1. Background
Acute myocardial infarction (AMI) is a sudden and deadly cardiac disease as the leading cause of death and disability all over the globe (1). More than 100,000 deaths occur among the American population over the year (2). Every 30 minutes of delay to take treatment after AMI occurrence, the patient’s life is shortened by 1-year (3). One study showed that of all deaths related to AMI almost 80% occurred as outside of hospital due to delay medical care seeking (4). Despite a constant reduction in mortality during hospital admission, the out of hospital mortality remains high in AMI sufferers (5).
The AMI is a myocardial cell death due to prolonged ischemia (6). It can be divided into “ST-segment elevation myocardial infarction (STEMI)”, which causes higher short-term mortality and “non-ST segment elevation myocardial infarction (NSTEMI)” (7). The most important risk factors among patients with AMI are smoking, obesity, diabetes, hypertension, dyslipidemia, and family history of heart disease (8). Diagnostic criteria for AMI include the identification of rising or falling cardiac biomarkers, electrocardiogram (ECG) changes, and imaging evidence of new loss of cardiac muscles (8). The most common presentation of AMI is severe excruciating pain or discomfort in the chest along with other symptoms such as dyspnea, fatigue, diaphoresis, nausea or syncope and so forth (6). According to the European Society of Cardiology, delay in medical care seeking has been defined by the time between symptom onset and definite medical therapy in the emergency department of the hospital (9). Some studies showed that mean total delay in medical care seeking time to definitive therapy was 11.0 (SD = 9.8) hours. Delay in medical care seeking was divided into prehospital delay, which mean total time was 8.7 (SD = 9.7) hours in which 66% was patient-related and 34% was transportation-related reason and the other was hospital delay, which the mean total time was 2.3 (SD = 0.95) hours in which 89.8% was system related and 34% was staff-related reason (10). Some other researchers identified that increased age and female gender have a longer delay in care seeking (11, 12). Early medical services coverage is vital to reduce further sufferings and events to prevent death caused by myocardial damage. However, there is little knowledge associated with a delay in medical care seeking.
Likewise, other countries, cardiovascular disease (CVD) is a progressive reason for increased mortality and services burden in Bangladesh, a developing country with about 160 million of the population as a country experiencing epidemiological transition (13-17). However, the precise prevalence and risk factors of CVD is yet to be identified (13). A nationwide survey focusing on the epidemiological aspects of coronary artery diseases in this country is yet to be conducted (13). There is scare research to explore the risk factors and implement prevention strategies for premature deaths (16).
2. Objectives
Therefore, we aimed to identify the factors related to delay in seeking medical care among patients with AMI.
3. Methods
This descriptive cross-sectional study was conducted at the National Institute of Advanced Nursing Education and Research (NIANER) between January 2017 and June 2018. Data were collected from 120 patients with AMI from Ibrahim Cardiac Hospital and Research Institute, which is a tertiary level hospital in Dhaka with convenient sampling technique via face-to-face interviews with a semi-structured questionnaire and analyzed by Statistical Package for the Social Science (SPSS) version 22.0 software. Descriptive statistics were used to summarize socio-demographic characteristics, clinical characteristics, and factors towards delay in medical care seeking of patients with AMI. Associations between influencing factors and delay in medical care seeking were examined using independent sample t-tests. The level of significance was considered to be P < 0.05.
Study variables consisted of patients’ socio-demographic characteristics, clinical characteristics, delay in medical care seeking time, and factors related to delay in medical care seeking among patients with AMI. The socio-demographic characteristics were comprised of age, height, weight, dinnertime, exercise, monthly family income, sex, religion, living area, and marital status, level of education, job status, and smoking status. Clinical characteristics included the history of the familial heart disease, AMI symptoms, nature pain, duration of pain, pain radiation, other medical problem, frequency of hospital admission, and pain intensity. Medical care delay factors and time included misinterpreting the nature of the pain, symptoms did not consider to be serious, symptoms would go away, tried to manage by self-treatment with drug or rest, pain resistance behavior, fear of the disease consequences, financial problem, did not want to be a burden on others, lack of knowledge related to AMI, misinterpretation of symptoms by primary caregiver, misdiagnosis by primary caregiver, living in long distance from hospital, suitable transport/traffic jam, delayed physician arrival, delayed nurses arrival, delayed technician arrival, laboratory test, lack of equipment, lack of proper supply of medication, shortage of beds, holiday admission, delay in admission process, lack of teamwork, first incidence of heart attack symptoms, the time between the patient leave home after showing heart attack symptoms and the time comes to the emergency department at hospital, time to arrive in the emergency department, and time to get first treatment in the hospital.
