribute to several futile medical treatments. Symmetric osteosclerosis of long tubular bones has been reported in mastocytosis, lymphoma, myeloid metaplasia, and metastasis (6, 7). Nevertheless, this finding is a classic sign to confirm the diagnosis of ECD, along with the characteristic histopathological results (1, 2).
Additionally, more than half of ECD patients have extraskeletal manifestations, such as retroperitoneal fibrosis, orbital infiltration, interstitial lung disease, bilateral adrenal involvement, testicular infiltration, and breast, central nervous system, and/or cardiovascular system involvement (8). It is known that fat infiltration and high levels of foamy histiocytes around the retroperitoneal structure are the main causes of retroperitoneal involvement. Besides, the associated fibrosis results in perirenal and/or ureteral obstruction, as well as renal problems; nearly 29 - 59% of patients with ECD experience this problem (6, 9).
In contrast, a small number of patients experience hepatic, pancreatic, mesenteric, and gastrointestinal tract problems (1, 2, 4). Considering our patient’s symptoms, such as reduced appetite, persistent nausea, and considerable weight loss, the diagnosis of ECD was challenging. Generally, all cases of ECD require tissue biopsy under imaging guidance (ultrasound or CT) using a percutaneous approach to confirm the diagnosis and detect related mutations to achieve the treatment goals. The omental biopsy of the patient confirmed omental involvement by infiltration of foamy cell sheets mixed occasionally with Touton giant cells that were positive for CD68 (a histiocyte marker) and negative for S100, Langerin, and cytokeratin.
Moreover, our patient had characteristics consistent with skeletal involvement. The radiological survey revealed the increased density of the long bones. Retroperitoneal involvement was another characteristic of ECD in our case. Among formerly reported cases of ECD, the present case is unique, because despite his characteristic histological and radiological findings that confirmed the diagnosis of ECD, the initial gastrointestinal manifestations of ECD, indicating omental caking in abdominal CT scans, differed from those described in the literature.
The mortality rate of ECD is high. Among patients with a diagnosis of ECD, oral corticosteroids are common treatments; however, recent studies have reported the positive effects of interferon-based therapy on increasing patient survival (10, 11). Pulmonary fibrosis and cardiac failure are major causes of mortality, and it is believed that the extent and distribution of extraskeletal involvement have a major contribution to prognosis. In our case, treatment was initiated with subcutaneous interferon-α (3,000,000 units three times per week). After six weeks, his clinical condition improved relatively. He is currently receiving follow-up care by our clinical team.
In conclusion, ECD is an uncommon, non-familial, multisystem, non-Langerhans cell histiocytosis, with various manifestations of highly variable severity. Extraskeletal manifestations also occur and predict a poor prognosis.
![A, Infiltration of peritoneal fat by fibrosis and histiocytic cells (Haemotoxylin and Eosin [H&E] staining, × 200 magnification); B, Infiltration by fibrohistiocytic cells, lymphocytes, and several Touton giant cells (H&E staining, × 400 magnification); C, Sheets of foam cells with abundant cytoplasm (H&E staining, × 400 magnification); and D, CD68-stained macrophages (immunohistochemistry, × 200 magnification). A, Infiltration of peritoneal fat by fibrosis and histiocytic cells (Haemotoxylin and Eosin [H&E] staining, × 200 magnification); B, Infiltration by fibrohistiocytic cells, lymphocytes, and several Touton giant cells (H&E staining, × 400 magnification); C, Sheets of foam cells with abundant cytoplasm (H&E staining, × 400 magnification); and D, CD68-stained macrophages (immunohistochemistry, × 200 magnification).](https://services.brieflands.com/cdn/serve/3170b/46356173e7960f5543fd9cbe9b0cce986cff63f9/iranjradiol-119390-g002-F2-preview.webp)