1. Introduction
Treatment for injuries to the oral region is common and accounts for 5% of all injuries (1). The prevalence of dental injuries within permanent dentition has been shown to occur in approximately 10 - 35% of the general population worldwide (2). Children between 8 and 10 years are more affected by permanent dentition, and the most ordinarily impacted teeth are the maxillary central incisors (3).
Crown fractures and luxations occur in most dental injuries, ranging from 15 to 61%. Therefore, an acceptable treatment for an injury is essential for a decent prognosis (1). An extrusion injury occurs after trauma when the tooth is displaced in the axial direction from its socket and could be considered a partial avulsion. According to reports, extrusion injuries account for about 3% of all traumatic injuries to dentition (4). Pulp necrosis is a frequent complication in teeth with extrusion or lateral luxation injuries (5). A subluxation injury is characterized by abnormal loosening of the tooth-supporting structures without tooth displacement. The etiology of the subluxation may be the result of a minor impact on the force unit, where the energy discharged leads to bleeding, edema, and tearing of PDL fibers resulting in abnormal loosening (6). A study showed pulp necrosis was relatively rare, especially when the teeth were immature (5).
Uncomplicated crown fractures are predominant in permanent dentition and often occur when a perpendicular or oblique force is applied to the tooth's incisal edge (7). Lower lip teeth fragments constantly move due to contractions of the orbicular musculature at the time of trauma, which can make identifying such cases challenging. Fractured incisors are typically the explanation for soft tissue lacerations during trauma. For this reason, special care should be taken for lacerations with fractured or missing teeth (8).
