1. Background
Calcifying tendonitis (CT) is a frequent pathology and a common cause of shoulder pain and labour inhability (1). The origin is the deposit of calcium phosphate/carbonate over a previously healthy tendon (2, 3). The pathogenesis is unknown but it is believed that fibrosis, tendon necrosis and associated degeneration could favour the deposit of crystals (4, 5). However, some authors believe it is not a degenerative process, but an active cell-mediated one (5-7).
Three stages with clinical/histological/radiological correlations are described, and sometimes overlap: 1) Pre-calcification: tenocyte metaplasia and chondrocyte transformation; 2) Calcification: a) formative (reservoir of vesicles in matrix), b) resorptive (spontaneous resorption by macrophages/multinucleated cells by phagocytosis); 3) Post-calcification: collagen remodeling and tendon repair (1, 2, 6).
The clinical picture is highly variable. There are asymptomatic patients (incidental radiological finding), patients with chronic pain and patients in acute painful crisis, mainly associated with the resorptive phase (8). The diagnosis is clinical and radiological (1, 8, 9). CT treatment is initially conservative and depends on its evolutionary stage (10).
CT could undergo spontaneous pain relief and calcification resorption, but with great variability. Bosworth reports a calcification reduction in 9.3% of cases during three years, Garner publishes a 33% resolution during three years, and Wagenhauser a 27.1% resorption during 10 years. That is a very long painful period of time, affecting patient’s quality of life; therefore, an adequate treatment should be accomplished (11).
Conservative treatment includes Non-Steroidal Anti-Inflammatory Drugs (NSAIDs), physiotherapy, electrotherapy (micro waves, short waves, transcutaneous electrical nerve stimulation (TENS), ultrasounds, iontophoresis, interferential and pulsed electromagnetic therapy) (8). It is demonstrated recently that different electrotherapy techniques are useful to reduce pain but not the calcification on CT patients (8).
Iontophoresis with acetic acid is a safe, common and cheap treatment and it was the only option available for decades capable of acting over the calcification. However, there are only a few clinical studies that support its effectiveness (1, 3, 12-15).
Electro shock wave therapy and arthroscopy are two advanced therapeutic options in CT treatment (16). They are as effective as iontophoresis; however, they are painful, expensive and not free of risks or complications (1).
2. Objectives
The current study aimed to clinically characterize CT through a prospective quasi-experimental before-and-after study which provides a level of demonstrable evidence to support the decision making and demonstrate the effectiveness of acetic acid iontophoresis and ultrasound to treat CT.
3. Methods
3.1. Design
Prospective, not randomized, quasi-experimental pretest-posttest intervention study.
3.2. Patients
The study included 44 patients diagnosed clinically and radiologically with shoulder CT who attended the rehabilitation department, Santísima Trinidad's General Foundation hospital, in Salamanca-Spain, from June 2014 to April 2016 (22 months).
Inclusion criteria: 1) All patients with clinical and radiological diagnosis of CT were referred to the rehabilitation department from traumatology, rheumatology, familiar Medicine departments, etc.; 2) Older than 18 years; 3) Signing the informed consent and accepting the proposed therapeutic method.
Exclusion criteria: 1) Any patients with electrical devices (pacemaker and electrical stimulator) which constitute formal contraindication to electrotherapy treatment; 2) Intolerance or allergy to acetic acid, erythema or burns caused by the treatment; 3) Osteoarthritis, inflammation or infection on the shoulder; 4) Cancer or any other severe or mental diseases.
3.3. Evaluation
Socio-demographic data (age, gender, occupation, laterality, dominance and occupation), personal history (diseases, pacemakers and electrical stimulator), and radiological characterization of calcification (formative/resorptive) were obtained. The articular balance and shoulder functional tests of the shoulder were evaluated at the start/end of treatment. The treatment protocol was approved by the ethical committee of the hospital.
