1. Context
Herbal medicine, which has focused on herbal materials for the treatment of diseases, has grown in recent years due to relative safety. Saffron (Crocus sativus L.) is among the important plants used as a medication for several centuries in different parts of the world, such as India, China, Spain, Italy, Greece, and Iran (1).
Saffron (Crocus sativus L.) has strong antioxidant properties. Crocin, crocetin, and safranal are the main active ingredients of saffron (2, 3). In addition, saffron contains more than 150 volatile and aroma-yielding compounds and many non-volatile active components, such as polysaccharides and carotenoids, including zeaxanthin, lycopene, and beta-carotene (4). Regarding the important role of oxidative stress in many diseases, considerable interest has been shown in the potential role of saffron supplementation as a treatment for some diseases (3).
Saffron and its extract are applied in traditional medicine as a sedative, analgesic, antiemetic, anti-cramp, and antidepressant. Moreover, saffron with hypnotic and anticonvulsant effects has been used as a medicine to treat menstrual irregularities and some other disorders (2). In traditional medicine, it is claimed that saffron stimulates menstruation and can be used as an emmenagogue in amenorrhea. Saffron can relieve spasmodic pains, cause miscarriage, and stimulate abortion (5). Saffron, through its antidepressant properties, has the potential to enhance mental health (6). In traditional Indian medicine (Ayurveda), saffron is considered an adaptogen, which increases body resistance to stress, including trauma, anxiety, and fatigue (2).
Regarding the high prevalence of reproductive disorders and due to the high cost and side effects of treatment by chemical drugs in these patients, numerous studies have been performed on the effect of medicinal plants on the treatment of reproductive system disorders.
2. Objectives
Due to the general attention and popularity of medicinal plants, especially saffron, among women, numerous studies have been performed on the effect of saffron in obstetrics and gynecology. Therefore, this study was conducted to review the studies on the impact of saffron on premenstrual syndrome (PMS), labor, childbirth, and menopause.
3. Methods
This systematic review, based on the PICO process, systematically searched PubMed, Scopus, Cochrane, Embase, Web of Science, Science Direct, Google Scholar, Research Gate, and Persian databases, such as Scientific Information Database (SID) and Magiran, until February 2023. The search was based on a search strategy. Strategy search included keywords saffron OR Crocus sativus Linn. OR safranal OR crocin using AND premenstrual syndrome, postpartum depression, pregnancy anxiety, pregnancy depression, menopause, perimenopause, labor pain, childbirth, active labor phase, delivery, episiotomy, and pregnancy.
The inclusion criteria were clinical trial studies related to the title of this article published in Persian and English. The animal studies or articles for which the full text was not available were excluded. For study selection and data extraction, initially, a list of all articles found in the databases based on the search strategy and keywords was prepared. The researchers reviewed the titles of the obtained articles, and duplicates were removed. Then, the titles and abstracts of the remaining articles were carefully studied, and irrelevant articles were removed. Finally, the full texts of 20 related articles were reviewed, and appropriate articles were selected. All the steps of extraction and review of sources were taken by two researchers independently to prevent bias. In cases of disagreement between the two researchers, the article was reviewed by a third person.
In the next step, the information of the selected studies, including the first author’s name, article title, year of study, year of publication, place of study, sample size, study population, type of intervention, comparison group, main results, and side effects, were recorded in a pre-designed form as a result of the intervention. The quality of the articles was evaluated using the Jadad scale (Table 1). The quality assessment of the included articles was carried out using the Jadad scale, consisting of four criteria, including the possibility of bias, randomization, patient follow-up, and blinding. This criterion’s minimum, maximum, and total scores are 1, 2, and 5, respectively. Data analysis was performed qualitatively (7).
