1. Introduction
Though very rare, heart tumors in pediatric age group may present either in fetal life or after birth. Most of them are benign but they may cause significant morbidity. During fetal life they may cause arrhythmia, congestive heart failure and hydrops fetalis. During infancy, they may be found due to cardiac evaluation for a murmur in an asymptomatic child but they also may present with syncope, valvular insufficiency or stenosis, cyanosis, respiratory distress, or even sudden death. Among benign tumors rhabdomyoma, teratoma, and fibroma are more common. Less than 10% of primary cardiac tumors are malignant. Secondary malignant tumors are also quite rare but more prevalent than primary malignant tumors. Echocardiography provides the first anatomical characteristics of the cardiac tumor including its location or effect on cardiac function. Magnetic resonance imaging (MRI) and CT scan can also be used to evaluate the tumor more precisely (1, 2). Here, we present an infant with a rare pathology finding.
2. Case Presentation
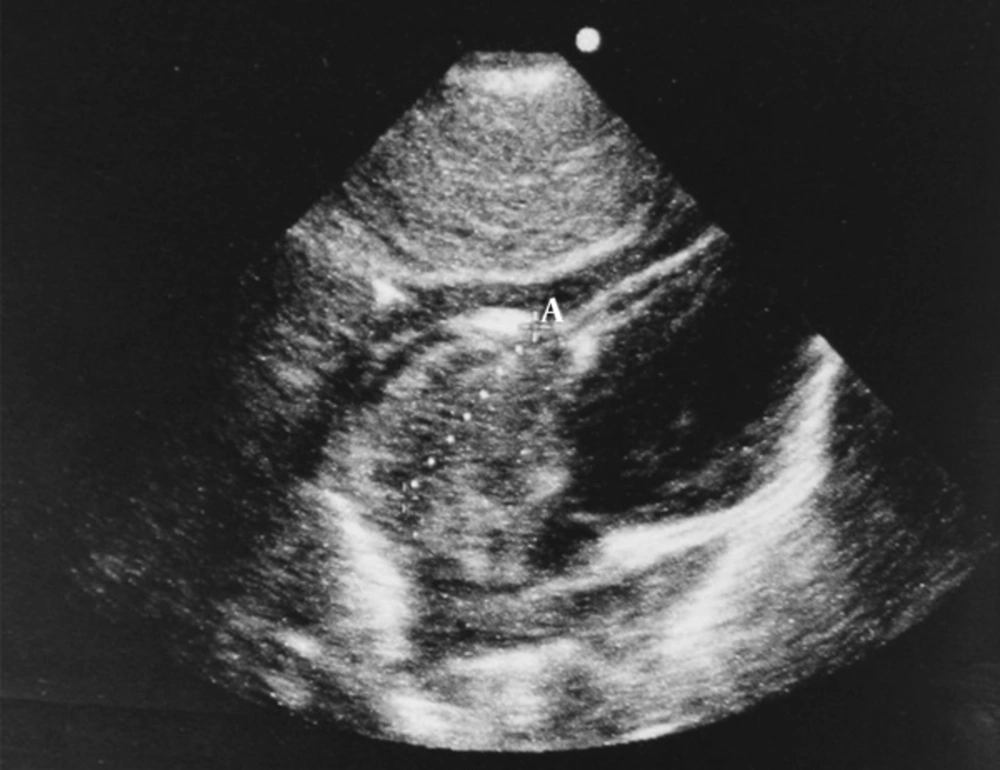
A nine-month-old female infant was admitted to the emergency ward of a general pediatric hospital due to severe tachypnea of two weeks duration which had become worse since the night before her admission. Her physical examination showed that she was well-developed, well-nourished, but mildly cyanotic with an oxygen saturation of 88%. A 3/6 systolic murmur was heard at the left sternal border. Respiratory rate was 60 /minute, heart rate was 110/minute and blood pressure was 90/50 mmHg. Chest X-ray showed normal heart size and pulmonary vascular markings. Electrocardiography revealed right axis deviation. Echocardiography showed a huge echogenic mass in the right atrium occupying almost half of its cavity. It was originated from the roof of RA and would herniate to RV during diastole causing tricuspid valve stenosis. Due to progressive dyspnea an emergency operation was performed and the tumor was resected completely.