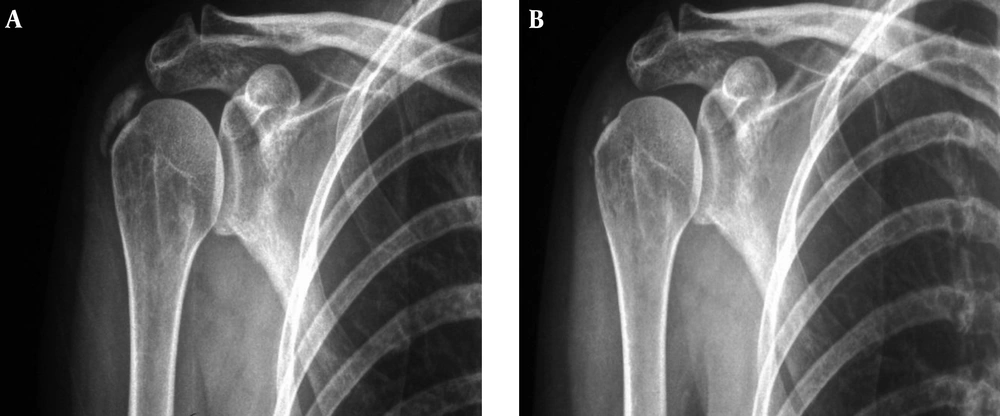
Outcome Measures: 1) Pain: measured by visual analogical scale (VAS); 2) Calcification size: in millimetres; both evaluated radiologically at the beginning/end of the treatment (Figure 1).
3.4. Intervention
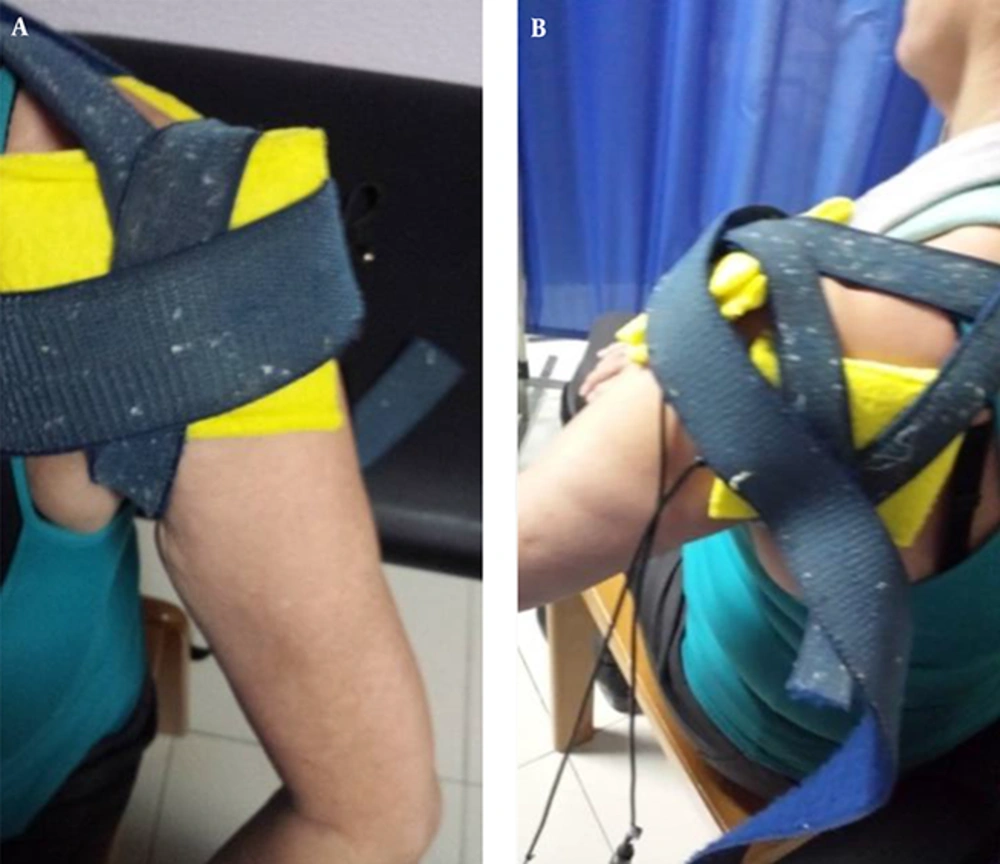
All recruited patients were given 5% acetic acid Iontophoresis, 2 mL dropped into a gauze and placed on a moistened cation (negative electrode) (Figure 2), on the anterior aspect of the affected greater tuberosity. The anion (positive electrode), also moistened, was placed at a distance of 10 cm from the cation (on supraspinous fossa muscle), to allow the passage of current flow. Both damp cloth coated electrodes were attached with a belt, allowing full contact, to avoid the risk of burning (Figure 3). A 4.7 mA galvanic current was applied for 10 minutes (Figure 2). Subsequently, continuous ultrasound with an intensity of 1 W/cm2/5 minutes and a 1 MHz frequency was applied on the greater tuberosity of the shoulder to promote drug absorption and decrease pain (3).
To perform the treatment protocol, two European medical devices were used: 1) For Iontophoresis, ENDOMED 581ID (Enraf Nonius® CE 0197), located on Salamanca (Spain), was used; 2) For ultrasound, SONOPULS 490 (Enraf Nonius ® CE 0197), located on Salamanca (Spain), was used.