| First Author, Year | Randomization or Appropriate Method | Two-way Blinding | Number of Dropouts and Causes of Dropouts | ||||||
|---|---|---|---|---|---|---|---|---|---|
| No Random Allocation (0) | Random Allocation Description (1) | Complete Description of Random Allocation (2) | No Blinding (0) | One-way Blinding (1) | Two-way Blinding (2) | No Description (0) | Mention the Number of Dropouts (0.5) | Complete Description of the Number of Dropouts and Causes (1) | |
| Tabeshpour, 2017 (8) | * | * | * | ||||||
| Kashani, 2017 (9) | * | * | * | ||||||
| Lopresti, 2021 (10) | * | * | * | ||||||
| Kashani, 2018 (11) | * | * | * | ||||||
| Ghorbani, 2019 (12) | * | * | * | ||||||
| Mahdavian, 2019 (13) | * | * | * | ||||||
| Taavoni, 2017 (14) | * | * | * | ||||||
| Ghaderi, 2019 (15) | * | * | * | ||||||
| Ali-Akbari-Sichani, 2020 (16) | * | * | * | ||||||
| Sadi, 2016 (17) | * | * | * | ||||||
| Ahmadi, 2017 (18) | * | * | * | ||||||
| Mohammadierad, 2018 (19) | * | * | * | ||||||
| Ahmadi, 2015 (20) | * | * | * | ||||||
| Darooneh, 2018 (21) | * | * | * | ||||||
| Azhari, 2014 (22) | * | * | * | ||||||
| Mehrabi, 2015 (23) | * | * | * | ||||||
| Pirdadeh Beiranvand, 2016 (24) | * | * | * | ||||||
| Agha-Hosseini, 2008 (25) | * | * | * | ||||||
| Rajabi, 2020 (26) | * | * | * | ||||||
| Nemat-Shahi, 2020 (27) | * | * | * | ||||||
4. Results
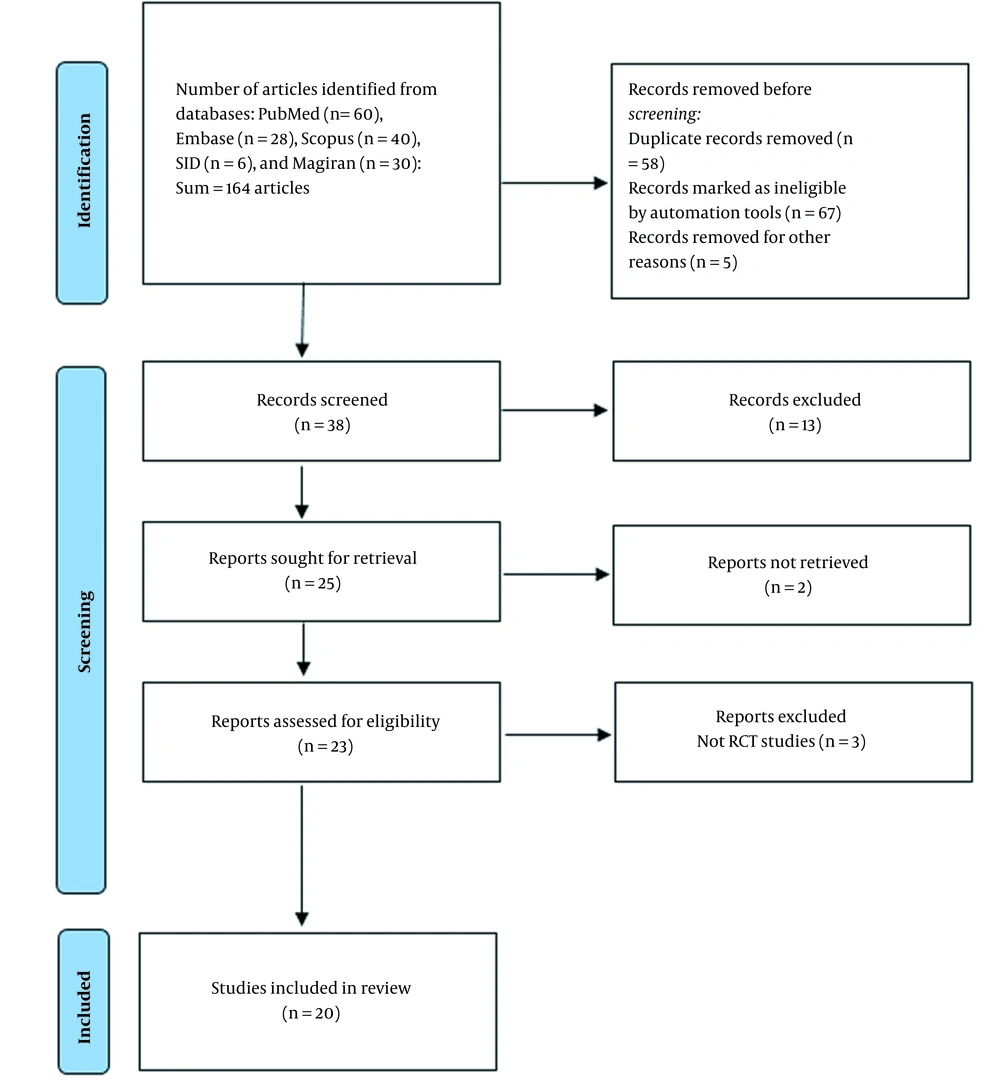
From a total of 164 articles, 128 studies were excluded after review (Figure 1). Finally, 20 randomized controlled trials (RCTs) were included in this study. Table 2 shows the details of the selected articles.