Some sequelae can occur following traumatized teeth, such as pulp necrosis, pulp cavity obliteration, and root and bone resorption. Many factors influence these complications, which may occur weeks, months, or years after the trauma (9).
2. Case Presentation
A 10-year-old female was referred to the pediatric department of the dental school of Hamadan University of Medical Sciences, Iran, nearly 48 hours after a sports accident and injury in her chin. At age five, a laceration of the lower lip and intrusion of the maxillary primary central incisors were experienced, but no other medical history was reported. In addition, the patient was vaccinated against tetanus.
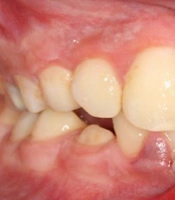
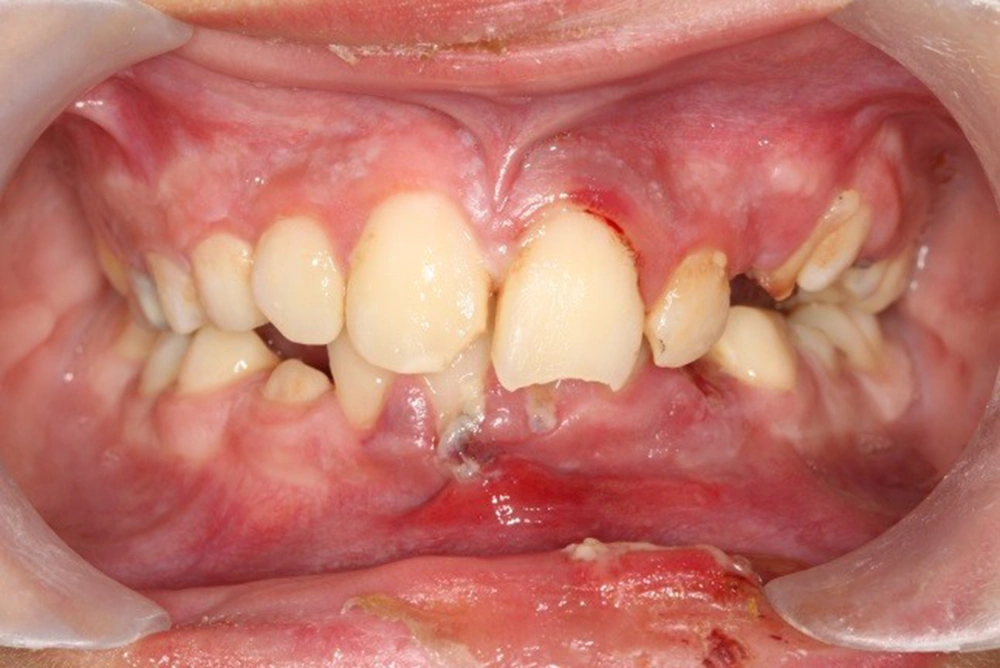
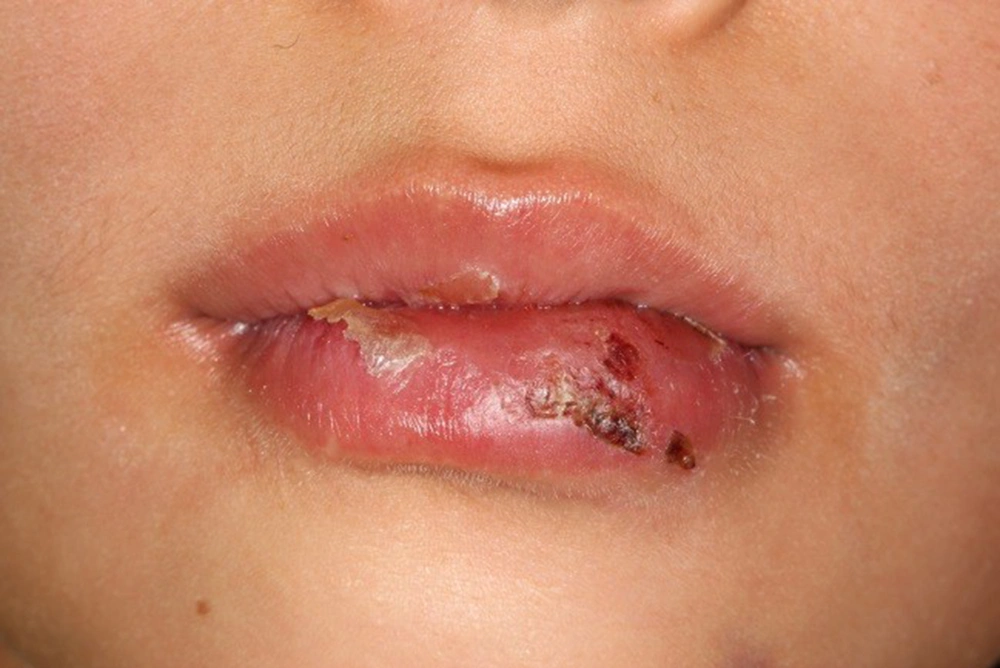
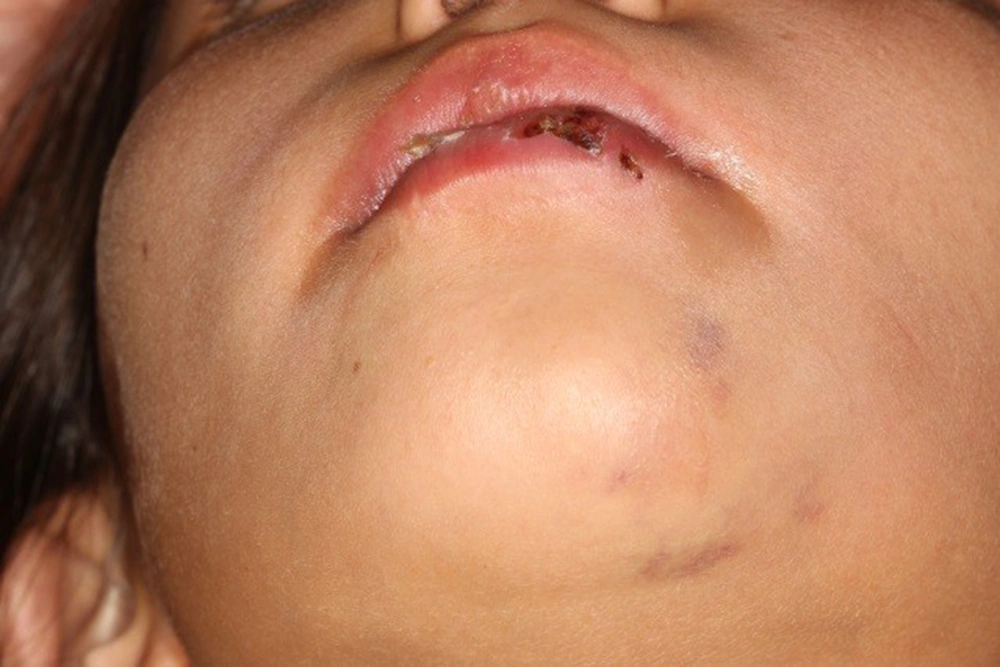
The clinical examination determined the extrusion and enamel-dentin fracture of tooth 11 (numbers of this article are being mentioned in the FDI system), extrusion and enamel fracture of tooth 21, and subluxation of teeth 12, 22, 31, 32, 41, and 42, socket wall fracture of the anterior segment of the mandible, laceration of the inferior lip with embedded fragments of teeth, and gingival tissue injury of the mandible (Figures 1-3).
The periapical radiographic examination did not show root fractures or any other injuries involving other teeth. The lateral root dilaceration of tooth 11 was seen because of past trauma history at age 5.
