1. Background
Rotator cuff tear (RCT) is a common pathology in adult populations, occurring in 25% of people up to age 60 and in more than 50% up to age 80 (1). RCT has a traumatic or degenerative cause. Traumatic tears occur due to severe traumas, while degenerative tears have highly frequent and multifactorial etiologies (2).
The advances made in shoulder surgery techniques over the past decades have led to pain relief and improved shoulder function in patients with RCT (3-7). About 75,000 to 250,000 rotator cuff repair (RCR) cases are performed annually in the United States.
There are different surgical techniques for RCR. Open RCR is recognized as the gold standard, but mini-open RCR (MRCR) has been shown to be an effective and reliable alternative (3, 8). Since the advent of arthroscopy, open surgical techniques have evolved into arthroscopic assisted and all-arthroscopic techniques. It appears that procedures with smaller incisions cause less tissue damage, which may reduce pain and complications. Arthroscopic RCR (ARCR) is a novel technique which has recently gained shoulder surgeons’ attention.
MRCR costs significantly less than ARCR and produces good outcomes in 90% of patients (3, 9-12). However, some surgeons believe that MRCR leads to higher rates of stiffness in the shoulder (13). On the other hand, ARCR has clinical outcomes equivalent to those of MRCR and open surgery, but less pain and stiffness and faster recovery. In addition, due to its smaller incisions, it is aesthetically superior (14-16). However, this procedure depends on the skill and experience of the shoulder surgeon and anesthesiologist and the quality of the arthroscopy in the operating room.
2. Objectives
Although systematic review studies compared ARCR and MRCR methods, shoulder surgeons have not yet reached consensus regarding the preferred method. The present study was designed to compare the short-term outcomes of ARCR and MRCR in the treatment of full thickness RCT.
3. Methods
3.1. Study Design and Participants
The present cohort study was conducted at Poursina Hospital of Rasht and Akhtar Hospital of Tehran. Using census method, we enrolled all the patients with a diagnosis of full RCT (based on clinical symptoms, examinations, and magnetic resonance imaging [MRI]) who had undergone ARCR and MRCR from 20 March 2017 to 20 March 2020.
The inclusion criteria were diagnosis of full RCT, failure to respond to six weeks of conservative treatment (treatment with non-steroidal anti-inflammatory drugs [NSAIDs], reduced physical activity, and receiving physiotherapy), consent to participate in the study, no history of diabetes, neurological diseases, surgery, and fractures in the shoulder, and absence of concomitant frozen shoulder. The patients with clear shoulder instability, shoulder labrum injury, superior labrum from anterior to posterior lesion, subscapularis tear, acromioclavicular degenerative joint disease, and massive tear (tear > 5 cm) were excluded from the study.
3.2. Surgical Techniques
All the surgeries were performed under general anesthesia and beach-chair position by a shoulder surgeon (the first author). All the patients received a diagnostic arthroscopy first. Then, if possible, arthroscopic repair of the cuff tear was carried out (using suture anchor and Ethibond 5). MRCR was carried out by a 3-cm-long transverse incision if, for any reason, performing arthroscopic repair was not an option (ie, the patient's inability to afford the equipment needed for arthroscopic repair, poor visibility for ARCR, and the patient’s poor medical conditions not allowing the resume of ARCR). Suture anchor, tunneling the humerus tuberosity, and Ethibond 5 were used in this technique. All the patients received acromioplasty with a burr.
3.3. Rehabilitation Protocol
Both groups of patients received the same rehabilitation program. Physiotherapy was performed by an experienced physiotherapist in the same clinic three sessions per week (30 - 50 sessions of 45 - 60 minutes). Sling immobilization was administered for the first four weeks, and the sling was removed only during bathing and physiotherapy during these four weeks. Physiotherapy began after two weeks of immobility. The administered physiotherapy included passive pendulum range of motion as a tolerable forward flexion, and internal rotation up to 40 degrees with 90-degree forward elevation. After week four, gentle active exercises, and in week six, strengthening the biceps and deltoid were pursued. From week nine to twelve, scapular stabilization and posterior capsular stretching were performed. Physiotherapy continued until full range of motion was reached. At months four to six, the emphasis was on restoring the patient to their previous work activities and exercise at the gym.
3.4. Data Collection
All data were collected by an orthopedic resident who did not know the patients’ group. First, the patients’ demographic details, such as age, sex, surgical method (MRCR or ARCR), involved side and dominance, duration of surgery, surgery complications (infection, axillary nerve injury, and deltoid muscle detachment), and symptomatic duration were extracted from their hospital records. In addition, their radiologic and arthroscopic findings, such as acromion type and RCT level were recorded. The patients were followed-up for up to six months after the surgery. The shoulder function, disability, range of motion (ROM), and severity of pain were recorded in the data collection form before and three, and six months after surgery. The pre-surgery data were collected from the patients' hospital records, and the post-surgery data were collected when the patient visited the orthopedic clinic.