3.5. Follow-up
Periodic reviews were performed (every 10 days) to assess pain and radiological change in size and/or disappearance of calcification by radiological evaluation. The minimum clinically significant change for pain measured by VAS is one point; it is considered a significant improvement if the change is greater than three points (17). The radiographic measurements of the calcification were made in millimetres, on 100%-size, posterior anterior plain radiographs of the shoulder, assessing the calcification in its longest axis. If there was more than one calcification, the full measure corresponded to the sum of these calcifications measured separately (1). The effectiveness of treatment with iontophoresis considering the result of variable “size of calcification” was measured as follows: 1) Cured/success (calcification diminishing more than 75% or total disappearance); 2) Improved (decreased calcification 25% - 75%); 3) Failure (if calcification decreased less than 25% or did not disappear). Clinical improvement included decreased pain (measured by VAS), the disappearance of the painful manoeuvres and functional mobility recovery.
3.6. Statistical Analysis
SPSS ® ver. 20.0 statistical package was used. To analyse quantitative descriptive variables, averages were used; while for qualitative variables, percentages and frequencies were used. To contrast the quantitative variables, paired T-test was used; while for qualitative variables, the Chi2 test was used. To compare the effect of different variables, a multiple logistic regression model was conducted, comparing the independent variable treatment (iontophoresis and ultrasound) with different variables (age, gender, location, time of illness, pain and calcification size). The level of significance was 99% (P < 0.01).
4. Results
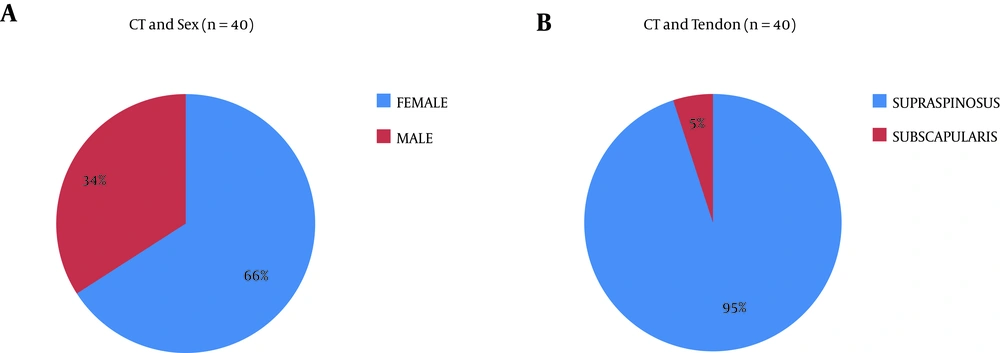
Mean age was 54.2 years (n = 44), 65.9% female (; n = 29) with a female to male ratio 2: 1 (Table 1, Figure 4). The most affected tendon was supraspinatus (95%; n = 38), followed by subscapularis tendon (5%; n = 2) (Table 1, Figure 4). As for laterality, the most frequently affected shoulder was left (55%; n = 22), right shoulder (45%; n = 18) and Bilateral (4.5%; n = 2) (Table 1). Most of the patients were right handed (93.18%; n = 41).
| Variables | Unit | % | AVa |
|---|---|---|---|
| Age, y | 54, 2 | 44 | |
| Female, n | 29 | 65.9 | 44 |
| Male, n | 15 | 34.1 | 44 |
| Ratio female/male | 2:1 | ||
| Supraspinosus, n | 38 | 95 | 40 |
| Subscapularis, n | 2 | 5 | 40 |
| Right shoulder, n | 19 | 43.2 | 44 |
| Left shoulder | 23 | 52.3 | 44 |
| Bilaterality, n | 2 | 4.5 | 44 |
| Right handed, n | 41 | 93.18 | 44 |
| Smoking, n | 15 | 34.09 | 44 |
| Time of illness (months) | 5.48 | ||
| Formative, n | 30 | 68.18 | 44 |
| Resorptive, n | 14 | 31.82 | 44 |
| Time of illness < 3months | 26 | 59.1 | 44 |
| Time of illness > 3months | 18 | 40.9 | 44 |
| Complications (burn) | 4 | 9.09 | 44 |
| Administrative works, n | 26 | 59.1 | 44 |
| Manual Works, n | 18 | 40.9 | 44 |
aAV, analyzed value.
The personal history associated with CT showed smoking (34.09%; n = 15), diabetes (4.5%; n = 2) and calcium intake secondary to osteoporosis (2.27%; n = 1) (Table 1).