The patient was urgently transferred to operation room (OR) in a cyanotic condition. After routine preparation and under the general anesthesia, thorax was exposed via a sternotomy incision. After that, pericardium was opened; heparin was infused, aortic cannula and also inferior and superior vena cava cannula were placed and the patient was attached to cardiopulmonary bypass (CPB) pump. The temperature was set on 32°C and total cardiac arrest was induced by infusion of cardioplegia solution. Right atrium was opened. A cardiac mass with a dimension of 4 × 4 cm which was attached to superior part of the atrium was removed. The connection part of the tumor was debrided and burned via cauterization. After that, atrium was closed, air was expunged from the heart, the patient was easily weaned from CPB pump, all the cannula were removed and protamine sulfate was given. Appropriate surgical drains and wire of pacemaker were placed. Finally, sternum was closed using No. 1 sternal steel wire and sub-cutaneous and cutaneous were sutured via routine methods.
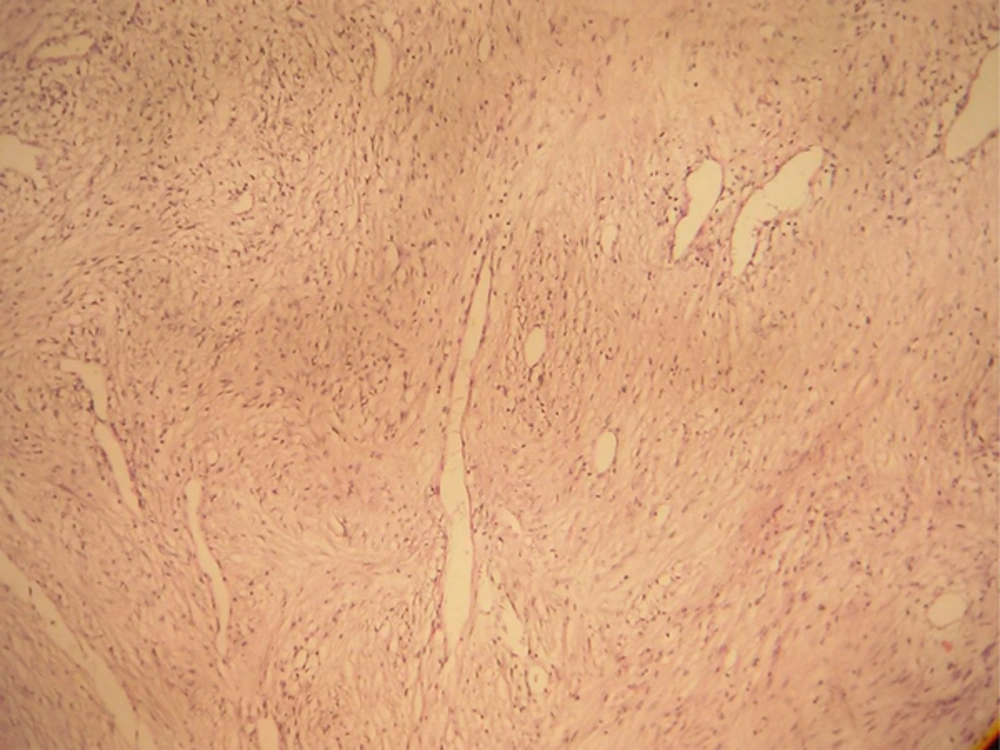
The specimen was sent to our pathology laboratory which consisted of a soft, lobulated and creamy piece, m: 3 × 2 × 2 cm. On cutting, it was creamy-brown and solid in appearance similar to a cardiac myxoma. Microscopically, a myxoid background was seen with foci of spindle cell proliferation, but no pleomorphism, mitotic activity, necrosis or hemorrhage was present. Based on the above morphology, we concluded that it was a low-grade myxoid spindle cell tumor and recommended immunohistochemical (IHC) studies for confirmation.
