1. Background
Hemorrhoids are a common condition in the anorectal region, yet determining their true incidence is challenging due to the nonspecific nature of symptoms and the sensitive location, which often leads to patient embarrassment and hesitation in seeking treatment (1-3). This delay in seeking care is particularly problematic because patients frequently only seek examination and treatment when the symptoms and complications begin to severely impact their daily activities and work (4-6). Hemorrhoid symptoms are often nonspecific, leading to wide variations in reported prevalence rates in the absence of confirmatory anal examinations (1, 7). Globally, the incidence of hemorrhoidal disease ranges between 4.4% and 16.5% of the population (1, 2, 4), affecting both genders with an age range of 33 to 57 years (8).
In Vietnam, hemorrhoids are a significant health problem, accounting for 58.5% of anorectal diseases (9). A study in Ho Chi Minh City that included people over 50 years old showed a prevalence of 25.13% (10). In recent years, the University Medical Center Ho Chi Minh City (UMC HCMC) recorded about 35,000 cases of anorectal disease, with hemorrhoids accounting for more than half of these cases. Furthermore, UMC HCMC has conducted more than 3,000 hemorrhoidectomy surgeries, with the stapled hemorrhoidectomy method being the choice for more than half of these cases. Although not life-threatening in nature, hemorrhoids significantly affect the patient's quality of life (11).
Regarding treatment outcomes, assessments now frequently include evaluations of quality of life. Post-surgery quality of life typically drops by 10% immediately following the procedure but sees a rapid improvement of 60% within a week and reaches 80% within a month, highlighting the dynamic nature of recovery and the critical need for ongoing monitoring (12). However, in Vietnam, there is a remarkable lack of focused studies on the quality of life before and after hemorrhoid surgery, leading to this study's critical research question: How does surgical intervention for hemorrhoids affect the quality of life and specific health dimensions of patients in Vietnam, both immediately and over the weeks following surgery?
2. Objectives
This study aims to fill the existing research gap by providing comprehensive data on the impacts of hemorrhoid surgery on patients' quality of life. This information will inform medical professionals and aid in planning for post-treatment support, thereby improving patient outcomes in a context where such considerations are often overlooked in medical research and practice.
3. Methods
3.1. Study Settings and Design
A before-and-after study was conducted in the Proctology Department at the University Medical Center Ho Chi Minh City (UMC HCMC), Vietnam, from February 2023 to February 2024. This design aimed to evaluate the direct effects of hemorrhoid surgery on patient quality of life by comparing pre- and post-operative outcomes within the same subjects.
3.2. Participants, Sample Size and Sampling
Eligibility criteria included individuals aged 18 years and older presenting with hemorrhoids as their chief complaint. Participants could be newly diagnosed or have a prior diagnosis but must not have received any invasive treatments within six months prior to study enrollment to ensure no recent interventions influenced the outcomes. The study excluded patients with mental illness, cognitive disorders, or aphasia affecting communication abilities, those who had undergone other surgical procedures within the last six months, were pregnant, or declined to participate. This was to ensure a homogeneous study population reflective of typical clinical outcomes for hemorrhoid surgery.
The sample size was calculated using a formula to estimate a mean with σ = 13.11 as the standard deviation of the quality of life score of hemorrhoid patients according to a pilot study, d = 1.73, and Z(1-α/2) = 1.96. The calculated sample size was n = 246. Consecutive sampling was used to select all hemorrhoid patients who met the sampling criteria during the study period.
3.3. Data Collection and Tools
Study participants were interviewed face-to-face using the HEMO-FISS-QoL (HF-QoL) questionnaire, which assesses the hemorrhoid-specific quality of life (QoL) of patients. The HF-QoL scores correlated well with those of the SF-12 and PGWBI (P < 0.001), indicating strong validity. Cronbach’s coefficients (> 0.7) reflected good internal reliability across the different dimensions (13). A pilot study conducted on 30 patients before hemorrhoid surgery at the Proctology Department at UMC HCMC showed that the questionnaire's reliability, as measured by Cronbach's Alpha, was 0.92 overall. The consistency coefficients for each component were as follows: Physical disorder (0.90), psychology (0.77), defecation (0.88), and sexuality (0.86).
The questionnaire was administered by interviewers in the patient's room before surgery and re-administered eight weeks post-surgery during the follow-up examination at the Clinic of the Proctology Department. If a patient did not attend the follow-up examination at the time of sample collection, the researcher contacted and interviewed the patient using the HF-QoL questionnaire via phone call. Data were collected through face-to-face interviews and by reviewing patient medical records.
Information collected included patient characteristics such as age, gender, ethnicity, education level, occupation, marital status, residence, religion, monthly income, comorbidities, surgical method, previous treatment of hemorrhoids, and duration of the disease (see Appendix In Supplementary File).
