Prostate cancer (PC) is one of the most frequently occurring cancers among men in Iran (
1). It is predicted that the number of cases will almost double (to 1.7 million) by 2030 (
1). Often, men with PC live longer post-diagnosis, with recent statistics indicating survival rates of up to 76.5% five years after diagnosis (
2). The high rate of cancer survival is likely related to advances in early detection such as through the screening of prostate-specific antigen (PSA) and treatment modalities such as surgery (e.g., radical prostatectomy), androgen deprivation therapy (ADT), and radiation therapy (
3). Regardless of the treatment strategies, PC survivors often experience a very high rate of morbidity caused by cancer and its treatments, particularly ADT. Examples of these side effects include significant reductions in various aspects of the quality of life, which often becomes more pronounced over time or with additional treatment (
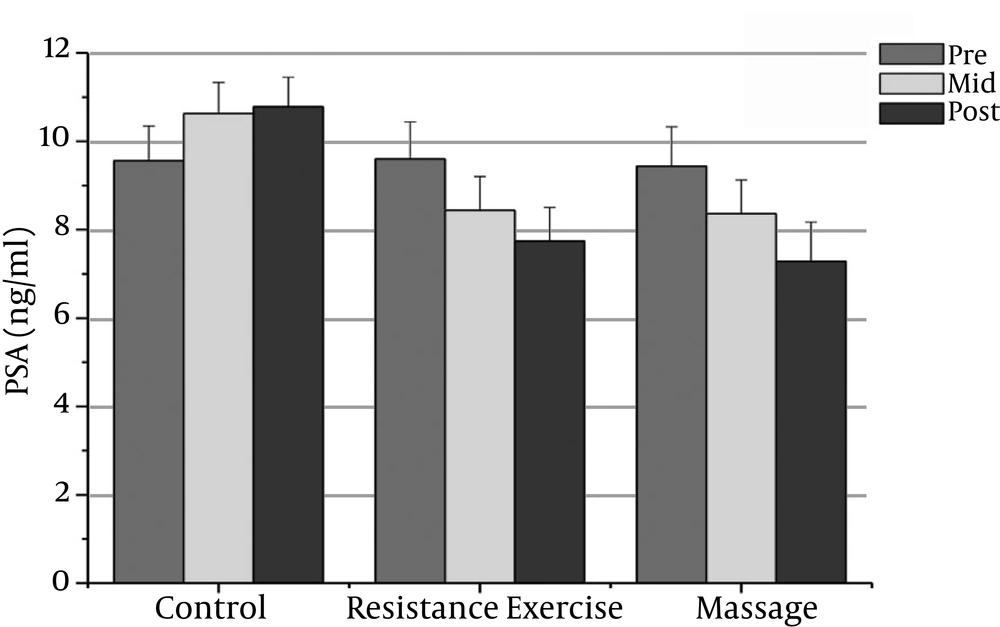
4). PSA is a widely used tumor marker in the screening and follow-up of PC. Because PSA measurement has such a crucial role in the management of PC, any urologic intervention that may cause PSA elevation must be detected (
5). PSA is a serine protease produced by the epithelial cells of the prostate, and it serves to cause liquefaction of the seminal fluid. Galvao et al. (2010) reported that a combined resistance and aerobic exercise program, twice a week for 12 weeks, had no effect on PSA levels (
6). Epidemiological studies have shown that chronic inflammation may be predisposed to certain kinds of cancer (
7). Prostatic inflammation may represent an important factor influencing prostatic growth and the progression of symptoms (
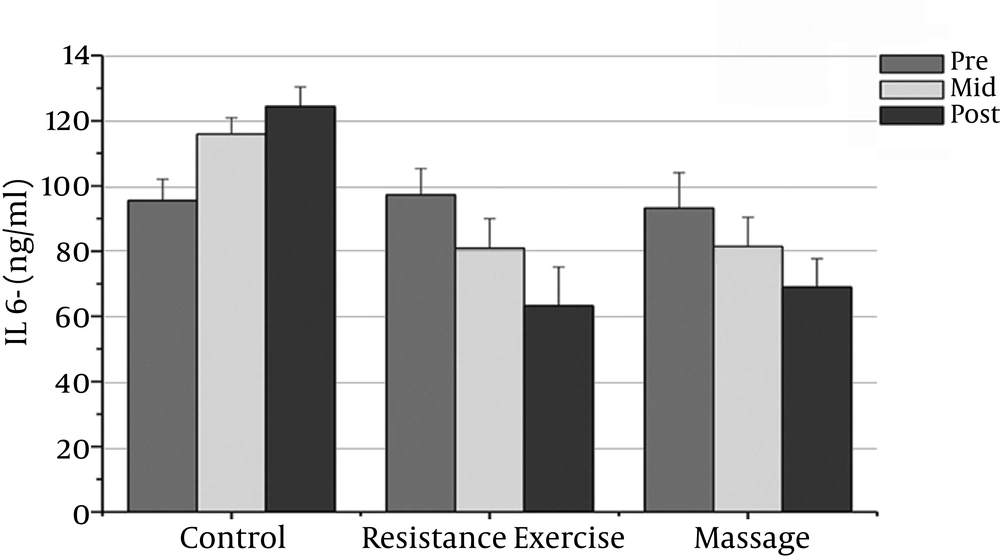
8). High-sensitivity C-reactive protein (hs-CRP), as an acute-phase plasma protein that increases during systemic inflammation, is one of the most frequently used inflammatory markers. CRP is produced primarily in the liver and is regulated by proinflammatory cytokines, especially interleukin-6 (