| No. | First Author, Year, Country | Population | Participants Intervention | Participants Control | Dropouts (%) | Main Results | Jadad Score |
|---|---|---|---|---|---|---|---|
| 1 | Tabeshpour, 2017, Iran (8) | Women with postpartum depression | N = 30, 30 mg saffron capsule twice a day for 8 weeks | N = 30, Placebo | 4% | Saffron decreased the severity of depression (P < 0.0001). | 4 |
| 2 | Kashani, 2017, Iran (9) | Women with postpartum depression | N = 34, 15 mg saffron capsule twice a day for 6 weeks | N = 34, 30 mg fluoxetine | 5.88% | Saffron and fluoxetine improved depressive symptoms of postpartum depression (P = 0.61). | 5 |
| 3 | Lopresti, 2021, Australia (10) | Premenopausal women | N = 43, 14 mg saffron tablet twice a day for 12 weeks | N = 43, Placebo | 11.62% | Saffron improved mood and psychological symptoms, compared to the placebo (P = 0.032). | 5 |
| 4 | Kashani, 2018, Iran (11) | Postmenopausal women | N = 30, 15 mg saffron capsules twice a day for 6 weeks | N = 30, 15 mg placebo | 7% | Saffron improved hot flashes and depressive symptoms in postmenopausal women (P = 0.0001). | 5 |
| 5 | Ghorbani, 2019, Iran (12) | Postmenopausal women | N = 40, 30 mg saffron capsule daily for 4 weeks | N = 40, 30 mg starch powder | 16.25% | Mean scores of happiness increased in the saffron group (P < 0.001). | 5 |
| 6 | Mahdavian, 2019, Iran (13) | Premenopausal women | N = 90, Divided into three groups: A (15 mg saffron); B (60 mg); D (30 mg) for 12 weeks | N = 30, 30 mg placebo (group C) | 11.11% | Physical, psychological, and urogenital symptoms improved in group B (P < 0.001). | 3.5 |
| 7 | Taavoni, 2017, Iran (14) | Postmenopausal women | N = 40, Aphrodite capsule containing 3 mg of Crocus sativus extract twice a day for 4 weeks | N = 40, Placebo | 21.25% | Aphrodite capsules significantly reduced menopausal symptoms (physical symptoms: P = 0.001; mental symptoms: P = 0.02). | 4 |
| 8 | Ghaderi, 2019, Iran (15) | Labor progression in nulliparous women | N = 30, Saffron syrup prepared with honey; n = 30, Saffron syrup prepared with sugar | N = 30, Placebo | 3.33% | The duration of the first stage of labor was shorter in the honey saffron syrup group than in the sugar saffron syrup group (P = 0.016). | 5 |
| 9 | Ali-Akbari-Sichani, 2020, Iran (16) | Women during labor | N = 30, A saffron capsule (250 mg) | N = 30, Placebo | 6.25% | The mean Bishop’s score in the saffron group was higher than before vs. after the study (P = 0.001). The average length of the first and second stages of labor was shorter in the saffron group (P > 0.05). | 5 |
| 10 | Sadi, 2016, Iran (17) | Women during labor | N = 25, Saffron pill (250 mg) three times in 24 hours | N = 25, Placebo | 8% | The Bishop’s score was higher in the saffron group (P = 0.029). | 5 |
| 11 | Ahmadi, 2017, Iran (18) | Women during labor | N = 30, 250 mg saffron capsule | N = 30, 250 mg placebo capsule | Not reported | Saffron reduced pain (P < 0.001), anxiety (P = 0.004), and length of the active phase of the first (p = 0.002) and second stages of labor (P < 0.000). | 4 |
| 12 | Mohammadierad, 2018, Iran (19) | Women during labor | N = 32, Oral syrup of saffron (80 ml) plus date (250 mg); n = 32, Oral syrup of saffron (250 mg) plus white sugar | N = 32, Placebo | 7.29% | Pain and anxiety were reduced in the intervention groups (P = 0.02). | 5 |
| 13 | Ahmadi, 2015, Iran (20) | Women during labor | N = 30, 250 mg saffron capsule | N = 30, 250 mg of starch | Not reported | Anxiety (P < 0.000) and fatigue (P = 0.004) were reduced in the saffron group. | 3 |