The HF-QoL questionnaire assesses the patient's quality of life (QoL) using 23 items across four domains: Physical disorders (11 items), psychology (7 items), defecation (3 items), and sexuality (2 items). Responses are given on a 5-point Likert scale: 1 = never, 2 = rarely, 3 = regularly, 4 = very often, and 5 = always. If fewer than 50% of the items are missing, scores are calculated for each dimension (items marked as "not applicable" are not considered missing data). If 50% or more of the items in a dimension are missing, a score cannot be calculated for that dimension.
For calculable scores (when fewer than 50% of items are missing), the score for each dimension is the sum of the scores for all answers in that dimension. Specific rules apply for calculating the score if there are any missing data:
(1) First rule: If a dimension contains items with scores ranging from 1 to 5 ("never" to "always"), the "not applicable" items and missing data are replaced with the mean score of the patient-completed items with scores ranging from 1 to 5 in the same dimension (13).
(2) Second rule: If a dimension has zero items scored from 1 to 5 (i.e., only "not applicable" items or both "not applicable" and missing items), the dimension score is substituted with the mean score of the study population for that dimension (13).
Therefore, a score is calculated for each dimension provided fewer than 50% of the items are missing (“not applicable” answers are counted as not missing). The score for each dimension is the sum of the items scored in that dimension. The overall QoL score is calculated if the scores of the four dimensions can be calculated independently (the overall score is not calculated if one dimension score is missing). The overall QoL score is the sum of the scores of all the answers. A lower QoL score reflects a higher QoL.
3.4. Statistical Analysis
The research data were entered using Excel software and analyzed using IBM SPSS Statistics for Windows, Version 26.0. We used frequency and percentage to describe participants’ characteristics and mean and standard deviation to describe the age, duration of the disease, and outcome variables. The Wilcoxon rank sum test was used to determine the association between the patient's QoL and each dimension's score after hemorrhoid surgery. Statistical significance was set at P < 0.05.
4. Results
There were a total of 255 hemorrhoid patients. However, four did not meet the inclusion criteria due to reasons such as accompanying gallbladder surgery or being underage, and five patients refused to participate. Consequently, the study results are based on 246 patients who completed the study.
4.1. Characteristics of Study Participants
As shown in Table 1, the study participants had a mean age of 42.80 ± 14.22 years, ranging from 19 to 93 years. The most represented age group was 30 to 39 years, accounting for 29.3% of the participants. A majority of the participants were female (54.9%), about 10% more than the male participants, and 96.7% were of the Kinh ethnic group. Nearly 50% of the participants had attained an intermediate level of education or higher, including college, university, and postgraduate degrees. The participants had diverse occupational backgrounds, with the largest group being 'Other'—including housewives, retirees, and freelancers—comprising 30.1%, followed by officers at approximately 5%. Most participants were married or living with a spouse or partner, representing more than two-thirds of the total. Additionally, about two-thirds resided in urban areas. Over 50% of the participants reported having no religious affiliation, and the most common income bracket was 6 - 10 million VND, representing 33.3% of participants, with the lowest income group (21 - 25 million VND) accounting for 4.9%.
| Characteristics | No. (%) |
|---|---|
| Gender | |
| Male | 111 (45.1) |
| Female | 135 (54.9) |
| Ethnicity | |
| Kinh | 238 (96.7) |
| Others | 8 (3.3) |
| Education level | |
| Under-primary | 0 (0) |
| Primary | 17 (6.9) |
| Junior high school | 49 (19.9) |
| High school | 63 (25.6) |
| Professional intermediate/college/university/postgraduate | 117 (47.6) |
| Occupation | |
| Pupils/students | 7 (2.8) |
| Healthcare workers | 8 (3.3) |
| Officers | 61 (24.8) |
| Workers/farmers | 45 (18.3) |
| Business/commerce | 51 (20.7) |
| Others | 74 (30.1) |
| Marital status | |
| Single | 54 (22.0) |
| Married/living with a spouse or partner | 181 (73.6) |
| Separated/divorced/widowed | 11 (4.5) |
| Residence | |
| Urban | 163 (66.3) |
| Rural | 83 (33.7) |
| Monthly income, (million VND) | |
| ≤ 5 | 55 (22.4) |
| 6 - 10 | 82 (33.3) |
| 11 - 15 | 34 (13.8) |
| 16 - 20 | 35 (14.2) |
| 21 - 25 | 12 (4.9) |
| > 25 | 28 (11.4) |
| Age, (y) | |
| Mean ± SD | 42,80 ± 14,22 |
| Maximum-minimum value | 19 - 93 |
