1. Background
Traditional medicine has been used in all societies and predates the advent of conventional or orthodox medicine (1). Anecdotal and empirical evidence suggest the co-existence of traditional and orthodox medical practices that are patronized by patients, especially in resource-limited countries (2). The continuous patronage of practitioners of traditional healthcare methods has often been concerned, which can help the poor health systems that are characterized by factors, such as the insufficient and skewed distribution of medical personnel between urban and rural areas, lack of transportation and access to facilities, and high cost of medical care (3). Despite limitations in conventional healthcare, some demands or patients-related factors, such as ignorance, peers and family pressure, poor socioeconomic status, aversion for implants, fear of amputation, cultural beliefs, and fondness for concoctions and incantations contribute to the support of traditional medicine (2).
Treatment by traditional bone setters (TBS) is a very specialized method of traditional medicine that is usually preserved along family lines with limited opportunities for non-family members to learn the practice via apprenticeship (4). Oyebola (4) reported that traditional medicine practitioners, such as traditional birth attendants, traditional medicine men (popularly called ‘Babalawo’ or ‘Dibia’) and TBS may provide primary healthcare for up to 90% of the rural dwellers in Nigeria. Also, in Nigeria, TBS have renowned for their roles in the management of fractures and dislocations (5-11) and compared with other groups of traditional caregivers, they enjoy high patronage and confidence by society (12, 13). However, the practice of TBS in Nigeria has been associated with many complications (11, 14-17), such as gangrene, non-union of fractures, limb shortening, osteomyelitis, and muscle contractures of the involved limb (15, 16, 18). Despite these complications, TBS services are still in high demand, as some patients abandon orthodox hospitals for treatment by TBS (18).
According to the World Health Organization (WHO), integrating trained traditional medicine practitioners in primary health care systems could lead to cost-effective and culturally-sensitive health delivery in developing countries (1). However, TBS services in Nigeria are not fully developed for MSK management. For example, rehabilitation is an essential component of the management of MSK disorders (19). Unfortunately, rehabilitation is virtually nonexistent in TBS services in Nigeria (4, 9, 16, 20), which raises a concern about the holistic role of traditional caregivers in healthcare delivery in Nigeria (21). Hence, more studies on knowledge and attitude about TBS services and their use in different regions in Nigeria should be conducted (15, 22-24), considering that the practices differ from region to region and are supported by the people’s beliefs more than their socio-demographic characteristics (24). Therefore, region-specific studies are needed on the practice of traditional bone setting in Nigeria.
2. Objectives
This study aimed at evaluating knowledge and attitude about the practice of TBS and its use for MSK disorders in selected rural communities in Southwestern Nigeria.
3. Methods
Community-dwelling individuals were included in this cross-sectional study from two rural communities (Ipetumodu and Asipa) in Ife North Local Government Area (LGA), Osun State, Southwestern Nigeria. They were randomly selected from 10 communities in the LGA. Both communities met the definition of a rural area concerning the limited social amenities and remoteness (25). Besides, Ipetumodu, and Asipa are patriarchal communities of predominantly Yoruba people with a population of about 120,000 and 12,500, respectively, according to the 2006 census in Nigeria (26).
3.1. Sample Method and Size
The sample size for this study was determined using the formula n = Z2pq/d2, where ‘n’ is a population of greater than 10,000; ‘Z’ represents normal deviation (1.96); ‘p’ is prevalence rate (i.e. 50% and is commonly used when the proportion of the certain characteristics in the target population is unknown); ‘q’ is 1-p; and ‘d’ is the degree of accuracy at the significance level of 0.05. A sample size of 384 cases was calculated. Considering unwillingness to participate and invalid responses, 10% was added to the calculated sample size and a total of 422 cases were estimated. However, a total of 398 consenting respondents participated in this study, therefore, yielding a response rate of 94.3%.
