1. Background
Dengue virus (DENV) is an RNA virus belonging to the family Flaviviridae of the genus Flavivirus. Globally, it has been estimated that 3.5 billion persons are at high risk of infection (1). Some patients have clear symptoms of the disease, while others remain asymptomatic. Dengue viruses are transmitted by one mosquito (Aedes aegypti), which causes the spread of dengue infection, as a viral infection transmitted by an infected suspect. The infection severely affects the white blood cells (WBC) and platelets. Under this infection, the cell count tends to be lower from the normal range and is associated with a high fever (2). Once the virus has infected an individual, the person develops dengue fever, referred to as "break-bone fever," given the severe pain in muscles and joints (3).
Dengue fever is caused by four closely related serotypes DENV (1-4), an emerging pandemic-prone viral disease in many regions of the world. Infection with one serotype does not guarantee infection by the others (2). Dengue fever is a leading cause of serious illness and death among children in some Asian countries, including Pakistan. During the last years, dengue fever developed into the hemorrhagic fever. Although Dengue virus has its four serotypes (1 to 4) and causes an almost similar infection, the serotypes (2 and 3) have more lethal effects, leading to dengue hemorrhagic effects (4-6). According to the literature, it is inferred that Dengue infection prevails in Asia, South America, and South Africa (7).
The annual identification of the dengue virus remains a keystone for the treatment of dengue fever (8, 9). It is noted that the dengue virus causes two types of infection (fever) (namely primary infection and secondary infection). The primary phase of the infection in a patient develops into an acute febrile infection known as dengue fever (DF). If the primary phase of infection remains untreated, then it develops into the secondary phase of the infection, which is more critical and severe than the primary phase of infection, leading to dengue hemorrhagic fever (DHF) and dengue shock syndrome (DSS) (10, 11). Signs and symptoms in DSS are high-grade fever, severe muscular pain, abdominal pain, and retro-orbital pain.
Clinically, leukopenia, thrombocytopenia, an increase in liver enzymes (AST and ALT), and a lower level of serum cholesterol and serum albumin have been reported in this regard (12). Non-structural protein 1 is a simple, easy, and quick method used in the acute phase of infection for the early detection of antigen (DEN virus) before consuming the antibodies (IgM, IgG) (12). The quantitative RT-PCR method is used for the detection of dengue virus serotyping. However, due to the limited sources available to the health care system, PCR is not accessible in remote areas. In a remote area where PCR facility is not available (13), health professionals mainly use platelets counter (thrombocytes) to detect the presence of dengue infection and cause of dengue fever (DHF and DSS) (14).
2. Objectives
Our study aimed to detect the effectiveness of haematological parameters (WBC’S, platelets, HCT), which are the early symptoms in dengue fever, along with its serological findings. This study was conducted to achieve an early diagnosis by analyzing the haematological parameters of serological patterns in the dengue virus and detecting the serotyping on a molecular basis.
3. Methods
3.1. Sample Collection
Blood samples were collected from dengue patients under 1 to 15 years by maintaining their history on a questionnaire. The participants were categorized into 4 groups: group A to D (A, 0 - 1-year; B, 1 - 5-year; C, 5 - 10 years; and D, 10 - 15 years of age). Patient fever history of one week was recorded by following the protocol according to WHO (2009) definition. Blood samples of patients were collected from those having the sign and symptoms of fever, headache, rash, vomiting, and having features of Thrombocytopenia, leucopenia, and increased hematocrits. 5 mL of samples of blood were collected in EDTA vials for hematology and chemical vacutainers. Three aliquots were made for non-structural protein 1 (NS1), chemical analysis, and quantitative RT-PCR.
3.2. Laboratory Investigation
One mL blood sample was collected and used to determine hematological parameters (namely hematocrits, leukocytes, and platelets) using a hematological analyzer (KX21 Sysmax). Serum aliquots were used to count liver enzymes using an instrument of a chemistry analyzer (AU680 Backman Coulter).
3.3. Non-structural Protein 1 Rapid ICT Based Diagnosis and Serotyping Analysis
The non-structural protein 1 test was carried out using the ICT (immune-chromatography) method as described by the manufacturer. The kit has a relatively high specificity of 95.9% and a sensitivity of 95.6%. Serotyping was done by using QRT-PCR. In QRT-PCR, to detect the DEN- DEN-V serotype, serum collected from infected patients has dengue sign and symptom. After the extraction process, RNA was transcribed into cDNA and amplified by PCR. Probes were labeled to amplify the DNA fragments. The analyzer monitors the amplification of DNA fragments and cycles.