Disease average time was 5.5 months. Acute-subacute pain (less than three months) was more frequent (59.1; n = 26) than chronic pain (greater than three months; 40.9%; n = 18) (Table 1).
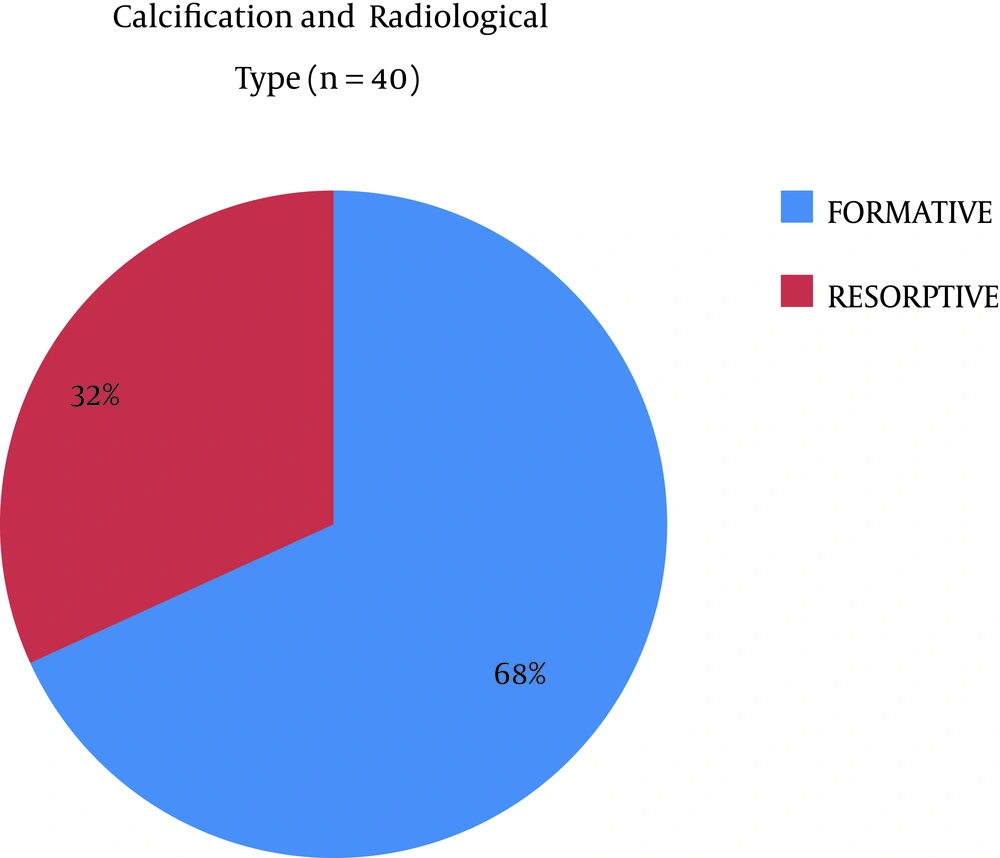
The most common radiological type was formative (68.18%; n = 30), followed by resorptive (38.72%; n = 14). The average number of sessions applied was 19. A 9.01% of patients (n = 4) discontinued treatment due to intolerance, erythema and/or burn; therefore, they completed treatment with ultrasound or short wave as tolerated. Regarding occupation, 59.1% (n = 26) had administrative positions, while 40.9% (n = 18) performed manual jobs (Table 1).
