1. Background
Erectile dysfunction (ED) is a common sexual disorder in men of reproductive age with an estimated prevalence of 1 - 10% in men younger than 40 years, which its incidence is on the rise. It is estimated that by 2025 about 322 million men will suffer from ED (1). ED and infertility are important health concerns with negative effects on the quality of life and couple’s relationship, which is emerging as an early marker for decreased general health (2). According to the evidence, the incidence of ED not only increases by age but also is associated with metabolic disorders, mental health disorders, and an unhealthy lifestyle (3, 4). Whether or not a cell phone or other electronic device usage is related to ED is still uncertain because of limited data. Marcin Słojewski shared a big concern that radiofrequency could pose a negative effect on ED (5). Al-Ali et al. investigated 20 ED and 10 healthy men and showed that ED men had significantly longer smartphone carrying time (6).
The number of ED patients who are seeking medical care at andrology clinics is on the rise. It has been shown that ED and infertility have a complex association with both male factors and their partners (2, 3). Of note, infertility can cause ED and other sexual problems (7), particularly infertile men had a higher prevalence of ED than those without fertility problems and the general population (8, 9). Also, ED is associated with the severity of impaired semen quality (10). Thus, an early diagnosis and identification of potentially related factors of ED occurrence would facilitate planning for consultation and receiving therapeutic interventions of infertile couples. In Vietnam, enough attention is not paid to sexual problems, particularly mainly because of cultural influences. Sexual function problem is a sensitive subject, and the suffered men usually feel embarrassed to discuss their problem, even to healthcare professionals. Besides, the andrology clinic was not fully developed. Therefore, there are a few reports about ED in Vietnam. For instance, Van Vo et al. investigated 746 men aged from 20 to 60 years (mean age of 44.3) in Hue city (central region of Vietnam) and reported a prevalence of 66.9% for ED (11) which is significantly higher than other reports. According to the best knowledge of the authors, no study has investigated the prevalence of ED, and there are evidence indicating an association between particular factors in men of infertile couples and ED in Vietnam. Within the context of Eastern culture, men in Vietnam still take more responsibility than women in some social aspects (12). The principle of male primogeniture is popular in Asian families, especially in Confucian countries like Vietnam. In terms of having descendants, the first-born man in a family (the biggest brother) gets pressure from his family and clan (13). If the first-born man suffered from infertility, he may get more pressure than others. These pressures might be one of the contributed factors of ED; however, no study has investigated this hypothesis. Hence, the current study intended to investigate the prevalence of ED in men of infertile couples, the relationship of several sociological lifestyles, and medical factors associated with ED.
2. Methods
2.1. Study Design and Population
The current cross–sectional study intended to investigate male patients referred to the Military Institute of Clinical Embryology and Histology of Vietnam Military Medical University to receive medical treatment for infertility from Jan 2018 to May 2018.
The sample size was calculated using the following formula with α of 0.05 and d (desired precision) of 0.075:
Following the study by Lotti et al, the prevalence of ED in men of the infertile family was considered as 17.8% (14), which resulted in a sample size of 100. A total of 138 men agreed to participate in the present study, who all of them underwent demographic and physical examination with a standard diagnostic protocol.
Inclusion criteria were being older than 18 years, heterosexual tendency, marital stability (not having marital troubles such as divorce or physical separation, etc.). Exclusion criteria included illiterateness, history of mental disorders, suffering from drug or alcohol addiction, having chronic diseases like hypertension, diabetes or hormone therapies, anatomic penile abnormalities, and not being sexually active.
2.2. Data Collection
All patients were guided to complete a Vietnamese version of the International Index of Sexual Function-15- Erectile dysfunction domain (IIEF-15-ED). According to the IIEF-15-ED, the severity of ED was classified into the following groups: no ED (EF score ≥ 26); mild ED (EF score 22 - 25); mild to moderate (EF score 17 - 21); moderate (EF score 11 - 16); and severe (EF score 1 - 10) (15).
Also, some sociological and lifestyle variables such as sleeping hours per day (hours), time spent on the smartphone (hours), total time spent on electronic devices (hours), smoking (pack per years: by multiplying the number of daily cigarette's packs (20 cigarettes per pack) using the number of year smoking), regular alcohol consumption, regular physical exercise, residence (rural or urban), occupation, working hours per week, monthly income, education level, number of siblings, being first-born (yes/no) were also collected.