3.4. RNA Extraction
According to the manufacturer's protocol, RNA extraction was done by the QIAamp DSP virus kit (QIAGEN, Valencia, CA). The kit is used for Dengue viral nucleic acid purification and isolation from whole blood. A concentration by 60 µL elute was extracted from 500 µL sample volume.
3.5. Polymerase Chain Reaction
To have serotyping, the researchers used the abTESTM DEN-4 qPCR Kit (AITbiotech Pte Ltd, Singapore), a multiplex real-time polymerase chain reaction kit for the simultaneous detection DENV-1 DENV-2, DENV-3, and DENV-4 in one reaction tube. The kit is specifically designed for four dengue serotypes using particular primer pairs and double dye hydrolysis probes, and it also included an internal control (IC) to check possible PCR inhibition. PCR was performed using the state-of-the-art CFX-96 real-time PCR machine (Bio-Rad laboratories Inc., USA). The following conditions were adjusted for the real-time plate-like Cy5 (DENV-1), FAM (DENV-2), Texas Red (DENV-3), Quaser 705 (DENV-4), and HEX (IC) (Tables 1 and 2).
| Serotype | Forward Primers | Reverse Primers |
|---|---|---|
| DENV-1 | 5´GGATCCAGGGGAAGTGGACAGCTT TTC3´ | 5´AAG CTTTGGTTAATGGTTTGC ATC CAA GAG A3´ |
| DENV-2 | 5´AACTCGAGAAAGAATGGATAGTGTTGCGTTGTGAG3´ | 5´AAGGTACCTTAGGCTGTGACAGGAGTTAC3´ |
| DENV-3 | 5´GGATCCATTACACTCTATCTGGGA3´ | 5´AAGCTTGTTGTCCATCTTTCCC3´ |
| DENV-4 | 5´GGATCCACATGGGTTGTGTGGTGTCAT3´ | 5´AAGCTTGCCGTCACCTGTGAT TTAAC3´ |
Sequence of Primers for Different Serotypes of Dengue Virus
| Phase | Description | No. of Cycles | Temperature | Duration |
|---|---|---|---|---|
| 1 | cDNA Synthesis | 1 | 53°C | 10 min |
| 2 | Taq activation | 1 | 95°C | 2 min and 30 sec |
| 3 | Amplification | 42 | 95°C | 17 sec |
| 59°C | 31 sec | |||
| 68°C | 32 sec |
PCR Amplification Conditions
3.6. Statistical Analysis
A chi-square test was used to evaluate the significance level. P < 0.05 was set as the level of statistical significance. Microsoft Excel and SPSS software were used for data analysis.
4. Results
4.1. Demographic Features
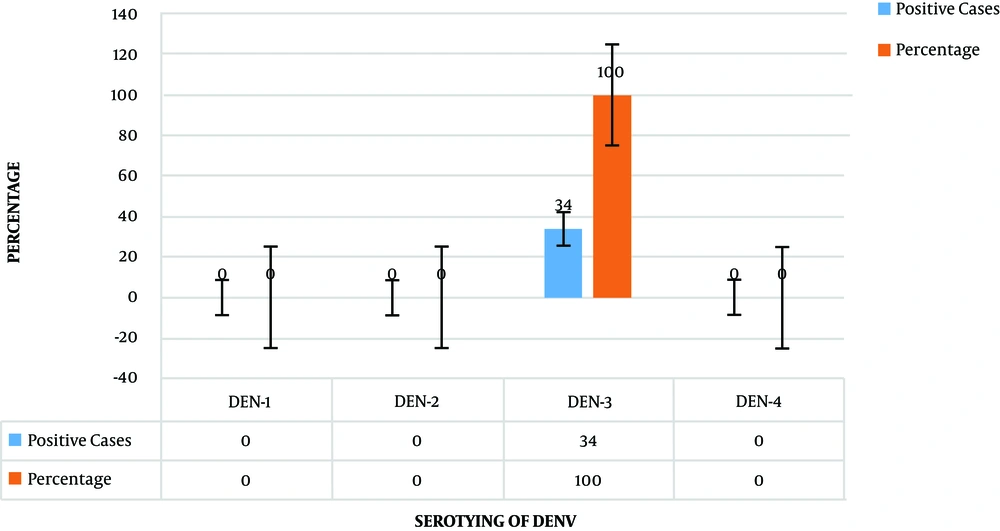
All 112 participants were analyzed, out of whom there were 34 cases with dengue (serotype-3) positive, and the 78 cases with dengue negative. The most predominant serotype was DEN-3, and there was no other type of dengue virus (1, 2, and 4) (Figure 1). Thus DEN-3 was the most frequent serotype identified in the sample of the suspects under study. Out of 112, 34 positive samples having DEN-3 serotype were confirmed by QRT-PCR. The ratio of DEN-3 serotype was more in boys than in girls. Out of 34 positive cases, 24 persons were males, and 10 participants were females (P < 0.05). The participants’ mean age range was 10 - 15 years. The above table shows gender-wise distribution of dengue fever in patients (Table 3). The highest percentage was observed in 34 males (70%) versus 10 females (29%) (P < 0.05).