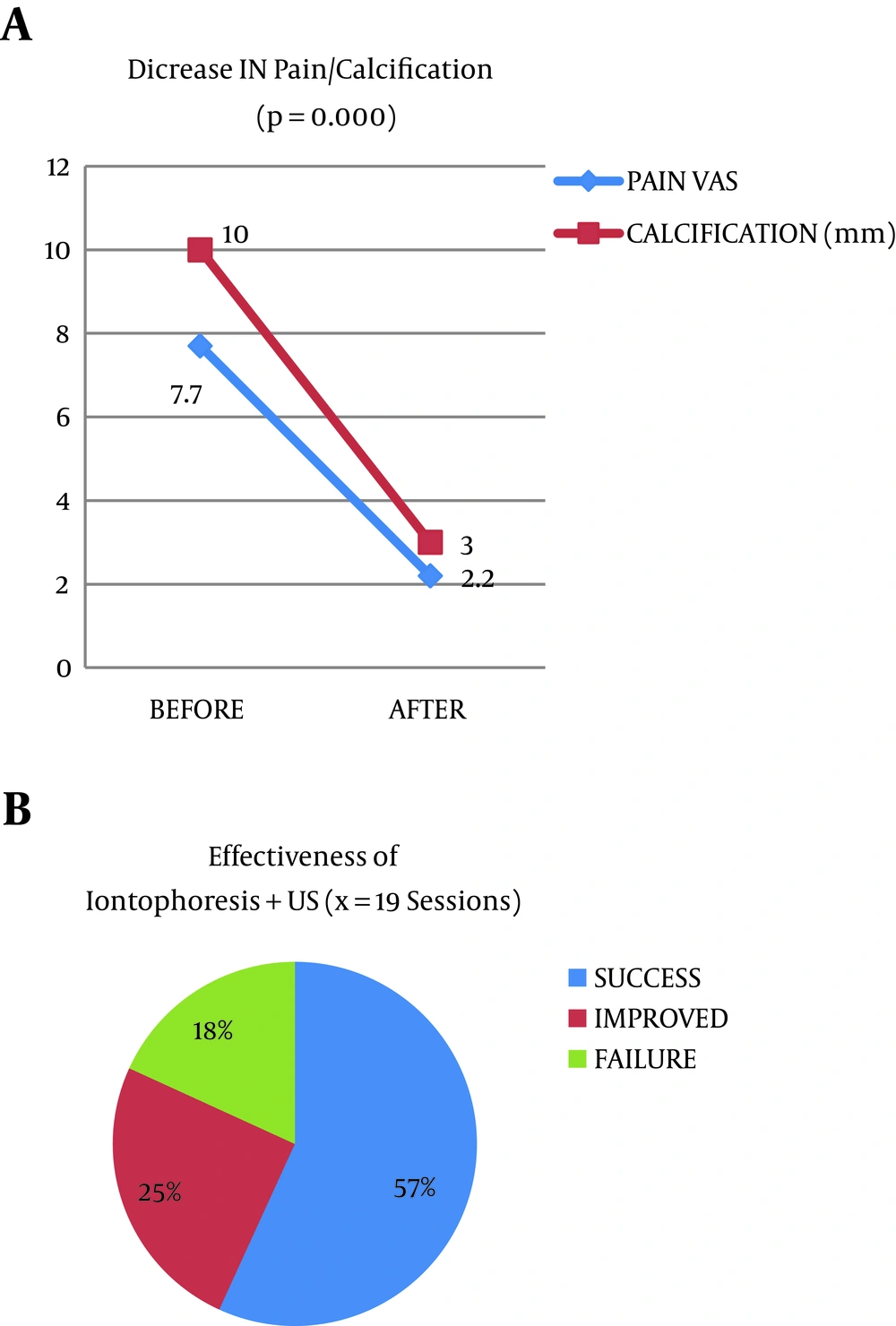
The average initial pain was 7.7 points, and significantly decreased (P = 0.0000) post treatment to 2.2 points (Figure 6). The initial average size of the calcifications was 10 mm and significantly decreased (P = 0.0000) post treatment to 3 mm (Figure 6).
The change of calcification was an outcome variable. This represented a success/cure rate of 56.8% (n = 25), an improvement rate of 25% (n = 11) and a failure rate of 18.2% (n = 8) (Figure 6).
The logistic regression study between the variables pain (VAS)/radiological change, when compared with other variables (age, gender, duration of disease, tendon, calcification type, laterality and smoking) reveals that pain post treatment and radiological change (size of calcification) were the most relevant data on all models. Thus, by controlling other variables, iontophoresis was positively related to radiological change (odd ratios (OR) was high and greater than 1). The effect of treatment (iontophoresis) in the size of the calcification was independent from other variables, except for post VAS value (Table 2). In the subjects where calcification disappeared, it was more likely to find a lower VAS pain post treatment. Thus, by eliminating the independent variable (iontophoresis) in the latest model, the adjustment decreased significantly, indicating the relevance of the treatment variable (iontophoresis) in the logistic model (Tables 3, 4, 5 and 6). Patients, whose calcification did not disappear, had more pain both before and after treatment (Tables 4 and 5); therefore, the presence of calcification positively influenced the presence of pain. Laterality (involvement of right or left shoulder) did not influence the pain before or after treatment (Table 6).