Furthermore, medical variables, including age, height, weight, Waist-to-Hip Ratio, body mass index (BMI), were measured by physicians and medical staff. All patients also underwent semen analysis (SA), according to World Health Organization (WHO) criteria (2010) (16), and hormones evaluation (FSH, LH, PRL, Testosterone), using the Roche's Access chemiluminescent immunoassay Elecsys 2010 (Roche Diagnostics). Semen parameters were divided into the Azoospermia groups (No spermatozoa was observed after at least 2 SA, using 500g-centrifuged sediment microscopic inspection); main abnormal semen quality: H, O, A, T group (aka Hypospermia, Oligozoospermia, Asthenozoospermia, or Teratozoospermia) and Normozoospermia group.
2.3. Ethics Statement
The study was approved by the Ethical Committee of Vietnam Military Medical University (No.1150/2017/VMMU-IRB). Also, written informed consent was obtained from all patients, and the 1964 Helsinki declaration and its later amendments, as well as comparable ethical standards, were respected.
2.4. Statistical Analysis
Statistical analysis was administered using STATA 14.0 (STATA Corp, Texas, USA.). Continuous variables are expressed as mean ± standard deviation (SD). Chi-square test, Fisher's exact tests, Student's t-tests, and Mann-Whitney U test were used to analyze the data, as appropriate. Univariate and multivariate binary logistic regression analysis was conducted to disclose odds ratios (ORs) for factors associated with ED. Statistical significance was considered when P-value < 0.05.
3. Results
3.1. Demographic Characteristics of Participants and Prevalence of ED in the Male of an Infertile Couple Using IIEF-15 (ED Domain)
The mean age of 138 participants was 33.07 ± 5.77 years (ranged from 22 to 52), and the mean age of their wives was 30.04 ± 5.65 years (ranged from 20 to 48). Also, the year of infertility was 4.37 ± 3.76 (ranged from 1 to 18).
The ED was observed in 25 participants (18.1%) with mean IIEF-15 (ED domain) scores of 19.52 (compared to 28.50 in 113 participants (89.9%) of the non-ED group), including 13 mild (9.4%), 7 (5.1%) mild to moderate, 2 (1.4%) moderate, and 3 (2.2%) severe ED men (Table 1).
| Variables | Range (Min-Max) | Mean ± SD | No. (%) |
|---|---|---|---|
| Age (y) | 22 - 52 | 33.07 ± 5.77 | 138 (100) |
| Wife’s age (y) | 20 - 48 | 30.04 ± 5.65 | 138 (100) |
| Duration of infertility (y) | 1 - 18 | 4.37 ± 3.76 | 138 (100) |
| Erectile dysfunction | 25 (18.12) | ||
| Mild | 3 (2.2) | ||
| Mild to moderate | 2 (1.4) | ||
| Moderate | 7 (5.1) | ||
| Severe | 13 (9.4) |
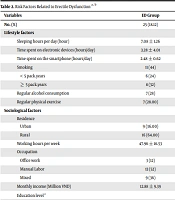
3.2. Risk Factors Associated with Erectile Dysfunction
All participants were divided into two subgroups of ED and non-ED. The mean age of ED and non-ED participants was 31.92 ± 6.32 and 33.32 ± 5.64 years, respectively. In addition, 80% of participants in the ED group were primary infertility compared to 64% in the non-ED group. There was no statistically significant difference between the study groups concerning the variables of age, wife's age, and duration and type of infertility.
Regarding the sociological aspect, the number of participants in the ED group that lived in the city was 9 (36%), compared to 48 (42%) in the non-ED group, but the statistical difference was not observed. Also, in the ED group, 3 (12%), 13 (52%), and 9 (36%) participants reported office work, manual labor, or mixed as their occupation, respectively.
There was no significant difference between the study groups concerning this variable. The monthly income and working hours per week were not significantly different between the study groups. Nevertheless, education was significantly different between the ED and non-ED groups. In the ED group, the proportion of participants who did not compete for junior-high-school, completed junior high school, or university (graduated or post-graduated) was 32%, 16%, 52%, respectively. While, in the non-ED group, these proportions were 9.73%, 28.32%, 61.95%, respectively. A similarity was observed concerning the mean number of siblings and being the first-born proportion in both groups. A detailed description of the abovementioned data is provided in Table 2.