Shoulder function was assessed using the University of California Los Angeles (UCLA) Shoulder Score, disability using the Quick Disabilities of the Arm, Shoulder, and Hand (DASH) score, and pain using the Visual Analog Scale (VAS). ROM was assessed by comparing the active external rotation, active forward elevation, and passive internal rotation on the involved side and the healthy shoulder with a goniometer.
3.5. Statistical Analysis
To describe quantitative and qualitative variables, mean (standard deviation) and number (percentage) were used, respectively. Shapiro-Wilk test was used to determine the normality of quantitative variables in both groups. Independent t-test was run to compare quantitative variables such as age, duration of surgery, VAS, UCLA, ROM, and Quick DASH scores in the two groups. Meanwhile, chi-square test was used to compare the qualitative variables (sex, dominant hand, involved shoulder, history of trauma, and follow-up period) in the two groups. Repeated measures analysis of variance (ANOVA) was run to study the changes in the scores in the measurement intervals. A P-value < 0.05 was considered as the significance level. All data were analyzed using SPSS version 20.
3.6. Ethical Issues
The study protocol was approved by the ethics committee of Guilan University of Medical Sciences (IRB no: 1559). All procedures were in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and the most recent version of Helsinki Declaration. Informed consent was obtained from all patients prior to the study.
4. Results
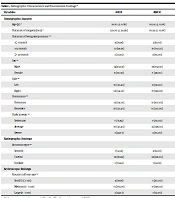
Out of a total of 73 subjects, 49 met the inclusion criteria. Two patients from the ARCR group were excluded due to failure to follow up. Finally, 22 patients in the ARCR group and 25 patients in the MRCR group were included. Table 1 shows patients’ demographic details, radiologic and arthroscopic findings. There was a significant difference between the two groups only in the duration of surgery (P < 0.05). No complications (infection, bleeding, auxiliary nerve damage, and deltoid muscle detachment) were observed in either of the groups.
| Variables | ARCR | MRCR | P-Value |
|---|---|---|---|
| Demographic features | |||
| Age (y) * | 59.95 ± 9.78 | 59.04 ± 9.09 | 0.74 |
| Duration of surgery (min) * | 125.50 ± 24.28 | 70.42 ± 33.97 | 0.00 |
| Duration of being symptomatic (mo) ** | 0.57 | ||
| ≤ 3 | 4 (18.18) | 2 (8.00) | |
| 3 - 12 | 15 (68.18) | 19 (76.00) | |
| ≥ 12 | 3 (13.64) | 4 (16.00) | |
| Sex ** | 0.53 | ||
| Male | 14 (63.64) | 18 (72.00) | |
| Female | 8 (36.36) | 7 (28.00) | |
| Side ** | 0.34 | ||
| Left | 10 (45.45) | 8 (32.00) | |
| Right | 12 (54.55) | 17 (68.00) | |
| Dominance ** | 0.70 | ||
| Dominant | 12 (54.55) | 15 (60.00) | |
| Recessive | 10 (45.45) | 10 (40.00) | |
| Daily activity ** | 0.83 | ||
| Sedentary | 7 (31.82) | 9 (36.00) | |
| Average | 10 (45.45) | 12 (48.00) | |
| Severe | 5 (22.73) | 4 (16.00) | |
| Radiographic findings | |||
| Acromion type ** | 0.46 | ||
| Smooth | 1 (4.54) | 2 (8.00) | |
| Curved | 18 (81.82) | 22 (88.00) | |
| Hooked | 3 (13.64) | 1 (4.00) | |
| Arthroscopic findings | |||
| Rotator cuff tear size ** | 0.62 | ||
| Small (≤ 1 cm) | 4 (18.18) | 5 (20.00) | |
| Medium (1 - 3 cm) | 13 (59.09) | 17 (68.00) | |
| Large (> 3 cm) | 5 (22.73) | 3 (12.00) |
a Values are expressed as mean ± SD or No. (%).
b * Independent t-test; ** Chi-square test.
The short-term outcomes on the three occasions showed significant improvements in shoulder function, disability, and ROM and a reduction in pain in both groups (P < 0.05), but there was no significant difference between the two groups on any of the three occasions (P > 0.05) (Table 2).