A multistage probability sampling based on the WHO guidelines for conducting a community-based survey was used in this study (27). In the Ipetumodu community, six out of the eighteen major streets were randomly selected. A household was served as the Primary Sampling Unit (PSU). A total of 60 PSUs were randomly selected from each street using the list of all households in the selected streets. Those within the PSU willing to participate were enrolled. In the Asipa community, smaller and more rural, enumeration of the areas for research was based on compounds. Six out of the nine compounds in Asipa were enumerated. Each compound has an average of about 30 households. Ten households from the selected compounds (60 households) were listed for the survey. All consenting adults in each primary sampling units were surveyed. The respondents were adult residents of the selected communities for no less than one year.
A structured questionnaire adapted from instruments employed in relevant studies (28, 29) was used and was scrutinized for face and content validity by experts. The questionnaire assessed demographic information, MSK disorders, and treatment by TBS. Some parts of the questionnaire were scored on a Likert scale to assess treatment by TBS. The reliability of the questionnaire was tested by a test-retest method among 20 rural dwellers in Ife central LGA and re-administered after seven days. The questionnaire was translated into the Yoruba language for those speaking in the Yoruba language.
3.2. Statistical Analysis
Descriptive statistics, including frequencies and percentages were used to summarized data. Chi-square was used to test the association between treatment by TBS and socio-demographic variables. Data were analyzed using the Statistical Package for Social Sciences (SPSS) version 16.0 and the alpha level was set at 0.05.
3.3. Ethical Approval
Ethical approval for this study was sought from the Ethics and Research Committees of the Institute of Public Health, Obafemi Awolowo University, Ile-Ife, Nigeria (HREC no.: IPH/12/296). All participants signed the informed consent to participate in the study following a full explanation about the purpose of the study.
4. Results
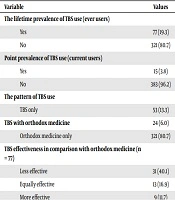
The socio-demographic characteristics of the respondents are shown in Table 1. The modal age group of the respondents was 26 - 33 years (28.4%). The respondents were largely males (53.5%) and of Christian background (50.0%). Lifetime, 12-month, and point prevalence of MSK disorders were 27.6%, 25.6%, and 21.1%, respectively (Table 2). The prevalence and pattern of MSK among respondents as highlighted in Table 2 showed that neck (21.6%), shoulder (17.6%) and wrist/arm (10.9%) were the most affected sites in 12-month prevalence. Also, neck (19.0%), lower trunk (15.5%), and shoulder (14.3%) were the most affected anatomical sites by MSK disorders for point prevalence analysis. The lifetime and point prevalence of the treatment by TBS for MSK disorders were 19.3% and 3.8%, respectively. More than one-tenth (13.3%) of the respondents utilized TBS services only, whereas 6.0% of them utilized both treatment by TBS and orthodox medicine. In addition, 16.9% of the TBS services users reported it as effective as orthodox medicine. Massage (61.0%) and splinting (14.3%) were the most common forms of treatment by TBS received for MSK disorders. Facilitators of TBS patronage were cheaper fees (42.9%); distance/accessibility (35.1%) and positive cultural beliefs (15.9%). Moreover, 41.6% of the users of services provided by TBS reported satisfaction with the services (Table 3). Table 4 shows the respondents’ knowledge about the complications of TBS services; 57.3% of the respondents were informed about the complications of the treatment by TBS, including malunion/non-union of fractures (36.0%), gangrene (19.7%), and paralysis (19.3%).