| Variables | ED Group | Non-ED Group |
|---|---|---|
| No. (%) | 25 (18.12) | 113 (81.88) |
| Lifestyle factors | ||
| Sleeping hours per day (hour) | 7.08 ± 1.26 | 7.45 ± 1.07 |
| Time spent on electronic devices (hours/day) | 3.28 ± 4.01 | 4.75 ± 3.96 |
| Time spent on the smartphone (hours/day) | 2.48 ± 0.62 | 2.61 ± 0.20 |
| Smoking | 11 (44) | 76 (67.26) |
| < 5 pack.years | 6 (24) | 20 (17.70) |
| ≥ 5 pack.years | 8 (32) | 17 (15.04) |
| Regular alcohol consumption | 7 (28) | 41 (36) |
| Regular physical exercise | 7 (28.00) | 53 (46.90) |
| Sociological factors | ||
| Residence | ||
| Urban | 9 (36.00) | 48 (42.48) |
| Rural | 16 (64.00) | 65 (57.52) |
| Working hours per week | 47.96 ± 16.53 | 48.13 ± 16.95 |
| Occupation | ||
| Office work | 3 (12) | 34 (30.09) |
| Manual Labor | 13 (52) | 48 (42.28) |
| Mixed | 9 (36) | 31 (27.43) |
| Monthly income (Million VND) | 12.88 ± 9.39 | 13.24 ± 7.88 |
| Education level c | ||
| Not completed junior-high-school | 8 (32.00) | 11 (9.73) |
| High school | 4 (16.00) | 32 (28.32) |
| University, graduated, post-graduated | 13 (52.00) | 70 (61.95) |
| First-born | 15 (60) | 67 (59) |
| Number of siblings | 3.56 ± 1.04 | 3.48 ± 1.59 |
| Medical factors | ||
| Age (y) | 31.92 ± 6.32 | 33.32 ± 5.64 |
| Duration of infertility (y) | 4.9 ± 3.68 | 4.2 ± 3.80 |
| Type of infertility | ||
| Primary | 20 (80) | 73 (64) |
| Secondary | 5 (20) | 40 (35.40) |
| Physical measures | ||
| BMI (kg/m2) | 22.36 ± 3.46 | 22.75 ± 2.75 |
| WHR | 0.83 ± 0.05 | 0.84 ± 0.06 |
| Hormonal profile | ||
| FSH, mIU/m | 10.76 ± 12.40 | 7.29 ± 9.19 |
| LH, mIU/mL | 7.33 ± 7.61 | 5.45 ± 4.63 |
| Prolactin, ng/mL | 16.31 ± 15.83 | 14.06 ± 10.16 |
| Testosterone, ng/mL | 4.26 ± 2.92 | 5.03 ± 2.21 |
| Semen analysis d | ||
| Azoospermia | 12 (48) | 21 (18.58) |
| HOAT | 7 (28) | 36 (31.86) |
| Normozoospermia | 6 (24) | 56 (49.56) |
Abbreviations: ED, erectile dysfunction; WHR, waist-to-hip ratio; BMI, body mass index; FSH, follicle-stimulating hormone; LH, luteinizing hormone; SD, standard deviation; HOAT (including hypospermia, oligozoospermia, asthenozoospermia, teratozoospermia); VND, vietnamese dong (1 million VND ~ 43 US$).
aValues are expressed as mean ± SD or No. (%) unless otherwise indicated.
b The statistical difference using mean comparison t-test.
c The statistical difference using Fisher exact test
d The statistical difference using a chi-square test
In several medical aspects, semen quality was related to ED. There was no significant difference concerning other medical factors (physical measurements and hormonal profiles) (Table 2).
Factors associated with ED occurrence by univariate and multivariate analysis are presented in Table 3.