| Model | Level of Significance | Pseudo-R2 (Wellness of Adjustment) | Variables on the Model (Sig.) |
|---|---|---|---|
| M1a | 0.238 | 0.576 | Post VAS (0.089) |
| M1b | 0.008 | 0.348 | Treatment, (0.032) Post VAS (0.026) |
| M2a | 0.066 | 0.496 | Treatment (0.048), Post VAS (0.059) |
| M2b | 0.007 | 0.352 | Treatment (0.031), Post VAS (0.024) |
| M3a | 0.321 | 0.505 | Post VAS (0.082) |
| M3b | 0.035 | 0.171 | Post VAS (0.043) |
aM1a, dependent variable radiological change with all variables; M1b, optimal: dependent variable radiological change with all variables analyzed with Wald statistics; M2a, dependent variable radiological change with selected variables (diagnosis, time of illness, number of sessions, smoking, VAS); M2b, optimal: dependent variable radiological change with selected variables (diagnosis, time of illness, age, number of sessions, smoking, VAS) analyzed with Wald statistics; M3a, dependent variable radiological change with all variables (without treatment); M3b, optimal: dependent variable radiological change with all variables (without treatment) analyzed with Wald statistics.
| Pain Measured by VAS (n = 44) | Mean VAS ± SD Pre-Treatment | Mean VAS ± SD Post-Treatment | Means Differences(95%CI) | P Value |
|---|---|---|---|---|
| Total | 7.7 ± 1.35 | 2.2 ± 1.89 | 5.57 (4.90; 6.24) | 0.001 |
Abbreviations: VAS, visual analogical scale; SD, standard deviation; CI, confidence interval.
| Radiological Change (n = 44) | Mean VAS ± SD Pre-Treatment | Mean VAS ± SD Post-Treatment | Means Differences (95%CI) | P Value |
|---|---|---|---|---|
| Disappearance | 7.71 ± 1.13 | 1.94 ± 1.349 | 5.77 (5.12;6,.43) | 0.001 |
| Non-disappearance | 8.29 ± 1.50 | 3.71 ± 3.302 | 4.58 (1.70; 7.44) | 0.01 |
Abbreviations: VAS, visual analogical scale; SD, standard deviation; CI, confidence interval.
| Radiological Change (n = 44) | Mean VAS ± SD Pre-Treatment | Mean VAS ± SD Post-Treatment | Means Differences (95%CI) | P Value |
|---|---|---|---|---|
| Disappearance | 7.83 ± 1.50 | 1.63 ± 1.28 | 6.20 (5.44; 6.98) | 0.001 |
| Diminish | 7.36 ± 0.92 | 2.91 ± 1.64 | 4.45 (2.88; 6.03) | 0.001 |
| Same | 8.43 ± 1.27 | 3.29 ± 3.15 | 5.14 (2.91; 7.37) | 0.01 |
Abbreviations: VAS, visual analogical scale; SD, standard deviation; CI, confidence interval.
| Shoulder Laterality (n = 44) | Median VAS ± SD Pre-Treatment | Median VAS ± SD Post-Treatment | Mean Differences (95%CI) | P Value |
|---|---|---|---|---|
| CT RSE | 7.33 ± 1.50 | 2.20 ± 2.21 | 5.13 (3.83; 6.44) | 0.001 |
| CT LSE | 7.84 ± 1.21 | 2.26 ± 1.85 | 5.58 (4.58; 6.57) | 0.001 |
Abbreviations: VAS, visual analogical scale; SD, standard deviation; CI, 95% confidence interval; CT, calcifying tendinitis; RSE, right supraspinosus; LSE, left supraspinosus.
5. Discussion
The use of acetic acid iontophoresis to treat CT of the shoulder is the most frequently applied therapeutic modality in rehabilitation departments for decades. However, there are few studies to support its use (3, 15); there are even conflicting results (13, 14). The current study is the first study that supports the use of iontophoresis with acetic acid and continuous ultrasound with demonstrable scientific evidence and a bigger sample size than those of the previous studies (3, 13, 14).
CT is a common, painful, crippling disease, with great socio economic impact (18), high demand and great use of resources (19) and labor absenteeism (8). Pain is the leading cause of disability due to loss of mobility. In the current study, 11.36% of patients (n = 5) had limited mobility. Some authors argue that this pain remains in 50% of cases up to a year after the first consultation (19), while others claim that CT can evolve spontaneously toward healing between three and ten years (11); this fact negatively affects patients’ quality of life in their personal, familial and work aspects (8).
CT is common in middle-aged working patients (30 - 50 years) (8, 15, 18). The mean age in the study was 54.2 years. It was similar to those of reported by Chico-Alvarez (52.5 years) (1), Fernández-Cuadros (53.96 years) (8), Ferrera (54 years) (20) and Arrebola et al. (53.1 years) (21), but differed from those of published by Rioja-Toro (48 years) (3) and Depalma and Kruper (45.2 years) (22). CT is more common in females (2, 8, 18, 20, 21), similar to the current study. The female/male ratio was 2:1. However, Jacobelli argued that CT was equally prevalent in both genders (8), while Hernandez-Díaz (15) and Hsu et al. (23) described a higher prevalence in males.