| 14 | Darooneh, 2018, Iran (21) | Women during labor | N = 30, 250 mg saffron capsule per night for 3 nights | N = 30, 250 mg placebo capsule | 21.25% | There was no significant difference between the intervention and placebo groups in mean anxiety score (P > 0.05). | 5 |
| 15 | Azhari, 2014, Iran (22) | Women during labor | N = 30, 250 mg saffron capsule with the onset of the active phase of labor | N = 30, Placebo | 0% | The mean pain intensity was reduced in the saffron group (P < 0.001). | 5 |
| 16 | Mehrabi, 2015, Iran (23) | Primiparous women with episiotomy | N = 30, Topical cream containing saffron extract three times a day for 2 weeks | N = 30, Placebo cream | 0% | Saffron extract cream 20% can be effective for episiotomy wound healing and wound edge continuity (P < 0.001). | 3 |
| 17 | Pirdadeh Beiranvand, 2016, Iran (24) | Students with premenstrual syndrome | N = 44, 30 mg saffron capsule once a day for two menstrual cycles | N = 44, Placebo | 11.36% | Saffron improved symptoms of PMS (P < 0.001). | 4 |
| 18 | Agha-Hosseini, 2008, Iran (25) | Women with PMS | N = 25, 30 mg saffron capsule twice a day for two menstrual cycles | N = 25, Placebo capsule | 6% | Saffron improved symptoms of PMS (P < 0.001) and Hamilton Depression Rating Scale (P < 0.001). | 4 |
| 19 | Rajabi, 2020, Iran (26) | Women with a diagnosis of premenstrual dysphoric disorder | N = 40, Saffron capsule (15 mg) twice a day; n = 40 Fluoxetine (20 mg) twice a day for 2 weeks in the luteal phase of two menstruation cycles | N = 40, Placebo | 0% | Saffron improved in all of the treatment approaches in terms of the Daily Record of Severity of Problems and Hamilton assessments (P < 0.001). | 5 |
| 20 | Nemat-Shahi, 2020, Iran (27) | Women with PMS | N = 82, 30 mg saffron capsule a day from day 14 to day 28 of the menstrual cycle | N = 82, 20 mg fluoxetine | Less than 10% | Saffron reduced PMS symptoms, such as abdominal bloating, depression, and mood swings (P = 0.01). | 4 |
Abbreviation: PMS, premenstrual syndrome.
Among these 20 studies, 19 RCTs were conducted in Iran and 1 in Australia within 2007 - 2023. Most studies (n = 13) used saffron as capsules (two studies as pills, two studies as syrup, one study as a topical cream, and two other studies in combination). In 17 studies, the control group received a placebo. Fluoxetine was given to the control group only in three studies. Among the studies, nine, five, four, and two studies applied saffron for labor and childbirth, during menopause, for PMS, and for postpartum depression, respectively.
4.1. Use of Saffron in Labor and Childbirth
Nine studies are related to using saffron in labor and childbirth. Some of these studies assessed the effect of saffron on the length of labor, and the results of all these studies showed that saffron is effective in reducing the length of the first, second, and third stages of labor (15-20). In three of these studies, Bishop’s score was examined before and after using saffron, indicating the effectiveness of saffron in Bishop’s score (16, 17, 21) Bishop containing five cervical characteristics (i.e., dilatation, effacement, position, presenting part station, and consistency) is scored within 0 - 10 and is probably an effective factor in successful labor induction (28). Pregnancy anxiety was assessed in five studies (18-22), labor pain intensity in three studies (18, 19, 22), and labor fatigue in one study (20). The results of all aforementioned studies showed that saffron could reduce the mean of fatigue and pain intensity of labor compared to the control group; however, contradictory findings were reported in terms of pregnancy anxiety.