| Variables | Univariate Analysis | Multivariate Analysis | ||
|---|---|---|---|---|
| OR (95% CI) | P | OR (95% CI) | P | |
| Lifestyle factors | ||||
| Sleeping hours per day (hours) | 0.74 (0.51;1.09) | 0.13 | ||
| Time spent on the electronic devices (hours) | 0.90 (0.79;1.02) | 0.10 | ||
| Time spent on the smartphone (hours) | 0.98 (0.80;1.18) | 0.80 | ||
| Smoking | ||||
| No | 1.00 (Reference) | 1.00 (Reference) | ||
| < 5 pack. years | 2.07 (0.68;6.29) | 0.20 | 2.51 (0.70;9.07) | 0.16 |
| ≥ 5 pack. years | 3.25 (1.14;9.31) | 0.03 | 3.16 (0.98;10.18) | 0.05 |
| Regular alcohol use | ||||
| Yes | 0.57 (0.18;1.82) | 0.35 | ||
| No | 1.00 (Reference) | |||
| Regular physical exercise | ||||
| Yes | 1.00 (Reference) | |||
| No | 2.27 (0.88; 5.86) | 0.09 | ||
| Sociological factors | ||||
| Residence | ||||
| Urban | 1.00 (Reference) | |||
| Rural | 1.31 (0.53;3.22) | 0.55 | ||
| Working hours per week | 1 (0.97;1.03) | 0.97 | ||
| Occupation | ||||
| Officer | 1.00 (Reference) | |||
| Manual Labor | 3.07 (0.81;11.60) | 0.1 | ||
| Mixed | 3.29 (0.82;13.27) | 0.09 | ||
| Monthly income (Million VND) | 0.99 (0.94;1.05) | 0.84 | ||
| Education level | ||||
| Not completed junior high-school | 5.82 (1.46;23.17) | 0.01 | 5.11 (1.10; 23.77) | 0.03 |
| High school | 1.00 (Reference) | 1.00 (Reference) | ||
| University, graduated, post-graduated | 1.49 (0.45;4.91) | 0.52 | 1.43 (0.40;5.07) | 0.58 |
| First-born child | ||||
| Yes | 1.03 (0.42;2.49) | 0.95 | ||
| No | 1.00 (Reference) | |||
| Number of siblings | 1.04 (0.78;1.38) | 0.80 | ||
| Medical factors | ||||
| Age (y) | 0.95 (0.93;1.16) | 0.27 | ||
| Duration of infertility (y) | 1.04 (0.93; 11.16) | 0.42 | ||
| Type of infertility | ||||
| Primary | 1.00 (Reference) | |||
| Secondary | 0.46 (0.16;1.31) | 0.14 | ||
| Physical measures | ||||
| BMI, kg/m2 | 0.95 (0.81;1.11) | 0.54 | ||
| WHR (0.1) | 0.56 (0.24;1.27) | 0.16 | ||
| Hormonal profile | ||||
| FSH, mIU/mL | 1.03 (0.99;1.07) | 0.12 | ||
| LH, mIU/mL | 1.06 (0.98;1.13) | 0.13 | ||
| Prolactin, ng/mL | 0.85 (0.69;1.05) | 0.14 | ||
| Testosterone, ng/mL | 1.02 (0.98;1.05) | 0.37 | ||
| Semen analysis | ||||
| Normozoospermia | 1.00 (Reference) | 1.00 (Reference) | ||
| HOAT | 1.81 (0.56;5.84) | 0.32 | 2.36 (0.66;8.40) | 0.19 |
| Azoospermia | 5.33 (1.77;16.04) | 0.003 | 7.55 (2.18;26.16) | 0.001 |
Abbreviations: WHR, waist-to-hip ratio; BMI, body mass index; FSH, follicle-stimulating hormone; LH, luteinizing hormone; SD, standard deviation; HOAT (including hypospermia, oligozoospermia, asthenozoospermia, teratozoospermia); OR, odd ratio; CI, confidential interval.
According to the univariate analysis, there was an association between educational level, duration of smoking, and semen analysis, and ED. Other factors were not associated with ED occurrence. Then, all variables with a p-value of < 0.05 were included in the multivariate regression analysis using a backward stepwise elimination approach to determine factors associated with ED. In the final logistic regression model, risk factors associated ED included smoking > 5 pack/years (OR = 3.16; CI = 0.98 - 10.18; P = 0.05), not graduating from junior high school (OR = 5.11; CI = 1.11 - 23.8; P = 0.03), and azoospermia (OR = 7.55; CI = 2.18 - 26.16; P = 0.001). We observed a relatively high OR in men with smoking < 5 pack/years (OR = 2.51), abnormal semen analysis (hypospermia, oligozoospermia, asthenozoospermia, or teratozoospermia) (OR = 2.36), but there was no significant difference compared to the reference group.