| Group I.D | Age (y) | Boys | Girls | Total Cases |
|---|---|---|---|---|
| A | 0 - 1 | - | - | - |
| B | 1 - 5 | - | - | - |
| C | 5 - 10 | 01 | 02 | 03 |
| D | 10 - 15 | 23 | 08 | 31 |
| Total | 24 | 10 | 34 | |
Distribution by Dengue Patients’ Age and Gender (n-34)
4.2. Clinical Profile
Considering the questionnaires and given the history of patients, data were collected from 112 dengue-suspected patients based on the signs and symptoms of dengue fever. Among the symptoms, the history of fever was the most common (100%) clinical symptom in all the patients. Other clinical features were headache (100%), nausea (64.2%), body pain (82.1%), arthralgia (100%), severe abdominal pain (80.3%), and urinary output (98.2%) (Table 4). A smaller number of clinical features such as rash, retro-orbital pain were observed. No mortality was reported in the participants.
| Sign and Symptoms | No. (%) |
|---|---|
| Fever | 112 (100) |
| Nausea | 72 (64.2) |
| Rash | 30 (26.8) |
| Headache | 112 (100) |
| Body aches (pain) | 92 (82.1) |
| Retro-orbital pain | 34 (30.3) |
| Arthralgia | 112 (100) |
| Severe abdominal pain | 90 (80.3) |
| Decrease urinary output | 110 (98.2) |
Participants’ Clinical Symptoms (n-112)
4.3. Laboratory Profile
4.3.1. Hematological and Clinical Chemistry Profile
The abnormalities in hematological and clinical chemistry were noted. According to the hematological abnormalities, leucopenia and Thrombocytopenia were the most common cases. Chemistry-related clinical parameters indicate the elevated level of liver enzymes (ALT & AST) and the low level of serum cholesterol and serum albumin (Table 5). In dengue positive cases, the Leukopenia (low WBC’S) < 4.0 × 103 was observed in 27 (79.4%) patients; however, > 4.0 × 103 was noticed in 16 (20.5%) patients who were negative dengue. Similarly, Thrombocytopenia (low platelets) was < 100 mm3 in 24 (70.5%) dengue positive cases, and > 100 mm3 was observed in 26 (33.3%) dengue negative cases. A raise in HCT was observed in 14 (41.17%) patients. Liver enzymes, both ALT and AST, were also found raised in 88 and 79% of dengue positive patients.
| Laboratory Parameters | Normal Range | Remarks |
|---|---|---|
| Leukocyte count × 103 | 4.0 - 11.0 | > 4.0 No. (%) = 07 (20.5); < 4.0 No. (%) = 27 (79.4) |
| Thrombocytes/mm3 | 150 - 450 | > 100 No. (%) = 10 (29.4); < 100 No. (%) = 24 (70.5) |
| Hematocrit % (HCT %) | 36 - 45 | > 40 No. (%) = 14 (41.1; < 40 No. (%) = 20 (58.8) |
| Alanine amino-transferase (ALT), u/L | Up to 40 | > 40 No. (%) = 30 (88.2); < 40 No. (%) = 04 (11.7) |
| Aspartate amino-transferase (AST), u/L | Up to 40 | > 40 No. (%) = 27 (79.4); < 40 No. (%) = 07 (20.5) |
| Serum albumin, g/dL | 3.5 - 5.5 | > 3.5 No. (%) = 09 (26.4); < 3.5 No. (%) = 25 (73.5) |
| Serum cholesterol, mg/dL | 150 - 200 | > 150 No. (%) = 24 (70.5); < 150 No. (%) = 10 (29.4) |
Clinical and Hematological Abnormality Profile in Dengue Patients
5. Discussion
Dengue fever has suddenly increased in Pakistan from 1994 - 2011. Dengue fever was first reported in 1982 in Pakistan among 174 samples undergoing the clinical trial, out of whom 12 cases were positive dengue fever (15, 16). In Karachi, dengue infection types 2 and 3 were reported during 2005 - 2006, and a dengue outbreak was also reported with a similar serotype in 2008 in Lahore. According to the previous studies, March - April and July - October are the peak months of the dengue incidence (17). Due to the progressive existence of the dengue virus in economic countries, it has converted into a significant epidemic threat (1). Due to the specific genetic makeup of virus, vector control is one of the best options to treat and manage dengue cases. However, community participation is an important factor for successful vector conventional techniques (18), is available to treat Dengue infection (fever). In clinical diagnoses, Fever history of fewer than two weeks, morbilliform rash, severe headache, nausea, vomiting, and body pain are the main symptoms of dengue fever. Similar clinical signs have been observed in the present study on children aged below 15 years.
