1. Background
Primary dysmenorrhea is a common gynecological problem among women of reproductive age. It is defined as recurrent menstrual cramps of uterine origin without obvious medical pathology, causing physical, mental, and social changes such as mood swings and socioeconomic changes. It can also cause considerable restrictions on all activities (1, 2). Dysmenorrhea affects between 45 - 95% of women with menstrual periods (3). In severe cases, it can cause absence from school, which happens among 14 - 51% of students (4). Pain is one of the most important influencing factors on lower quality of life (QOL) (5). QOL is defined as an individual’s perception of life from different aspects and is regarded as a daily routine challenge (6, 7). Researchers have shown a decline in health-related QOL in women with dysmenorrhea (8).
2. Objectives
This study aimed to assess QOL in medical students with dysmenorrhea.
3. Methods
The present cross-sectional survey included 298 female medical students in Shohada Tajrish hospital affiliated to Shahid Beheshti University of Medical Sciences, Tehran, Iran between December 2021 and August 2022. Out of 315 participants, 17 students were excluded due to not meeting inclusion criteria, and 298 subjects were enrolled in the study. The inclusion criteria were female medical students aged at least 18 years old. Exclusion criteria were psychological disorders, chronic pain in other organs, irregular menses, cancer, and known cases of endometriosis or amenorrhea.
All participants signed the informed consent documents. The survey was distributed online using the Google platform to fill out the EQ-5D-3L questionnaires. The reliability and validity of the Persian version of this questionnaire were evaluated by Dastourani et al. (9). EQ-5D-3L scale as a useful tool for measuring health-related QOL consists of five dimensions: mobility, self-care, daily activity, pain or discomfort, and anxiety or depression (10). Each item is scored based on a three-point scale (never = 0, sometimes = 1, and always = 2). Data including age, weight, height, sleep hours per day, and exercise hours per week were also evaluated. The study protocol was approved by the ethics committee of the Functional Neurosurgery Research Center (FNRC) at Shohada Tajrish Hospital. The data were analyzed using the Statistical Package for the Social Sciences (SPSS) version 22 (IBM Inc.). P-value < 0.05 was regarded statistically significant.
4. Results
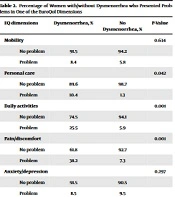
Out of a total of 315 medical students, we included 298 individuals with a mean age of 20.32 ± 3.19 years and BMI of 21.65 ± 3.22 kg/m2. The prevalence of dysmenorrhea among students was 83.6% (n = 249), while only 16.4% of them reported no menstrual pain. The lifestyle variables of groups with/without dysmenorrhea were demonstrated in Table 1. EQ dimensions were presented in Table 2. There was a statistically significant difference between the two groups considering exercise hours per week (P = 0.049) and daily activities (P = 0.001). Students with dysmenorrhea experienced significantly higher pain and discomfort (P = 0.001). Also, personal care was reduced among subjects with dysmenorrhea (P = 0.04). Sleep hours per day, BMI, age, mobility, and anxiety were similar between the two groups. Regarding the self-perception scores of EuroQol, the mean score of the study samples was 75.33 ± 11.20 with a minimum of 18 and a maximum of 100.
| Lifestyle Variables | Dysmenorrhea | No Dysmenorrhea | P-Value |
|---|---|---|---|
| Age | 20.70 ± 2.25 | 20.16 ± 3.20 | 0.281 |
| BMI | 20.23 ± 3.19 | 19.99 ± 3.38 | 0.163 |
| Hours of sleep/day | 8.23 ± 1.05 | 8.17 ± 1.20 | 0.315 |
| Hours of exercise/week | 1.52 ± 1.07 | 3.57 ± 0.60 | 0.049 |
a Values are expressed as mean ± SD.