4. Results
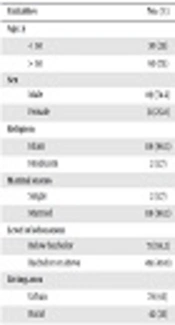
The current study aimed to unveil the factors responsible for delaying the care seeking in patients with AMI of Bangladesh. A total of 120 patients were interviewed to satisfy the study objective. The mean ± SD age of the respondents was 57.97 ± 10.76 years, the majority of the patients were male (74.2%), Muslim (98.3), and married (98.3%) (Table 1). In terms of education above half of the patients (59.2%) were below bachelor and less than half of patients (40.8%) were bachelor or above. About half of the patients (48.3%) were overweight or obese, did not take regular exercise (54.2%), and 45.8% were smoker (Table 1). Above one-third of the patients (37.5%) had family history of heart disease, majority of patients (94.2%) experienced heavy with other nature of pain, more than half of the respondents (55.8%) reached hospital after 6 hours, 77.5% of the patients had no radiation of pain, and 80% were admitted in the hospital for the first time (Table 1). The mean duration to leave home for the hospital after the appearance of symptoms of chest discomforts was 11.61 hours. About 77% of the patients reached the hospital within 6 hours, 18% within 6 - 12 hours, and 5% after 12 hours.
| Variables | No. (%) | Mean ± SD |
|---|---|---|
| Age, y | 57.97 ± 10.76 | |
| < 50 | 30 (25) | |
| > 50 | 90 (75) | |
| Sex | ||
| Male | 89 (74.2) | |
| Female | 31 (25.8) | |
| Religion | ||
| Islam | 118 (98.3) | |
| Hinduism | 2 (1.7) | |
| Marital status | ||
| Single | 2 (1.7) | |
| Married | 118 (98.3) | |
| Level of education | ||
| Below bachelor | 71 (59.2) | |
| Bachelor or above | 49 (40.8) | |
| Living area | ||
| Urban | 78 (65) | |
| Rural | 42 (35) | |
| BMI | 24.92 ± 3.80 | |
| Normal | 62 (51.7) | |
| Overweight | 58 (48.3) | |
| Exercise per week | ||
| No exercise | 65 (54.2) | |
| Exercise | 55 (45.8) | |
| Smoking status | ||
| Non-smoker | 65 (54.2) | |
| Smoker | 55 (45.8) | |
| Family history of heart disease | ||
| No | 75 (62.5) | |
| Yes | 45 (37.5) | |
| AMI symptoms | ||
| No chest pain | 7 (5.8) | |
| Chest pain with others | 113 (94.2) | |
| Nature of pain | ||
| No nature | 7 (5.8) | |
| Heavy with other | 113 (94.2) | |
| Duration of pain, h | 15.74 ± 13.85 | |
| < 6 | 53 (44.2) | |
| ≥ 6 | 67 (55.8) | |
| Radiation of pain | ||
| No radiation | 93 (77.5) | |
| Radiation | 27 (22.5) | |
| Related medical problem | ||
| Non DM | 28 (23.3) | |
| DM | 92 (76.7) | |
| Hospital admission | ||
| First time | 96 (80) | |
| Two or more | 24 (20) |
Abbreviations: AMI, acute myocardial infarction; BMI, body mass index.
The majority of delays was related to the patients per se (76.75%) due to misinterpreting the nature of pain, about 66% delayed because of they did not consider the symptoms to be serious, 65% of the patients were waiting to see for their symptoms would go away, about 86% tried to manage their sign-symptoms by self-treatment or rest (Table 2). However, a few patients (12.5%) delayed because of financial problem, about 76% of delays occurred due to the lack of knowledge related to AMI, about one-third (36.7%) of the patients were living long distance from hospital, about 48% lacked suitable transport, and 82% experienced traffic jam causing delay to seek medical care (Table 2).
| Variables | No. (%) |
|---|---|
| Misinterpreting the nature of pain | 92 (76.7) |
| Did not consider the symptoms serious | 79 (65.8) |
| Waited to see whether my symptoms would go away | 78 (65) |
| Tried to manage by self-treatment or rest | 103 (85.8) |
| Pain resistance behavior | 29 (24.2) |
| Fear of the disease consequences | 26 (21.7) |
| Financial problem | 15 (12.5) |
| Did not want to be a burden on others | 16 (13.3) |
| Lack of knowledge related to AMI | 93 (77.5) |
| Symptoms misinterpreted by first caregiver | 25 (20.8) |
| Misdiagnosis by primary caregiver | 26 (21.7) |
| Living in long distance from hospital | 44 (36.7) |
| Lack of suitable transport | 57 (47.5) |
| Traffic jam | 99 (82.5) |
Independent t-test was used to identify the relationship in gender, age, religion, marital status, education, job status, monthly family income, living area, body mass index (BMI), dinnertime, exercise, smoking status family history of heart disease, AMI symptoms, nature of pain, duration of pain, radiation of pain, related other medical problems, and the frequency of hospital admission. Patients who lived in a rural area showed significantly higher delay time to seek medical care (P = 0.01) than those who lived in an urban area. Moreover, the patients who suffered from pain less than 6 hours showed significantly higher delay time to seek medical care (P = 0.01) than those who suffered from pain for 6 hours or more (Table 3).