4. Discussion
According to the WHO, infertility is a major problem worldwide, affecting up to 15% of all couples. Male factors contributed to up to 50% of infertile cases (17). In the diagnostic workup of infertile couples, male sexual dysfunction is a common complaint. Specifically, ED is a frustrating condition that affects not only an individual's health but also has a high sociological and psychological burden. ED shares a complex association with infertility. There are several pieces of evidence that the prevalence of ED is higher in men of an infertile couple than in the general population. In the present study, we reported the rate of ED in men of infertile couples was 18.1%, equivalent to the prevalence of ED in many previous studies reported (14, 18). However, this rate is significantly lower than the rate reported by Satkunasivam et al. and Yang et al. (18.1% vs. 30.5% and 18.1% vs. 57.8%, respectively) (19, 20). Van Vo et al. reported a prevalence of 66.9% for males with obvious ED symptoms, which is significantly high compared to the present study. This difference might be due to sample selection, as in Van Vo's research, the mean age of the participant was 44.3, while in our study, the mean age of participants was 33.06. However, Van Vo also reported that the prevalence of ED among men aged from 20 to 29, from 30 to 39, and over 40 was 5.5%, 24.7%, over 30%, respectively (11), which is quite similar to our study. The prevalence of severe ED is in agreement with other studies, but the overall rate of ED in male infertility is higher than that of men in normal couples of a similar reproductive age. This can be attributed to the sexual dysfunction caused by applied diagnosis and treatment. Besides, cultural and religious differences between various patient populations, different diagnostic criteria, and validated instruments of sexual disorders are potential factors that may contribute to the ED, according to the published studies (2).
In the present study, several sociological risk factors were examined. According to the findings, only low education (not completed junior high school) was a risk factor for ED (OR = 5.13) compared to the reference values (completed junior high school). Low-level education is considered a risk factor for ED, according to the Fourth International Consultation on Sexual Medicine (FICSM) (21). According to Yang et al., high educational level (high school and above) was a risk factor for ED. The difference between the findings of our study and those reported by Yang may be due to the difference in the socioeconomic statuses of participants (20). In addition, the difference between our study and Yang may be due to the difference in characteristics of populations and sample sizes. In the present study, we did not find any association between other variables (i.e., residence, occupation, working hours per week, monthly income, number of siblings, first-born) and ED. In Vietnamese culture, the first-born man in a family experience pressures from his family and clan. Therefore, due to the desire of having a descendant, he may get more pressure if he is suffered from infertility. We hypothesized that the pressure might be a contributed factor of ED, but no statistical difference was observed.
It is well known that smoking is a risk factor for ED in both the general male population and men of infertility (20, 22). In the present study, we confirmed that more than 5 packs/years of smoking is a significant risk factor for ED (OR = 3.16).
In the basic diagnostic workup of male infertility, a semen analysis is the first diagnostic test (23, 24). In this study, we analyzed a possible association between ED and semen parameters, indicating that azoospermia is a risk factor for ED (OR = 7.55). Patients with at least the main abnormal semen quality (including hypospermia, oligozoospermia, asthenozoospermia, or teratozoospermia) had a higher rate of ED (OR = 2.36), but there was no statically difference. Similar results are reported by other studies (10), which reflect the association between ED and sperm production in infertile males. In addition, the diagnosis and treatment process of men undergoing infertile evaluation with azoospermia has a negative impact on hypoactive sexual desire due to psychological burden and, therefore, they are aware that sexual acts cannot lead to pregnancy (18). Hence, an early diagnosis of ED may allow andrologists and therapists to make an interventional decision for men of infertile couples before receiving assisted reproductive technology.
As far as we know, this is the first report intended to determine factors associated with ED in males of infertile couples in the northern region of Vietnam. FSH, LH, and T profiles may play important roles in spermatogenesis and pregnancy rates (25, 26). Some articles showed that the T could affect male sexual behavior and function (27). Some studies showed a notable proportion of men of infertile couples suffered from T deficiency syndrome (TDS: 38%) and ED (28%) (7). However, the measurement of T depends on the type of T. The FICSM concluded that testosterone (free, total, or albumin-bound) levels had a weak relation with ED (21). ED in infertile men seems to be unrelated to hormone changes. Raj Satkunasivam indicated that T and bioavailable T serum levels were not associated with ED significantly, only LH level was a risk factor for ED (19). The positive impacts of Exogenous T therapy on male sexual function have not been proved yet (21), but it is known as a cause of infertility in men. Thus, T therapy is not recommended in men with infertility.
This study suffers from some limitations, including small sample size and not being a multicenter research. In addition, we did not investigate several mental health factors associated with ED, such as anxiety and depression. Hence, the results might not be representative, so a large-scale study is needed to extend our knowledge.
According to the findings, ED was more common in men of infertile couples than in men of non-infertile. Low level of education, smoking for a long period, and azoospermia were the main risk factors of ED in men of infertile couples. However, further large-scale studies are needed to extend the results.