| EQ dimensions | Dysmenorrhea, % | No Dysmenorrhea, % | P-Value |
|---|---|---|---|
| Mobility | 0.634 | ||
| No problem | 91.5 | 94.2 | |
| Problem | 8.4 | 5.8 | |
| Personal care | 0.042 | ||
| No problem | 89.6 | 98.7 | |
| Problem | 10.4 | 1.3 | |
| Daily activities | 0.001 | ||
| No problem | 74.5 | 94.1 | |
| Problem | 25.5 | 5.9 | |
| Pain/discomfort | 0.001 | ||
| No problem | 61.8 | 92.7 | |
| Problem | 38.2 | 7.3 | |
| Anxiety/depression | 0.297 | ||
| No problem | 91.5 | 90.5 | |
| Problem | 8.5 | 9.5 |
5. Discussion
In the present study, dysmenorrhea was found to be a prevalent gynecological pain amongst medical students with 249 (83%) affected individuals; however, other studies estimated its prevalence in the world at 50 - 90% (11, 12). This result was in line with other studies that reported the prevalence of dysmenorrhea by 75 - 85% (13-15). In a meta-analysis study, Omani Samani et al. reported that prevalence of menstrual disorders in Iran was 73.27% (16). This dispersion in prevalence can be explained by the difference in the age of the participants in the study, the assessment methods of dysmenorrhea, or even a different definition of dysmenorrhea. Some studies showed that with increasing age, disorders related to dysmenorrhea decreased (17-19). This study showed that the hours of physical activity per week in the group without dysmenorrhea was significantly higher than those who experienced dysmenorrhea. In line with our study, Joshi et al. reported that dysmenorrhea had a negative impact on QOL; however, they found no association between exercise and dysmenorrhea (14). A clinical trial by Kannan et al. reported that physical activity significantly reduced pain associated with dysmenorrhea, even though it had no effect on the occurrence of pain (2). A meta-analysis study indicated that exercise and physical activity reduced the intensity of pain and other symptoms related to menstruation (20). Ortiz stated that probably 50 minutes of exercise three times a week could have positive effects in reducing menstrual pain (1, 11). Another study reported that home exercise could lead to a significant improvement in the QOL related to health and pain in patients with dysmenorrhea (21). In general, studies have stated the positive effects of exercise on improving the QOL during menstruation period. The findings of this study indicated that dysmenorrhea can significantly reduce daily activity. In line with this study, Joshi et al. showed that people with dysmenorrhea experience three times more chance of reducing daily activities than people without dysmenorrhea (14). In the study by Sima et al. which was conducted on medical students, people with dysmenorrhea had less energy for their physical activities, and its amount depended on the severity of dysmenorrhea symptoms (15). Another study indicated that moderate and severe dysmenorrhea had a negative impact on school and daily activities (22). In addition, more than 60% of women with dysmenorrhea reported its effects on their daily activities, including attending the classroom (23). In the study by Rostami, dysmenorrhea decreased daily activity and school attendance, and it did not even improve by using painkillers (24). The study by Rakhshaee reported that severe dysmenorrhea led to increased absence from the university and limited the social and daily activities of the individuals (25). The results of numerous studies showed that the severity of dysmenorrhea could affect the QOL of people, such as presence in the society and daily activities. Regarding the indicators of QOL, there was no significant correlation between anxiety and depression and QOL in dysmenorrhea; a similar study also approved this issue (13). Also, a study conducted on 376 medical students found no association between stress and dysmenorrhea (26). In a study conducted on girls aged 12 - 18, the results indicated that dysmenorrhea could increase anxiety and depression, while the degree of depression had no effect on dysmenorrhea (4). In another study, Onur et al. reported that dysmenorrhea increased feelings of pain and stress and also affected communication with family and friends (21). In a systematic review, it was shown that women during menstruation experience a poor mental state compared to the follicular phase (painless period), or people with dysmenorrhea (3, 27, 28). In addition, there was a high correlation between depression and anxiety with menstrual pain (3, 29, 30). The different results in the studies can result from the other factors that affect mental health, including the socioeconomic status of the subjects or the dietary pattern that can affect inflammatory factors and oxidative stress. Pain and discomfort in dysmenorrhea have been stated as one of the influencing factors in the QOL of people during menstruation, which can affect various dimensions of a person's life, including social activity and physical activity (3, 31-33).
The present study showed that people with dysmenorrhea experience significantly higher pain and discomfort. In line with our study, Fernandez-Martinez et al. found that pain and discomfort levels were higher in people with dysmenorrhea (13). In the study by Fernandez et al., the results showed that severe pain was more common in younger women (12). Also, another study showed that moderate to severe pain was significantly higher in people with dysmenorrhea (19). Mohapatra et al. showed that people with a lower BMI experienced higher levels of dysmenorrhea pain (34). In the present survey, BMI was similar among participants. However, a longitudinal study in Australia demonstrated that underweight and obese women were at higher risk for dysmenorrhea (35). This inconsistency is because most of the participants in our survey had a normal BMI. The results indicated that the intensity of pain in dysmenorrhea is different, and it is related to the conditions of people. This study also showed that personal care significantly reduced in people with dysmenorrhea. However, in the study by Bavil et al., that there was no difference between the self-care of people with dysmenorrhea and without dysmenorrhea (36). Also, the study by Fernandez-Martinez et al. did not observe any difference between these two groups (13).
5.1. Conclusions
This study was conducted on medical students. Therefore, due to the cross-sectional study design, the causality between QOL and dysmenorrhea is ambiguous. Since our study sample was limited to medical students, the study population cannot represent the whole society. In addition, we collected data through self-report, which is based on the individual's perception of pain. Also, we did not consider marital status, socioeconomic status, and cigarette or alcohol consumption, which can be confounding factors and influence QOL. Also, we did not calculate the minimum sample size. There is a relatively small sample size in groups without dysmenorrhea. In conclusion, further studies with higher sample sizes are recommended.