1. Introduction
Overally the anomaly of the coronary arteries are rare. Its incidence according to angiographic, autopsy and echocardiographic findings, is about 1% (1-4), 0.29% (5) and less than 0.1% respectively (6). Usually these are the incidental finding during angiography without clinical presentation. But a significant percentage of young age sudden cardiac deaths are due to these anomalies (7-9). The contralateral sinus origin of the right coronary artery (RCA) is more common than left coronary artery (LCA) (1-4).
These anomalies may be accompanied by myocardial ischemia, arrhythmia, syncope and sudden death (10, 11).
2. Case Presentation
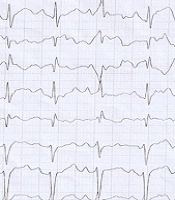
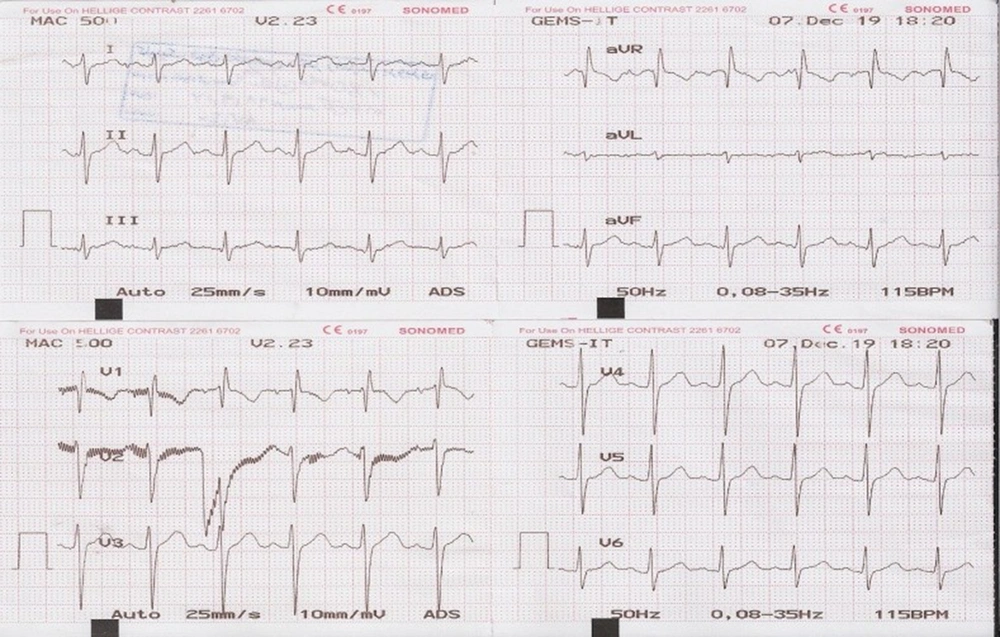
A 14-year-old Iranian boy reported experiencing shortness of breath and chest pain after exerting himself. His heart rate, rhythm and blood pressure were normal. He had non-specific changes in the ECG (Figure 1).
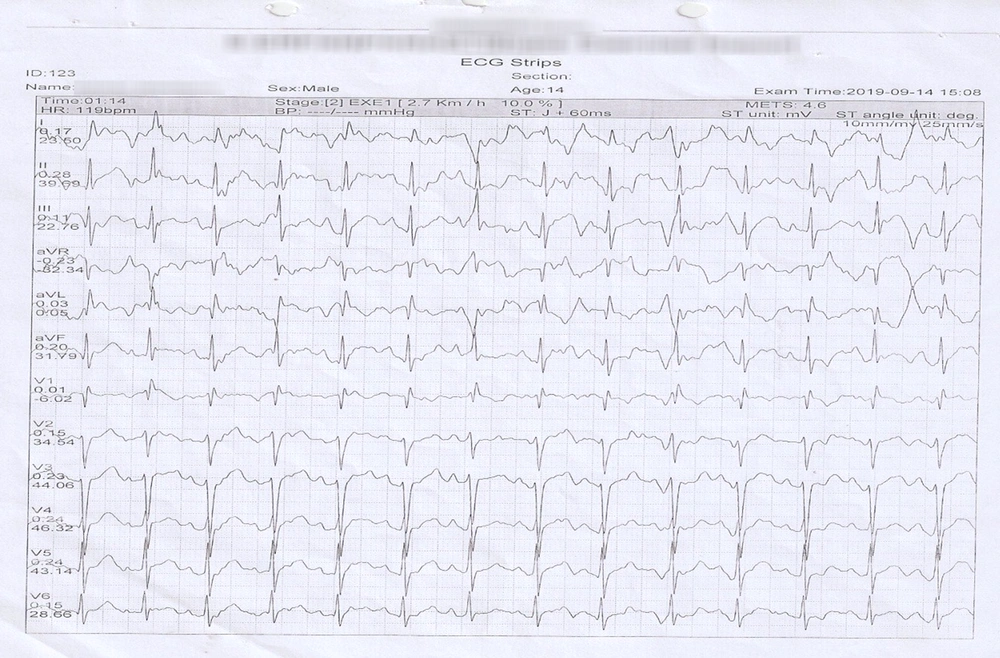
The findings of the exercise stress test were not specific (Figure 2).