9). Both chronic and acute inflammation may lead to events that can cause proliferation in the prostatic tissue through a variety of mechanisms like special oxidative stress (
8). Inflammatory cells can become attracted to the prostate tissue microenvironment and can selectively promote the proliferation of prostate epithelial cells (
10). Recent studies suggest that hs-CRP levels are positively associated with cancer (
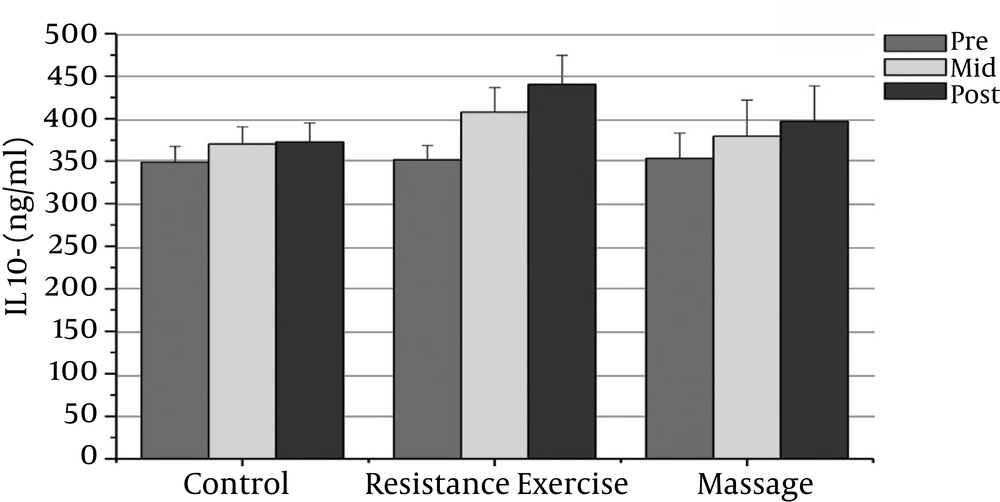
11). Therefore, it seems that high levels of CRP can promote the risk of PC and its metastasis. Interleukin-10 (IL-10), an anti-inflammatory cytokine, suppresses T1-helper cell responses and regulates lymphocytes, which are natural killer (NK) cells (
12). In PC, an overexpression of IL-10 has been reported (
12), but a reduced expression has been found when common polymorphisms in the promoters of the IL-10 gene were examined (
13,
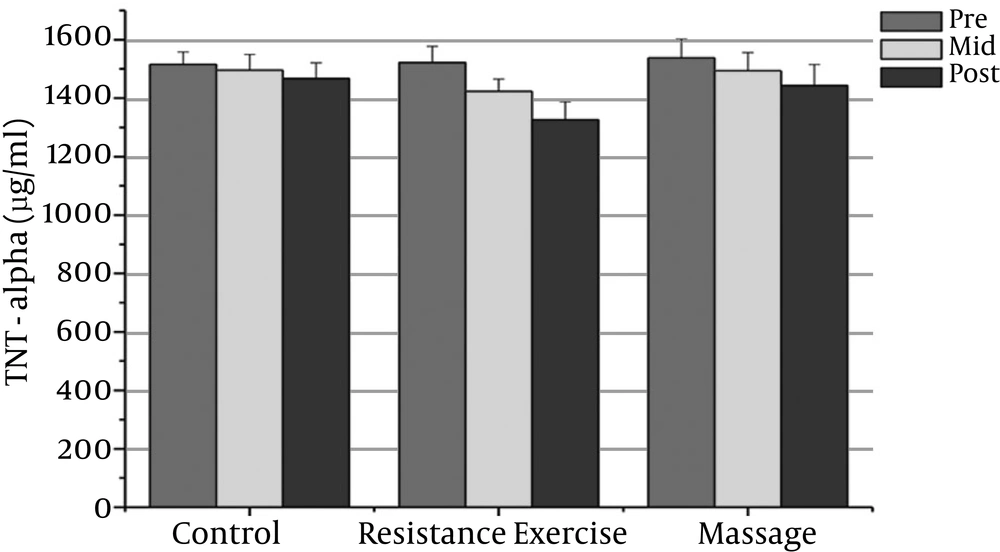
14). IL-6 expression is largely regulated by gene transcription. The tumor necrosis factor (TNF-α) is a strong promoter of IL-6. TNF-α is a cytokine that serves two conflicting functions: apoptosis or survival (
15). A high expression of TNF-α has been correlated with the proliferation and survival of malignant cells, the stimulation of angiogenesis, and the metastases and alteration of the response to chemotherapeutic agents (
16). Studies have shown that IL-6 involved in the regulation of immune responses causes cell growth rather than separation in many cell types. However, the effects of IL-6 on PC cells are contradictory (
17). Physical activity and exercise training has been suggested as a key lifestyle intervention due to its potential to limit, and even reverse, some toxicities (
18). Some authors examined the effects of exercise training in men with PC. Galvao et al. (2010) indicated that combined resistance and aerobic exercise improves muscle mass, strength, physical functions, and inflammatory markers in men undergoing ADT for PC (