| Variables | Values |
|---|---|
| Age, y | |
| 18 - 25 | 72 (18.1) |
| 26 - 33 | 113 (28.4) |
| 34 - 41 | 51 (12.8) |
| 42 - 49 | 60 (15.1) |
| 50 - 57 | 35 (8.8) |
| 58 - 65 | 33 (8.3) |
| > 65 | 34 (8.5) |
| Sex | |
| Male | 213 (53.5) |
| Female | 185 (46.5) |
| Marital status | |
| Single | 176 (44.2) |
| Married | 174 (43.7) |
| Divorced | 23 (5.8) |
| Separated | 25 (6.3) |
| Religion | |
| Christianity | 199 (50.0) |
| Islamic | 171 (43.0) |
| Traditionalism | 26 (6.5) |
| Others | 2 (0.5) |
| Educational status | |
| Primary | 118 (29.6) |
| Secondary | 109 (27.4) |
| Tertiary | 167 (42.0) |
| Others | 4 (1.0) |
| Occupational status | |
| Professional | 72 (18.1) |
| Skilled | 126 (31.7) |
| Unskilled | 154 (38.7) |
| Unemployed | 46 (11.6) |
| Ethnicity | |
| Yoruba | 254 (63.8) |
| Igbo | 92 (23.1) |
| Hausa | 33 (8.3) |
| Others | 19 (4.8) |
| Monthly income, # | |
| < 7500 | 125 (31.4) |
| 7500 - 15000 | 150 (37.7) |
| 15000 - 50000 | 74 (18.6) |
| 50000 - 100000 | 35 (8.8) |
| 100000 - 50000 | 6 (1.5) |
| > 150000 | 8 (2.0) |
aValues are expressed as No. (%).
| Variable | Values |
|---|---|
| Lifetime prevalence | |
| Yes | 110 (27.6) |
| No | 288 (72.4) |
| 12-month prevalence | |
| Yes | 102 (25.6) |
| No | 296 (74.4) |
| Point prevalence | |
| Yes | 84 (21.1) |
| No | 314 (78.9) |
| Pattern of 12-month prevalence (n = 102) | |
| Neck | 22 (21.6) |
| Shoulder | 18 (17.6) |
| Upper trunk | 8 (7.8) |
| Elbow | 9 (8.8) |
| Wrist/arm | 11 (10.9) |
| Lower trunk | 10 (9.8) |
| Thumbs | 8 (7.8) |
| Lips/thighs | 6 (5.9) |
| Knees | 7 (6.9) |
| Others | 3 (2.9) |
| Pattern of point prevalence (n = 84) | |
| Neck | 16 (19.0) |
| Shoulder | 12 (14.3) |
| Upper trunk | 9 (10.7) |
| Elbow | 3 (3.6) |
| Wrist/arm | 11 (13.1) |
| Lower trunk | 13 (15.5) |
| Hips/thighs | 5 (6.0) |
| Knees | 9 (10.7) |
| Others | 6 (7.1) |
aValues are expressed as No. (%).
bNB, questions of the musculoskeletal disorders were answered using multi-choice tests.
| Variable | Values |
|---|---|
| The lifetime prevalence of TBS use (ever users) | |
| Yes | 77 (19.3) |
| No | 321 (80.7) |
| Point prevalence of TBS use (current users) | |
| Yes | 15 (3.8) |
| No | 383 (96.2) |
| The pattern of TBS use | |
| TBS only | 53 (13.3) |
| TBS with orthodox medicine | 24 (6.0) |
| Orthodox medicine only | 321 (80.7) |
| TBS effectiveness in comparison with orthodox medicine (n = 77) | |
| Less effective | 31 (40.1) |
| Equally effective | 13 (16.9) |
| More effective | 9 (11.7) |
| Not sure | 23 (29.9) |
| Type of TBS use (n = 77) | |
| Massage | 47 (61.0) |
| Splinting | 11 (14.3) |
| Traction | 9 (11.7) |
| Scarification | 8 (10.4) |
| Sacrifices and Incantations | 2 (2.6) |
| Reason for TBS use (n = 77) | |
| Cost-effectiveness | 33 (42.9) |
| Distance | 27 (35.1) |
| Availability | 1 (1.3) |
| The family or peer pressure | 1 (1.3) |
| Better services | 3 (4.0) |
| Cultural beliefs | 12 (15.9) |
| Satisfaction with TBS services (n = 77) | |
| Satisfied | 32 (41.6) |
| Unsatisfied | 18 (23.4) |
| Indifferent | 27 (35.1) |
aValues are expressed as No. (%).