The transthoracic echocardiogram showed normal size and function of ventricles but showed abnormal origin of RCA from left sinus of Valsalva.
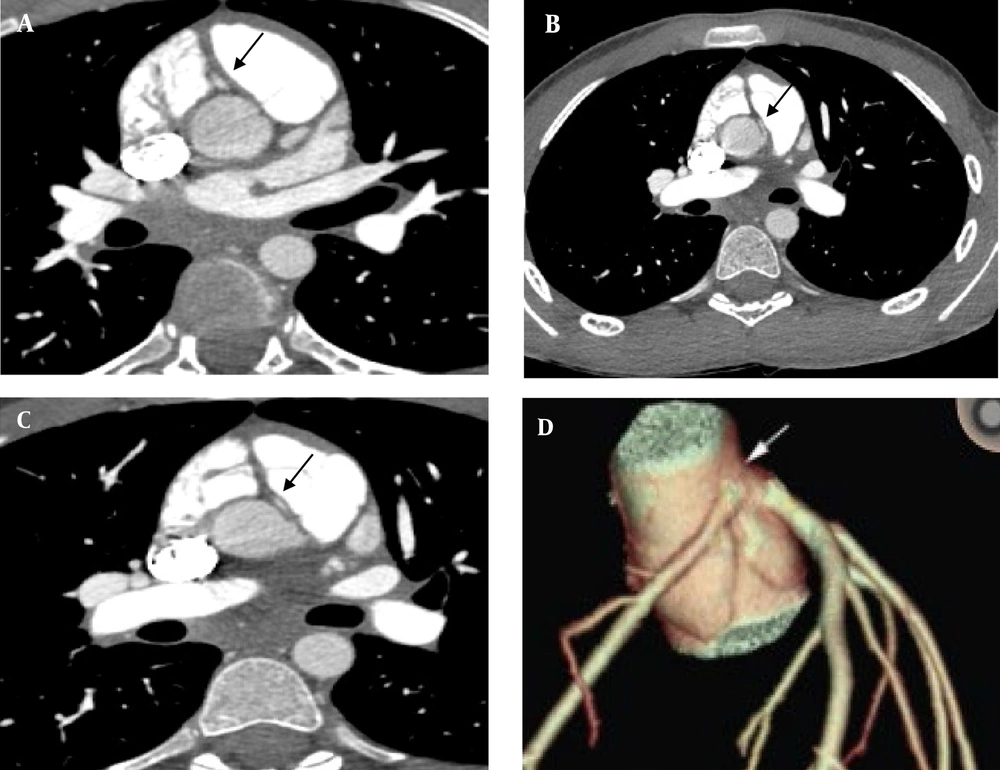
The RCA was found to originate from the left sinus of Valsalva with a distinct ostium and an intramural and inter-arterial course by computed tomographic coronary angiography (CTCA).
The RCA began adjunct to the ostium of the left main coronary artery and coursed intramural at proximal segment and then between the aorta and pulmonary artery (Figure 3).