| 18 - 29 | 49 (19.9) |
| 30 - 39 | 72 (29.3) |
| 40 - 49 | 47 (19.1) |
| 50 - 59 | 38 (15.4) |
| ≥ 60 | 40 (16.3) |
| Religion | |
| No religion | 145 (58.9) |
| Buddhism | 63 (25.6) |
| Others | 38 (15.4) |
| Comorbidities | |
| No | 177 (72.0) |
| Hypertension | 39 (15.9) |
| Diabetes | 9 (3.7) |
| Hypertension and diabetes | 7 (2.8) |
| Others | 28 (11.4) |
| Surgical method | |
| Stapled hemorrhoidopexy | 84 (34.1) |
| Hemorrhoidectomy | 162 (65.9) |
| Previous treatment of hemorrhoids | |
| No | 137 (55.7) |
| Yes | 109 (44.3) |
| Duration of disease, (y) | |
| Mean ± SD | 7.24 ± 8.24 |
| Maximum-minimum value | < 1 - 51 |
| ≤ 1 | 69 (28.0) |
| 2 - 5 | 73 (29.7) |
| 6 - 10 | 55 (22.4) |
| > 10 | 49 (19.9) |
Table 1 also revealed that over two-thirds of the study participants did not have comorbidities. Among those with comorbidities, hypertension was the most common (15.9%), followed by other diseases (11.4%) and diabetes (3.7%). Additionally, a small percentage of subjects had both hypertension and diabetes (2.8%). Regarding surgical procedures, two-thirds of the surgeries performed were hemorrhoidectomies, and one-third were stapled hemorrhoidopexies. Of the 246 patients undergoing surgery, two-thirds had only the hemorrhoid surgery without any accompanying procedures. One-third of the patients underwent additional procedures, with treatments for skin tags being the most common (17.9%), followed by polypectomy (12.6%) and surgery to treat anal fissures (9.8%). Among these, 30.5% of the patients had one additional surgery, and 4.9% had two. The median duration of the disease was four years (quartile interval 1-10 years), with durations ranging from less than one year to a maximum of 51 years. The largest duration group, two to five years, comprised 28.7% of the patients, followed by one year or less at 28.0%, and more than ten years at 19.9%. Notably, 55.7% of the study subjects had not received previous treatment for hemorrhoids.
4.2. Health-related Quality of Life Scores
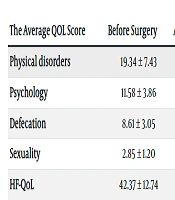
There was a statistically significant improvement in the patients’ mean Quality of Life (QoL) scores, which decreased from 42.37 ± 12.74 before surgery to 23.54 ± 2.19 eight weeks after surgery. The improvements in QoL dimensions were particularly notable post-surgery, especially in the defecation dimension, which saw the most significant reduction. The smallest change was observed in the sexuality dimension. The differences were statistically significant with a P-value of < 0.001, as detailed in Table 2.
a Values are expressed as Mean ± SD.
b Wilcoxon Signed Rank test.
5. Discussion
This study was conducted at the University Medical Center Ho Chi Minh City (UMC), a tertiary university hospital, to assess the quality of life of patients with hemorrhoids before and after surgery. It included 246 subjects with a mean age of 42.80 ± 14.22 years, ranging from 19 to 93 years old. This age range is comparable to those reported in other studies, such as 45.4 ± 13.4 years in Ho Chi Minh City, Vietnam (14), 44.1 ± 3.2 years in Saudi Arabia (15), and 44.3 ± 13.71 years in India (16), with China reporting a slightly younger range of 40 - 42 years (17). In contrast, other studies noted older age groups, including 46 ± 24 years in Nghe An, Vietnam (18), 48 years in Italy (19), and 55 years in Sweden (20). Additional studies by Abramowitz et al. (46.2 ± 13.9 years) (13), Ayari et al. (46.8 ± 10.9 years) (21), and others in Italy (53.1 ± 15.9 years) (22) and Sri Lanka (47.7 ± 14.3 years) (23) also noted older age groups. These findings suggest a trend of younger hemorrhoid patients compared to the largest epidemiological study from 1990, which documented ages ranging from 45 to 65 years (4). This change may indicate a shift in either the onset age or detection rates of hemorrhoids, fitting within the age range noted in recent systematic reviews: 33 to 57 years old (8), 34.7 to 47.0 years old (24), and 33.7 to 49.0 years old (25).
Our study revealed a majority of female participants, accounting for 54.9%, about 10% higher than males. This aligns with trends seen in an Italian study, which reported 58.3% female participants (22). However, contrasts exist in other studies where males predominated (14, 18-20, 23). Systematic reviews reflect variable gender distributions, indicating that gender does not significantly impact the quality of life in hemorrhoid sufferers (24, 25). Regarding occupational characteristics, 30.1% of our participants were housewives, retirees, and freelancers, with a significant portion being housewives, likely due to risk factors associated with pregnancy and less active lifestyles (26). Office workers also showed a higher incidence of hemorrhoids, attributed to prolonged sedentary periods (26).
