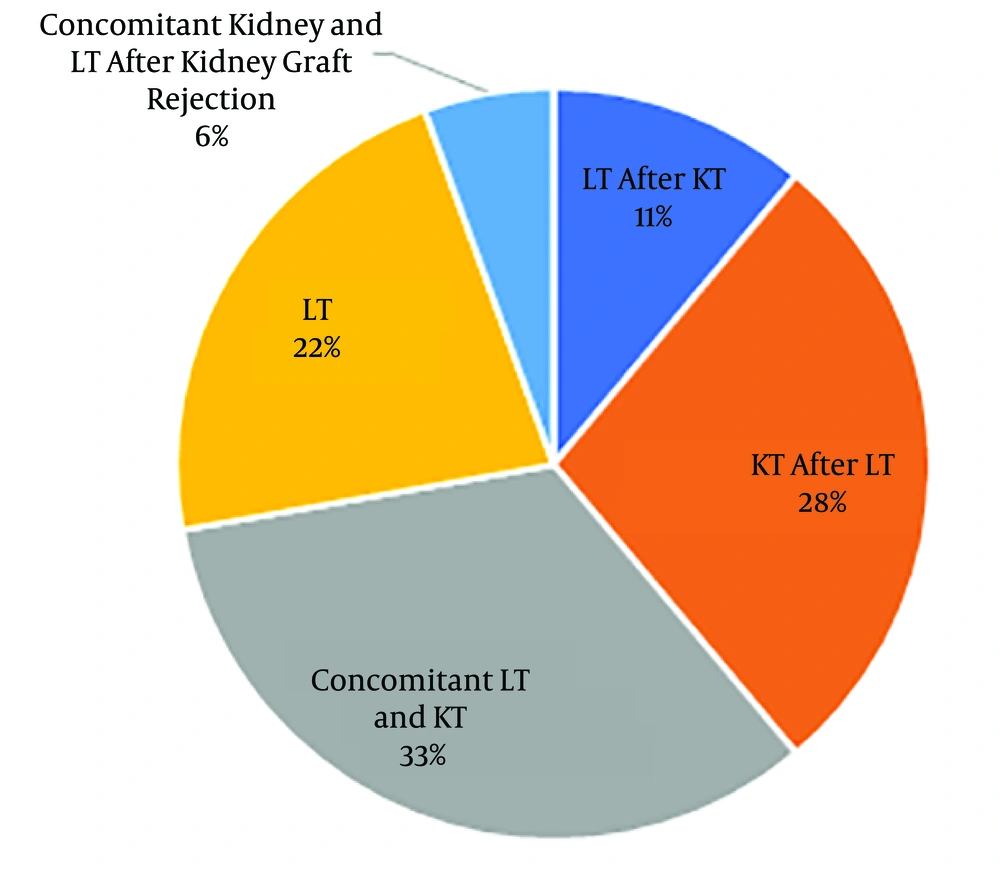
As PH is caused by a deficiency of the hepatic enzymes, it seems that liver transplantation can be an appropriate approach to prevent renal insufficiency and ESRD in these patients. However, ethical issues, the risk, and mortality of transplantation complications have limited early LT in these patients. Accordingly, concomitant kidney and LT after ESRD has been considered as the preferred therapeutic approach in patients with PH. It is noticeable that because of the hepatic nature of the disease and deficiency of hepatic enzymes as the triggering element, kidney transplantation is not the definite treatment for PH, and the deterioration of renal function after kidney transplantation is possible. In patients with high-grade CKD and GFR < 15, initial LT, and consequently kidney transplantation is warranted. In these cases, it is possible to conduct hemodialysis and remove excessive oxalate after LT and protect the grafted kidney from precipitated oxalate (
9).
The first case of concomitant liver and kidney transplantation in PH was conducted in 1984 for a patient who already had a damaged kidney graft due to re-precipitation of oxalate within the organ (
11). The survival rate in adult PH patients underwent isolated kidney transplantation has been 45%, whereas this rate has reported as 64% in those with simultaneous liver and kidney transplant. In children, these rates have been 14% and 76%, respectively, highlighting the importance of concomitant liver and kidney transplantation in children (
12,
13).
The systemic presence of calcium oxalate precipitations in other organs along with kidney stones are still probable even years after transplantation. For this reason, patients should be managed by crystallization inhibitors and be advised to consume a high volume of liquid (
12). Nevertheless, isolated kidney transplantation may be appropriate in type 2 PH, as a slow-progressing disease. No report of kidney insufficiency has been found due to PH type 3 (
9).
In a study conducted in Germany on 13 children with PH, 2 cases with ESRD underwent isolated LT, 4 cases underwent LT before kidney insufficiency, and finally, 7 cases were subjected to concomitant liver and kidney transplantations. One of the cases with ESRD who had been treated with isolated LT and managed by peritoneal dialysis died of peritoneal infection and hepatic abscess 11 months after transplantation. The second patient with ESRD treated with isolated LT also died of cytomegalovirus infection four weeks after the surgery. Among four children with early LT, 3 cases were completely recovered, whereas one patient developed kidney stones and then ESRD after 5.5 years. This patient underwent kidney transplantation 1.8 years later and now has a good clinical condition. Among patients simultaneously transplanted for liver and kidney, they had suitable clinical conditions with only one patient suffering from graft rejection due to steroid resistance. Another patient in this group was infected with polyoma. Overall, it seems that concomitant liver and kidney transplantation renders better therapeutic outcomes in patients with PH. On the other hands, isolated LT in patients with PH complicated by ESRD may not be effective in preventing mortalities. Early LT may also be partially beneficial; nevertheless, these patients may suffer from secondary complications and need kidney transplantation in the future (
14).