The surgical procedure included repositioning the teeth and bone fragments with finger pressure under local anesthesia. Two periapical radiographs were taken to ensure that the teeth were adequately positioned within the socket. A semi-rigid, wire-composite splint using a 0.7 mm stainless steel wire was applied from the primary right canine to the immediate left first premolar in the maxilla and from the first right permanent premolar to the first left primary molar in the mandible. The occlusion of opposite teeth in the anterior portion of the jaws prevented its removal after splinting. The parents were reminded about the necessity of maintaining optimal oral hygiene and regular visits for clinical and radiographic examinations.
The lower lip was incised from the mucosal side, and the fragments were explored and carefully removed. A 4-0 nylon thread was used to suture the tissue. During the surgery, a periapical radiograph (with ¼ dosage) was taken to confirm the complete removal of the fragments. Clinical treatment included antibiotic (Cap Amoxicillin 250 mg, three times a day) and anti-inflammatory (Tab Ibuprofen 400 mg, four times a day) agents.
The patient was told to brush meticulously with a soft toothbrush and rinse with chlorhexidine gluconate mouthwash for two weeks.
The maxillary left central incisor was treated with calcium hydroxide paste two weeks after the first visit and was completed a month later.
Three weeks after the first visit, the maxillary dental splint was removed during the third visit. However, the dental splint in the mandible was maintained for one month. The appropriate composite restoration was done for the maxillary central incisor during that visit since its crown fractured.
Periapical radiographs of maxillary and mandibular anterior teeth were taken every visit, and their normal condition was evaluated.
3. Discussion
The 10-year-old girl in this case report had a complex trauma involving dentoalveolar structures and soft tissues caused by a sports accident. Time elapsed since injury can have an impact on treatment selection. According to Andreasen et al., repositioning teeth is more difficult after 48 hours of damage. For the present case, repositioning was performed around 48 hours after the injury. Thus, treatment was doable and had satisfactory results (10). Therefore, tooth fragments in the lower lip should be evaluated with radiography. The presence or absence of a foreign body must always be determined by taking an X-ray of any tissues showing signs of bleeding, swelling, or laceration. A lip surgery appointment was scheduled after a radiographic examination of lower lip tooth fragments revealed a scar on her lip.
Periodontal ligament therapy requires a splinting period of 2 - 4 weeks, but in cases of low periodontal support or marginal bone breakdown, a splinting extension to eight weeks may be appropriate (3). In the present case, the maxillary splint was removed after three weeks, but the splint of the mandible was released after four weeks. Stabilizing traumatically displaced teeth with orthodontic wire and composite resin, as performed in the present case, has provided satisfactory results because it permits physiological movements and easy cleaning.
Variable analyses have shown that the stage of root development and type of luxation is the most critical factors affecting pulp healing in teeth with luxation injury. However, pulp healing critically consists of the absence of bacteria (11). Injuries to the dentition caused by extrusive luxation make up nearly 2.6% of all traumatic injuries, with pulpal necrosis being the most common consequence, which is more frequent in mature teeth than with open apices (12). In the present case, the luxation injury was severe (extrusion), root development was completed, and the concomitant crown fracture was observed. Consequently, pulp healing is expected to be problematic. Two weeks later, pulp necrosis and periapical lesions necessitate an endodontic treatment with Ca(OH)2 for the upper left central incisor. After one month, the endodontic treatment was completed by obturation root canal with gutta-percha.
There is some doubt concerning etiologic factors inflicting pulp necrosis in the upper right primary central incisor tooth with dilaceration. Katz-Sagi et al. (13) found uncommon canal obliteration after trauma to their associated primary teeth. The dilacerated tooth was healthy, despite the research, and showed no signs of necrosis. Dental trauma that affects a 4-year-old child could cause root dilacerations due to the permanent upper central incisor crown in the final stage of formation and starting the root development process (Nölla’s stage six) (14). In this case, the girl suffered a traumatic injury at the age of five that caused damage to the upper right primary central incisor, resulting in lateral root dilaceration of the permanent one.
Approximately 3% of permanent teeth are dilacerated due to intrusion or avulsion of their primary predecessors, most frequently the maxillary or mandibular central incisors. Maxillary incisors are more often involved compared to their mandibular counterparts. The highest rate of dilaceration prevalence is found in maxillary incisors (52%) and the mandibular third molar (12.8%) (15).
Approximately 50% of teeth with dilaceration become impacted commonly or in the wrong labiolingual direction. In the present case, the dilacerated tooth was found in the correct position in her mouth.
3.1. Conclusions
In the present case, clinical and radiographic analysis disclosed that the incisors presented reasonable esthetic and functional demands. Long-term clinical and radiographic follow-up is essential for the prognosis of the trauma. Maintenance of the tooth after traumatic episodes directly affects the patient's quality of life, restoring psychological and emotional states.