| Variables | Mean ± SD | t (P) |
|---|---|---|
| Gender | 0.72 (0.64) | |
| Male | 16.09 ± 13.84 | |
| Female | 14.72 ± 14.04 | |
| Age, y | 0.728 (0.49) | |
| < 50 | 17.33 ± 16.99 | |
| > 50 | 15.20 ± 12.70 | |
| Religion | -1.336 (0.41) | |
| Islam | 15.22 ± 13.04 | |
| Hindu | 46.00 ± 32.52 | |
| Marital status | 0.772 (0.44) | |
| Single | 23.25 ± 29.34 | |
| Married | 15.61 ± 15.61 | |
| Education | 1.115 (0.27) | |
| Below bachelor | 16.91 ± 15.16 | |
| Bachelor or above | 14.04 ± 14.04 | |
| Living area | -2.805 (0.01) | |
| Urban | 12.94 ± 11.37 | |
| Rural | 20.93 ± 16.47 | |
| BMI | 0.407 (0.68) | |
| Normal or less | 16.24 ± 12.37 | |
| Overweight or obese | 15.21 ± 17.37 | |
| Exercise | 0.848 (0.39) | |
| No exercise | 16.73 ± 13.85 | |
| Exercise | 14.57 ± 13.87 | |
| Smoking status | 0.848 (0.39) | |
| Non-smoker | 16.72 ± 13.85 | |
| Smoker | 14.57 ± 14.57 | |
| Family heart disease | -1.417 (0.64) | |
| No | 14.36 ± 12.75 | |
| Yes | 18.04 ± 15.39 | |
| AMI symptoms | 0.275 (0.78) | |
| No chest pain | 17.14 ± 13.26 | |
| Chest pain | 15.65 ± 13.94 | |
| Nature of pain | 0.275 (0.78) | |
| No heaviness | 17.14 ± 17.14 | |
| Heaviness | 15.65 ± 15.65 | |
| Duration of pain, h | 2.645 (0.01) | |
| < 6 | 19.41 ± 15.33 | |
| ≥ 6 | 12.84 ± 11.89 | |
| Radiation of pain | -2.443 (0.02) | |
| No radiation | 13.58 ± 10.89 | |
| Radiation | 23.20 ± 19.60 | |
| Medical problem | 1.167 (0.25) | |
| Non DM | 18.81 ± 16.72 | |
| DM | 14.81 ± 11.81 | |
| Hospital admission | 0.396 (0.69) | |
| First time | 15.99 ± 13.29 | |
| Two or more |
Independent t-test was used to identify the relationship in misinterpreting the nature of pain, symptoms were not serious, symptoms would go away, tried to manage by self-treatment with drug or rest, resistance behavior, fear of the disease consequences, financial problem, a burden on others, lack of knowledge related to AMI, misinterpretation of symptoms by primary caregiver, misdiagnosis by primary caregiver, living in long distance from hospital, lack of suitable transport and traffic jam. Among 14 factors, five showed a significant relationship with a delay in medical care seeking. The bivariate analysis predicted that the factors of self-treatment with drug or rest (P = 0.04), misinterpretation of symptoms by primary caregiver (0.04), living in long distance from hospital (P = 0.01), lack of suitable transport (0.045), and traffic jam (0.00) were significantly higher in relation to delay in medical care seeking (Table 4).
