Dear Editor,
In the last days leading up to the end of 2019, the Chinese government officially announced the outbreak of an epidemic with a new type of coronavirus, which later became known as COVID-19 (1). The disease soon spread not only to various cities and regions in China but also to other countries; then, the disease spread across the world and became a global pandemic (2).
Kawasaki disease (KD), also known as Kawasaki syndrome, is a rare disease in children that causes vasculitis (inflammation of the walls of blood vessels in the body). According to the British National Health Service (NHS), this condition, also known as mucosal lymph node syndrome, usually affects children age five years or younger (3). Symptoms of KD include high fever that lasts for at least five days, accompanied by scarlet-like skin rash, swollen lymph nodes in the neck, chapped lips, redness of the fingers and toes, and redness of the eyes. Kawasaki disease is very rare, just like COVID-19, which does not currently cause serious and complex complications in children, but it is important for physicians to be aware of any possible link between KD and COVID-19; therefore, immediate action can be taken if necessary.
Kawasaki disease is a leading cause of acquired heart disease in the United States, and serious complications can include aneurysms and dilation of the coronary arteries (4). The cause of KD has not been fully understood to date; however, there is a theory that children with the disease may have been genetically predisposed to it, meaning that they inherited certain genes from their parents. Kawasaki disease is not contagious in itself, meaning it is unlikely to be caused by a virus alone. Standard treatment for this condition, which includes aspirin and intravenous immunoglobulin (IVIG), can significantly prevent coronary heart disease (CHD). According to the NHS, approximately 25% of children with untreated KD develop heart failure. It was reported that most children with KD recover entirely if treated immediately (5).
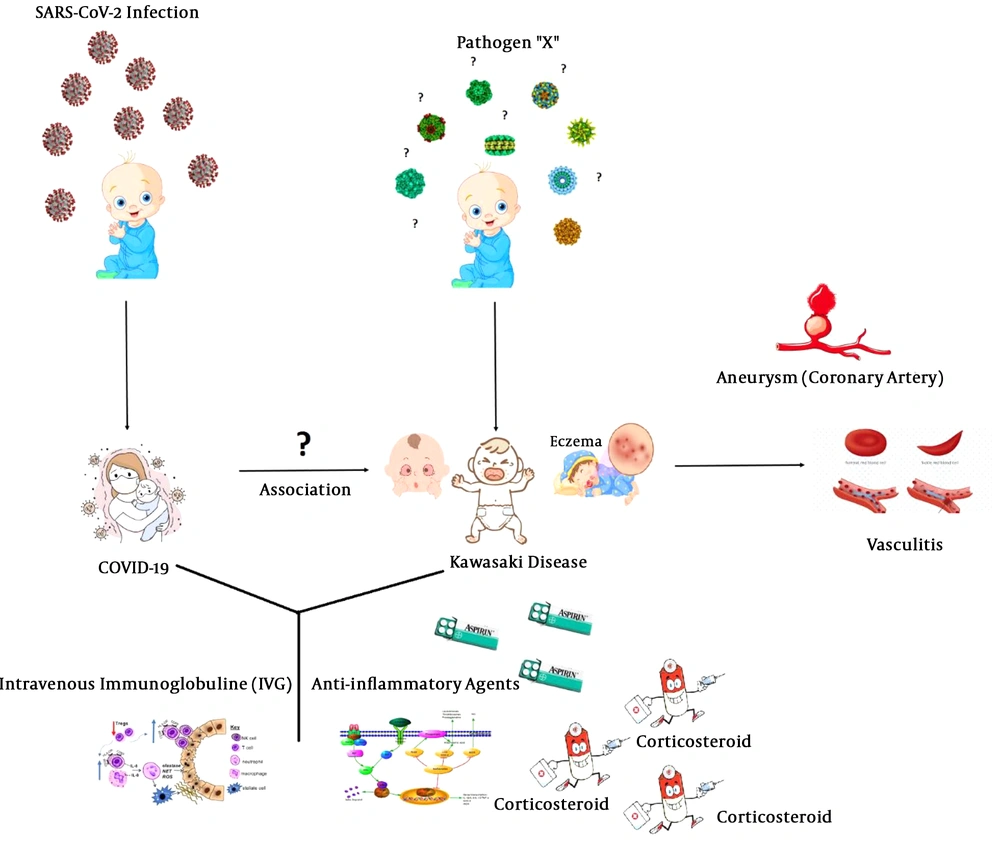
The possible link between KD and COVID-19 is unclear, but clinicians and experts have assured parents that the risk of developing COVID-19 in children with severe symptoms is low (Figure 1).
The Centers for Disease Control and Prevention (CDC) recently reported that children infected with COVID-19 had mild KD symptoms. COVID-19 cases are still low among children, and although a very low percentage of children and infants have COVID-19, adults still make up the majority of the cases. The current evidence suggests that most cases of COVID-19 in children who have been treated have mild KD symptoms; moreover, half of them had a fever, about 40% had a cough, and less than 10% had gastrointestinal symptoms.
Our knowledge of KD in children is limited. COVID-19 in adults as an inflammatory disease affects a number of organs in the body, but children with KD should be carefully screened for COVID-19. Kawasaki disease is very rare, just like COVID-19, which does not currently cause serious and complex complications in children, but it is important to be aware of any possible link between KD and COVID-19; therefore, immediate action can be taken if necessary. Countries with a higher prevalence of COVID-19 reported a higher number of children with KD of which some of these children had COVID-19, and some did not (6). It is not clear exactly what the relationship is between KD and COVID-19; however, researchers are investigating the cause of the sudden increase in the incidence of KD among children infected with COVID-19.
Nevertheless, we have to declare that it takes months for epidemiologists to tell us whether there is a link between KD and COVID-19. This is not a simple question at all, and it is a very complex subject. But at the same time, parents should keep in mind that any type of fever does not mean COVID-19, and due to the proximity of KD and COVID-19 symptoms, families should definitely send their child to a physician or medical center if they had such symptoms.