1. Introduction
Bilateral supernumerary kidney is uncommonly a renal abnormality. The real frequency of supernumerary kidney could not be computed due to its unusual appearance. There are five cases presented in the literature (1-5). In embryogenesis, the atypical section of nephrogenic cord into two metanephric blastemas with bifurcation of one bud shapes supernumerary kidneys. Genuinely, supernumerary kidney that is an accessory organ has its own collecting system, blood supply, and separate encapsulated tissue. The supernumerary kidney may be completely distinct from the usual renal tissue or linked to it by loose connective tissue (6, 7). In our case, we demonstrate radiological findings in a young man with bilateral supernumerary kidney on computed tomography.
2. Case Presentation
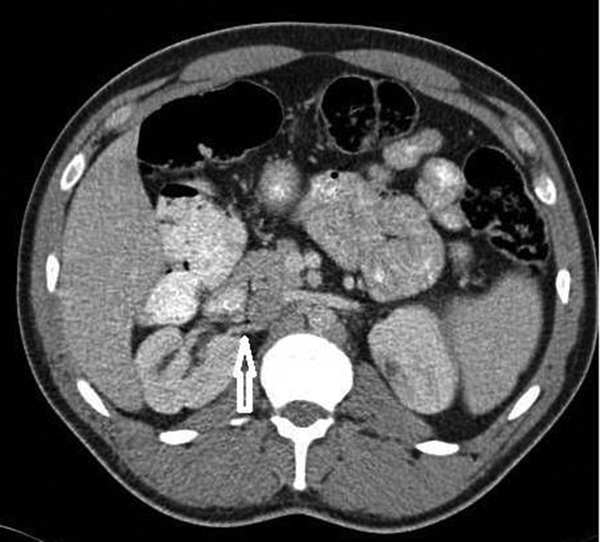
A 23-year-old man was admitted to the endocrinology clinic with a one-year history of hypertension. His laboratory tests were normal. US showed bilateral lobulated kidneys and dilated collecting systems. The renal parenchyma was normal on ultrasonography (USG). The color Doppler study was performed, but the renal arteries were not shown because of gas artifact. Then, abdominopelvic computed tomography (CT) examination (Somatom Emotion Duo CT, Siemens, Berlin, Germany) with 100 mL of nonionic intravenous contrast material (Ultravist 300; Schering, Germany) was performed for differential diagnosis with the following scanning parameters: 0.6 mm collimation, 5 mm slice thickness, 1.4 mm increment, 100 kV, 135 mAs, and a pitch of 0.9. Intravenous contrast material was administered through a catheter in the right cephalic vein. It was injected at a flow rate of 5 mm/second applying an automatic injector. Bilateral supernumerary kidneys were demonstrated on CT (Figure 1A-C). On each side, there was fusion between the two kidneys. A significant rotation anomaly was found at the inferiorly located kidneys that were smaller than the superiorly located kidneys on each side. The collecting system of all four kidneys was expanded (Figure 2). On each side, there were two renal arteries that originated from the aorta (Figure 3 and 4). Intravenous pyelogram and CT angiography were not performed for the patient. A conservative approach was decided with regular follow-up including urine and blood analysis and US.
3. Discussion
Bilateral supernumerary kidney is an uncommon renal abnormality, which influences both genders evenly (8). It is commonly smaller, situated usually in the left quadrant and it may be placed in a caudal situation. The supernumerary kidneys may be established in the iliac or sacral region (9). A narrow stratum of fibrous structure may closely separate supernumerary kidneys or it is entirely discrete from the opposite side. Embryologically, the fundamental difference must discriminate the rare supernumerary kidney from the usual combined duplex systems. A sprout diverges and every division permeates a freely mixed metanephric mesenchymal mass and bifid ureters in combined duplex bifid kidneys. Once two sprouts originate disparately from the Wolffian duct and permeate the similar metanephric mass, two free nephritic collecting structures shape, but the parenchymas abide blended. A sprout divides into two and every division permeates separately a metanephric mass, which improves into unrelated simple kidneys in supernumerary kidneys with bifid ureters (6, 10). The supernumerary kidney disagrees from the duplex kidney and megapolycalycosis in that its own divided parenchyma crowns each pelvicaliceal system (4). In most of the patients with supernumerary kidneys, the pathologies of upper urinary tract have been reported. The ureter of the supernumerary kidney may have calculus disorder and hydronephrosis (11). Supernumerary kidney may be cranial or caudal to the normal kidney. In our case, the location of the supernumerary kidneys was caudal. Coarctation of the aorta, ectopic ureteral opening, duplication of the penis or female urethra, vaginal atresia and horseshoe kidneys are congenital anomalies associated with the supernumerary kidney (12). Bilateral supernumerary kidney in conjunction with horseshoe anomaly was described by Mustafa (5). Bilateral supernumerary kidney with vaginal atresia was described by Shane (1). No other congenital anomalies could be discovered in our case. Oto et al. described bilateral supernumerary kidney with bifid ureters bilaterally in intravenous pyelography (IVP) (3). In our case, we could not perform IVP for the patient. So, we could not demonstrate bifid ureters. Pinter et al. described supernumerary kidneys with ureteral atresia (4). We could not signify ureteral atresia. Supernumerary kidney may be symptomatic in most of the patients. A palpable abdominal mass, pain and fever are commonly the demonstrating symptoms (6, 9). If there is no symptom in the patient with supernumerary kidneys, medical care is not needed and regular follow-up is suggested. If renal disease is found, nephrectomy is advised (11). Associated with supernumerary kidneys, many complications such as pyelonephritis, stones, pyonephrosis, hydronephrosis, and malignant changes (clear cell carcinoma, Wilms’ tumor) have been reported (11, 13). In our case, bilateral supernumerary kidney associated with hypertension was observed. Excretory urography, USG, CT, nuclear scintigraphy, and magnetic resonance imaging (MRI) can be used for the diagnosis of supernumerary kidney. Favorito et al. reported that it is possible to observe supernumerary kidneys. In addition, they reported that MRI can show the presence of individual ureters (14). It is hard to diagnose supernumerary kidney before operation and clinicians have not observed most cases preoperatively. On excretory urograms, it is difficult to identify supernumerary kidney since they are commonly smaller and have a decreased function (9, 11). On each side, in our case, CT had characteristic findings and obviously presented the combination of kidneys. We think that CT commonly appears to be enough for the diagnosis of supernumerary kidneys. CT angiography may be a useful radiological method to discover the compound anatomy of arteries in kidneys and to discern the origin of renal arteries non-invasively. The use of MR angiography to detect the origin of renal arteries could be an alternative.