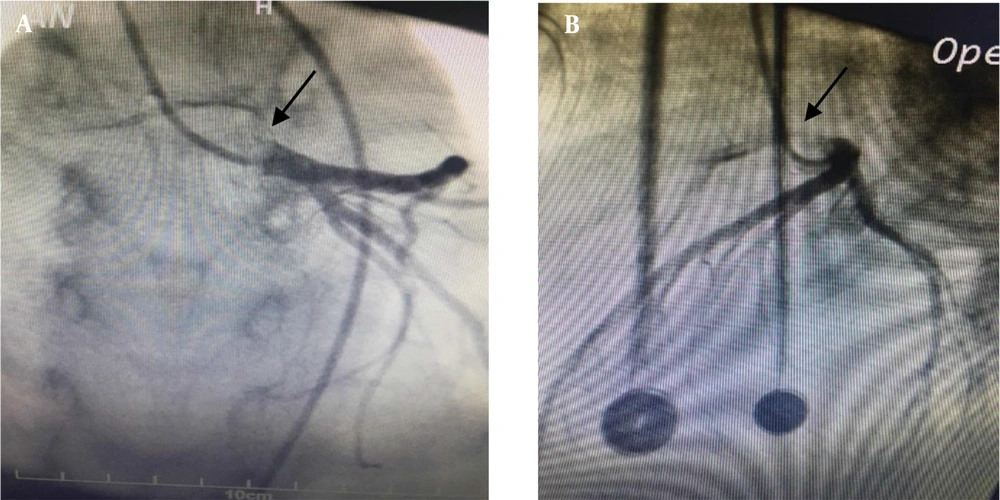
Selective coronary arteries angiography also confirmed this and RCA stenosis and slit-like coronary compressed between the pulmonary artery an aorta.
This finding is generally known as anomalous coronary artery from the opposite sinus (ACAOS) (Figure 4).
The patient underwent corrective surgery. The RCA was cut from between the aorta and pulmonary artery and connected to the right coronary sinus after preparing the sinus.
The post-operative period was uneventful. The patient recovered well and he was discharged with the ability to perform sports activity. During one year follow up the patient was asymptomatic with normal clinical evaluation.
3. Discussion
The solitary ostium coronary arteries anomaly was classified by Lipton et al. based on its origin and progression (12). In 2019 and 2020 Al Jarallah et al. and Rajan et al. introduced the modified classification (13, 14). Among coronary artery anomalies, ACAOS can be considered as a high risk factor for sudden death, particularly in young patients with inter-arterial course of anomalous artery (15). According to a study, of the 387 sudden fatalities of young athletes, 53 (13.7%) were caused by coronary artery abnormalities, the majority of which were ACAOS (15).
Right ACAOS is more common and more benign than left ACAOS (where the left main coronary artery originated from right coronary sinus). This anomaly can lead to myocardial ischemia and sudden death. This is a rare congenital anomaly with an incidence of 0.5%.
When symptoms do arise, they may include chest pain, fainting, palpitations, syncope, and sudden death. This anomaly is frequently asymptomatic (10, 11). The right ACAOS was initially suspected by trans thoracic echocardiography and later confirmed by CT-Angiography in this patient who experienced chest pain and exertional dyspnea.
The mechanisms of the signs and symptoms is not fully understood in these patients, but several mechanisms have been proposed:
(1) Compression of the RCA between pulmonary artery and aorta; (2) partially orifice stenosis in RCA; (3) compression of the intramural segment of RCA by aortic wall and (4) coronary artery spasm due to endothelial injury.
The presented patients' symptoms were multifactorial: intramural course and partial hypoplasia of intramural segment, inter-arterial course, oblique and stenotic ostium (Figure 4). These risk factors dispose the patient to be symptomatic and sudden death specially during or after physical activity or emotional stress.
Treatment for asymptomatic patients include observation and limiting competitive sports. In symptomatic patients, corrective surgery is recommended. Corrective surgery procedures include coronary bypass, direct implantation of anomalous artery, un-roofing the intramural segment of the vessel within aortic wall and osteoplasty, which aims at creating a new ostium in its proper place.
3.1. Conclusions
Although the single ostium coronary arteries anomalies are rare but they are increasingly diagnosed in recent years by non-invasive methods such as trans thoracic echocardiography confirmed by CT angiography or conventional angiography. These patients are susceptible to sudden death due to above mentioned risk factors, so attention to symptoms of the patients and comprehensive approach to them especially by non-invasive methods can be lifesaving.