| Variable | Values |
|---|---|
| Informed about the complications of TBS | |
| Yes | 228 (57.3) |
| No | 170 (42.7) |
| Complications of TBS (n = 228) | |
| Gangrene | 45 (19.7) |
| Malunion/nonunion of fractures | 82 (36.0) |
| Paralysis | 44 (19.3) |
| Chronic osteomyelitis | 15 (6.6) |
| Compartment syndrome | 8 (3.5) |
| Joint instability | 17 (7.5) |
| Limb shortening | 2 (0.9) |
| Osteoarthritis | 5 (2.2) |
| Soft tissue injury | 1 (0.4) |
| Wound infection | 9 (3.9) |
aValues are expressed as No. (%).
Table 5 shows the respondents’ beliefs and attitudes towards treatment by TBS. The subjects considered that treatment by TBS is needed in maintaining a healthy life (40.7%) and are more effective in healing than orthodox medicine (23.1%). Tables 6 and 7 indicate the associations between lifetime/point prevalence of treatment by TBS and socio-demographic variables. The findings indicated that treatment by TBS was not significantly influenced by socio-demographic variables (P > 0.05).
| Variable | Agree | Undecided | Disagree |
|---|---|---|---|
| Treatment by TBS was effective in maintaining a healthy life | 162 (40.7) | 126 (31.7) | 110 (27.6) |
| Treatment by TBS is associated with fewer side effects | 119 (30.0) | 140 (35.2) | 139 (34.9) |
| More healthy then orthodox medicine | 92 (23.1) | 173 (43.5) | 133 (33.4) |
| The herbal concoction in the treatment by TBS can build up the body’s natural defense system | 146 (36.7) | 158 (39.7) | 94 (23.6) |
| More users by opening clinics for TBS by the Government | 173 (43.5) | 127 (31.9) | 98 (24.6) |
| The increased knowledge about treatment by TBS leads to more use of this practice | 111 (27.9) | 91 (22.9) | 86 (21.6) |
| Parents should teach their children about treatment by TBS | 132 (33.2) | 131 (32.9) | 135 (33.9) |
| There are more users of the treatment by TBS, if it is used by friends | 160 (40.2) | 132 (33.2) | 106 (26.6) |
| Treatment by TBS is more effective than orthodox medicine | 98 (24.6) | 179 (45.0) | 121 (30.4) |
| Treatment by TBS is good for physical, mental and spiritual health | 114 (28.6) | 137 (34.4) | 147 (36.9) |
| Those who are afraid of going to the doctor use treatment by TBS | 134 (33.7) | 142 (35.7) | 122 (30.7) |
| People with a lower level of income are more likely to use treatment by TBS | 170 (42.7) | 102 (25.6) | 126 (31.7) |
aValues are expressed as No. (%).