6). Segal et al. (2003) found that 12 weeks of resistance training in men that receive ADT reduces fatigue and improves the quality of life and overall muscular strength (
19). Galvao et al (2006) showed that progressive resistance exercise has beneficial effects on muscle strength, functional performance, and balance in older men that receive ADT for PC and should be considered in preserving body composition and reducing treatment side effects (
20). In addition, Culos-Reed et al. (2010) showed that physical activity effectively attenuates many of the side effects of ADT and should be recommended to prostate survivors as an alternative therapy. Findings from their study further support the role of resistance training in preserving composition and improving physical functions in PC patients (
21). It seems that exercise training, especially resistance training, has functional benefits in patients with PC. Classic massage is one of the oldest and most regularly used complementary therapies, and it has become more and more popular in the past few years. It has been proven as an effective treatment for symptom relief in non-cancer patients (
22), and cancer patients also reportedly benefit from massage therapy. They experience pain relief and a reduction in nausea, fatigue, and other cancer-related symptoms (
23). Krohn et al. (2011) found that massage therapy is an efficient treatment for reducing depression in breast cancer patients. Insignificant results about stress, mood, and immunological parameters indicate that further study is needed to determine psychological and immunological changes under massage therapy (
22). Tarhan et al. (2005) reported that prostatic massage increases serum-completed PSA concentration but to a lesser extent than the total PSA and free PSA (
5). The effects of massage therapy in men with PC remain unclear.