The paraffin blocks of the specimen were sent to another pathology laboratory, where IHC study was performed. The markers used were as follows: Vimentin (+), Desmin, H-Caldesmon, myogenin, and myo-D were all negative, meaning that the tumor was of smooth muscle and not skeletal muscle origin. In addition, ki67 which is an index of proliferative activity was estimated to be only 10% - 12%. Based on the above IHC findings, a second pathologist in another center diagnosed the tumor to be a low-grade spindle cell tumor with myxoid stroma, consistent with cardiac myxoma.
To further elaborate on the histogenesis of the tumor, the paraffin blocks were given to a third pathology laboratory where more markers were used with the following result: Vimentin, smooth muscle actin, and muscle specific actin were positive, while CD34 and S-100 were negative. The conclusion which was made by the third pathologist based on the IHC findings was that it was a tumor of smooth muscle origin, but no specific name was given to it. Fortunately, our follow-up up to nine months after surgery is inconsequential (Figures 1 and 2).
3. Discussion
Heart tumors in children are very rare. Here we presented a nine-month-old female infant who was admitted to the emergency ward due to severe tachypnea. A huge echogenic mass was detected in the right atrium (RA) occupying almost half of its cavity. Microscopically, a myxoid background with foci of spindle cell proliferation was present with no pleomorphism, mitotic activity, necrosis or hemorrhage. Consequently, immunohistochemical (IHC) studies were done for confirmation. The markers Desmin, H-Caldesmon, myogenin, and myo-D were all negative, meaning that the tumor was of smooth muscle and not skeletal muscle origin. In addition, ki67, an index of proliferative activity was only 10% - 12%. Based on IHC findings, a second pathologist in another center diagnosed the tumor to be a low-grade spindle cell tumor with myxoid stroma, consistent with cardiac myxoma. Histogenesis of the tumor had to be confirmed, so, the paraffin blocks were given to a third pathology laboratory where more markers were used. Smooth muscle actin, and muscle specific actin were positive, while CD34 and S-100 were negative. The conclusion was that it was a tumor of smooth muscle origin, but no specific name was given to it. This benign smooth muscle tumor, which may superficially resemble myxoma, yet is morphologically different from the typical myxoma is called “Benign Tumor with Perivascular myoid differentiation”. This is a rare, yet interesting entity which was firstly defined at 1998 and conforms to our findings. The nature and clinic-pathological features of tumors were described elsewhere (3). Recently, the immunohistochemical characteristics of such neoplasms are much more interesting and new findings are progressively discovered (4). This type of tumors have been observed in other organs (3, 5, 6) but to our knowledge, only one case was reported in the heart so far (7).
It may recur, mainly in adults. Microscopically, round, undifferentiated to epithelioid cells surrounding prominent, thin walled, stag horn vessels are noted. Mitosis and necrosis are absent. IHC studies reveal that Positive staining for Alpha smooth muscle actin is seen whereas the tumoral cells are CD34 negative. This new entity, recently described in soft tissues, can easily recur. Its recognition helps to differentiate from metastasis and other primitive cardiac tumors sharing the same morphological features but a different clinical behavior, with consequent improvement to the management of patient care (7, 8).
To our knowledge, a few similar cases were presented in the literature. Orlando et al. reported a healthy 70-year-old woman with the chief complaint of fatigue and dyspnea and a large mass in the RA originating from the roof. Pathologic examination showed a tumor with myoid glomangiopericytoma-type and haemangiopericytoma-like patterns. Mitosis and necrosis were absent. For the patient, diagnosis of tumor with perivascular myoid differentiation was made.
Differential diagnosis can include other masses with differentiation towards myoid cells/pericytes, such as solitary myofibroma, epithelioid haemangioendothelioma, glomus tumour, and vascular leiomyoma. Malignant tumours, such as leiomyosarcoma, malignant peripheral nerve sheath tumour, monophasic synovial sarcoma, myxofibrosarcoma, and malignant fibrous histiocytoma should be also considered (7).
3.1. Conclusions
This was a very rare case. However, we should remember that seeing a myxoid tumor in the heart is not equal to the diagnosis of myxoma. Other more rare differential diagnosis should be considered to prevent the diagnostic pitfalls.