| Variable | Yes | No | χ2 | P Value |
|---|---|---|---|---|
| Sex | 0.503 | 0.478 | ||
| Male | 44 (11.1) | 169 (42.5) | ||
| Female | 33 (8.3) | 152 (38.2) | ||
| Age, y | 0.515 | 0.520 | ||
| 18 - 25 | 16 (4.0) | 56 (14.1) | ||
| 26 - 33 | 21 (5.3) | 92 (23.1) | ||
| 34 - 41 | 7 (1.8) | 44 (11.1) | ||
| 42 - 4 | 14 (3.5) | 46 (11.6) | ||
| 50 - 65 | 2 (0.5) | 33 (8.3) | ||
| 58 - 65 | 10 (2.5) | (5.8) | ||
| > 65 | 7 (1.8) | 27 (6.9) | ||
| Marital status | 0.866 | 0.352 | ||
| Single | 34 (8.5) | 142 (35.7) | ||
| Married | 37 (9.3) | 137 (34.4) | ||
| Divorced | 4 (1.0) | 19 (4.8) | ||
| Separated | 2 (0.5) | 23 (5.8) | ||
| Religion | 0.755 | 0.385 | ||
| Islam | 30 (7.5) | 141 (35.4) | ||
| Christianity | 40 (10.1) | 159 (39.9) | ||
| Traditionalism | 7 (1.8) | 19 (4.8) | ||
| Others | 0 (0.0) | 2 (0.5) | ||
| Education | 1.757 | 0.185 | ||
| Primary | 17 (4.3) | 101 (25.4) | ||
| Secondary | 25 (6.3) | 84 (21.1) | ||
| Tertiary | 33 (8.3) | 134 (36.7) | ||
| Others | 2 (0.5) | 2 (0.5) | ||
| Occupation | 2.460 | 0.117 | ||
| Professional | 8 (2.0) | 64 (16.1) | ||
| Skilled | 25 (6.3) | 101 (25.4) | ||
| Unskilled | 35 (8.8) | 119 (29.9) | ||
| Unemployed | 9 (2.3) | 37 (9.3) | ||
| Personal monthly income, N | 0.34 | 0.853 | ||
| < 7,500 | 31 (7.8) | 94 (23.6) | ||
| 7,500 - 15,00 | 17 (4.3) | 133 (33.4) | ||
| 15,00 - 50,00 | 17 (4.3) | 57 (14.3) | ||
| 50,00 - 100,000 | 8 (2.0) | 27 (6.8) | ||
| 100,000 - 150,000 | 3 (0.8) | |||
| > 150,000 | 1 (0.3) | 7 (1.8) | ||
| Ethnicity | 0.296 | 0.586 | ||
| Yoruba | 50 (12.6) | 204 (51.3) | ||
| Igbo | 18 (4.5) | 74 (18.6) | ||
| Hausa | 7 (1.8) | 26 (6.5) | ||
| Others | 2 (0.5) | 17 (4.3) |
aValues are expressed as No. (%).
| Variable | Yes | No | χ2 | P Value |
|---|---|---|---|---|
| Sex | 0.293 | 0.588 | ||
| Male | 7 (1.8) | 206 (51.8) | ||
| Female | 8 (2.0) | 177 (44.5) | ||
| Age group, y | 1.961 | 0.161 | ||
| 18 - 25 | 5 (1.3) | 67 (16.8) | ||
| 26 - 33 | 6 (1.5) | 107 (26.9) | ||
| 34 - 41 | 1 (0.3) | 50 (12.6) | ||
| 42 - 49 | 1 (0.3) | 59 (14.8) | ||
| 50 - 57 | 0 (0.0) | 35 (8.8) | ||
| 58 - 65 | 1 (0.3) | 32 (8.0) | ||
| > 65 | 1 (0.3) | 33 (8.3) | ||
| Religion | 0.017 | 0.895 | ||
| Islam | 7 (1.8) | 164 (41.2) | ||
| Christianity | 6 (1.5) | 193 (48.5) | ||
| Traditionalism | 2 (0.5) | 24 (6.0) | ||
| Others | 0 (0.0) | 2 (0.5) | ||
| Ethnicity | 0.001 | 0.974 | ||
| Yoruba | 9 (2.3) | 245 (61.6) | ||
| Igbo | 4 (1.0) | 88 (22.1) | ||
| Hausa | 2 (0.5) | 31 (7.9) | ||
| Others | 0 (0.0) | 19 (4.8) | ||
| Occupation | 0.491 | 0.483 | ||
| Professional | 0 (0.0) | 72 (18.1) | ||
| Skilled | 7 (1.8) | 119 (29.9) | ||
| Unskilled | 7 (1.8) | 147 (36.9) | ||
| Unemployed | 1 (0.3) | 45 (11.3) | ||
| Educational status | ||||
| Primary | 6 (1.5) | 112 (28.1) | ||
| Secondary | 3 (0.8) | 106 (26.6) | ||
| Tertiary | 5 (1.3) | 162 (40.7) | ||
| Others | 1 (0.3) | 3 (0.8) | ||
| Personal monthly income, N | 0.365 | 0.546 | ||
| < 7,500 | 5 (1.3) | 120 (30.2) | ||
| 7,500 - 15,00 | 5 (1.3) | 145 (36.4) | ||
| 15,00 - 50,00 | 5 (1.3) | 69 (17.3) | ||
| 50,000 - 100,000 | 0 (0.0) | 35 (8.8) | ||
| 100,000 - 150,000 | 0 (0.0) | 6 (1.5) | ||
| > 150,000 | 0 (0.0) | 8 (2.0) | ||
| Marital status | 0.453 | 0.501 | ||
| Single | 6 (1.5) | 170 (42.7) | ||
| Married | 9 (2.3) | 165 (41.5) | ||
| Divorced | 0 (0.0) | 23 (5.8) | ||