| Variables | Mean ± SD | t (P) |
|---|---|---|
| Misinterpreting the nature of pain | -0.802 (0.424) | |
| Yes | 13.90 ± 15.07 | |
| No | 16.30 ± 16.30 | |
| Did not consider the symptoms to be serious | -1.127 (0.262) | |
| Yes | 16.77 ± 13.90 | |
| No | 13.76 ± 13.70 | |
| Waited to see symptoms would going | 1.005 (0.317) | |
| Yes | 16.67 ± 13.95 | |
| No | 14.00 ± 13.65 | |
| Tried to manage by self-treatment or rest | -2.021 (0.046) | |
| Yes | 16.77 ± 14.13 | |
| No | 9.52 ± 10.27 | |
| Pain resistance behavior | -1.253 (0.213) | |
| Yes | 18.54 ± 14.84 | |
| No | 14.85 ± 13.49 | |
| Fear of the disease consequences | -0.331 (0.741) | |
| Yes | 16.54 ± 11.32 | |
| No | 15.52 ± 14.52 | |
| Financial problem | -0.667 (0.506) | |
| Yes | 17.98 ± 11.88 | |
| No | 15.42 ± 14.13 | |
| Did not want to be a burden on others | -0.042 (0.967) | |
| Yes | 15.88 ± 11.47 | |
| No | 15.72 ± 14.23 | |
| Lack of knowledge related to AMI | -0.595 (0.553) | |
| Yes | 16.15 ± 13.43 | |
| No | 14.34 ± 15.40 | |
| Symptoms misinterpreted by primary caregiver | 2.021 (0.046) | |
| Yes | 18.25 ± 10.96 | |
| No | 15.07 ± 14.50 | |
| Misdiagnosis by primary caregiver | 1.777 (0.078) | |
| Yes | 19.97 ± 14.03 | |
| No | 14.57 ± 13.64 | |
| Living in long distance from hospital | 2.908 (0.005) | |
| Yes | 20.90 ± 16.58 | |
| No | 12.75 ± 11.05 | |
| Lack of suitable transport | 2.025 (0.045) | |
| Yes | 18.34 ± 15.58 | |
| No | 13.34 ± 11.69 | |
| Traffic jam | 3.874 (0.000) | |
| Yes | 17.35 ± 14.24 | |
| No | 8.17 ± 8.64 |
5. Discussion
In AMI, the myocardial injury may happen after twenty minutes of ischemia (8). Reduction of the lag period to receive the treatment, as well as maximization of myocardial salvage, have been presented as a logistic challenge (8). Therefore, the current study evaluated the factors related to delay care seeking in the patients with AMI in a specialized hospital of Dhaka City. A total of 120 patients were interviewed, which the mean age of respondents was 57.97 years. Although adequate steps were ensured to include males and females equally, 74% of the respondents were male. This gender distribution is consistent with other studies, while fewer studies had a near equal distribution with respect to the sex of the respondents (18).
There was a significant difference among the patients with AMI, those having a longer delay in care seeking had a significantly longer duration of pain (Table 3). So as to manage the challenges, primary prevention initiatives such as informative sessions may be important issues for identifying the typical and atypical symptoms of AMI (1). It is also essential for nurses and other healthcare participants to emphasize the paybacks of early medical care for patients with AMI (1). High-risk individuals such as those having a past history of cardiac events along with active caregiver may be important preventive strategies highlighting the symptom identification and delay in medical care seeking (1).
The study showed that only 27.5% of patients with AMI arrived at the hospital in less than 6 hours after the onset of symptoms. In similar studies in Pakistan, revealed 36% of patients reached the medical care setting before 3 hours of symptom onset; in Iran, about 43% of patients arrived between 1 - 6 hours after the onset of symptoms (19). The mean delay in medical care seeking was 15.74 hours, which is more than the duration found in the GRACE study, where median delay in medical care seeking time was 4 hours in Brazil, 2.5 hours in Australia, 3 hours in Europe, and 2.7 hours in the United States (10). Beig et al. showed that the median medical care delay time was 250 minutes, whereas delay before hospitalization constituted about 83.8% of total medical care delay (3). The current study demonstrated most of the delay in medical care seeking was related to earlier events of deciding to provide the medical care services, which signifies the lack of awareness among the lay persons. The profile of patients who came early to the hospital (less than 6 hours) was quite similar to those who came late (more than 6 hours).
Multiple factors have been found to be associated with longer delay in medical care seeking in AMI sufferers, including lived in rural area (P = 0.01), longer duration of pain (P = 0.01), pain radiated to others parts of the body (P = 0.02), manage by self-treatment with drug or rest (0.04), misinterpretation of symptoms by primary caregiver (0.04), living in long distance from hospital (P = 0.00), lack of suitable transport (P = 0.04) and traffic jam (0.00), which is nearly similar to other observational studies (1, 6, 8, 10, 19, 20). The patients with AMI could measure the symptoms as a non-severe discomfort, moreover, gradual appearance and intermittent symptoms are related to a longer delay in care seeking (12). Fear of the disease consequence related to the presented symptoms could affect the care seeking delay (20).
Cross-sectional study design, relatively smaller sample size, study in a single urban hospital would hinder to generalize the study results. Future studies involving the larger sample size with involvement of community inhabiting patients is needed to get the real picture and improve the compliance status.
5.1. Conclusions
Delay in help-seeking imposes risk on cardiac status, which may rise the expenses due to staying in the hospitals and treatment of further complications. It is necessary to develop a strategy for reducing delay in medical care seeking in patients with AMI to reduce cardiovascular mortality and morbidity. There could be strategic awareness programs focusing on the identification of alarming symptoms of AMI. Raising awareness could help to lessen the delay time related to the patients before providing medical care. There is also a need to develop a strategy to provide emergency ambulance services and to set traffic rules to reduce time in roads and allow the patients to access hospital service rapidly.