| Variables | Measuring Tools | Groups | Before | 3 Months | 6 Months | P-Value ** |
|---|---|---|---|---|---|---|
| Shoulder function | UCLA shoulder score | ARCR | 14.77 ± 4.66 | 25.90 ± 3.57 | 32.90 ± 1.79 | < 0.001 |
| MRCR | 16.16 ± 4.55 | 26.92 ± 3.71 | 33.40 ± 1.35 | < 0.001 | ||
| P-value * | Ptime < 0.001, Pgroup = 0.26, Pint.time × group = 0.67 | |||||
| Disability | DASH score | ARCR | 57.90 ± 16.29 | 31.13 ± 7.62 | 16.72 ± 5.87 | < 0.001 |
| MRCR | 56.68 ± 13.24 | 29.64 ± 7.85 | 15.28 ± 6.36 | < 0.001 | ||
| P-value * | Ptime < 0.001, Pgroup = 0.59, Pint.time × group = 0.96 | |||||
| ROM | Active forward elevation | ARCR | 51.13 ± 9.48 | 76.77 ± 6.18 | 82.04 ± 23.21 | < 0.001 |
| MRCR | 51.00 ± 12.58 | 75.80 ± 6.49 | 91.00 ± 14.06 | < 0.001 | ||
| P-value * | Ptime < 0.001, Pgroup = 0.3, Pint.time × group = 0.12 | |||||
| Active external Rotation | ARCR | 50.81 ± 9.97 | 74.40 ± 13.85 | 90.40 ± 14.98 | < 0.001 | |
| MRCR | 51.08 ± 9.30 | 77.64 ± 5.98 | 93.28 ± 11.42 | < 0.001 | ||
| P-value * | Ptime < 0.001, Pgroup = 0.3, Pint.time × group = 0.7 | |||||
| Passive internal rotation | ARCR | 51.50 ± 9.22 | 77.18 ± 5.63 | 88.00 ± 18.13 | < 0.001 | |
| MRCR | 51.48 ± 10.25 | 77.16 ± 5.92 | 89.08 ± 16.69 | < 0.001 | ||
| P-value* | Ptime < 0.001, Pgroup = 0.86, Pint.time × group = 0.9 | |||||
| Pain | VAS | ARCR | 8.04 ± 0.95 | 3.36 ± 1.00 | 0.81 ± 0.79 | < 0.001 |
| MRCR | 7.96 ± 1.24 | 2.92 ± 1.07 | 0.60 ± 0.70 | < 0.001 | ||
| P* | Ptime < 0.001, Pgroup = 0.26, Pint.time × group = 0.54 | |||||
Abbreviations: UCLA, University of California Los Angeles; ROM, range of motion; VAS, visual analog scale; SD, standard deviation. ARCR: arthroscopic rotator cuff repair; MRCR: mini-open rotator cuff repair.
a Values are expressed as mean ± SD. * Repeated measures ANOVA. ** Independent t-test.
5. Discussion
This study compared the short-term outcomes of ARCR and MRCR. The findings did not show any significant difference between the two groups in the initial and pre-surgery data. The surgery outcomes improved significantly over time in both groups. No significant difference was found between the two groups on any of the three measurement occasions.
In a two-year follow-up, Bond et al. reported no difference between the MRCR and ARCR groups in terms of shoulder pain and function (17). In their meta-analysis, Morse et al. reported no difference between these two surgical techniques (18). Liu et al. reported that ARCR produced better short-term outcomes, although long-term outcomes were the same in both groups (19). Conversely, Barnes et al. showed better integrity of the repair and shoulder function in the MRCR group (20). Contrary to the present findings, it appears that patients experienced less pain with ARCR due to the smaller incision and were therefore more cooperative during their physiotherapy, which resulted in a better quality of physiotherapy and better functional outcomes (19). In agreement with the present findings, Cho et al. reported no short-term differences in the functional and pain outcomes of ARCR and MRCR (21), thereby rejecting the hypothesis that ARCR has better short-term outcomes.
In assessing the complications of these two surgery techniques, no complications were observed in either of the two groups. Hughes et al. reported significantly higher infection rates in open surgery (22). As noted, due to the smaller incision made in ARCR, the chances of complications such as infection, bleeding, and deltoid muscle detachment were minimized. The reason for the disparities between the results of different studies might be the surgeons’ skill in managing the surgery.
In the present study, the duration of surgery was significantly longer in ARCR than that in MRCR. Van der Zwaal et al. (23) showed that, on average, fully arthroscopic surgeries took longer time compared to MRCR, but the difference was not significant. Liu et al. also reported that ARCR took almost 15 minutes longer than MRCR (19). ARCR is highly dependent on the surgeon’s skills and experience. In addition, only implantable suture anchor can be used in ARCR, and the surgeon has to spend more time on this step. Since it has a variety of repair options, from bone tunneling to implantable suture anchor, MRCR is apparently easier to learn and takes less time to perform. In addition, the quality of the arthroscopy device may also affect the duration of surgery.
This study had some limitations. The choice of surgical method for patients was based on their financial ability; if patients could afford arthroscopy, it was used. The poor quality of arthroscopy devices in our medical centers made surgery in the ARCR group longer and more difficult. Furthermore, patients were not monitored between follow-up times, and some issues, such as patient exercise at home, which plays an important role in patient recovery, could not be assessed. In addition, a relatively small sample size was another limitation of our study.
5.1. Conclusions
We witnessed that shoulder function, disability, ROM, and pain were not different between mini-open and arthroscopic rotator cuff surgeries. However, the MRCR appeared to be a better choice than arthroscopic repair due to its cost-effectiveness and shorter duration of surgery.