| Separated | 0 (0.0) | 25 (6.3) |
aValues are expressed as No. (%).
5. Discussion
This study assessed the knowledge and attitude about the practice of TBS and its use for MSK disorders. The modal age group of the ever and current users of the treatment by TBS was 26 - 33 years. This age group represents the productive and mobile age group frequently involved in accidents that possibly have patronized bonesetters (9, 15). The practice of traditional bone setting in developing countries has partly rooted in erroneous socio-cultural beliefs in many of these societies. Particularly, there are pervading sentiments and beliefs that treatment by TBS, especially for fractures is more effective than orthodox medicine (13, 30), which may be accounted for as much as 19.3% of TBS use observed in this study. Furthermore, as a contributing factor for TBS patronage, it is the aversion for implants and the fear of amputation associated with conventional medical practice. It is noteworthy that Nigerians still believe that amputation is the only available option for the management of fractures, especially in complex cases in conventional medical practice (2, 13, 22).
The major services offered by TBS in this study was massage. This finding is consistent with previous reports that massage is a common practice among TBS, especially for closed injuries (9, 16, 31-33). However, in open wounds, patients may be reluctant to visit the TBS. Since TBS lack basic principles of infection control in wound management, their intervention in the treatment of the open fracture is associated with complications. Based on the results, 40.1% of the patients who had ever used treatment by TBS believed that TBS were less effective in the treatment of MSK disorders than orthodox medicine, whereas 11.7% of them believed the treatment by TBS was more effective. However, relevant studies conducted by Thanni (13) in Shagamu, Southwestern Nigeria and another study by Aderibigbe et al. (34) conducted in Ilorin, Northcentralal Nigeria revealed that the majority of patients who patronized treatment by TBS believed that it was very effective, competent and indispensable. Furthermore, in this study, 41.6% of the patients who had ever used treatment by TBS considered its outcome satisfactory. This finding is not consistent with that of Thanni (13), where only 4.3% of the patients felt that treatment by TBS led to very satisfactory outcomes. Lastly, socio-demographic factors (age, sex, marital status, religion, educational qualification, ethnicity, occupation, and personal monthly income) did not seem to influence patients’ views on the treatment by TBS and the outcome of their treatment. This study assessed the lifetime, 12 months period and point prevalence of MSK disorders and treatment by TBS. Similar to all cross-sectional or self-report studies, it is likely that the respondents in this study might have given imprecise answers concerning the MSK disorders or refused using TBS, which affect the external validation of the findings.
5.1. Conclusions
There was a positive attitude towards treatment by TBS for MSK disorders, despite the complications and shortcomings of the practices. Cost-effectiveness, socio-cultural beliefs, and easy access can increase patronage of treatment by TBS irrespective of the socio-demographic characteristics of the people.