Chronic rotator cuff disease and CT are associated with work in awkward postures, lifting weights and performing repetitive movements. Recently, Chico-Alvarez (1) reported that 34.7% of her patients were manual workers and 65.3% administrative. This is in line with the current study, where 40.9% were manual workers and 59.1% administrative.
CT affects the right shoulder (1, 3, 8, 21, 24), although up to 25% to 30% can be bilateral (9, 18, 24). In the current study there was greater involvement of the left shoulder (52.3%; n=23), rather than the right one (43.2%, n = 19). Bilateral involvement in 4.5% (n = 2), although most patients (93.18%, n = 41) were right handed. CT most often affects the supraspinatus tendon, then the infraspinatus and subscapularis (8, 20, 24, 25). In the current series, CT affected mainly supraspinatus tendon (95%, n = 38), and to a lesser extent the subscapularis (5%, n = 2). Similar findings were published by Fernández-Cuadros et al. (8) and Adamietz (25).
The radiological diagnosis was made by radiography or ultrasound. MRI was only performed for cases suspected with muscle/tendon pathology. The various radiological classifications agreed that type I corresponded to located deposits, well-defined contours, dense texture and homogeneous consistency; whereas type II corresponded to scattered deposits, not-well-defined contours, cloudy consistency and heterogeneous texture1. This radiological characterization was important because type II (resorptive) had a better prognosis than type I (formative) (8).
CT treatment was controversial. A recent article demonstrated the effectiveness of different rehabilitation techniques to reduce pain but not the calcification (8). Until a few decades ago, the only option used to treat calcification was acetic acid iontophoresis. However, there are only three classic papers that assess their effectiveness; one favorably (Rioja-Toro et al.) (3), and two unfavorably (Perron and Leduc) (13, 14). A recent doctoral study favorably supported the use of iontophoresis on CT (1).
Iontophoresis is a noninvasive technique that increases the penetration of transdermal substances (drugs) through the skin layers (epidermis, dermis and hypodermis) in a controlled manner and by the application of electric current, based on physical-chemical principles of attraction and repulsion of charges (26). Its most common applications are: 1) Calcifying tendinitis and myositis ossificans (acetic acid) (27); 2) Controlling muscle spasms (calcium chloride and magnesium sulfate); 3) Inflammation (dexamethasone); 4) Soft tissue swelling (lidocaine); 5) Acute joint pain in rheumatoid arthritis (zinc oxide) (26). This technique is cheap based on the economic use of topical medications and since the electrotherapy equipment decreased in size and are more accessible due to low-production-costs (28).
Applying ultrasound to the skin increases its permeability and facilitates diffusion of different substances into the skin. This transport is called sonoferesis (29). Low frequency sonophoresis works synergistically with iontophoresis; Le et al. (30) used ultrasound 10 minutes prior to the application of iontophoresis, with good results.
In 1955 Psaki and Carrol introduced acetic acid iontophoresis as an effective treatment in shoulder CT (13, 14, 31). Kahn (31) considered that insoluble calcium carbonate precipitates could become soluble salts of calcium acetate, which could favor the reabsorption of the calcification: CaCO3 + 2H (CaH302)2 = Ca (C2H3O2)2 + H20 + CO2. Furthermore, the use of ultrasound for their mechanical and thermal effects could help disintegrate and reabsorb calcification due to increase in local vascularization.
The current study protocol consisted in applying iontophoresis with 2 mL of 5% acetic acid, 4.7 mA × 10 minutes, followed by continuous ultrasound 1 W/cm2/1MHz x 5 minutes. This protocol differed from those of Rioja-Toro et al. (3) (3 mL of 5% acetic acid iontophoresis for 20 minutes at 4.7 mA plus ultrasound 1.5 W/cm2), Perron (5% acetic acid iontophoresis (not specified amount) at 5 mA × 20 minutes followed by ultrasound 0.8 W/cm2 × 5 minutes) (13), Leduc (5% acetic acid iontophoresis, 20 mL at 5 mA × 15 - 20 minutes without ultrasound) (14) and Chico-Alvarez (5% acetic acid iontophoresis (not specified amount) at 4.7 mA for 20 minutes without ultrasounds) (1).