One study showed that a 20% saffron extract cream could be effective for episiotomy wound healing and wound edge continuity. There was a significant difference between intervention and control groups in terms of episiotomy location healing on the 7th and 14th days and the continuous process of the wound edges on the 1st, 7th, and 14th days. There was no statistically significant difference between the intervention and control groups in opening the wound on the first day; nevertheless, a statistically significant difference was observed between the two groups on the 7th and 14th days (23).
4.2. Use of Saffron in Menopause
In two studies, which used saffron alone, the results showed that saffron could improve mood and psychological symptoms but had no effect on improving vasomotor symptoms, physical symptoms, or quality of life (10, 11). In two other studies, saffron was used in combination with other herbal remedies (e.g., ginger, fennel, chamomile, Tribulus terrestris, or Cinnamomum). The results showed that treatment with saffron extract improved the symptoms of menopause, including physical, psychological, and genital symptoms (13, 14). The results of one study also showed that saffron could increase happiness in menopause (12).
4.3. Use of Saffron in Premenstrual Syndrome
In two studies, the mean severity of PMS was lower in the saffron group than in the control group, which used a placebo (24, 25). Additionally, in one study, the mean Hamilton depression score was lower in the saffron group (25). However, the results were different in another study that used fluoxetine for the control group. The mean severity of PMS in the saffron group was slightly different from the fluoxetine group but lower than the placebo group. Moreover, saffron was an efficacious herbal agent for treating the premenstrual dysphoric disorder with minimal adverse effects (26). A study performed by Nemat-Shahi et al. showed that using saffron in PMS reduced the symptoms, such as abdominal bloating, depression, and mood swings (27).
4.4. Use of Saffron in Postpartum Depression
Kashani et al. used saffron versus fluoxetine to treat mild to moderate postpartum depression. They observed no significant difference between the two groups in the Hamilton Depression Rating Scale (HDRS) (P = 0.37). In the saffron group, 13 patients (40.60%) experienced a complete response (≥ 50% reduction in HDRS score), compared to 16 patients (50%) in the fluoxetine group. The difference between the two groups was not statistically significant (P = 0.61). Therefore, Kashani et al. suggested saffron as a safe herbal medicine for improving depressive symptoms of postpartum depression (9). Another study showed that daily use of saffron (30 mg), 8 weeks after treatment, decreased the severity of postpartum depression (P < 0.0001) (8).
4.5. Adverse Effects
In the studies reviewed in this article, there was no major adverse effect or death related to using saffron. Mild side effects reported in various studies included weakness and severe increase in fetal movements (21), lethargy and redness in the face and limbs, heartbeat (15, 16), and nausea (19, 21).
5. Discussion
This study generally focused on articles on the effects of saffron on PMS, labor, childbirth, and menopause. The clinical evidence shows that consuming saffron in different doses can reduce fatigue and anxiety during pregnancy, facilitate the delivery process, and reduce unpleasant moods during pregnancy and after delivery.
To date, numerous studies have been performed on the effect of saffron on depression, almost all of which have confirmed the effect of saffron on depression (9, 29). Hosseinzadeh et al. measured the antidepressant effects of saffron on mice and showed that safranal, which is responsible for saffron fragrance, has antidepressant effects (30). Unfortunately, there were only two clinical trials on the effect of saffron on postpartum depression. In the aforementioned two studies, saffron was as effective as chemical drugs used to treat depression, such as fluoxetine. However, due to the small number of studies performed in the postpartum period, it is necessary to design and conduct further studies in this field.
Studies have also shown that saffron reduces anxiety and fatigue during labor. It is stated that the effect of saffron is similar to the activity of diazepam with anti-anxiety, analgesic, and muscle relaxant effects (20). The results of some studies are consistent with the aforementioned findings (19, 20, 31-33). Nonetheless, in a study by Darooneh et al. (2018), saffron capsules did not reduce labor anxiety (21). In the above-mentioned studies, the sample size and dose of saffron were almost the same; probably, this discrepancy in the results of the studies can be attributed to the different tools used to measure anxiety in Darooneh et al.’s study. In addition, in Darooneh et al.’s study, the time of measuring anxiety differed from other studies. They measured anxiety at the time of admission (without labor contractions); however, in other studies, anxiety was measured when individuals were in labor.