Non-structural protein 1antigen detection is the early marker to diagnose dengue fever from blood samples during the first week of infection. Non-structural protein 1antigen in patients suffering from severe dengue fever could be identified during the first three days of DHF infection (19). IgM response developed seven days post-infection and remained 2 - 3 months as such it is known as an early diagnostic markers in the acute phase of illness (20). According to the findings of the present study, the NS1 antigen-based detection was more proficient and appropriate marker to be used in the early and acute phases (21). DENV-3 was the leading serotype in Dehli, India, with a high rate of dengue infection in male patients, compared to females in the age group of 20 - 30 years. This study is consistent with the present study; however, the patients in our study were children aged below 15 years. Another study reported the high prevalence of this disease in patients aged 21 - 30 years, while few children were found to be infected (14). Due to an insufficient carrier control program, the dengue virus has spread worldwide since 1960. It is observed that a considerable increase in population growth, lack of knowledge, and traveling from one place to another place were the main factors to propagate the dengue virus among a population (22).
According to our findings, 11 out of 34 cases had low levels of thrombocytes. This may be due to bone marrow suppression in the acute phase of dengue virus infection and defects in megakaryocytes, leading to platelet destruction (23). Consistent with the other reports (24), leucopenia was observed during three to four days of post-infection by the dengue virus. Leukocytopenia was the primary outcome of dengue, causing damage to the myeloid series of WBC and also bone marrow suppression (23). Low white blood cells were the key in the early dengue diagnosis. Infected mosquito’s bite signs usually last for two to seven days, following incubations for 4 - 10 days (25, 26). Moreover, 10105 (78.6%) persons were suspected during the last five years, suggesting that severe dengue is a life-threatening complication causing plasma leak and fluid accumulation, respiratory distress, severe bleeding, or impairment (27). The alert symptoms appear in conjunction with the temperature decay (< 38°C/100°F) 3 - 7 days after the emergence of early symptoms, including extreme abdominal discomfort, constant shaking, fast coughing, gum bleeding, exhaustion, restlessness, and blood vomiting (28).
In this study, 12611 participants reported dengue fever within the last five years. Concerning DF, most of the respondents ranked DF as dangerous to very dangerous (29). The early DF symptoms mostly described by the respondents were fever for more than 3 - 4 days (76.6%) and headache and knee pain (43.7%). Some of the participants indicated that their early DF signs included fever for two days (85.5%) and fatigue and particular pains (55.5%) (29). In a previous study, 17 (0.1%) and 9 (1%) participants were diagnosed with DHF and DSS, respectively (30). In another study estimating dengue prevalence, 3.9 individuals were at risk of infection by the dengue virus. In one hundred twenty-nine countries at risk of infection, Asia accounts for 70% of the actual burden. The number of dengue cases reported to WHO increased over 15 fold during the last 20 years. In 2000 a total of 505,430 cases, 2,400,138 cases in 2010 and 3,312,040 cases in 2015 were reported (31). Like Mexico, the United States, Bangladesh, India, Thailand, and Indonesia, the rising prevalence of dengue was also observed in Pakistan. These findings led researchers to develop and conduct spatial analyses on dengue cases (32).
Dengue virus directly harms the liver, leading to liver necrosis and an increase in liver enzymes (33). Accordingly, DENV-3 is the most repeated serotype of dengue in Lahore, Pakistan, identified by quantitative real-time PCR. The highest percentage of dengue was noticed among the participants aged 11 - 15 years, and the dengue was more prevalent in male patients than females. The most common clinical symptoms in the DENV-3 serotype are fever, nausea, skin rash, body aches with thrombocytopenia, raised hematocrit, and increased liver enzymes (ALT & AST). Low levels of cholesterol and serum albumin were also observed in the dengue patients.
5.1. Conclusions
This study could facilitate understanding the current scenario of the DENV-3 serotypes in children and may provide the grounds for future epidemiological studies at a large scale. Like other lethal infections such as COVID-19 (34, 35), public awareness of dengue is also necessary to stop or minimize its spread. It is necessary to adopt precautionary measures to control the dengue infection in our population.