Demographically, over 95% of participants identified as Kinh and more than 50% were non-religious, with the majority being married or living with a partner and possessing at least high school education—attributes reflecting urban demographics in Vietnam (27). The study also noted that most participants resided in urban areas and had incomes exceeding the 2022 national average, which supports the profile of patients who can afford care at a higher-cost facility like UMC HCMC (28).
The majority of subjects did not have significant comorbidities, with hypertension being the most common, reflecting the prevalence of non-communicable diseases among nearly 30% of the Vietnamese population (29). Surgical preferences in our study favored hemorrhoidectomy over stapled hemorrhoidopexy, a deviation from recent trends possibly due to temporary shortages in medical supplies. Patients had an average disease duration of 7.24 ± 8.24 years, with most not having received prior treatments, differing from findings in other studies and highlighting variability in patient histories and treatment approaches (13, 30).
This study revealed significant improvements in quality of life (QoL) following hemorrhoid surgery, as evidenced by decreased overall HF-QoL scores from 42.37 ± 12.74 before surgery to 23.54 ± 2.19 after surgery, marking a statistically significant enhancement in physical, psychological, defecation, and sexual health dimensions (Table 3). These findings are similar to Ayari et al.'s study, which documented considerable improvements in QoL post-rubber band ligation of hemorrhoids (21), and contrast with Giua's findings, where sucralfate ointment application led to substantial QoL benefits (22). The variations in QoL outcomes among these studies likely stem from differences in sample sizes, methodologies, and cultural settings.
| Interview Time | This Research | Ayari et al. 2020 (21) | Giua et al. 2021 (22) | |||||
|---|---|---|---|---|---|---|---|---|
| Before Surgery | After Surgery Eight Weeks | P-Value | Before Procedure | After Procedure | P-Value | Mean Change from Baseline in Score | P-Value | |
| Physical disorders | 19.34 | 11.06 | < 0.001 | 32.40 | 17.40 | < 0.001 | -15.90 | < 0.001 |
| Psychology | 11.58 | 7.06 | < 0.001 | 19.68 | 10.63 | 0.001 | -8.72 | < 0.001 |
| Defecation | 8.61 | 3.42 | < 0.001 | 11.22 | 5.63 | < 0.001 | -5.25 | < 0.001 |
| Sexuality | 2.85 | 2.00 | < 0.001 | 4.96 | 2.96 | 0.02 | -2.52 | < 0.001 |
| Overall HF-QoL | 42.37 | 23.54 | < 0.001 | 68.32 | 36.63 | < 0.001 | -32.58 | < 0.001 |
Furthermore, the research parallels studies that employ other QoL assessment tools, showcasing consistent QoL improvements post-hemorrhoid treatment. Notably, Rørvik's cross-sectional and cohort analysis using multiple QoL scales, including SF-12, SF-36, EuroQoL 5-dimensions 5-levels, and Short Health Scale for hemorrhoidal disease, revealed significant QoL enhancements, similar to the findings from Martinsons’s randomized trial comparing conventional hemorrhoidectomy and stapled hemorrhoidopexy (31, 32). Erdogdu’s research further corroborates these results, with significant post-surgical improvements in physical health scores assessed by SF-36 (33). Garg's observational study using the WHOQOL-BREF highlighted improvements in physical and psychological well-being one month post-stapled hemorrhoidopexy, though social domains showed minimal change (16).
While primarily set in an urban medical center, this study successfully provided robust insights into the effectiveness of hemorrhoid treatments. It benefited from a comprehensive quality of life assessment and a substantial sample size, ensuring the reliability of the findings. One of the notable strengths of this research is that it is one of the few studies of its kind in Vietnam, a developing country where such detailed health data are often scarce. This study contributes valuable knowledge to the medical community, both locally and globally, by highlighting specific demographic and socioeconomic factors that influence treatment outcomes.
However, the study faces certain limitations, including its focus on an urban population, which might not accurately represent the rural or lower-income groups in Vietnam. The setting in a single group of patients at a single center further limits the generalizability of the findings across different geographic and cultural settings within the country. Future research should include more diverse geographic settings and population groups to better understand the broader applicability of the findings across Vietnam.
5.1. Conclusions
The findings from this study confirm the efficacy of hemorrhoid surgery in improving quality of life across multiple dimensions. These outcomes not only highlight the physical benefits of the treatment but also emphasize the psychological and social improvements, which are crucial for comprehensive patient care. Future research should aim to address the noted limitations by including a more diverse population and implementing culturally adapted assessment tools. Additionally, exploring long-term outcomes and the sustainability of treatment effects will be vital in optimizing hemorrhoid management strategies.