According to studies, saffron improved labor and reduced labor length (2, 16, 17). Saffron plays an important role in the stimulation and intensity of uterine contractions due to the increased function of smooth uterine muscles due to the presence of crocin, crocetin, alfa carotene, anthocyanin, zigzantin, tannin, picrocrocin, and safranal (15). Despite the fact that several studies have shown the stimulatory properties of saffron on the uterus, the property of relieving uterine contractions has been mentioned in a review study (34) Additionally, by another mechanism, saffron reduced labor pain (22). Recent studies on saffron have been able to control the bias through blinding and having a control group. The use of similar doses and methods in these studies strengthens the consensus on the effect of saffron on labor and delivery. The identification of saffron components and their biological function also confirms the findings of the above-mentioned studies. However, further studies are needed to identify the mechanism of saffron components that cause different effects on the uterine smooth muscle in different doses.
The result showed that saffron has positive effects on PMS. It can improve mood and psychological symptoms of menopause and PMS (24-27). Components of saffron, such as flavonoids and carotenoids, have antioxidant effects and could prevent the production of prostaglandins by trapping free radicals, such as oxygen and superoxide radicals (24). Therefore, the antioxidant property of saffron is one of the mechanisms of its pain-relieving activity. According to other studies on the effect of saffron on pain and depression and its reduction effect, the results of the above-mentioned studies can be justified. The questionnaires used for PMS diagnosis, saffron dose, and age range of participants were almost similar in most studies. Although, in these studies, random allocation has been used and an attempt has been made to some extent eliminate the effect of the confounding variable, studies with longer follow-ups and larger sample sizes and age group ranges are needed to better control the effective factors, such as lifestyle and nutrition. Most studies have been performed on the age group over 20 years. Adolescents are at childbearing age and are exposed to this disorder due to hormonal changes. Therefore, the results of these studies cannot be generalized to the whole community.
According to the findings, saffron can improve mood and psychological symptoms and increase happiness in menopause (10-14). The women in these studies were older and might have different physical and mental problems due to menopause. On the other hand, according to studies, saffron has an effect on all organs of the body. Therefore, before generalizing the results of these studies and the routine use of saffron supplements, further extensive studies should be conducted to determine the appropriate dose of saffron without adverse effects on other organs. One of the possible mechanisms for the effects of saffron is its effect on female sex hormones. In various animal studies, saffron increases the levels of the hormones estrogen, progesterone, luteinizing hormone, and follicle-stimulating hormone (10).
In the reviewed articles, there was no evidence that the dose of saffron used was toxic or lethal. Side effects of the used doses were mild, and there was no significant side effect in the follow-up of individuals who had these side effects. The dose used in studies on postpartum depression, PMS, and menopause was within the range of 14 - 60 mg (i.e., 14, 15, 30, and 60). All four used doses had a positive effect on the studied variables. However, in a study by Mahdavian et al., who studied different doses (i.e., 15, 30, and 60 mg) of saffron in premenopausal syndrome, the results showed that the dose of 60 mg was more effective in relieving symptoms and did not have any specific side effects (13). Other studies related to labor and delivery stages used saffron at a dose of 250 mg in various forms, such as capsules and syrups, which were effective in reducing pain and anxiety, accelerating cervical maturation, and helping delivery progress (Table 2).
Due to the sensitivity of pregnancy regarding the use of drugs, there are studies that have used a dose of 250 mg. This dose in these studies has some positive effects on the studied variables, such as pain and cervical ripening. Moreover, the fact that it did not have any specific side effects has encouraged other researchers to use this dose. This can be a reason for the similarity of dosage used in studies that have investigated the effect of saffron on various variables in labor and delivery. Due to the difference in the severity and nature of pain and contraction during labor, compared to the symptoms of PMS, increasing the effective dose from 15 - 30 mg to 250 mg seems reasonable.
In some studies, such as Mohammadierad et al.’s study, there were some side effects in the saffron group, such as nausea, high heart rate, and redness of the face (19). However, in a study by Sadi et al. that used a similar dose of saffron, there were no side effects (17). Therefore, since one of the goals of using herbal medicines instead of chemical medicines, especially in pregnant women, is to reduce side effects, it is better to design and conduct further similar studies in this field by adjusting the saffron dose.
5.1. Conclusions
Saffron is suggested as a medicinal plant that can help improve women’s complications. However, due to the limited number of studies in this area and the limitation of some studies, it is recommended to perform further studies without the limitations of previous studies before applying saffron in clinical medicine. The positive point of this study is the collection of all the related studies on the effect of saffron in gynecology and obstetrics. This study can help researchers select the subjects which need further research.