The average number of sessions in the current series was 19 (from 10 to a maximum of 40 sessions). The criterion to continue or discontinue treatment was the radiological evolution. Perron treated his patients for nine sessions (three sessions/week for three weeks) (13). Leduc treated them for ten sessions (three sessions/week the first two weeks, and then weekly for four weeks) (14). Rioja-Toro treated his patients for 40 sessions (five sessions per week) and evaluated them on 20th and 40th sessions (3). Chico-Alvarez treated his patients in 15 - 30 sessions depending on the radiological evolution (five sessions per week) (1).
The current study was quasi-experimental pretest-posttestd intervention. Rioja-Toro et al. (3) conducte a similar experimental pretest-posttest intervention. Perrón (13) conducted a randomized-experimental-study, similar to those of the Leduc et al. (14) and Chico-Álvarez (1).
To the best of authors’ knowledge, the present study supported the highest number of patients; the importance lies in the difficulty of prospectively collect such a number of patients. Perrón (13) invested four years to find 21 patients; Leduc (14), three years for 36 patients, but only 27 were used at the end. Rioja-Toro et al. (3) recruited 34 patients in two years; and Chico-Álvarez (1) spent a year to recruit 25 patients for each control group. The current study recruited 44 patients in a two-year prospective study.
The study achieved a significant decrease in pain from 7.7 to 2.2 points on the VAS scale. This finding was similar to that of Chico-Álvarez (1), who reduced pain from 5.7 to 2.7. Perrón and Malouin (13) and Leduc et al. (14) achieved improvements on pain, but not significantly. Rioja-Toro et al. (3) reported 54% disappearance of pain and 25.6% improvement in his series. All studies (including the current study) showed that iontophoresis with acetic acid reduced pain in CT of the shoulder.
The current study treatment protocol significantly decreased the size of calcification from 10 mm (beginning) to 3 mm (the end). There was a 56.8% (n = 25) success rate (disappearance calcification 75% - 100%), a 25% (n = 11) improvement rate (decrease in calcification between 25% - 75%), and an 18.2% (n = 8) failure rate (less than 25% decrease). The obtained results were consistent with those of Rioja-Toro et al. (3), who reported a 13.2% disappearance of calcification and a 46.4% decrease; that was a 59.6% modification of calcium deposits. Hernandez-Diaz reported a success rate of 43.5%, an improvement rate of 52.2% and a failure rate of 4.3% (15). Chico-Alvarez observed a radiological decrease in calcification from 9.1 mm (start) to 5.7 mm (at the end of treatment), and 3.4 mm in six months follow-up. In the current series, the rapid decline in calcification was probably because ultrasound enhances, the absorption of acetic acid and the resorption thereof. Leduc and Perron obtained radiological improvement of calcium deposits after iontophoresis, although no difference was observed between the groups. These differences were probably due to the lower number of sessions (nine and ten respectively).
In a previous study with a similar sample size (n = 40) authors found that the different rehabilitation techniques could reduce pain but not the calcification (EVA 5.47 to 2.28, improving 3 points) (8); therefore, authors wondered if pain was associated with calcification, for which a logistic regression study was conducted to see if calcification disappeared and pain diminished in the subjects. The findings of the current study confirmed the hypothesis. This explains that in a similar sample (n = 40) from a similar population (same geographical area), in which iontophoresis disappeared calcification, pain decreased from 7.7 to 2.2; improving 5.5 points on the VAS scale (more pain reduction than the cited article (8)).
5.1. Study Limitations
An important limitation of the study was the lack of a control group. It was mainly due to the limited number of cases. A 2-year-follow-up was needed to collect such a sample size. As the effectiveness of acetic acid Iontophoresis on CT was accepted for decades and all patients accepted the treatment, it was not ethical to deny the intervention. A pretest-posttest intervention study was applied in this specific situation, to solve the lack of control group, and to give clinical based evidence.
As a contribution to the study, it should be stated that it was difficult to accomplish prospective studies capable of collecting a sample size similar to that of the current experimental study. It was even more difficult to combine clinical-care with teacher-researcher practice. In such studies, the final goal of doctors is the benefit of science, students and ultimately patients. Researchers are urged to conduct similar studies to reproduce the current study and increase consistency and demonstrable clinical-based-evidence, given the encouraging results observed in the study.
5.2. Conclusions
CT is more common in middle-aged working females. It affects the supraspinatus tendon. It is associated with smoking and occupational risks (awkward positions and lifting weights).
Iontophoresis with 5% acetic acid and ultrasound is a safe, simple and inexpensive technique capable to reduce pain and calcification on the shoulder.
The current study showed a level of evidence 2B and grade of recommendation B that allows authors to postulate acetic acid iontophoresis with ultrasound as an effective technique, with a recommended degree of scientific evidence.