It has been suggested that early LT precedent to kidney failure can be beneficial in children with slow-progressing PH or those with PH presented during infancy. Nevertheless, simultaneous liver and kidney transplantation is the optimal choice in patients with ESRD (
15).
Based on the Cochat et al. (
10) study, selecting the type of transplantation in patients with PH can be optimized based on GFR condition. Accordingly, in patients with GFR of 40 - 60, isolated LT is applicable; however, transplantation is not the immediate option in these patients. Among those with GFR of 20 - 40, concomitant liver and kidney transplantation is considered; nonetheless, isolated kidney transplantation is sometimes inevitable in developing countries due to limited facilities and financial resources in these countries. Besides, concomitant liver and kidney transplantation cannot be performed in some patients because of their clinical condition. In patients with GFR < 20, isolated liver or kidney transplantation will be certainly insufficient, and concomitant or consecutive transplantation is the sole therapeutic choice. Also, the simultaneous graft strategy is warranted in PH patients who developed ESRD during the two first years of life (
10).
In PH patients who were subjected to kidney transplantation, it is recommended to perform extensive and prolonged dialysis to remove excessive and systemic oxalate from the body before surgery. Furthermore, living donors and close relatives as the source of organs can reduce the risk of graft rejection. Finally, the administration of nephrotoxic drugs, such as cyclosporine should be avoided in these patients (
16).
In our study, no patient developed kidney problems post-LT. However, infections occurred in some patients secondary to suppression of the immune system by immunosuppressive drugs. In addition, hepatic arterial and portal vein thrombosis were among common post-surgery incidences. Other post-transplant events were biliary problems observed in 5 patients, of whom one died of biliary obstruction. Such complications highlight the necessity for implementing novel approaches, such as gene therapy, cell therapy, regenerative medicine approaches in this field. Overall, the transplantation was tolerated by ten patients. Nevertheless, the ratio of mortality was relatively high, which should be more scrutinized in future studies.
In our study, we noticed that blood urea nitrogen and creatinine dramatically decreased from the peak averages of 50.39 and 6.59 pre-surgery to 38.67 and 2.42, respectively, which indicated a remarkable improvement in renal function. Also, the mean GFR boosted from 15.86 pre-transplant to 44.63 post-transplant.
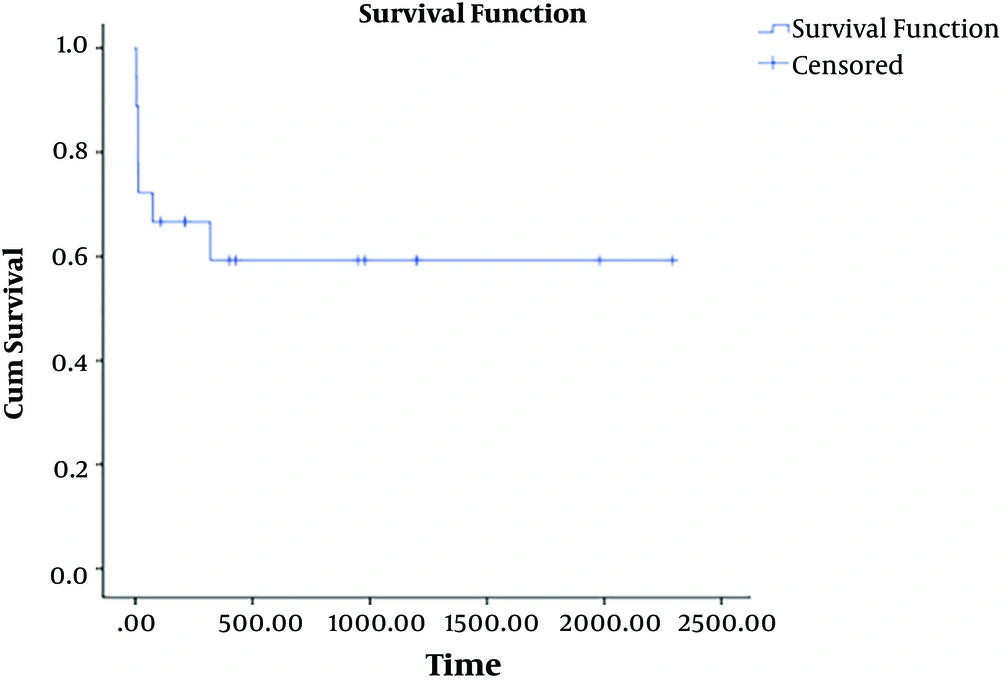
All the deaths occurred during the first year post-transplant. This indicates the high risk of mortality early after surgery. However, our study was performed in a relatively short period (a maximum of 6 years), and the mortality rate should be measured over longer periods.
LT can be considered as a definite treatment to avoid renal failure in PH patients. Post-transplant intensive care can escalate the success rate of organ transplantations in patients suffering from PH. Conducting studies over a long period is recommended to evaluate late-presenting complications in these patients.